Related Research Articles
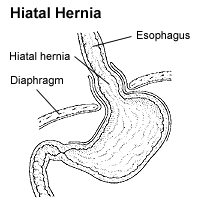
A hiatal hernia or hiatus hernia is a type of hernia in which abdominal organs slip through the diaphragm into the middle compartment of the chest. This may result in gastroesophageal reflux disease (GERD) or laryngopharyngeal reflux (LPR) with symptoms such as a taste of acid in the back of the mouth or heartburn. Other symptoms may include trouble swallowing and chest pains. Complications may include iron deficiency anemia, volvulus, or bowel obstruction.
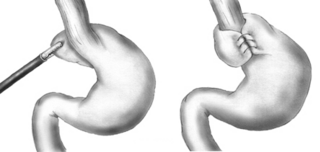
A Nissen fundoplication, or laparoscopic Nissen fundoplication when performed via laparoscopic surgery, is a surgical procedure to treat gastroesophageal reflux disease (GERD) and hiatal hernia. In GERD, it is usually performed when medical therapy has failed; but, with a Type II (paraesophageal) hiatus hernia, it is the first-line procedure. The Nissen fundoplication is total (360°), but partial fundoplications known as Thal, Belsey, Dor, Lind, and Toupet fundoplications are alternative procedures with somewhat different indications and outcomes.
Gastric bypass surgery refers to a technique in which the stomach is divided into a small upper pouch and a much larger lower "remnant" pouch and then the small intestine is rearranged to connect to both. Surgeons have developed several different ways to reconnect the intestine, thus leading to several different gastric bypass procedures (GBP). Any GBP leads to a marked reduction in the functional volume of the stomach, accompanied by an altered physiological and physical response to food.
The duodenal switch (DS) procedure, gastric reduction duodenal switch (GRDS), is a weight loss surgery procedure that is composed of a restrictive and a malabsorptive aspect.

A laparoscopic adjustable gastric band, commonly called a lap-band, A band, or LAGB, is an inflatable silicone device placed around the top portion of the stomach to treat obesity, intended to decrease food consumption.
Sleeve gastrectomy or vertical sleeve gastrectomy, is a surgical weight-loss procedure, typically performed laparoscopically, in which approximately 75 - 85% of the stomach is removed, along the greater curvature, which leaves a cylindrical, or "sleeve"-shaped stomach the size of a banana. Weight loss is affected not only through the reduction of the organ's size, but by the removal of the portion of it that produces ghrelin, the hormone that stimulates appetite. Patients can lose 50-70 percent of excess weight over the course of the two years that follow the surgery. The procedure is irreversible, though in some uncommon cases, patients can regain the lost weight, via resumption of poor dietary habits, or dilation of the stomach over time, which can require gastric sleeve revision surgery to either repair the sleeve or convert it to another type of weight loss method that may produce better results, such as a gastric bypass or duodenal switch.

A vagotomy is a surgical procedure that involves removing part of the vagus nerve. It is performed in the abdomen.

A bowel resection or enterectomy is a surgical procedure in which a part of an intestine (bowel) is removed, from either the small intestine or large intestine. Often the word enterectomy is reserved for the sense of small bowel resection, in distinction from colectomy, which covers the sense of large bowel resection. Bowel resection may be performed to treat gastrointestinal cancer, bowel ischemia, necrosis, or obstruction due to scar tissue, volvulus, and hernias. Some patients require ileostomy or colostomy after this procedure as alternative means of excretion. Complications of the procedure may include anastomotic leak or dehiscence, hernias, or adhesions causing partial or complete bowel obstruction. Depending on which part and how much of the intestines are removed, there may be digestive and metabolic challenges afterward, such as short bowel syndrome.
Bariatric surgery is a medical term for surgical procedures used to manage obesity and obesity-related conditions. Long term weight loss with bariatric surgery may be achieved through alteration of gut hormones, physical reduction of stomach size, reduction of nutrient absorption, or a combination of these. Standard of care procedures include Roux en-Y bypass, sleeve gastrectomy, and biliopancreatic diversion with duodenal switch, from which weight loss is largely achieved by altering gut hormone levels responsible for hunger and satiety, leading to a new hormonal weight set point.
StomaphyX is an endoscopic suturing system designed to treat patients who have had previous Roux-en-Y gastric bypass surgery. Following this surgery, the stomach pouch and stomach outlet (stoma) becomes enlarged in some patients. The StomaphyX device can be used to restrict the size of the stoma without exposing the patient to further surgical risk.
Jejunoileal bypass (JIB) was a surgical weight-loss procedure performed for the relief of morbid obesity from the 1950s through the 1970s in which all but 30 cm (12 in) to 45 cm (18 in) of the small bowel were detached and set to the side.
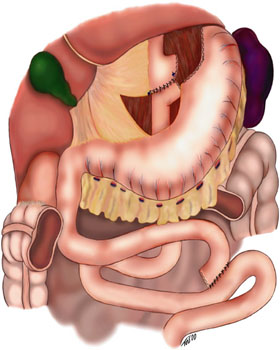
In general surgery, a Roux-en-Y anastomosis, or Roux-en-Y, is an end-to-side surgical anastomosis of bowel used to reconstruct the gastrointestinal tract. Typically, it is between stomach and small bowel that is distal from the cut end.
Revision weight loss surgery is a surgical procedure that is performed on patients who have already undergone a form of bariatric surgery, and have either had complications from such surgery or have not achieved significant weight loss results from the initial surgery. Procedures are usually performed laparoscopically, though open surgery may be required if prior bariatric surgery has resulted in extensive scarring.

Internal hernias occur when there is protrusion of an internal organ into a retroperitoneal fossa or a foramen in the abdominal cavity. If a loop of bowel passes through the mesenteric defect, that loop is at risk for incarceration, strangulation, or for becoming the lead point of a small bowel obstruction. Internal hernias can also trap adipose tissue (fat) and nerves. Unlike more common forms of hernias, the trapped tissue protrudes inward, rather than outward.

SADI-S is a bariatric surgical technique to address metabolic disorders and to lose weight. It is a variation on the Duodenal Switch surgery, incorporating a vertical sleeve gastrectomy with a gastric bypass technique.
I. Michael Leitman is an American surgeon and medical educator. He is Professor of Surgery and Medical Education and Dean for Graduate Medical Education at the Icahn School of Medicine at Mount Sinai. He previously held the position of Chairman of the Department of Surgery at Mount Sinai Beth Israel in New York City.
Stomach Intestinal Pylorus-Sparing (SIPS) surgery is a type of weight-loss surgery. It was developed in 2013 by two U.S. surgeons, Daniel Cottam from Utah and Mitchell S. Roslin from New York.
In medicine, endoscopic sleeve gastroplasty (ESG) is a minimally-invasive, non-surgical (incisionless), endoscopic weight loss procedure that is part of the field of endoscopic bariatric therapies. To perform ESG, a physician sutures a patient’s stomach into a narrower, smaller tube-like configuration. The result is a more restricted stomach that forces patients to feel fuller sooner, eating fewer calories, which facilitates weight loss.

Edward Eaton Mason was an American surgeon, professor, and medical researcher who specialized in obesity surgery. He is known for developing restrictive gastric surgery for morbidly obese patients. Mason introduced the first gastric bypass surgery in 1966 and was the inventor of the first vertical banded gastroplasty surgery in 1980.

Antrectomy, also called distal gastrectomy, is a type of gastric resection surgery that involves the removal of the stomach antrum to treat gastric diseases causing the damage, bleeding, or blockage of the stomach. This is performed using either the Billroth I (BI) or Billroth II (BII) reconstruction method. Quite often, antrectomy is used alongside vagotomy to maximise its safety and effectiveness. Modern antrectomies typically have a high success rate and low mortality rate, but the exact numbers depend on the specific conditions being treated.
References
- ↑ "jejunojejunostomy" – via The Free Dictionary.
- ↑ Lewis CE, Jensen C, Tejirian T, Dutson E, Mehran A (1 March 2009). "Early jejunojejunostomy obstruction after laparoscopic gastric bypass: case series and treatment algorithm". Surgery for Obesity and Related Diseases. 5 (2): 203–7. doi:10.1016/j.soard.2008.10.003. PMID 19136308.
- ↑ Kohli A, Gutnik L, Berman D, Narula A (7 December 2016). "Jejunojejunostomy intussusception after gastric bypass: Case report of a rare but serious complication". International Journal of Surgery Case Reports. 30: 101–102. doi:10.1016/j.ijscr.2016.10.068. PMC 5192243 . PMID 28006717.
- ↑ Sacks BC, Mattar SG, Qureshi FG, Eid GM, Collins JL, Barinas-Mitchell EJ, Schauer PR, Ramanathan RC (2006). "Incidence of marginal ulcers and the use of absorbable anastomotic sutures in laparoscopic Roux-en-Y gastric bypass". Surgery for Obesity and Related Diseases. American Society for Bariatric Surgery. 2 (1): 11–6. doi:10.1016/j.soard.2005.10.013. PMID 16925306.
Marginal ulceration is a known complication of both open and laparoscopic Roux-en-Y gastric bypass, with an incidence of approximately 1% to 16%; most recent studies cite an incidence of approximately 2%
- ↑ John S, Hoegerl C (November 2009). "Nutritional deficiencies after gastric bypass surgery". The Journal of the American Osteopathic Association. 109 (11): 601–4. doi:10.7556/jaoa.2009.109.11.601 (inactive 31 January 2024). PMID 19948694.
{{cite journal}}: CS1 maint: DOI inactive as of January 2024 (link)