Related Research Articles

Coronary artery bypass surgery, also known as coronary artery bypass graft, is a surgical procedure to treat coronary artery disease (CAD), the buildup of plaques in the arteries of the heart. It can relieve chest pain caused by CAD, slow the progression of CAD, and increase life expectancy. It aims to bypass narrowings in heart arteries by using arteries or veins harvested from other parts of the body, thus restoring adequate blood supply to the previously ischemic heart.

Cardiopulmonary bypass (CPB) is a technique in which a machine temporarily takes over the function of the heart and lungs during cardiac surgery, maintaining the circulation of blood and oxygen to the body. The CPB pump itself is often referred to as a heart-lung machine or "the pump". Cardiopulmonary bypass pumps are operated by perfusionists. CPB is a form of extracorporeal circulation. Extracorporeal membrane oxygenation (ECMO) is generally used for longer-term treatment.
Cardiothoracic surgery is the field of medicine involved in surgical treatment of organs inside the thoracic cavity — generally treatment of conditions of the heart, lungs, and other pleural or mediastinal structures.

Cardiac surgery, or cardiovascular surgery, is surgery on the heart or great vessels performed by cardiac surgeons. It is often used to treat complications of ischemic heart disease ; to correct congenital heart disease; or to treat valvular heart disease from various causes, including endocarditis, rheumatic heart disease, and atherosclerosis. It also includes heart transplantation.
Aortic valve replacement is a procedure whereby the failing aortic valve of a patient's heart is replaced with an artificial heart valve. The aortic valve may need to be replaced because:

Cardiac catheterization is the insertion of a catheter into a chamber or vessel of the heart. This is done both for diagnostic and interventional purposes.
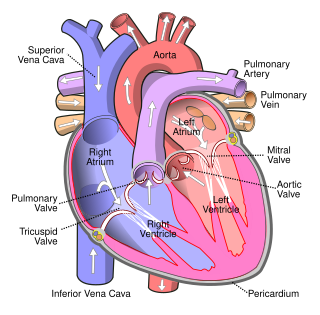
Mitral valve repair is a cardiac surgery procedure performed by cardiac surgeons to treat stenosis (narrowing) or regurgitation (leakage) of the mitral valve. The mitral valve is the "inflow valve" for the left side of the heart. Blood flows from the lungs, where it picks up oxygen, through the pulmonary veins, to the left atrium of the heart. After the left atrium fills with blood, the mitral valve allows blood to flow from the left atrium into the heart's main pumping chamber called the left ventricle. It then closes to keep blood from leaking back into the left atrium or lungs when the ventricle contracts (squeezes) to push blood out to the body. It has two flaps, or leaflets, known as cusps.

Median sternotomy is a type of surgical procedure in which a vertical inline incision is made along the sternum, after which the sternum itself is divided using a sternal saw. This procedure provides access to the heart and lungs for surgical procedures such as heart transplant, lung transplant, corrective surgery for congenital heart defects, or coronary artery bypass surgery.
Hybrid coronary revascularization (HCR) or hybrid coronary bypass is a relatively new type of heart surgery that provides an alternative to traditional coronary artery bypass surgery (CABG) or percutaneous coronary intervention by combining the two into one operation. It is this combining aspect that "hybrid" refers to. HCR is one of several types of hybrid cardiac surgery; it is not to be confused with a MIDCAB procedure, which uses the smaller thoracotomy incision but does not involve coronary stenting.
Minimally invasive direct coronary artery bypass (MIDCAB) is a surgical treatment for coronary heart disease that is a less invasive method of coronary artery bypass surgery (CABG). MIDCAB gains surgical access to the heart with a smaller incision than other types of CABG. MIDCAB is sometimes referred to as "keyhole" heart surgery because the operation is analogous to operating through a keyhole.
Postperfusion syndrome, also known as "pumphead", is a constellation of neurocognitive impairments attributed to cardiopulmonary bypass (CPB) during cardiac surgery. Symptoms of postperfusion syndrome are subtle and include defects associated with attention, concentration, short-term memory, fine motor function, and speed of mental and motor responses. Studies have shown a high incidence of neurocognitive deficit soon after surgery, but the deficits are often transient with no permanent neurological impairment.

Off-pump coronary artery bypass or "beating heart" surgery is a form of coronary artery bypass graft (CABG) surgery performed without cardiopulmonary bypass as a treatment for coronary heart disease. It was primarily developed in the early 1990s by Dr. Amano Atsushi. Historically, during bypass surgeries, the heart is stopped and a heart-lung machine takes over the work of the heart and lungs. When a cardiac surgeon chooses to perform the CABG procedure off-pump, also known as OPCAB, the heart is still beating while the graft attachments are made to bypass a blockage.
Cardiothoracic anesthesiology is a subspeciality of the medical practice of anesthesiology, devoted to the preoperative, intraoperative, and postoperative care of adult and pediatric patients undergoing cardiothoracic surgery and related invasive procedures.
Vessel harvesting is a surgical technique that may be used in conjunction with a coronary artery bypass graft (CABG). For patients with coronary artery disease, a physician may recommend a bypass to reroute blood around blocked arteries to restore and improve blood flow and oxygen to the heart. To create the bypass graft, a surgeon will remove or "harvest" healthy blood vessels from another part of the body, often from the patient's leg or arm. This vessel becomes a graft, with one end attaching to a blood source above and the other end below the blocked area, creating a "conduit" channel or new blood flow connection across the heart.

A hybrid cardiac surgical procedure in a narrow sense is defined as a procedure that combines a conventional, more invasive surgical part with an interventional part, using some sort of catheter-based procedure guided by fluoroscopy imaging in a hybrid operating room (OR) without interruption. The hybrid technique has a reduced risk of surgical complications and has shown decreased recovery time. It can be used to treat numerous heart diseases and conditions and with the increasing complexity of each case, the hybrid surgical technique is becoming more common.
Dr R Ravi Kumar graduated from Stanley Medical College and obtained the FRCS from Edinburgh. He worked at the Harefield Hospital, UK, under Sir Magdi Yacoub involving himself with adult cardiac surgery including heart and lung transplant and aortic homografts. Dr Ravi Kumar then underwent surgical residency in Boston, MA, United States. Following this he worked with Dr Albert Starr in Portland, Oregon. He pursued his cardiothoracic residency at the University of Texas, South Western Medical Center, Dallas, Texas, U.S. He continued at the same institution as an advanced fellow in Heart & Lung Transplant and is UNOS, certifiable for Heart & Lung Transplant.
Uwe Klima is UAE based professor of surgery and a faculty member at the Hannover Medical School, Germany. He also is the medical and managing director at German Heart Centre, Dubai.

Dr. Anil Bhan is the Chairman of Cardiac Surgery Heart Institute, Medanta Hospital, Gurugram, India. He graduated from Medical College Srinagar. He has the largest experience in aortic surgery in India since he has designed and developed more than 50 surgical instruments in the field of cardiac surgery. He was one of the team members to perform the first successful heart transplant in India in1994. He served as a co-founder of Max Heart and Vascular Institute, Saket, New Delhi, Director and Chief Co-Ordinator, Cardio thoracic and Vascular Surgery, MHVI, Saket.Additional Professor, Cardiothoracic Surgery and Vascular Surgery, AIIMS, New Delhi.
John D. Puskas is an American researcher, author, inventor and cardiovascular surgeon. As of 2022, he is Professor, Cardiovascular Surgery, Icahn School of Medicine at Mount Sinai, and chairman, Department of Cardiovascular Surgery at Mount Sinai Morningside, Mount Sinai Beth Israel and Mount Sinai West. He holds 11 U.S. patents and co-founded the International Coronary Congress and the International Society for Coronary Artery Surgery. He is credited by ResearchGate with 330 publications and 15,234 citations and as of 2022 Scopus reports an h-index of 62. Puskas is known for advancing coronary artery bypass (CABG) surgery by refining surgical techniques for all-arterial, off-pump CABG and inventing finer instruments to be used for advanced coronary bypass surgical procedures. He is credited with performing the first totally thoracoscopic bilateral pulmonary vein isolation procedure. He is the co-editor of State of the Art Surgical Coronary Revascularization, the first textbook solely devoted to coronary artery surgery.
Mario F.L. Gaudino, MD, PhD, MSCE, FEBCTS, FACC, FAHA is an Italian cardiothoracic surgeon who is the Stephen and Suzanne Weiss Professor in Cardiothoracic Surgery (II) and Professor of Clinical Epidemiology and Health Services Research at Weill Cornell Medicine and an attending cardiac surgeon at NewYork-Presbyterian Hospital and Weill Cornell Medical Center. He is an expert in coronary revascularization and clinical trialist. He is known for conducting the PALACS trial, which demonstrated that posterior pericardiotomy at the time of cardiac surgery reduced the incidence of post-operative atrial fibrillation and pericardial effusion.
References
- ↑ Mihaljevic, T; Cohn, LH; Unic, D; Aranki, SF; Couper, GS; Byrne, JG (September 2004). "One thousand minimally invasive valve operations: early and late results". Annals of Surgery. 240 (3): 529–34, discussion 534. doi:10.1097/01.sla.0000137141.55267.47. PMC 1356443 . PMID 15319724.
- ↑ Sef, D; Bahrami, T; Raja, SG; Klokocovnik, T (June 2022). "Current trends in minimally invasive valve-sparing aortic root replacement-Best available evidence". Journal of Cardiac Surgery. 37 (6): 1684–1690. doi:10.1111/jocs.16453. PMID 35348237.
- 1 2 "MICS CABG Technique Overview: Minimally Invasive CABG (MICS CABG) Procedure", "", 2010, p. 1
- ↑ "NYU Langone Medical Center", "", December 29, 2009
- 1 2 "The Heart Institute"," Archived 2016-08-04 at the Wayback Machine ", March 25, 2011
- ↑ Zhao, Dong Fang (February 28, 2017). "Coronary Artery Bypass Grafting With and Without Manipulation of the Ascending Aorta: A Network Meta-Analysis". Journal of the American College of Cardiology. 69 (8): 924–936. doi:10.1016/j.jacc.2016.11.071. PMID 28231944. S2CID 33400664.
- 1 2 McGinn JT, Usman S, Lapierre H, Pothula VR, Mesana TG, Ruel M (September 2009). "Minimally invasive coronary artery bypass grafting: dual-center experience in 450 consecutive patients". Circulation. 120 (11 Suppl): S78–84. doi: 10.1161/CIRCULATIONAHA.108.840041 . PMID 19752390.
- ↑ Loop FD, Lytle BW, Cosgrove DM, et al. (January 1986). "Influence of the internal-mammary-artery graft on 10-year survival and other cardiac events". The New England Journal of Medicine. 314 (1): 1–6. doi:10.1056/NEJM198601023140101. PMID 3484393.
- ↑ Acinapura AJ, Rose DM, Jacobowitz IJ, et al. (August 1989). "Internal mammary artery bypass grafting: influence on recurrent angina and survival in 2,100 patients". The Annals of Thoracic Surgery. 48 (2): 186–91. doi: 10.1016/0003-4975(89)90065-9 . PMID 2788393.
- ↑ "Medtronic", "", 2009
- 1 2 McGinn JT Jr, Usman S, Lapierre H, Pothula VR, Mesana TG, Ruel M (2009). "Minimally invasive coronary artery bypass grafting: dual-center experience in 450 consecutive patients". Circulation. 120 (11 Suppl): S78–84. doi: 10.1161/CIRCULATIONAHA.108.840041 . PMID 19752390.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ 2014 International Society for Minimally Invasive Cardiothoracic Surgery (ISMICS) Annual Scientific Meeting- Boston,, May 2014
- ↑ McGinn JT, Shariff MA, Nabagiez JP, Sadel S, Sharma R, Abogato P, Daniele E, Fazio L, Lapierre H, Sohmer B, Ruel M. (May 2014) Minimally Invasive CABG is Safe and Reproducible: Report on the First Thousand Cases. Presentation at International Society for Minimally Invasive Cardiothoracic Surgery (ISMICS) 2014 in Boston,, 2014
- ↑ Ruel M, Shariff MA, Lapierre H, et al. (January 2014). "Results of the Minimally Invasive Coronary Artery Bypass Grafting Angiographic Patency Study". The Journal of Thoracic and Cardiovascular Surgery. 147 (1): 203–8. doi: 10.1016/j.jtcvs.2013.09.016 . PMID 24183338.
- ↑ 2012 American Heart Association's Scientific Sessions and Resuscitation Science Symposium, , 2012.
- ↑ De C, Laffery J, Lakhani M, Shariff M, Ramchandani M, McGinn J. Minimally Invasive Coronary Artery Bypass Grafting: An Alternative Approach to Perform Coronary Artery Bypass Grafting on the Beating Heart. Poster presented at: International Society for Minimally Invasive Cardiothoracic Surgery (ISMICS) June 2010, Berlin, Germany, , 2010
- ↑ University of Ottawa Heart Center, http://www.ottawaheart.ca/misc/marc-ruel_research-clinical-interests.htm
- ↑ Houston Methodist DeBakey Heart Center, http://www.houstonmethodist.org/DrMaheshRamchandani
- ↑ Vanderbilt University Medical Center, "Department of Cardiac Surgery - Steven J. Hoff, M.D." Archived from the original on 2014-07-14. Retrieved 2014-07-07.