Related Research Articles
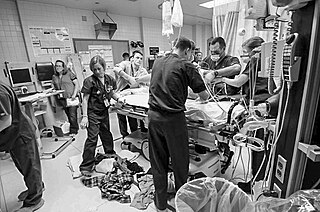
Emergency medicine is the medical speciality concerned with the care of illnesses or injuries requiring immediate medical attention. Emergency physicians specialize in providing care for unscheduled and undifferentiated patients of all ages. As first-line providers, in coordination with emergency medical services, they are primarily responsible for initiating resuscitation and stabilization and performing the initial investigations and interventions necessary to diagnose and treat illnesses or injuries in the acute phase. Emergency medical physicians generally practice in hospital emergency departments, pre-hospital settings via emergency medical services, and intensive care units. Still, they may also work in primary care settings such as urgent care clinics.
In the medical profession, a general practitioner (GP) or family physician is a physician who treats acute and chronic illnesses and provides preventive care and health education to patients of all ages. GPs' duties are not confined to specific fields of medicine, and they have particular skills in treating people with multiple health issues. They are trained to treat patients to levels of complexity that vary between countries. The term "primary care physician" is more usually used in the US. In Asian countries like India, this term has been replaced mainly by Medical Officers, Registered Medical Practitioner etc.
Internal medicine, also known as general internal medicine in Commonwealth nations, is a medical specialty for medical doctors focused on the prevention, diagnosis, and treatment of internal diseases in adults. Medical practitioners of internal medicine are referred to as internists, or physicians in Commonwealth nations. Internists possess specialized skills in managing patients with undifferentiated or multi-system disease processes. They provide care to both hospitalized (inpatient) and ambulatory (outpatient) patients and often contribute significantly to teaching and research. Internists are qualified physicians who have undergone postgraduate training in internal medicine, and should not be confused with "interns”, a term commonly used for a medical doctor who has obtained a medical degree but does not yet have a license to practice medicine unsupervised.
Palliative care is an interdisciplinary medical caregiving approach aimed at optimizing quality of life and mitigating suffering among people with serious, complex, and often terminal illnesses. Within the published literature, many definitions of palliative care exist. The World Health Organization (WHO) describes palliative care as "an approach that improves the quality of life of patients and their families facing the problems associated with life-threatening illness, through the prevention and relief of suffering by means of early identification and impeccable assessment and treatment of pain and other problems, physical, psychosocial, and spiritual". In the past, palliative care was a disease specific approach, but today the WHO takes a broader patient-centered approach that suggests that the principles of palliative care should be applied as early as possible to any chronic and ultimately fatal illness. This shift was important because if a disease-oriented approach is followed, the needs and preferences of the patient are not fully met and aspects of care, such as pain, quality of life, and social support, as well as spiritual and emotional needs, fail to be addressed. Rather, a patient-centered model prioritizes relief of suffering and tailors care to increase the quality of life for terminally ill patients.

Primary care is the day-to-day healthcare given by a health care provider. Typically this provider acts as the first contact and principal point of continuing care for patients within a healthcare system, and coordinates other specialist care that the patient may need. Patients commonly receive primary care from professionals such as a primary care physician, a physician assistant, a physical therapist, or a nurse practitioner. In some localities, such a professional may be a registered nurse, a pharmacist, a clinical officer, or an Ayurvedic or other traditional medicine professional. Depending on the nature of the health condition, patients may then be referred for secondary or tertiary care.
International emergency medicine is a subspecialty of emergency medicine that focuses not only on the global practice of emergency medicine but also on efforts to promote the growth of emergency care as a branch of medicine throughout the world. The term international emergency medicine generally refers to the transfer of skills and knowledge—including knowledge of ambulance operations and other aspects of prehospital care—from developed emergency medical systems (EMSs) to those systems which are less developed. However, this definition has been criticized as oxymoronic, given the international nature of medicine and the number of physicians working internationally. From this point of view, international emergency medicine is better described as the training required for and the reality of practicing the specialty outside of one's native country.

The American Academy of Family Physicians (AAFP) was founded in 1947 to promote and maintain high-quality standards for family medicine, an offshoot of the classical general practitioner. It is headquartered in Leawood, Kansas.
Health psychology is the study of psychological and behavioral processes in health, illness, and healthcare. The discipline is concerned with understanding how psychological, behavioral, and cultural factors contribute to physical health and illness. Psychological factors can affect health directly. For example, chronically occurring environmental stressors affecting the hypothalamic–pituitary–adrenal axis, cumulatively, can harm health. Behavioral factors can also affect a person's health. For example, certain behaviors can, over time, harm or enhance health. Health psychologists take a biopsychosocial approach. In other words, health psychologists understand health to be the product not only of biological processes but also of psychological, behavioral, and social processes.
A practice-based research network (PBRN) is a group of practices devoted principally to the care of patients and affiliated for the purpose of examining the health care processes that occur in practices. PBRNs are characterized by an organizational framework that transcends a single practice or study. They provide a "laboratory" for studying broad populations of patients and care providers in community-based settings.

A primary care physician (PCP) is a physician who provides both the first contact for a person with an undiagnosed health concern as well as continuing care of varied medical conditions, not limited by cause, organ system, or diagnosis. The term is primarily used in the United States. In the past, the equivalent term was 'general practitioner' in the US; however in the United Kingdom and other countries the term general practitioner is still used. With the advent of nurses as PCPs, the term PCP has also been expanded to denote primary care providers.
Behavioral medicine is concerned with the integration of knowledge in the biological, behavioral, psychological, and social sciences relevant to health and illness. These sciences include epidemiology, anthropology, sociology, psychology, physiology, pharmacology, nutrition, neuroanatomy, endocrinology, and immunology. The term is often used interchangeably, but incorrectly, with health psychology. The practice of behavioral medicine encompasses health psychology, but also includes applied psychophysiological therapies such as biofeedback, hypnosis, and bio-behavioral therapy of physical disorders, aspects of occupational therapy, rehabilitation medicine, and physiatry, as well as preventive medicine. In contrast, health psychology represents a stronger emphasis specifically on psychology's role in both behavioral medicine and behavioral health.

The Brody School of Medicine at East Carolina University (BSOM) is a public medical school located in Greenville, North Carolina, United States. It offers a Doctor of Medicine program, combined Doctor of Medicine / Master of Public Health and Doctor of Medicine / Master of Business Administration programs, and standalone Doctor of Philosophy and Master of Public Health programs. Brody is a national leader in family medicine, ranking No. 1 in North Carolina and No. 2 nationally in the percentage of graduates who choose careers in family medicine, based on the 2017 American Academy of Family Physicians report on MD-granting medical schools. Brody ranks in the top 10 percent of U.S. medical schools for graduating physicians who practice in the state, practice primary care and practice in rural and underserved areas. Brody graduates currently practice in 83 of North Carolina's 100 counties.
The medical home, also known as the patient-centered medical home (PCMH), is a team-based health care delivery model led by a health care provider to provide comprehensive and continuous medical care to patients with a goal to obtain maximal health outcomes. It is described in the "Joint Principles" as "an approach to providing comprehensive primary care for children, youth and adults."
Patient participation is a trend that arose in answer to medical paternalism. Informed consent is a process where patients make decisions informed by the advice of medical professionals.
Shared decision-making in medicine (SDM) is a process in which both the patient and physician contribute to the medical decision-making process and agree on treatment decisions. Health care providers explain treatments and alternatives to patients and help them choose the treatment option that best aligns with their preferences as well as their unique cultural and personal beliefs.
Guided Care is a model of proactive, comprehensive health care for people with several chronic conditions. A form of medical home, the model has been developed and tested by a multidisciplinary team of experts at the Roger C. Lipitz Center for Integrated Health Care in the Johns Hopkins Bloomberg School of Public Health. Guided Care is provided by physician-nurse teams in primary care practices to the physicians' most complex patients, mainly older adults with chronic conditions and complicated health needs. It is designed to increase patients' quality of care and quality of life, while improving the efficiency of their use of health care resources, thus reducing their overall health care costs.
The Improvement Science Research Network (ISRN) is a research network for academics and physicians who are conducting studies in the new medical field of improvement science.

David Bates is an American-born physician, biomedical informatician, and professor, who is internationally renowned for his work regarding the use of health information technology (HIT) to improve the safety and quality of healthcare, in particular by using clinical decision support. Bates has done work in the area of medication safety. He began by describing the epidemiology of harm caused by medications, first in hospitalized patients and then in other settings such as the home and nursing homes. Subsequently, he demonstrated that by implementing computerized physician order entry (CPOE), medication safety could be dramatically improved in hospitals. This work led the Leapfrog Group to call CPOE one of the four changes that would most improve the safety of U.S. healthcare. It also helped hospitals to justify investing in electronic health records and in particular, CPOE. Throughout his career, Bates has published over 600 peer reviewed articles and is the most cited researcher in the fields of both patient safety and biomedical informatics, with an h-index of 115. In a 2013 analysis published by the European Journal of Clinical Investigation, he ranked among the top 400 living biomedical researchers of any type. He is currently editor of the Journal of Patient Safety.

Neil S. Calman is a family physician and the president, CEO, and co-founder of the Institute for Family Health. He is the Chairman of the Department of Family Medicine & Community Health at the Icahn School of Medicine at Mount Sinai and the Board Chair of the Community Health Care Association of New York State.
Jacqueline Nwando Olayiwola is an American family physician, public health professional, author, professor, and women's empowerment leader. She is the Senior Vice President and Chief Health Equity Officer of Humana and a chair and Professor in the Department of Family Medicine at The Ohio State University Wexner Medical Center. Prior to her appointment at OSU, she served as the inaugural Chief Clinical Transformation Officer for RubiconMD, an eConsult platform that improves primary care access to specialty care for underserved patients. Olayiwola is dedicated to serving marginalized patient populations and addressing the social determinants through community and technology-based infrastructures of healthcare reform. She has published articles on the use of eConsults and telehealth to provide underserved patients with primary care treatments so that they have a low cost and efficient means of reaching specialized care. Olayiwola has founded numerous non-profits and healthcare start-ups such as GIRLTALK Inc, Inspire Health Solutions LLC, and the Minority Women Professionals are MVPs Program. She has been recognized at the national and international level for her work and efforts to educate, advocate and provide healthcare to those in need. She was named Woman of the Year by the American Telemedicine Association in 2019, and received the Public Health Innovator Award from Harvard School of Public Health in 2019, as well as being named one of America's Top Family Doctors from 2007 to 2008 by the Consumers Research Council of America.
References
- ↑ From the North American Primary Care Research Group. (2003). The Genesis of the North American Primary Care Research Group. The Annals of Family Medicine, 1(4), 247.
- ↑ Ewigman, B., Chen, F., Davis, A., Green, L., King, D., Kuzel, T., ... & Vansaghi, T. (2016). The Building Research Capacity (BRC) Initiative: To Be Launched at the 2016 Annual Napcrg Meeting. The Annals of Family Medicine, 14(6), 585-586.
- ↑ Robinson, K., & Westfall, J. (2011). NAPCRG puts the increase of primary care research funding at the top of the priority list. The Annals of Family Medicine, 9(5), 468-469.
- ↑ Sand, J., Felzien, M., Haeme, R., Tapp, H., Derkowski, D., & Westfall, J. M. (2017). The North American Primary Care Research Group’s Patient and Clinician Engagement Program (PaCE): Demystifying patient engagement through a dyad model. Family practice, 34(3), 285-289.
- ↑ Willenborg, M. (2017). NAPCRG LAUNCHES TRAINEE ENGAGEMENT PROGRAM. The Annals of Family Medicine, 15(2), 184-185.
- ↑ Nease, D. E., & Campbell-Scherer, D. (2018). 2018 PBRN CONFERENCE HIGHLIGHTS: ADDRESSING HEALTH DISPARITIES IN PBRN RESEARCH. The Annals of Family Medicine, 16(5), 470-471.
- ↑ Nagykaldi, Z., Davis, M. M., Lipman, P. D., Dluzak, L., Haught, J., & ICPF Steering Committee. (2020). THIRD INTERNATIONAL CONFERENCE ON PRACTICE FACILITATION (ICPF) FOCUSES ON EXTENDING FACILITATION TO THE COMMUNITY. The Annals of Family Medicine, 18(1), 89-90.