Related Research Articles

Over-the-counter (OTC) drugs are medicines sold directly to a consumer without a requirement for a prescription from a healthcare professional, as opposed to prescription drugs, which may be supplied only to consumers possessing a valid prescription. In many countries, OTC drugs are selected by a regulatory agency to ensure that they contain ingredients that are safe and effective when used without a physician's care. OTC drugs are usually regulated according to their active pharmaceutical ingredient (API) rather than final products. By regulating APIs instead of specific drug formulations, governments allow manufacturers the freedom to formulate ingredients, or combinations of ingredients, into proprietary mixtures.

Pharmacy is the science and practice of discovering, producing, preparing, dispensing, reviewing and monitoring medications, aiming to ensure the safe, effective, and affordable use of medicines. It is a miscellaneous science as it links health sciences with pharmaceutical sciences and natural sciences. The professional practice is becoming more clinically oriented as most of the drugs are now manufactured by pharmaceutical industries. Based on the setting, pharmacy practice is either classified as community or institutional pharmacy. Providing direct patient care in the community of institutional pharmacies is considered clinical pharmacy.
A medical error is a preventable adverse effect of care ("iatrogenesis"), whether or not it is evident or harmful to the patient. This might include an inaccurate or incomplete diagnosis or treatment of a disease, injury, syndrome, behavior, infection, or other ailment.
Polypharmacy (polypragmasia) is an umbrella term to describe the simultaneous use of multiple medicines by a patient for their conditions. The term polypharmacy is often defined as regularly taking five or more medicines but there is no standard definition and the term has also been used in the context of when a person is prescribed 2 or more medications at the same time. Polypharmacy may be the consequence of having multiple long-term conditions, also known as multimorbidity and is more common in people who are older. In some cases, an excessive number of medications at the same time is worrisome, especially for people who are older with many chronic health conditions, because this increases the risk of an adverse event in that population. In many cases, polypharmacy cannot be avoided, but 'appropriate polypharmacy' practices are encouraged to decrease the risk of adverse effects. Appropriate polypharmacy is defined as the practice of prescribing for a person who has multiple conditions or complex health needs by ensuring that medications prescribed are optimized and follow 'best evidence' practices.
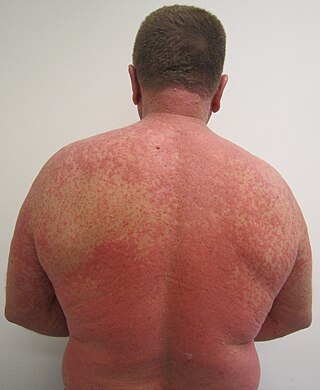
An adverse drug reaction (ADR) is a harmful, unintended result caused by taking medication. ADRs may occur following a single dose or prolonged administration of a drug or may result from the combination of two or more drugs. The meaning of this term differs from the term "side effect" because side effects can be beneficial as well as detrimental. The study of ADRs is the concern of the field known as pharmacovigilance. An adverse event (AE) refers to any unexpected and inappropriate occurrence at the time a drug is used, whether or not the event is associated with the administration of the drug. An ADR is a special type of AE in which a causative relationship can be shown. ADRs are only one type of medication-related harm. Another type of medication-related harm type includes not taking prescribed medications, which is also known as non-adherence. Non-adherence to medications can lead to death and other negative outcomes. Adverse drug reactions require the use of a medication.
A consultant pharmacist is a pharmacist who works as a consultant providing expert advice on clinical pharmacy, academic pharmacy or practice, public health pharmacy, industrial pharmacy, community pharmacy or practice, pharmaceutical analysis etc., regarding the safe use and production of medications or on the provision of pharmaceutical services to medical institutions, hospitals, universities, research institutions, medical practices and individual patients.

Rivaroxaban, sold under the brand name Xarelto among others, is an anticoagulant medication used to treat and prevent blood clots. Specifically it is used to treat deep vein thrombosis and pulmonary emboli and prevent blood clots in atrial fibrillation and following hip or knee surgery. It is taken by mouth.
Pharmacotherapy, also known as pharmacological therapy or drug therapy, is defined as medical treatment that utilizes one or more pharmaceutical drugs to improve ongoing symptoms, treat the underlying condition, or act as a prevention for other diseases (prophylaxis).
Patient safety is a discipline that emphasizes safety in health care through the prevention, reduction, reporting and analysis of error and other types of unnecessary harm that often lead to adverse patient events. The frequency and magnitude of avoidable adverse events, often known as patient safety incidents, experienced by patients was not well known until the 1990s, when multiple countries reported significant numbers of patients harmed and killed by medical errors. Recognizing that healthcare errors impact 1 in every 10 patients around the world, the World Health Organization (WHO) calls patient safety an endemic concern. Indeed, patient safety has emerged as a distinct healthcare discipline supported by an immature yet developing scientific framework. There is a significant transdisciplinary body of theoretical and research literature that informs the science of patient safety with mobile health apps being a growing area of research.

A hospital pharmacy is a department within a hospital that prepares, compounds, stocks and dispenses inpatient medications. Hospital pharmacies usually stock a larger range of medications, including more specialized and investigational medications, than would be feasible in the community setting. Hospital pharmacies may also dispense over-the-counter and prescription medications to outpatients.

An auxiliary label is a label added on to a dispensed medication package by a pharmacist in addition to the usual prescription label. These labels are intended to provide supplementary information regarding the safe administration, use, and storage of the medication. Auxiliary labels provide information which can augment but not replace verbal counselling from a pharmacist.
A veterinary pharmacist is a specially trained pharmacist who dispenses veterinary drugs and supplies or products and advice to owners of companion animals and livestock. In addition, they advise the regulatory bodies and are involved in the formulation of veterinary drugs. Veterinary pharmacy is a field of pharmacy practice, in which veterinary pharmacists may compound medications, fill prescriptions, and manage drug therapies for animals. Veterinary pharmacists are licensed pharmacists who specialize in the distribution of medications for animals.
Health information technology (HIT) is health technology, particularly information technology, applied to health and health care. It supports health information management across computerized systems and the secure exchange of health information between consumers, providers, payers, and quality monitors. Based on a 2008 report on a small series of studies conducted at four sites that provide ambulatory care – three U.S. medical centers and one in the Netherlands, the use of electronic health records (EHRs) was viewed as the most promising tool for improving the overall quality, safety and efficiency of the health delivery system.
Medication therapy management, generally called medicine use review in the United Kingdom, is a service provided typically by pharmacists, medical affairs, and RWE scientists that aims to improve outcomes by helping people to better understand their health conditions and the medications used to manage them. This includes providing education on the disease state and medications used to treat the disease state, ensuring that medicines are taken correctly, reducing waste due to unused medicines, looking for any side effects, and providing education on how to manage any side effects. The process that can be broken down into five steps: medication therapy review, personal medication record, medication-related action plan, intervention and or referral, and documentation and follow-up.
Drug therapy problems (DTPs) represent the categorization and definition of clinical problems related to the use of medications or "drugs" in the field of pharmaceutical care. In the course of clinical practice, DTPs are often identified, prevented, and/or resolved by pharmacists in the course of medication therapy management, as experts on the safety and efficacy of medications, but other healthcare professionals may also manage DTPs.
Deprescribing is a process to taper or stop medications with the intention to achieve improved health outcomes by reducing exposure to medications that are potentially either harmful or no longer required. Deprescribing is important to consider with changing health and care goals over time, as well as polypharmacy and adverse effects. Deprescribing can improve adherence, cost, and health outcomes but may have adverse drug withdrawal effects. More specifically, deprescribing is the planned and supervised process of intentionally stopping a medication or reducing its dose to improve the person's health or reduce the risk of adverse side effects. Deprescribing is usually done because the drug may be causing harm, may no longer be helping the patient, or may be inappropriate for the individual patient's current situation. Deprescribing can help correct polypharmacy and prescription cascade.

David Bates is an American-born physician, biomedical informatician, and professor, who is internationally renowned for his work regarding the use of health information technology (HIT) to improve the safety and quality of healthcare, in particular by using clinical decision support. Bates has done work in the area of medication safety. He began by describing the epidemiology of harm caused by medications, first in hospitalized patients and then in other settings such as the home and nursing homes. Subsequently, he demonstrated that by implementing computerized physician order entry (CPOE), medication safety could be dramatically improved in hospitals. This work led the Leapfrog Group to call CPOE one of the four changes that would most improve the safety of U.S. healthcare. It also helped hospitals to justify investing in electronic health records and in particular, CPOE. Throughout his career, Bates has published over 600 peer reviewed articles and is the most cited researcher in the fields of both patient safety and biomedical informatics, with an h-index of 115. In a 2013 analysis published by the European Journal of Clinical Investigation, he ranked among the top 400 living biomedical researchers of any type. He is currently editor of the Journal of Patient Safety.
Drug recycling, also referred to as medication redispensing or medication re-use, is the idea that health care organizations or patients with unused drugs can transfer them in a safe and appropriate way to another patient in need. The purpose of such a program is reducing medication waste, thereby saving healthcare costs, enlarging medications’ availability and alleviating the environmental burden of medication.
The Medication Appropriateness Tool for Comorbid Health conditions during Dementia (MATCH-D) criteria supports clinicians to manage medication use specifically for people with dementia without focusing only on the management of the dementia itself.
The Institute for Safe Medication Practices (ISMP) is an American 501(c)(3) organization focusing on the prevention of medication errors and promoting safe medication practices. It is affiliated with ECRI.
References
- ↑ National Patient Safety Agency. NICE NPSA medicines reconciliation adults in hospital. Patient Safety Alert, Reference number 1035. Issue date 1 December 2007. London, UK.
- ↑ "Medicines reconciliation to be an essential service from 2020/2021, says NHS England". Pharmaceutical Journal. 28 January 2020. Retrieved 22 March 2020.
- ↑ Prey, Jennifer E.; Polubriaginof, Fernanda; Grossman, Lisa V.; Masterson Creber, Ruth; Tsapepas, Demetra; Perotte, Rimma; Qian, Min; Restaino, Susan; Bakken, Suzanne; Hripcsak, George; Efird, Leigh (2018-11-01). "Engaging hospital patients in the medication reconciliation process using tablet computers". Journal of the American Medical Informatics Association. 25 (11): 1460–1469. doi: 10.1093/jamia/ocy115 . PMC 7263785 . PMID 30189000.
- ↑ "Hospital 2020 National Patient Safety Goals". www.jointcommission.org. Retrieved 2020-10-29.
- ↑ Urban, R; Armitage, G; Morgan, J; et al. (2014). "Custom and practice: a multi-center study of medicines reconciliation following admission in four acute hospitals in the UK". Res Social Adm Pharm. 10 (2): 355–68. doi:10.1016/j.sapharm.2013.06.009. PMID 24529643.
- ↑ Bell, CM; Bajcar, J; Bierman, AS; Li, P; Mamdani, MM; Urbach, DR (2006). "Potentially unintended discontinuation of long-term medication use after elective surgical procedures". Arch Intern Med. 166 (22): 2525–31. doi: 10.1001/archinte.166.22.2525 . PMID 17159020.
- ↑ Bell, Chaim M.; Rahimi-Darabad, Parisa; Orner, Avi I. (2006-09-01). "Discontinuity of chronic medications in patients discharged from the intensive care unit". Journal of General Internal Medicine. 21 (9): 937–941. doi:10.1111/j.1525-1497.2006.00499.x. ISSN 1525-1497. PMC 1831608 . PMID 16918738.
- ↑ Yeung, E (November 11, 2016). "Are we legitimately stopping medications? Use of pharmacist and junior doctor teaching to improve medication reconciliation". Br J Gen Pract.
- ↑ Yeung, Eugene Y. H. (2015-10-01). "Adverse drug reactions: a potential role for pharmacists". The British Journal of General Practice. 65 (639): 511.1–511. doi:10.3399/bjgp15X686821. ISSN 1478-5242. PMC 4582849 . PMID 26412813.
- ↑ Gondora, Nyasha; Versteeg, Sarah G.; Carter, Caitlin; Bishop, Lisa D.; Sproule, Beth; Turcotte, Dana; Halpape, Katelyn; Beazely, Michael A.; Dattani, Shelita; Kwong, Mona; Nissen, Lisa; Chang, Feng (May 2022). "The role of pharmacists in opioid stewardship: A scoping review". Research in Social and Administrative Pharmacy. 18 (5): 2714–2747. doi:10.1016/j.sapharm.2021.06.018. ISSN 1551-7411.