
Pain in the hip is the experience of pain in the muscles or joints in the hip/ pelvic region, a condition commonly arising from any of a number of factors. Sometimes it is closely associated with lower back pain.

Pain in the hip is the experience of pain in the muscles or joints in the hip/ pelvic region, a condition commonly arising from any of a number of factors. Sometimes it is closely associated with lower back pain.
Causes of pain around the hip joint may be intra-articular, extra-articular, or referred pain from neighboring structures, such as sacroiliac joint, spine, symphysis pubis, or the inguinal canal. [1]
Common etiologies include:
Pain in the groin, called anterior hip pain, is most often the result of osteoarthritis, osteonecrosis, occult fracture, acute synovitis, and septic arthritis; pain on the sides of the hip, called lateral hip pain, is usually caused by bursitis; pain in the buttock, called posterior or gluteal hip pain, which is the least common type of hip pain, is most often caused by sacroiliac joint dysfunction as well as sciatica (whether from a hemorrhaged spinal disk or a tense piriformis muscle). Herpes zoster (shingles) may also cause posterior hip pain.
Clinical tests are adapted to identify the source of pain as intra-articular or extra-articular. The flexion-abduction-external rotation (FABER), internal range of motion with overpressure (IROP), and scour tests show sensitivity values in identifying individuals with intra-articular pathology ranging from 0.62 to 0.91. [1]
Projectional radiography ("X-ray") is the first imaging technique of choice in hip pain, not only in older people with suspected osteoarthritis but also in young people without any such suspicion. In this case plain radiography allows categorization as normal hip or dysplastic hip, or with impingement signs, pincer, cam, or a combination of both. [1]
Imaging of the hip needs to be complementary to the clinical history and physical examination because it is well known that imaging findings do not always correlate with the presence of pain and vice versa. [1]
Projectional radiography ("X-ray") is currently useful not only in older people in whom osteoarthritis of the hip is suspected but also in younger people without osteoarthritis, who are being evaluated for femoroacetabular impingement (FAI) or hip dysplasia. [1]
Plain radiography allows us to categorize the hip as normal or dysplastic or with impingement signs (pincer, cam, or a combination of both). Besides these, pathologic processes like osteoarthritis, inflammatory diseases, infection, or tumors can also be identified (Figure 1). [1]
Figure 1.
X-ray of infants should be obtained with the pelvis in neutral position with the lower limbs held in neutral rotation and slight flexion.
Despite the widespread of ultrasound, pelvis X-ray is still frequently used to diagnose and/or monitor hip dysplasia or for assessing other congenital conditions or bone tumors. [1]
The most useful lines and angles that can be drawn in the pediatric pelvis assessing DDH are as follows: [1]
Most cases of Legg-Calvé-Perthes disease (LCPD) develop between the ages of 4 and 10 years (Figure 3). Classification of its severity can be assessed by radiographs. Herring or lateral pillar classifications and the patient’s age strongly correlate with the outcome.

In Group A, which has a better prognosis, there are no loss of height in the lateral third of the femoral head and little density changes; in Group B, there is lucency and lateral height loss of less than 50%; and in Group C, the most severe form, there is more than 50% loss of lateral height. Group B/C is considered when the loss of lateral pillar height is at 50%. People who are over the age of 8 years at the time of onset and have a hip in the lateral pillar B group or B/C border group have a better outcome with surgical treatment than they do with conservative treatment. Group B hips in children who are less than 8 years at the time of onset have a very favorable outcome unrelated to the treatment, whereas Group C hips in children of all ages usually have poor outcome unrelated to the treatment. [1]
Slipped capital femoral epiphyses (SCFE) usually affect 11- to 14-year-old adolescents (Figure 4). Radiographs may show widening and irregularity of the physis and posterior inferior displacement of the capital femoral epiphysis. On the AP view Klein’s line, tangent to the lateral aspect of the femoral neck, does not intersect the femoral head indicating that it is displaced. SCFE may compromise the blood supply to the femoral head and cause avascular necrosis, mainly when there is instability between the fragments. [1]

Measurements of hip dysplasia in adults are quite different from those in children. [1]
In adults, one of the main indications for radiographs is the detection of osteoarthritic changes (Figure 1(e)). Nevertheless, radiographs usually detect advanced osteoarthritis that can be graded according to the Tönnis classifications. The grading system ranges from 0 to 3, where 0 shows no sign of osteoarthritis. Intermediate grade 1 shows mild sclerosis of the head and acetabulum, slight joint space narrowing, and marginal osteophyte lipping. Grade 2 presents with small cysts in the femoral head or acetabulum, moderate joint space narrowing, and moderate loss of sphericity of the femoral head. Grade 3 is the severest form of osteoarthritis, which manifests as severe narrowing of the joint space, large subchondral cyst with productive bone changes that may lead to deformity of the bone components of the joint, while secondary osteoarthritis due to calcium pyrophosphate deposition can be diagnosed when calcification of hyaline cartilage and fibrocartilage is detected. [1]
There are other pathological conditions that can affect the hip joint and radiographs help to make the appropriate diagnosis. Acute bacterial septic arthritis can be diagnosed by radiographs when a fast regional osteoporosis and destructive monoarticular process develops (Figure 1(f)). In case of tuberculous or brucella arthritis it is manifested as a slow progressive process, and diagnosis may be delayed. [1]
Synovial chondromatosis can be confidently diagnosed by X-ray when calcified cartilaginous chondromas are seen. However, other synovial proliferative processes, such as pigmented villonodular synovitis, require MRI for accurate diagnosis, although noncalcified synovitis can be suspected in radiographs by indirect signs, such as soft tissue swelling and/or erosions in the femoral head, femoral neck, or acetabulum (Figure 7). [1]
Figure 7:
Radiological signs of transient osteoporosis of the hip include localized osteoporosis of the femoral head and neck (Figure 8). Nevertheless, final diagnosis has to be made with MRI to differentiate it from avascular necrosis and from insufficiency or stress fractures of the femoral head or neck. In case of AVN, radiographs can only demonstrate delayed or advanced signs. Staging according to Ficat classification ranges between normal appearance (stage I), slight increased density in the femoral head (stage II), subchondral collapse of the femoral head with or without “crescent” sign (stage III), and advanced collapse with secondary osteoarthritis (stage IV). In the case of stress or insufficiency fractures X-ray sensitivity has been proven to be much lower than MRI, which is currently the gold standard. [1]
Figure 8:
Many pathological conditions of the hip are detected early by MRI due to its high soft tissue resolution and sensitivity. Its accuracy in studying acute hip pain in children has proved to be superior to ultrasound and plan film radiography. However, MRI accessibility and the need of sedation relegate its use to selected cases in which diagnosis is not clear with less demanding techniques. These include differentiating transient synovitis from a septic arthritis or osteomyelitis, diagnosis of inflammatory joint disease or bone tumors, and early detection and follow-up of Perthes disease. [1]
MRI findings correlate with prognosis in LCPD. These include extent and distribution of epiphyseal necrosis, subchondral ossified nucleus fracture, involvement of the lateral pillar, and disturbance of physeal growth, including presence of transphyseal neovascularity or bridging. [1]
Recent studies have been focused on the role of diffusion weighted MRI because it does not need contrast medium administration. ADC ratio of the femoral metaphysis was positively correlated with the Herring classification. ADC ratio superior to 1.63 indicates bad prognosis with 89% sensitivity and 58% specificity. [1]
In adults, MRI is currently playing a definite role in the assessment of osteoarthritis. Although traditionally belonging to the arena of radiographs, the role of MRI has been stressed after the term femoral acetabular impingement was coined in 2003. Growing interest has been focused in accurate diagnosis of the acetabular and femoral morphological abnormalities that may lead to early osteoarthritis. [1]
MR imaging is considered paramount to these objectives, mainly when surgery is considered, due to the ability of MRI to portray the whole section of the femoral neck surface, as well as to image the labrum and articular cartilage. [1]
Diagnosis of impingement can only be achieved if, besides imaging findings, there are also clinical symptoms and positive impingement maneuvers. [1]
Most of the angles and measurements described in the plain radiograph section can be accurately reproduced on MRI. In addition, the superiority of MRI resolution with intra-articular contrast allows detection of labral and chondral abnormalities that may influence the choice of medical, percutaneous, or surgical management (Figure 9). [1]
Figure 9:
MR arthrography has proven superior in accuracy when compared to native MR imaging. It is considered the best technique to assess the labrum. Knowledge of the normal variable morphology of the labrum helps to differentiate tears from normal variants. A triangular shape is most commonly seen in 66% of asymptomatic volunteers, but round, flattened, and absent labra can also be found in asymptomatic populations. MR arthrography has demonstrated sensitivity over 90% and specificity close to 100% in detecting labral tears. Loose bodies are demonstrated as filling defects surrounded by the hyperintense gadolinium. [1]
Association between labral tears and chondral damage has been demonstrated. This underscores the interaction between cartilage and labrum damage in the progression of osteoarthritis. Chondral damage to the posteroinferior part of the acetabulum as a contrecoup lesion occurs in approximately one-third of pincer cases secondary to persistent abutment on the anterior part of the joint leading to a slight posteroinferior subluxation. This is considered a bad prognosis sign. [1]
MR arthrography can also demonstrate ligamentum teres rupture or capsular laxity, which are debated causes of microinstability of the hip. Elongation of the capsule or injury to the iliofemoral ligament or labrum may be secondary to microtrauma in athletes. MR can demonstrate abnormalities in these cases, such as increased joint volume or a ligamentum teres tear (Figure 9). [1]
Intra-articular osseous causes of pain include several conditions: avascular necrosis (AVN), transient osteoporosis of the hip (TOH), tumors, and stress or insufficiency fractures. All these entities may present with a pattern of bone marrow edema characterized by decreased signal intensity on T1 weighted images and increased signal intensity on fluid sensitive sequences, such as fat saturated T2-weighted or STIR images. When there is no evidence of a focal lesion associated with the edema pattern, TOH is suspected. When a band of low intensity is seen inside the edematous area, the shape and length of this band become important. It is generally convex to the articular surface in the case of subchondral stress or insufficiency fractures, whereas it is concave, circumscribing all of the necrotic segment, in cases of AVN. When doubts do persist, gadolinium-enhanced MRI tends to show that the proximal portion beyond the band is enhanced in fractures but is not in AVN. [1]
MRI has been shown to have 100% sensitivity and specificity in prospective studies of occult hip fractures. These fractures were diagnosed by bone marrow edema and a low signal fracture line, mainly on T1 or T2 weighted images (Figure 10). [1]
Figure 10:
In synovial proliferative disorders, MRI demonstrates synovial hypertrophy. In the case of PVNS, characteristic foci of low signal intensity related to hemosiderin deposition are better seen on gradient echo T2* images (Figure 7). In the case of synovial osteochondromatosis, the synovial hypertrophy is accompanied by intermediate signal cartilaginous loose bodies and/or low signal calcified loose bodies. [1]
Due to radiation concerns, CT has been relegated after MRI in the study of intra-articular causes of hip pain. The only exception where CT is considered superior to MRI is in bone tumors, because of its ability in characterizing matrix calcifications, and in depicting the anatomy of acute traumatic fractures. Typical matrix calcifications include the following: (a) osteoid mineralization, like a dense cloud, (b) chondroid calcification, reproducing a punctate popcorn pattern, or (c) fibrous calcification, ground glass-like appearance. There are also tumors that typically do not show matrix calcification. CT is also used for accurate localization of the nidus in osteoid osteomas and this must be differentiated from Brodie’s abscess or a stress fracture. The current standard treatment of osteoid osteoma is percutaneous radiofrequency ablation and this is usually performed under CT guidance. [1]
Quite often, CT is widely available unlike MRI, especially in the acute setting. CT is performed in this setting when doubt about the existence of a fracture persists following plain radiograph. Modern multidetector computed tomography (MDCT) shows results comparable with MRI for detecting occult fractures. [1]
Due to the submillimeter resolution of MDCT arthrography, many authors consider this technique complementary to MR arthrography. It may even have superior sensitivity in detecting cartilage pathology, but lesser detecting labral tears. [1]
CT can also be used to obtain accurate measurement of the femoral version and torsion. The femoral version is measured by an angle formed between a line through the femoral head-neck axis and another horizontal line drawn between both ischial tuberosities. Normal values range between 5 and 25°. Retroversion is considered abnormal. [1]
Femoral torsion is the angle between a line along the femoral head and neck axis and a second line that is touching the posterior border of both femoral condyles. The normal value at birth is approximately 32° and decreases gradually with age. In adults, the normal value ranges from 10° to 20°. [1]
Ultrasound is the first-choice technique for diagnosis of newborns hip dysplasia. In experienced hands with appropriate technology, ultrasound can also be useful during the first year of life. Some European healthcare systems encourage universal ultrasound screening in neonates between the sixth and eighth weeks. Although it shows higher initial costs caused, it leads to significant reduction in the total number and overall costs of dysplastic hips undergoing operative and nonoperative treatment. [1]
Ultrasound allows categorizing pediatric hips, according to Graf’s criteria, in four main types: normal, immature, and dysplastic (subluxed and dislocated). This classification is based on measurements of the acetabular inclination angle (alpha), cartilage roof angle (beta), and infant age. The femoral head coverage can also be determined by dividing the length of the femoral head covered by the acetabular fossa and the diameter of the femoral head. Its lower normal limits are 47% for boys and 44% for girls (Figure 11). [1]
Figure 11:
In a recent study, including newborns with high clinical suspicion for DDH (Ortolani/Barlow test, asymmetry in abduction of 20° or greater, breech presentation, leg-length discrepancy, and first-degree relative treated for DDH), hip sonography led to a change in clinical diagnosis in 52% of hips and to a change in management plan in 32% of hips. It obviated further follow-up in 23%, strengthening its role as an important technique reassuring the clinical diagnosis. [1]
During childhood, ultrasound is a quick method to assess hip pain and quite often may be used to avoid use of irradiating techniques, such as radiography or CT. Ultrasound allows evaluation of joint effusion, synovial thickening and neovascularity, the bone/cartilage contour, and the femoral head-neck alignment. Although sonography is extremely sensitive in detecting increased synovial fluid, it is nonspecific and cannot be used with accuracy to determine the type of fluid. Transient synovitis of the hip, despite being the most frequent cause of pain in children between 3 and 10 years, remains a diagnosis of exclusion. It usually shows anechoic fluid, but echogenic fluid can also be found. The effusion is considered pathologic when it is measured at >2 mm in thickness. The differential diagnosis is wide, including osteomyelitis, septic arthritis, primary or metastatic lesions, LCPD, and SCFE. Discrimination from septic arthritis is challenging, often requiring joint aspiration. In septic arthritis, US is able to demonstrate a hip joint effusion, synovial thickening, and cartilage damage, although the appearances are nonspecific. [1]
A step between the head and the physis can be detected in children with SCFE, while abnormalities in the femoral head contour may suggest the presence of LCPD. In both cases, radiographs are mandatory to confirm diagnosis and severity (Figure 12). [1]
Figure 12:
In adults, the most common application for US is to detect tendon or muscle injuries, effusion or synovitis within the hip joint or its adjacent bursae. Joint effusions may be due to many intra-articular processes and this may need another imaging technique to achieve a specific diagnosis. [1]
Bone scanning in people with hip pain can be complementary to other imaging studies, mainly in indeterminate bone lesions to clarify whether it is an active lesion with abnormal radiotracer accumulation. Nevertheless, MRI has replaced scintigraphy in the diagnosis of most of these conditions. An example is stress or insufficiency fractures: increased uptake is usually present in around 80% of fractures within 24 h, and 95% of fractures reveal activity by 72 h following trauma, showing an overall sensitivity of 93% and specificity of 95%. MRI is superior to bone scans in terms of sensitivity (99%-100%) and specificity (100%). Moreover, a bone scan does not provide detailed anatomical location of the fracture, and further imaging is usually required. [1]
Dry needling for hip pain and its integration with physical therapy is gaining popularity as a therapeutic approach for various musculoskeletal issues.
Research studies extensively delve into the effectiveness of dry needling in alleviating hip pain, particularly targeting myofascial trigger points and taut bands. Various trials highlight its positive impact on pain reduction, improved muscle strength, and enhanced physical function, especially in patients dealing with hip osteoarthritis. [2]
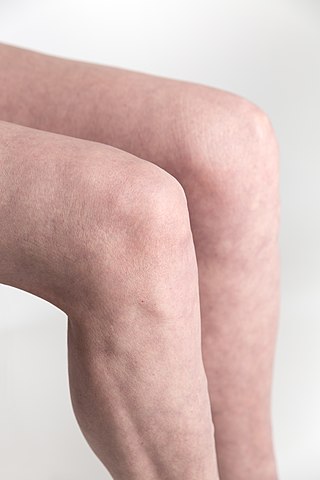
In humans and other primates, the knee joins the thigh with the leg and consists of two joints: one between the femur and tibia, and one between the femur and patella. It is the largest joint in the human body. The knee is a modified hinge joint, which permits flexion and extension as well as slight internal and external rotation. The knee is vulnerable to injury and to the development of osteoarthritis.
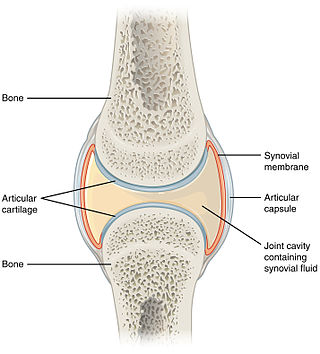
A synovial joint, also known as diarthrosis, joins bones or cartilage with a fibrous joint capsule that is continuous with the periosteum of the joined bones, constitutes the outer boundary of a synovial cavity, and surrounds the bones' articulating surfaces. This joint unites long bones and permits free bone movement and greater mobility. The synovial cavity/joint is filled with synovial fluid. The joint capsule is made up of an outer layer of fibrous membrane, which keeps the bones together structurally, and an inner layer, the synovial membrane, which seals in the synovial fluid.

A limp is a type of asymmetric abnormality of the gait. Limping may be caused by pain, weakness, neuromuscular imbalance, or a skeletal deformity. The most common underlying cause of a painful limp is physical trauma; however, in the absence of trauma, other serious causes, such as septic arthritis or slipped capital femoral epiphysis, may be present. The diagnostic approach involves ruling out potentially serious causes via the use of X-rays, blood tests, and sometimes joint aspiration. Initial treatment involves pain management. A limp is the presenting problem in about 4% of children who visit hospital emergency departments.
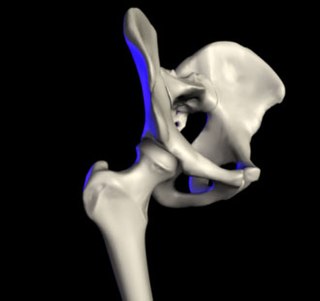
In vertebrate anatomy, the hip, or coxa(pl.: coxae) in medical terminology, refers to either an anatomical region or a joint on the outer (lateral) side of the pelvis.

Synovial osteochondromatosis (SOC) (synonyms include synovial chondromatosis, primary synovial chondromatosis, synovial chondrometaplasia) is a rare disease that creates a benign change or proliferation in the synovium or joint-lining tissue, which changes to form bone-forming cartilage. In most occurrences, there is only one joint affected, either the knee, the hip, or the elbow. Rarely involves the TMJ.

Calcium pyrophosphate dihydrate (CPPD) crystal deposition disease, also known as pseudogout and pyrophosphate arthropathy, is a rheumatologic disease which is thought to be secondary to abnormal accumulation of calcium pyrophosphate dihydrate crystals within joint soft tissues. The knee joint is most commonly affected. The disease is metabolic in origin and its treatment remains symptomatic.

Synovitis is the medical term for inflammation of the synovial membrane. This membrane lines joints that possess cavities, known as synovial joints. The condition is usually painful, particularly when the joint is moved. The joint usually swells due to synovial fluid collection.
PennHIP is a program which evaluates the quality of the hips in dogs. The program was established at the University of Pennsylvania School of Veterinary Medicine by Gail Smith in 1993, with the primary objective of reducing the prevalence of hip dysplasia in dogs. To assess a dog's hip joints, three radiographs (X-rays) are taken from different angles while the dog is under general anesthesia. Radiographs are submitted to the PennHIP for assessment, and are assigned a score, called a distraction index. Veterinarians must be trained members of the PennHIP Network in order to take radiographs for these assessments. The scheme is available through veterinarians in the United States and Canada. It was considered as the most evidence-based radiographic method to diagnose hip dysplasia.

Synovial chondromatosis is a locally aggressive bone tumor of the cartilaginous type. It consists of several hyaline cartilaginous nodules and has the potential of becoming cancerous.

Transient synovitis of hip is a self-limiting condition in which there is an inflammation of the inner lining of the capsule of the hip joint. The term irritable hip refers to the syndrome of acute hip pain, joint stiffness, limp or non-weightbearing, indicative of an underlying condition such as transient synovitis or orthopedic infections. In everyday clinical practice however, irritable hip is commonly used as a synonym for transient synovitis. It should not be confused with sciatica, a condition describing hip and lower back pain much more common to adults than transient synovitis but with similar signs and symptoms.

Orthopedic pathology, also known as bone pathology is a subspecialty of surgical pathology which deals with the diagnosis and feature of many bone diseases, specifically studying the cause and effects of disorders of the musculoskeletal system. It uses gross and microscopic findings along with the findings of in vivo radiological studies, and occasionally, specimen radiographs to diagnose diseases of the bones.
Lameness is an abnormal gait or stance of an animal that is the result of dysfunction of the locomotor system. In the horse, it is most commonly caused by pain, but can be due to neurologic or mechanical dysfunction. Lameness is a common veterinary problem in racehorses, sport horses, and pleasure horses. It is one of the most costly health problems for the equine industry, both monetarily for the cost of diagnosis and treatment, and for the cost of time off resulting in loss-of-use.
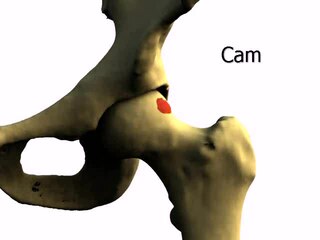
Femoroacetabular impingement (FAI) is a condition involving one or more anatomical abnormalities of the hip joint, which is a ball and socket joint. It is a common cause of hip pain and discomfort in young and middle-aged adults. It occurs when the ball shaped femoral head contacts the acetabulum abnormally or does not permit a normal range of motion in the acetabular socket. Damage can occur to the articular cartilage, or labral cartilage, or both. The condition may be symptomatic or asymptomatic. It may cause osteoarthritis of the hip. Treatment options range from conservative management to surgery.
Milwaukee shoulder syndrome (MSS) (apatite-associated destructive arthritis/Basic calcium phosphate (BCP) crystal arthritis/rapid destructive arthritis of the shoulder is a rare rheumatological condition similar to pseudogout, associated with periarticular or intra-articular deposition of hydroxyapatite or basic calcium phosphate (BCP) crystals. While primarily associated with the shoulder joint, it can affect any joint in the body below the head. Along with symptomatology, the disease typically presents with positive radiologic findings, often showing marked erosion of the humeral head, cartilage, capsule, and bursae. Though rare, it is most often seen in females beginning in their 50s or 60s. Patients often have a history of joint trauma or overuse, calcium pyrophosphate dehydrate crystal deposition, neuroarthropathy, dialysis-related arthropathy or denervation.

Orthopedic surgery is the branch of surgery concerned with conditions involving the musculoskeletal system. Orthopedic surgeons use both surgical and nonsurgical means to treat musculoskeletal injuries, sports injuries, degenerative diseases, infections, bone tumours, and congenital limb deformities. Trauma surgery and traumatology is a sub-specialty dealing with the operative management of fractures, major trauma and the multiply-injured patient.
An occult fracture is a fracture that is not readily visible, generally in regard to projectional radiography ("X-ray"). Radiographically, occult and subtle fractures are a diagnostic challenge. They may be divided into 1) high energy trauma fracture, 2) fatigue fracture from cyclical and sustained mechanical stress, and 3) insufficiency fracture occurring in weakened bone. Independently of the cause, the initial radiographic examination can be negative either because the findings seem normal or are too subtle. Advanced imaging tools such as computed tomography, magnetic resonance imaging (MRI), and scintigraphy are highly valuable in the early detection of these fractures.
X-rays of hip dysplasia are one of the two main methods of medical imaging to diagnose hip dysplasia, the other one being medical ultrasonography. Ultrasound imaging yields better results defining the anatomy until the cartilage is ossified. When the infant is around 3 months old a clear roentgenographic image can be achieved. Unfortunately the time the joint gives a good x-ray image is also the point at which nonsurgical treatment methods cease to give good results.

Ultrasound-guided hip joint injection is a joint injection in the hip, assisted by medical ultrasound. Hip and groin pain often presents a diagnostic and therapeutic challenge. The differential diagnosis is extensive, comprising intra-articular and extra-articular pathology and referred pain from lumbar spine, knee and elsewhere in the pelvis. Various ultrasound-guided techniques have been described in the hip and groin region for diagnostic and therapeutic purposes. Ultrasound has many advantages over other imaging modalities, including portability, lack of ionizing radiation and real-time visualization of soft tissues and neurovascular structures. Many studies have demonstrated the safety, accuracy and efficacy of ultrasound-guided techniques, although there is lack of standardization regarding the injectates used and long-term benefit remains uncertain.

Trabecular edema, also known as bone marrow edema (BME), is a traditional term describing the interstitial fluid accumulation at the trabecular bone marrow. The term was first used in 1988, referring to the changes in the bone marrow due to inflammation. Bone marrow edema was later renamed to bone marrow lesion (BML), as later studies show that the increased fluid content in the trabecular bone was more likely caused by inflammatory responses instead of fluid influx. Hence, this narrows down the condition to the damage at the articular surface of the trabecular bones. Despite so, the terms BME and BML are still used interchangeably in radiology.
Radiosynoviorthesis (RSO) is a minimally invasive therapeutic procedure for managing joint inflammation, particularly synovitis associated with osteoarthritis. Radiosynoviorthesis involves the intra-articular injection of radioactive isotopes to specifically treat the inflamed synovial membrane. Synovitis, a hallmark of various joint disorders, including osteoarthritis, manifests as inflammation within the synovial membrane lining the joints. RSO aims to suppress overactive macrophage and synovial cells responsible for the inflammatory response, providing relief from pain and improving joint functionality.