Related Research Articles
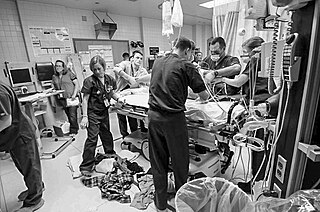
Emergency medicine is the medical speciality concerned with the care of illnesses or injuries requiring immediate medical attention. Emergency physicians specialise in providing care for unscheduled and undifferentiated patients of all ages. As first-line providers, in coordination with emergency medical services, they are primarily responsible for initiating resuscitation and stabilization and performing the initial investigations and interventions necessary to diagnose and treat illnesses or injuries in the acute phase. Emergency medical physicians generally practise in hospital emergency departments, pre-hospital settings via emergency medical services, and intensive care units. Still, they may also work in primary care settings such as urgent care clinics.

Proposition 215, or the Compassionate Use Act of 1996, is a California law permitting the use of medical cannabis despite marijuana's lack of the normal Food and Drug Administration testing for safety and efficacy. It was enacted, on November 5, 1996, by means of the initiative process, and passed with 5,382,915 (55.6%) votes in favor and 4,301,960 (44.4%) against.
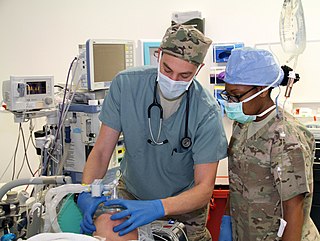
Anesthesiology, anaesthesiology, or anaesthesia is the medical specialty concerned with the total perioperative care of patients before, during and after surgery. It encompasses anesthesia, intensive care medicine, critical emergency medicine, and pain medicine. A physician specialized in anesthesiology is called an anesthesiologist, anaesthesiologist, or anaesthetist, depending on the country. In some countries, the terms are synonymous, while in other countries they refer to different positions, and anesthetist is only used for non-physicians, such as nurse anesthetists.

Kaiser Permanente is an American integrated managed care consortium, based in Oakland, California, United States, founded in 1945 by industrialist Henry J. Kaiser and physician Sidney Garfield. Kaiser Permanente is made up of three distinct but interdependent groups of entities: the Kaiser Foundation Health Plan, Inc. (KFHP) and its regional operating subsidiaries; Kaiser Foundation Hospitals; and the regional Permanente Medical Groups. As of 2023, Kaiser Permanente operates in eight states and the District of Columbia, and is the largest managed care organization in the United States.

The Supreme Court of California is the highest and final court of appeals in the courts of the U.S. state of California. It is headquartered in San Francisco at the Earl Warren Building, but it regularly holds sessions in Los Angeles and Sacramento. Its decisions are binding on all other California state courts. Since 1850, the court has issued many influential decisions in a variety of areas including torts, property, civil and constitutional rights, and criminal law.
A subpoena duces tecum, or subpoena for production of evidence, is a court summons ordering the recipient to appear before the court and produce documents or other tangible evidence for use at a hearing or trial. In some jurisdictions, it can also be issued by legislative bodies such as county boards of supervisors.
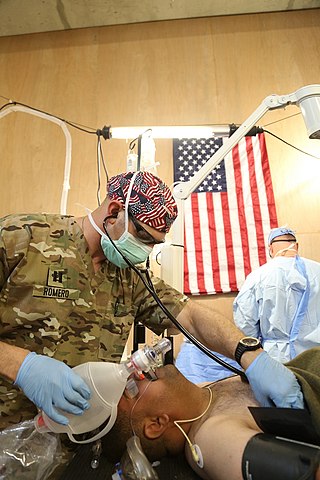
A nurse anesthetist is an advanced practice nurse who administers anesthesia for surgery or other medical procedures. They are involved in the administration of anesthesia in a majority of countries, with varying levels of autonomy.
Medical malpractice is professional negligence by act or omission by a health care provider in which the treatment provided falls below the accepted standard of practice in the medical community and causes injury or death to the patient, with most cases involving medical error. Claims of medical malpractice, when pursued in US courts, are processed as civil torts. Sometimes an act of medical malpractice will also constitute a criminal act, as in the case of the death of Michael Jackson.
The Lanterman–Petris–Short (LPS) Act regulates involuntary civil commitment to a mental health institution in the state of California. The act set the precedent for modern mental health commitment procedures in the United States. The bipartisan bill was co-authored by California State Assemblyman Frank D. Lanterman (R) and California State Senators Nicholas C. Petris (D) and Alan Short (D), and signed into law in 1967 by Governor Ronald Reagan. The Act went into full effect on July 1, 1972. It cited seven articles of intent:
Tarasoff v. Regents of the University of California, 17 Cal. 3d 425, 551 P.2d 334, 131 Cal. Rptr. 14, was a case in which the Supreme Court of California held that mental health professionals have a duty to protect individuals who are being threatened with bodily harm by a patient. The original 1974 decision mandated warning the threatened individual, but a 1976 rehearing of the case by the California Supreme Court called for a "duty to protect" the intended victim. The professional may discharge the duty in several ways, including notifying police, warning the intended victim, and/or taking other reasonable steps to protect the threatened individual.
New York State Department of Health Code, Section 405, also known as the Libby Zion Law, is a regulation that limits the amount of resident physicians' work in New York State hospitals to roughly 80 hours per week. The law was named after Libby Zion, who died in 1984 at the age of 18 under the care of what her father believed to be overworked resident physicians and intern physicians. In July 2003, the Accreditation Council for Graduate Medical Education adopted similar regulations for all accredited medical training institutions in the United States.
In the United States, anesthesia can be administered by physician anesthesiologists, an anesthesiologist assistant, or nurse anesthetist.
The Healthcare Quality Improvement Act of 1986 (HCQIA) was introduced by Congressman Ron Wyden from Oregon.
Pascack Valley Medical Center formerly known as Hackensack University Medical Center at Pascack Valley is a full-service boutique hospital located in Westwood, New Jersey, at the site of the former Pascack Valley Hospital. Owned 35% by Hackensack University Medical Center (HackensackUMC) and 65% by Ardent Health Services, HackensackUMC at Pascack Valley serves the Pascack Valley and Northern Valley communities in northern Bergen County. In 2021 it was given a grade A by the Leapfrog patient safety organization.

Landeros v. Flood was a 1976 court case in the state of California involving child abuse and alleged medical malpractice.
Clinical peer review, also known as medical peer review is the process by which health care professionals, including those in nursing and pharmacy, evaluate each other's clinical performance. A discipline-specific process may be referenced accordingly.
Certified anesthesiologist assistants (CAAs) are highly trained master’s degree level non-physician anesthesia care providers. CAAs are integral members of the anesthesia care team as described by the American Society of Anesthesiologists (ASA). This designation must be disambiguated from the Certified Clinical Anesthesia Assistant (CCAA) designation conferred by the Canadian Society of Respiratory Therapists. All CAAs possess a baccalaureate degree, and complete an intensive didactic and clinical program at a postgraduate level. CAAs are trained in the delivery and maintenance of all types of anesthesia care as well as advanced patient monitoring techniques. The goal of CAA education is to guide the transformation of student applicants into competent clinicians.

The Winkler County nurse whistleblower case was a series of legal proceedings in West Texas concerning the retaliation against two nurses who submitted an anonymous state medical board complaint against a physician in 2009. The case attracted national attention for its implications on whistleblowing by nurses.
TeamHealth is a physician practice in the U.S. founded in 1979 and based in Knoxville, Tennessee, pursuing medical outsourcing. Originally a provider of emergency department services, it is outsourcing physicians in emergency medicine, hospital medicine, anesthesiology, critical care, obstetrics, orthopedic surgery, general surgery, ambulatory care, post-acute care and medical call centers to approximately 2,900 acute and post-acute facilities nationwide. After numerous acquisitions in the 2010s it has become the largest market share in U.S. physician outsourcing. TeamHealth has affiliated partner companies, including D&Y Locum Tenens, Spectrum Healthcare Resources and AccessNurse.

Los Angeles County Medical Association (LACMA) is a professional organization representing physicians from every medical specialty and practice setting as well as students, interns and residents. The organization was founded in 1871 and is a constituent of the California Medical Association (CMA). It advocates quality care for all patients and provides services to meet the professional needs of its physician members. The group serves to represent its professional members in public policy, government relations, and community relations. LACMA, together with CMA physicians, strives to preserve and protect the noble pursuit of healthcare delivery.
References
- ↑ Roland Chalifoux, Jr (2005). "So What Is a Sham Peer Review?". Medscape General Medicine. 7 (4): 47. PMC 1681729 . PMID 16614669.
- 1 2 "Inappropriate Peer Review. Report of the Board of Trustees of the American Medical Association."
- ↑ "JCAHO Periodic Performance Review". Legal Bulletin of Oregon Association of Hospital and Health Systems. Archived from the original on September 28, 2007.
- ↑ Greg Abrams, Esq. (May–June 2006). "Attacking Bad Faith Peer Review: Is It a SLAPP?". Sierra Sacramento Valley Medicine. 57 (3). Archived from the original on 2011-07-21.
- ↑ Bruce Adornato, MD (March 2005). "Column by the President of the Medical Staff: Purple fingers, Purple toes". Stanford Hospital and Clinics Medical Staff Updates.
- ↑ Arnold MS (2000). ""Employment: Physician Not Protected From Termination For Advocating Medically Appropriate Health Care"—Khajavi v. Feather River Anesthesia Medical Group, 100 Cal. Rptr. 2d 627 (Cal. App. 3d 2000)". American Journal of Law & Medicine .
- ↑ California Appeals Court (October 10, 2000). "Khajavi v. Feather River Anesthesia Medical Group, Inc".
{{cite journal}}: Cite journal requires|journal=(help) - ↑ Mileikowsky v. Tenet Healthsystem (April 18, 2005) 128 Cal.App.4th 531, 27 Cal.Rptr.3d 171.
- ↑ "Health Policy in the Courts – California Medical Association's participation in Amicus Curiae Briefs – January 2007" (PDF). California Medical Association. January 2007.
- ↑ Mileikowsky v. West Hills Hosp. and Medical Center (2009) 45 Cal.4th 1259, 203 P.3d 1113, 91 Cal.Rptr.3d 516.
- ↑ Horvit M and Jarviss J, "Board revokes doctor's license," Fort Worth Star-Telegram (TX), 12 June 2004, p.1B
- ↑ Mitchell M, "Former Texas neurosurgeon granted licenses in West Virginia," Fort Worth Star-Telegram (TX), 7 July 2005
- ↑ Thevenot, C., "Jury awards $8.8 million to anesthesiologist," Las Vegas Review-Journal (NV), 26 May 2011, http://www.reviewjournal.com/news/crime-courts/jury-awards-88-million-anesthesiologist
- ↑ Chudacoff v. Univ. Med. Ctr. of S. Nev., 609 F.Supp. 2d 1163, 1172–73 (D. Nev. 2009)
- ↑ Chudacoff v. Univ. Med. Ctr. of S. Nev., 649 F.3d 1143 (9th Cir. 2011)
- ↑ William E. Fassett, PhD (2006). "Patient Safety Organizations". Ann Pharmacother. 40 (5): 917–924. Retrieved 2007-06-10.