Related Research Articles

Surgery is a medical specialty that uses manual and/or instrumental techniques to physically reach into a subject's body in order to investigate or treat pathological conditions such as a disease or injury, to alter bodily functions, to improve appearance, or to remove/replace unwanted tissues or foreign bodies. The subject receiving the surgery is typically a person, but can also be a non-human animal.

Anesthesia or anaesthesia is a state of controlled, temporary loss of sensation or awareness that is induced for medical or veterinary purposes. It may include some or all of analgesia, paralysis, amnesia, and unconsciousness. An individual under the effects of anesthetic drugs is referred to as being anesthetized.
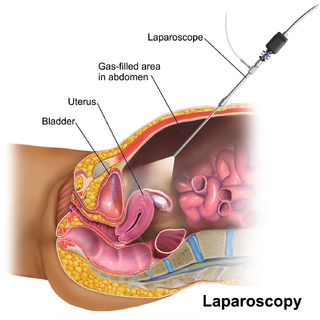
Laparoscopy is an operation performed in the abdomen or pelvis using small incisions with the aid of a camera. The laparoscope aids diagnosis or therapeutic interventions with a few small cuts in the abdomen.

An appendectomy or appendicectomy is a surgical operation in which the vermiform appendix is removed. Appendectomy is normally performed as an urgent or emergency procedure to treat complicated acute appendicitis.

Tonsillectomy is a surgical procedure in which both palatine tonsils are fully removed from the back of the throat. The procedure is mainly performed for recurrent tonsillitis, throat infections and obstructive sleep apnea (OSA). For those with frequent throat infections, surgery results in 0.6 fewer sore throats in the following year, but there is no evidence of long term benefits. In children with OSA, it results in improved quality of life.

General anaesthesia (UK) or general anesthesia (US) is a method of medically inducing loss of consciousness that renders a patient unarousable even with painful stimuli. This effect is achieved by administering either intravenous or inhalational general anaesthetic medications, which often act in combination with an analgesic and neuromuscular blocking agent. Spontaneous ventilation is often inadequate during the procedure and intervention is often necessary to protect the airway. General anaesthesia is generally performed in an operating theater to allow surgical procedures that would otherwise be intolerably painful for a patient, or in an intensive care unit or emergency department to facilitate endotracheal intubation and mechanical ventilation in critically ill patients. Depending on the procedure, general anaesthesia may be optional or required. Regardless of whether a patient may prefer to be unconscious or not, certain pain stimuli could result in involuntary responses from the patient that may make an operation extremely difficult. Thus, for many procedures, general anaesthesia is required from a practical perspective.
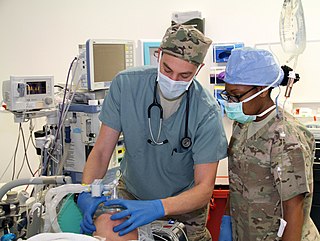
Anesthesiology, anaesthesiology, or anaesthesia is the medical specialty concerned with the total perioperative care of patients before, during and after surgery. It encompasses anesthesia, intensive care medicine, critical emergency medicine, and pain medicine. A physician specialized in anesthesiology is called an anesthesiologist, anaesthesiologist, or anaesthetist, depending on the country. In some countries, the terms are synonymous, while in other countries, they refer to different positions and anesthetist is only used for non-physicians, such as nurse anesthetists.

Spinal anaesthesia, also called spinal block, subarachnoid block, intradural block and intrathecal block, is a form of neuraxial regional anaesthesia involving the injection of a local anaesthetic or opioid into the subarachnoid space, generally through a fine needle, usually 9 cm (3.5 in) long. It is a safe and effective form of anesthesia usually performed by anesthesiologists that can be used as an alternative to general anesthesia commonly in surgeries involving the lower extremities and surgeries below the umbilicus. The local anesthetic with or without an opioid injected into the cerebrospinal fluid provides locoregional anaesthesia: true analgesia, motor, sensory and autonomic (sympathetic) blockade. Administering analgesics in the cerebrospinal fluid without a local anaesthetic produces locoregional analgesia: markedly reduced pain sensation, some autonomic blockade, but no sensory or motor block. Locoregional analgesia, due to mainly the absence of motor and sympathetic block may be preferred over locoregional anaesthesia in some postoperative care settings. The tip of the spinal needle has a point or small bevel. Recently, pencil point needles have been made available.
Awareness under anesthesia, also referred to as intraoperative awareness or accidental awareness during general anesthesia (AAGA), is a rare complication of general anesthesia where patients regain varying levels of consciousness during their surgical procedures. While anesthesia awareness is possible without resulting in any long-term memory of the experience, it is also possible for victims to have awareness with explicit recall, where they can remember the events related to their surgery.
Postoperative nausea and vomiting (PONV) is the phenomenon of nausea, vomiting, or retching experienced by a patient in the post-anesthesia care unit (PACU) or within 24 hours following a surgical procedure. PONV affects about 10% of the population undergoing general anaesthesia each year. PONV can be unpleasant and lead to a delay in mobilization and food, fluid, and medication intake following surgery.

Dupuytren's contracture is a condition in which one or more fingers become permanently bent in a flexed position. It is named after Guillaume Dupuytren, who first described the underlying mechanism of action, followed by the first successful operation in 1831 and publication of the results in The Lancet in 1834. It usually begins as small, hard nodules just under the skin of the palm, then worsens over time until the fingers can no longer be fully straightened. While typically not painful, some aching or itching may be present. The ring finger followed by the little and middle fingers are most commonly affected. It can affect one or both hands. The condition can interfere with activities such as preparing food, writing, putting the hand in a tight pocket, putting on gloves, or shaking hands.
Perioperative mortality has been defined as any death, regardless of cause, occurring within 30 days after surgery in or out of the hospital. Globally, 4.2 million people are estimated to die within 30 days of surgery each year. An important consideration in the decision to perform any surgical procedure is to weigh the benefits against the risks. Anesthesiologists and surgeons employ various methods in assessing whether a patient is in optimal condition from a medical standpoint prior to undertaking surgery, and various statistical tools are available. ASA score is the most well known of these.

Plantar fascial fibromatosis, also known as Ledderhose's disease, Morbus Ledderhose, and plantar fibromatosis, is a relatively uncommon non-malignant thickening of the feet's deep connective tissue, or fascia. In the beginning, where nodules start growing in the fascia of the foot, the disease is minor. Over time, walking becomes painful. The disease is named after Georg Ledderhose, a German surgeon who described the condition for the first time in 1894. A similar disease is Dupuytren's disease, which affects the hand and causes bent hand or fingers.

Robot-assisted surgery or robotic surgery are any types of surgical procedures that are performed using robotic systems. Robotically assisted surgery was developed to try to overcome the limitations of pre-existing minimally-invasive surgical procedures and to enhance the capabilities of surgeons performing open surgery.
Hand surgery deals with both surgical and non-surgical treatment of conditions and problems that may take place in the hand or upper extremity including injury and infection. Hand surgery may be practiced by post graduates of orthopedic surgery and plastic surgery.

Thoracoscopy is a medical procedure involving internal examination, biopsy and/or resection/drainage of disease or masses within the pleural cavity, usually with video assistance. Thoracoscopy may be performed either under general anaesthesia or under sedation with local anaesthetic.
An exploratory laparotomy is a general surgical operation where the abdomen is opened and the abdominal organs are examined for injury or disease. It is the standard of care in various blunt and penetrating trauma situations in which there may be life-threatening internal injuries. It is also used in certain diagnostic situations, in which the operation is undertaken in search of a unifying cause for multiple signs and symptoms of disease, and in the staging of some cancers.

Intravenous regional anesthesia (IVRA) or Bier's block anesthesia is an anesthetic technique on the body's extremities where a local anesthetic is injected intravenously and isolated from circulation in a target area. The technique usually involves exsanguination of the target region, which forces blood out of the extremity, followed by the application of pneumatic tourniquets to safely stop blood flow. The anesthetic agent is intravenously introduced into the limb and allowed to diffuse into the surrounding tissue while tourniquets retain the agent within the desired area.

Carpal tunnel surgery, also called carpal tunnel release (CTR) and carpal tunnel decompression surgery, is a nerve decompression in which the transverse carpal ligament is divided. It is a surgical treatment for carpal tunnel syndrome (CTS) and recommended when there is constant (not just intermittent) numbness, muscle weakness, or atrophy, and when night-splinting no longer controls intermittent symptoms of pain in the carpal tunnel. In general, milder cases can be controlled for months to years, but severe cases are unrelenting symptomatically and are likely to result in surgical treatment. Approximately 500,000 surgical procedures are performed each year, and the economic impact of this condition is estimated to exceed $2 billion annually.
The effects of early-life exposures to anesthesia on the brain in humans are controversial. Evidence from nonhuman primate research suggests significant developmental neurotoxicity and long-term social impairment, with a dose–response relationship where repeated exposures cause a more severe impact than single ones. Research in humans has not found conclusive clinical evidence of cognitive impairment; however, systematic reviews imply the possibility of greater behavioural impairments in children exposed to anesthesia before the age of three than control subjects.
References
- ↑ Hoffman, Jan (March 25, 2017). "Going Under the Knife, With Eyes and Ears Wide Open". The New York Times. Retrieved 2019-09-11.
- Bismil, M.; Bismil, Q.; Harding, D.; Harris, P.; Lamyman, E.; Sansby, L. (18 April 2012). "Transition to total one-stop wide-awake hand surgery service-audit: a retrospective review". JRSM Short Reports. 3 (4): 23. doi:10.1258/shorts.2012.012019. PMC 3375846 . PMID 22715424.
- Bismil, QMK.; Bismil, M.; Bismil, A.; Neathey, J.; Gadd, J.; Roberts, S.; Brewster, J. (July 2012). "The development of one-stop wide-awake dupuytren's fasciectomy service: a retrospective review". JRSM Short Reports. 3 (7): 48. doi:10.1258/shorts.2012.012050. PMC 3422854 . PMID 22908029.