Related Research Articles
A mental disorder, also referred to as a mental illness, a mental health condition, or a psychiatric disability, is a behavioral or mental pattern that causes significant distress or impairment of personal functioning. A mental disorder is also characterized by a clinically significant disturbance in an individual's cognition, emotional regulation, or behavior, often in a social context. Such disturbances may occur as single episodes, may be persistent, or may be relapsing–remitting. There are many different types of mental disorders, with signs and symptoms that vary widely between specific disorders. A mental disorder is one aspect of mental health.
Drug rehabilitation is the process of medical or psychotherapeutic treatment for dependency on psychoactive substances such as alcohol, prescription drugs, and street drugs such as cannabis, cocaine, heroin or amphetamines. The general intent is to enable the patient to confront substance dependence, if present, and stop substance misuse to avoid the psychological, legal, financial, social, and physical consequences that can be caused.Citation needed
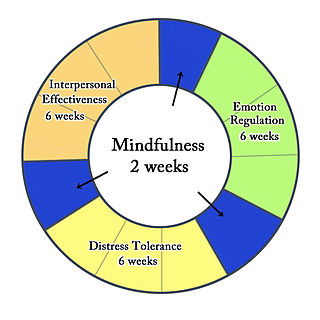
Dialectical behavior therapy (DBT) is an evidence-based psychotherapy that began with efforts to treat personality disorders and interpersonal conflicts. Evidence suggests that DBT can be useful in treating mood disorders and suicidal ideation as well as for changing behavioral patterns such as self-harm and substance use. DBT evolved into a process in which the therapist and client work with acceptance and change-oriented strategies and ultimately balance and synthesize them—comparable to the philosophical dialectical process of thesis and antithesis, followed by synthesis.

Mental health encompasses emotional, psychological, and social well-being, influencing cognition, perception, and behavior. According to World Health Organization (WHO), it is a "state of well-being in which the individual realizes his or her abilities, can cope with the normal stresses of life, can work productively and fruitfully, and can contribute to his or her community". It likewise determines how an individual handles stress, interpersonal relationships, and decision-making. Mental health includes subjective well-being, perceived self-efficacy, autonomy, competence, intergenerational dependence, and self-actualization of one's intellectual and emotional potential, among others. From the perspectives of positive psychology or holism, mental health may include an individual's ability to enjoy life and to create a balance between life activities and efforts to achieve psychological resilience. Cultural differences, personal philosophy, subjective assessments, and competing professional theories all affect how one defines "mental health". Some early signs related to mental health difficulties are sleep irritation, lack of energy, lack of appetite, thinking of harming oneself or others, self-isolating, and frequently zoning out.
Psychiatric nursing or mental health nursing is the appointed position of a nurse that specialises in mental health, and cares for people of all ages experiencing mental illnesses or distress. These include: neurodevelopmental disorders, schizophrenia, schizoaffective disorder, mood disorders, addiction, anxiety disorders, personality disorders, eating disorders, suicidal thoughts, psychosis, paranoia, and self-harm.
Emergency psychiatry is the clinical application of psychiatry in emergency settings. Conditions requiring psychiatric interventions may include attempted suicide, substance abuse, depression, psychosis, violence or other rapid changes in behavior.
Suicide intervention is a direct effort to prevent a person or persons from attempting to take their own life or lives intentionally.
Mental disorders are classified as a psychological condition marked primarily by sufficient disorganization of personality, mind, and emotions to seriously impair the normal psychological and often social functioning of the individual. Individuals diagnosed with certain mental disorders can be unable to function normally in society. Mental disorders may consist of several affective, behavioral, cognitive and perceptual components. The acknowledgement and understanding of mental health conditions has changed over time and across cultures. There are still variations in the definition, classification, and treatment of mental disorders.

Telepsychiatry or telemental health refers to the use of telecommunications technology to deliver psychiatric care remotely for people with mental health conditions. It is a branch of telemedicine.
A mental health professional is a health care practitioner or social and human services provider who offers services for the purpose of improving an individual's mental health or to treat mental disorders. This broad category was developed as a name for community personnel who worked in the new community mental health agencies begun in the 1970s to assist individuals moving from state hospitals, to prevent admissions, and to provide support in homes, jobs, education, and community. These individuals were the forefront brigade to develop the community programs, which today may be referred to by names such as supported housing, psychiatric rehabilitation, supported or transitional employment, sheltered workshops, supported education, daily living skills, affirmative industries, dual diagnosis treatment, individual and family psychoeducation, adult day care, foster care, family services and mental health counseling.

Pine Rest Christian Mental Health Services is a psychiatric hospital and behavioral health provider, with the main treatment campus located in Gaines Township, Michigan. The Chief Executive Officer and President is Dr. Mark Eastburg, appointed December, 2006.
Experience Focussed Counselling (EFC) is a normalising, non-pathologizing approach to counselling or psychosocial support/accompaniment aimed particularly, but not exclusively, at persons who may be distressed by experiences such as hearing voices aka auditory hallucinations, visions or other phenomena which are commonly associated with diagnoses such as schizophrenia and other mental disorders.(Schnackenberg & Burr, 2017)
Community mental health services (CMHS), also known as community mental health teams (CMHT) in the United Kingdom, support or treat people with mental disorders in a domiciliary setting, instead of a psychiatric hospital (asylum). The array of community mental health services vary depending on the country in which the services are provided. It refers to a system of care in which the patient's community, not a specific facility such as a hospital, is the primary provider of care for people with a mental illness. The goal of community mental health services often includes much more than simply providing outpatient psychiatric treatment.
Supportive psychotherapy is a psychotherapeutic approach that integrates various therapeutic schools such as psychodynamic and cognitive-behavioral, as well as interpersonal conceptual models and techniques.
The mainstay of management of borderline personality disorder is various forms of psychotherapy with medications being found to be of little use.
The primary care behavioral health (PCBH) consultation model is a psychological approach to population-based clinical health care that is simultaneously co-located, collaborative, and integrated within the primary care clinic. The goal of PCBH is to improve and promote overall health within the general population. This approach is important because approximately half of all patients in primary care present with psychiatric comorbidities, and 60% of psychiatric illness is treated in primary care.

In a study in Western societies, homeless people have a higher prevalence of mental illness when compared to the general population. They also are more likely to suffer from alcoholism and drug dependency. It is estimated that 20–25% of homeless people, compared with 6% of the non-homeless, have severe mental illness. Others estimate that up to one-third of the homeless have a mental illness. In January 2015, the most extensive survey ever undertaken found 564,708 people were homeless on a given night in the United States. Depending on the age group in question and how homelessness is defined, the consensus estimate as of 2014 was that, at minimum, 25% of the American homeless—140,000 individuals—were seriously mentally ill at any given point in time. 45% percent of the homeless—250,000 individuals—had any mental illness. More would be labeled homeless if these were annual counts rather than point-in-time counts. Being chronically homeless also means that people with mental illnesses are more likely to experience catastrophic health crises requiring medical intervention or resulting in institutionalization within the criminal justice system. Majority of the homeless population do not have a mental illness. Although there is no correlation between homelessness and mental health, those who are dealing with homelessness are struggling with psychological and emotional distress. The Substance Abuse and Mental Health Services Administration conducted a study and found that in 2010, 26.2 percent of sheltered homeless people had a severe mental illness.
Substance use disorders (SUD) can have a significant effect on one's function in all areas of occupation. Physical and psychosocial issues due to SUD can impact occupational performance. Unfulfilled life roles and disruption in meaningful activity can result from lack of structure or routine, poor motivation, limited skills, and poor social networks. These deficits may also contribute to stress, affecting the ability to cope with challenges. While SUD can affect a client's participation in therapy and ability to follow recommendations, occupational therapists are trained to facilitate occupational participation and performance.

Internet-based treatments for trauma survivors is a growing class of online treatments that allow for an individual who has experienced trauma to seek and receive treatment without needing to attend psychotherapy in person. The progressive movement to online resources and the need for more accessible mental health services has given rise to the creation of online-based interventions aimed to help those who have experienced traumatic events. Cognitive behavioral therapy (CBT) has shown to be particularly effective in the treatment of trauma-related disorders and adapting CBT to an online format has been shown to be as effective as in-person CBT in the treatment of trauma. Due to its positive outcomes, CBT-based internet treatment options for trauma survivors has been an expanding field in both research and clinical settings.
Sexual trauma therapy is medical and psychological interventions provided to survivors of sexual violence aiming to treat their physical injuries and cope with mental trauma caused by the event. Examples of sexual violence include any acts of unwanted sexual actions like sexual harassment, groping, rape, and circulation of sexual content without consent.
References
- ↑ "WHO | Countries in action for mental health". WHO. Archived from the original on January 9, 2008. Retrieved 2019-10-23.
- 1 2 "Interpersonal Psychotherapy". Psychologytoday.com. Retrieved 2019-11-21.
- 1 2 O'Donnell, Allison N.; Williams, Mark; Kilbourne, Amy M. (4 June 2013). "Overcoming Roadblocks: Current and Emerging Reimbursement Strategies for Integrated Mental Health Services in Primary Care". Journal of General Internal Medicine. 28 (12): 1667–1672. doi:10.1007/s11606-013-2496-z. ISSN 0884-8734. PMC 3832738 . PMID 23733375.
- 1 2 "Out-Of-Network, Out-Of-Pocket, Out-Of-Options: The Unfulfilled Promise Of Parity". NAMI.org. Retrieved 2019-11-21.
- ↑ "Behavioral Health Treatments and Services". samhsa.gov. 2020-04-21.
- 1 2 Jacobson, Sherri (January 18, 2019). "Psychodynamic Psychotherapy vs CBT: Which to Choose?". harleytherapy.co.uk.
- ↑ Chinman, Matthew; George, Preethy; Dougherty, Richard H.; Daniels, Allen S.; Ghose, Sushmita Shoma; Swift, Anita; Delphin-Rittmon, Miriam E. (2014-04-01). "Peer Support Services for Individuals With Serious Mental Illnesses: Assessing the Evidence". Psychiatric Services. 65 (4): 429–441. doi:10.1176/appi.ps.201300244. ISSN 1075-2730. PMID 24549400.
- 1 2 "Supportive Housing Helps Vulnerable People Live and Thrive in the Community". Center on Budget and Policy Priorities. 2016-05-31. Retrieved 2019-11-21.
- ↑ "Securing Stable Housing". NAMI.org. Retrieved 21 November 2019.
- ↑ McKay, Colleen; Nugent, Katie L.; Johnsen, Matthew; Eaton, William W.; Lidz, Charles W. (2018-01-01). "A Systematic Review of Evidence for the Clubhouse Model of Psychosocial Rehabilitation". Administration and Policy in Mental Health and Mental Health Services Research. 45 (1): 28–47. doi:10.1007/s10488-016-0760-3. ISSN 1573-3289. PMC 5756274 . PMID 27580614.
- ↑ "Mental Health Hotline | 24 Hour Psychiatric & Mental Illness Helpline". PsychGuides.com. Retrieved 2019-11-20.
- ↑ "About the Lifeline". suicidepreventionlifeline.org. Retrieved 2019-11-20.
- ↑ "About Drughelpline.org | Read About Our Mission & Cause" . Retrieved 2019-11-20.
- 1 2 Shaver, Julia (December 2022). "The State of Telehealth Before and After the COVID-19 Pandemic". Primary Care. 49 (4): 517–530. doi:10.1016/j.pop.2022.04.002. ISSN 0095-4543. PMC 9035352 . PMID 36357058.
- 1 2 3 4 5 6 "Worsening Faster Than It's Improving: The U.S. Mental Health Care Delivery System". Penn LDI. 2022-09-29. Retrieved 2024-03-18.
- 1 2 "Technology and the Future of Mental Health Treatment - National Institute of Mental Health (NIMH)". www.nimh.nih.gov. Retrieved 2024-03-19.
- 1 2 "The Ten Key Components of Mental Health Court" (PDF). mental-health-court.org/. Retrieved 2019-11-21.
- ↑ "LPS (Mental Health) Conservatorship - The Superior Court of California, County of Santa Clara". www.scscourt.org. Retrieved 2019-11-21.
- ↑ "Number of people with mental and substance use disorders". Our World in Data. Retrieved 2019-10-29.
- ↑ "Number with a mental or neurodevelopmental disorder by type". Our World in Data. Retrieved 2019-10-29.
- ↑ "Mental and substance use disorders as a share of total disease burden". Our World in Data. Retrieved 2019-10-29.
- ↑ Lancet Global Mental Health Group; Chisholm, D.; Flisher, A. J.; Lund, C.; Patel, V.; Saxena, S.; Thornicroft, G.; Tomlinson, M. (2007). "Scale up services for mental disorders: a call for action". The Lancet. 370 (9594): 1241–1252. doi:10.1016/S0140-6736(07)61242-2. PMID 17804059. S2CID 21045215.
- ↑ World Health Organization WHO urges more investments, services for mental health WHO website, September 2007
- ↑ "Payment by Results: mental health payments for 2013 to 2014". GOV.UK.
- ↑ "A quick guide to mental health payment by results and its impact on social work - 4/16/2013 - Community Care". www.communitycare.co.uk. Archived from the original on 2013-05-07.
- ↑ Nortje, Gareth; Oladeji, Bibilola; Gureje, Oye; Seedat, Soraya (2016-02-01). "Effectiveness of traditional healers in treating mental disorders: a systematic review". The Lancet Psychiatry. 3 (2): 154–170. doi:10.1016/S2215-0366(15)00515-5. ISSN 2215-0366. PMID 26851329.
- ↑ Que, Jianyu; Lu, Lin; Shi, Le (2019-02-01). "Development and challenges of mental health in China". General Psychiatry. 32 (1): e100053. doi:10.1136/gpsych-2019-100053. ISSN 2517-729X. PMC 6551437 . PMID 31179426.
- ↑ "Fast Facts about Mental Illness". CMHA National. Retrieved 2019-11-21.
- ↑ "The State of Mental Health in America". Mental Health America. Retrieved 2024-02-27.
- ↑ Silberner, Joanne (October 15, 2018). "Report:World Support For Mental Health Care Is 'Pitifully Small'". npr.org. Retrieved March 18, 2024.
- ↑ "Technology and the Future of Mental Health Treatment - National Institute of Mental Health (NIMH)". www.nimh.nih.gov. Retrieved 2024-03-19.