
Medicare is a government national health insurance program in the United States, begun in 1965 under the Social Security Administration (SSA) and now administered by the Centers for Medicare and Medicaid Services (CMS). It primarily provides health insurance for Americans aged 65 and older, but also for some younger people with disability status as determined by the SSA, including people with end stage renal disease and amyotrophic lateral sclerosis.

Medicare is an unofficial designation used to refer to the publicly funded single-payer healthcare system of Canada. Canada's health care system consists of 13 provincial and territorial health insurance plans, which provide universal healthcare coverage to Canadian citizens, permanent residents, and depending on the province or territory, certain temporary residents. The systems are individually administered on a provincial or territorial basis, within guidelines set by the federal government. The formal terminology for the insurance system is provided by the Canada Health Act and the health insurance legislation of the individual provinces and territories.
Diagnosis-related group (DRG) is a system to classify hospital cases into one of originally 467 groups, with the last group being "Ungroupable". This system of classification was developed as a collaborative project by Robert B Fetter, PhD, of the Yale School of Management, and John D. Thompson, MPH, of the Yale School of Public Health. The system is also referred to as "the DRGs", and its intent was to identify the "products" that a hospital provides. One example of a "product" is an appendectomy. The system was developed in anticipation of convincing Congress to use it for reimbursement, to replace "cost based" reimbursement that had been used up to that point. DRGs are assigned by a "grouper" program based on ICD diagnoses, procedures, age, sex, discharge status, and the presence of complications or comorbidities. DRGs have been used in the US since 1982 to determine how much Medicare pays the hospital for each "product", since patients within each category are clinically similar and are expected to use the same level of hospital resources. DRGs may be further grouped into Major Diagnostic Categories (MDCs). DRGs are also standard practice for establishing reimbursements for other Medicare related reimbursements such as to home healthcare providers.
The Major Diagnostic Categories (MDC) are formed by dividing all possible principal diagnoses into 25 mutually exclusive diagnosis areas. MDC codes, like diagnosis-related group (DRG) codes, are primarily a claims and administrative data element unique to the United States medical care reimbursement system. DRG codes also are mapped, or grouped, into MDC codes.
Case mix, also casemix and patient mix, is a term used within healthcare as a synonym for cohort; essentially, a case mix groups statistically related patients. An example case mix might be male patients under the age of 50, who present with a myocardial infarction and also undergo emergency coronary artery bypass surgery.
Resource-based relative value scale (RBRVS) is a schema used to determine how much money medical providers should be paid. It is partially used by Medicare in the United States and by nearly all health maintenance organizations (HMOs).

Mark Barr McClellan is the director of the Robert J Margolis Center for Health Policy and the Margolis Professor of Business, Medicine and Health Policy at Duke University. Formerly, he was a senior fellow and director of the Health Care Innovation and Value Initiative at the Engelberg Center for Health Care Reform at The Brookings Institution, in Washington, D.C. McClellan served as commissioner of the United States Food and Drug Administration under President George W. Bush from 2002 through 2004, and subsequently as administrator of the Centers for Medicare and Medicaid Services from 2004 through 2006.

The quality-adjusted life year (QALY) is a generic measure of disease burden, including both the quality and the quantity of life lived. It is used in economic evaluation to assess the value of medical interventions. One QALY equates to one year in perfect health. QALY scores range from 1 to 0 (dead). QALYs can be used to inform health insurance coverage determinations, treatment decisions, to evaluate programs, and to set priorities for future programs.
Health care prices in the United States of America describe market and non-market factors that determine pricing, along with possible causes as to why prices are higher than in other countries.
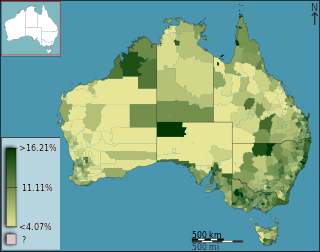
Health care in Australia operates under a shared public-private model underpinned by the Medicare system, the national single-payer funding model. State and territory governments operate public health facilities where eligible patients receive care free of charge. Primary health services, such as GP clinics, are privately owned in most situations, but attract Medicare rebates. Australian citizens, permanent residents, and some visitors and visa holders are eligible for health services under the Medicare system. Individuals are encouraged through tax surcharges to purchase health insurance to cover services offered in the private sector, and further fund health care.
Severity of illness (SOI) is defined as the extent of organ system derangement or physiologic decompensation for a patient. It gives a medical classification into minor, moderate, major, and extreme. The SOI class is meant to provide a basis for evaluating hospital resource use or to establish patient care guidelines.
The risk of mortality (ROM) provides a medical classification to estimate the likelihood of in-hospital death for a patient. The ROM classes are minor, moderate, major, and extreme. The ROM class is used for the evaluation of patient mortality.
A long-term acute care hospital (LTACH), also known as a long-term care hospital (LTCH), is a hospital specializing in treating patients requiring extended hospitalization. Hospitals specializing in long-term care have existed for decades in the form of sanatoriums for patients with tuberculosis and other chronic diseases. The modern hospital known as an LTACH came into existence as a result of the Medicare, Medicaid, and SCHIP Balanced Budget Refinement Act of 1999. The Act defines an LTACH as “a hospital which has an average inpatient length of stay of greater than 25 days.” Traditionally, LTACHs provide care for patients receiving prolonged mechanical ventilation.
Bundled payment is the reimbursement of health care providers "on the basis of expected costs for clinically-defined episodes of care." It has been described as "a middle ground" between fee-for-service reimbursement and capitation, given that risk is shared between payer and provider. Bundled payments have been proposed in the health care reform debate in the United States as a strategy for reducing health care costs, especially during the Obama administration (2009–2016). Commercial payers have shown interest in bundled payments in order to reduce costs. In 2012, it was estimated that approximately one-third of the United States healthcare reimbursement used bundled methodology.
The Medicare Physician Group Practice (PGP) demonstration was Medicare's first physician pay-for-performance (P4P) initiative. The demonstration established incentives for quality improvement and cost efficiency. Ten large physician groups participated in the demonstration, which started on April 1, 2005 and ran for 5 years. Previous funding arrangements, like the volume performance standard (VPS) and the sustainable growth rate (SGR) did not provide incentives to slow the growth of services. The Medicare PGP demonstration was intended to overcome that limitation in previous funding arrangements.
Health care finance in the United States discusses how Americans obtain and pay for their healthcare, and why U.S. healthcare costs are the highest in the world based on various measures.
Clinical documentation improvement (CDI), also known as "clinical documentation integrity", is the best practices, processes, technology, people, and joint effort between providers and billers that advocates the completeness, precision, and validity of provider documentation inherent to transaction code sets sanctioned by the Health Insurance Portability and Accountability Act in the United States.
A hospital readmission is an episode when a patient who had been discharged from a hospital is admitted again within a specified time interval. Readmission rates have increasingly been used as an outcome measure in health services research and as a quality benchmark for health systems. Generally, higher readmission rate indicates ineffectiveness of treatment during past hospitalizations. Hospital readmission rates were formally included in reimbursement decisions for the Centers for Medicare and Medicaid Services (CMS) as part of the Patient Protection and Affordable Care Act (ACA) of 2010, which penalizes health systems with higher than expected readmission rates through the Hospital Readmission Reduction Program. Since the inception of this penalty, there have been other programs that have been introduced, with the aim to decrease hospital readmission. The Community Based Care Transition Program, Independence At Home Demonstration Program, and Bundled Payments for Care Improvement Initiative are all examples of these programs. While many time frames have been used historically, the most common time frame is within 30 days of discharge, and this is what CMS uses.
Health care efficiency is a comparison of delivery system outputs, such as physician visits, relative value units, or health outcomes, with inputs like cost, time, or material. Efficiency can be reported then as a ratio of outputs to inputs or a comparison to optimal productivity using stochastic frontier analysis or data envelopment analysis. An alternative approach is to look at latency times and delay times between a care order and completion of work, and stated accomplishment in relation to estimated effort.




