Related Research Articles

Shock is the state of insufficient blood flow to the tissues of the body as a result of problems with the circulatory system. Initial symptoms of shock may include weakness, fast heart rate, fast breathing, sweating, anxiety, and increased thirst. This may be followed by confusion, unconsciousness, or cardiac arrest, as complications worsen.

The autonomic nervous system (ANS), formerly the vegetative nervous system, is a division of the peripheral nervous system that supplies smooth muscle and glands, and thus influences the function of internal organs. The autonomic nervous system is a control system that acts largely unconsciously and regulates bodily functions, such as the heart rate, digestion, respiratory rate, pupillary response, urination, and sexual arousal. This system is the primary mechanism in control of the fight-or-flight response.
The diving reflex, also known as the diving response and mammalian diving reflex, is a set of physiological responses to immersion that overrides the basic homeostatic reflexes, and is found in all air-breathing vertebrates studied to date. It optimizes respiration by preferentially distributing oxygen stores to the heart and brain, enabling submersion for an extended time.

Intracranial pressure (ICP) is the pressure exerted by fluids such as cerebrospinal fluid (CSF) inside the skull and on the brain tissue. ICP is measured in millimeters of mercury (mmHg) and, at rest, is normally 7–15 mmHg for a supine adult. The body has various mechanisms by which it keeps the ICP stable, with CSF pressures varying by about 1 mmHg in normal adults through shifts in production and absorption of CSF.
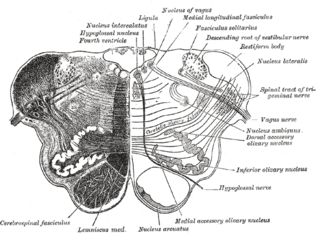
The nucleus ambiguus is a group of large motor neurons, situated deep in the medullary reticular formation named by Jacob Clarke. The nucleus ambiguus contains the cell bodies of neurons that innervate the muscles of the soft palate, pharynx, and larynx which are associated with speech and swallowing. As well as motor neurons, the nucleus ambiguus contains preganglionic parasympathetic neurons which innervate postganglionic parasympathetic neurons in the heart.

A cardiac stress test is a cardiological test that measures the heart's ability to respond to external stress in a controlled clinical environment. The stress response is induced by exercise or by intravenous pharmacological stimulation.

Cerebral circulation is the movement of blood through a network of cerebral arteries and veins supplying the brain. The rate of cerebral blood flow in an adult human is typically 750 milliliters per minute, or about 15% of cardiac output. Arteries deliver oxygenated blood, glucose and other nutrients to the brain. Veins carry "used or spent" blood back to the heart, to remove carbon dioxide, lactic acid, and other metabolic products.
Hypovolemic shock is a medical emergency and an advanced form of hypovolemia due to insufficient amounts of blood and/or fluid inside the human body to let the heart pump enough blood to the body. More specifically, hypovolemic shock occurs when there is decreased intravascular volume to the point of cardiovascular compromise. The hypovolemic shock could be due to severe dehydration through a variety of mechanisms or from blood loss.
Cushing reflex is a physiological nervous system response to increased intracranial pressure (ICP) that results in Cushing's triad of increased blood pressure, irregular breathing, and bradycardia. It is usually seen in the terminal stages of acute head injury and may indicate imminent brain herniation. It can also be seen after the intravenous administration of epinephrine and similar drugs. It was first described in detail by American neurosurgeon Harvey Cushing in 1901.
The baroreflex or baroreceptor reflex is one of the body's homeostatic mechanisms that helps to maintain blood pressure at nearly constant levels. The baroreflex provides a rapid negative feedback loop in which an elevated blood pressure reflexively causes the heart rate to decrease and also causes blood pressure to decrease. Decreased blood pressure decreases baroreflex activation and causes heart rate to increase and to restore blood pressure levels. The baroreflex can begin to act in less than the duration of a cardiac cycle and thus baroreflex adjustments are key factors in dealing with postural hypotension, the tendency for blood pressure to decrease on standing due to gravity.

Cardiogenic shock (CS) is a medical emergency resulting from inadequate blood flow due to the dysfunction of the ventricles of the heart. Signs of inadequate blood flow include low urine production, cool arms and legs, and altered level of consciousness. People may also have a severely low blood pressure and heart rate.
Hypoxemia is an abnormally low level of oxygen in the blood. More specifically, it is oxygen deficiency in arterial blood. Hypoxemia has many causes, and often causes hypoxia as the blood is not supplying enough oxygen to the tissues of the body.
Pulsus paradoxus, also paradoxic pulse or paradoxical pulse, is an abnormally large decrease in stroke volume, systolic blood pressure and pulse wave amplitude during inspiration. The normal fall in pressure is less than 10 mmHg. When the drop is more than 10 mmHg, it is referred to as pulsus paradoxus. Pulsus paradoxus is not related to pulse rate or heart rate, and it is not a paradoxical rise in systolic pressure. The normal variation of blood pressure during breathing/respiration is a decline in blood pressure during inhalation and an increase during exhalation. Pulsus paradoxus is a sign that is indicative of several conditions, including cardiac tamponade, chronic sleep apnea, croup, and obstructive lung disease.
Cardiorespiratory fitness (CRF) refers to the ability of the circulatory and respiratory systems to supply oxygen to skeletal muscles during sustained physical activity. The primary measure of CRF is VO2 max. In 2016, the American Heart Association published an official scientific statement advocating that CRF be categorized as a clinical vital sign and should be routinely assessed as part of clinical practice.
The Bainbridge reflex, also called the atrial reflex, is an increase in heart rate due to an increase in central venous pressure. Increased blood volume is detected by stretch receptors located in both sides of atria at the venoatrial junctions.
Autoregulation is a process within many biological systems, resulting from an internal adaptive mechanism that works to adjust that system's response to stimuli. While most systems of the body show some degree of autoregulation, it is most clearly observed in the kidney, the heart, and the brain. Perfusion of these organs is essential for life, and through autoregulation the body can divert blood where it is most needed.
Central chemoreceptors of the central nervous system, located on the ventrolateral medullary surface in the vicinity of the exit of the 9th and 10th cranial nerves, are sensitive to the pH of their environment.
Reflex bradycardia is a bradycardia in response to the baroreceptor reflex, one of the body's homeostatic mechanisms for preventing abnormal increases in blood pressure. In the presence of high mean arterial pressure, the baroreceptor reflex produces a reflex bradycardia as a method of decreasing blood pressure by decreasing cardiac output.
The vasomotor center (VMC) is a portion of the medulla oblongata. Together with the cardiovascular center and respiratory center, it regulates blood pressure. It also has a more minor role in other homeostatic processes. Upon increase in carbon dioxide level at central chemoreceptors, it stimulates the sympathetic system to constrict vessels. This is opposite to carbon dioxide in tissues causing vasodilatation, especially in the brain. Cranial nerves IX and X both feed into the vasomotor centre and are themselves involved in the regulation of blood pressure.
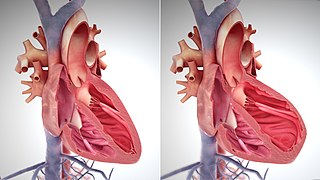
The main pathophysiology of heart failure is a reduction in the efficiency of the heart muscle, through damage or overloading. As such, it can be caused by a wide number of conditions, including myocardial infarction, hypertension and amyloidosis. Over time these increases in workload will produce changes to the heart itself:
References
- ↑ Saladin, Kenneth S. Anatomy and Physiology, The Unity of Form and Function. v4. McGraw-Hill. NY, 2007. (767)