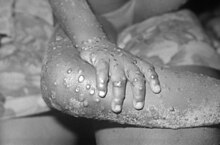
Mpox is an infectious viral disease that can occur in humans and other animals. Symptoms include a rash that forms blisters and then crusts over, fever, and swollen lymph nodes. The illness is usually mild and most of those infected will recover within a few weeks without treatment. The time from exposure to onset of symptoms ranges from five to twenty-one days and symptoms typically last from two to four weeks. Cases may be severe, especially in children, pregnant women or people with suppressed immune systems.

The monkeypox virus, is a species of double-stranded DNA virus that causes mpox disease in humans and other mammals. The monkeypox virus is a zoonotic virus belonging to the orthopoxvirus genus, making it closely related to the variola, cowpox, and vaccinia viruses. MPV is oval-shaped with a lipoprotein outer membrane. The genome is approximately 190 kb.

In 2014, an outbreak of Ebola virus disease in the Democratic Republic of the Congo (DRC) occurred. Genome sequencing has shown that this outbreak was not related to the 2014–15 West Africa Ebola virus epidemic, but was of the same EBOV species. It began in August 2014 and was declared over in November of that year, after 42 days without any new cases. This is the 7th outbreak there, three of which occurred during the period of Zaire.
The Democratic Republic of the Congo (DRC) was identified by the World Health Organization (WHO) on 11 May 2017 as having one Ebola-related death.

The 2018 Équateur province Ebola outbreak occurred in the north-west of the Democratic Republic of the Congo (DRC) from May to July 2018. It was contained entirely within Équateur province, and was the first time that vaccination with the rVSV-ZEBOV Ebola vaccine had been attempted in the early stages of an Ebola outbreak, with a total of 3,481 people vaccinated. It was the ninth recorded Ebola outbreak in the DRC.

Jean-Jacques Muyembe is a Congolese microbiologist. He is the general director of the Democratic Republic of the Congo Institut National pour la Recherche Biomedicale (INRB). He was part of team at the Yambuku Catholic Mission Hospital that investigated the first Ebola outbreak, and was part of the effort that discovered Ebola as a new disease, although his exact role is still subject to controversy. In 2016, he led the research that designed, along with other researchers at the INRB and the National Institute of Health Vaccine Research Center in the US, one of the most promising treatment for Ebola, mAb114. The treatment was successfully experimented during recent outbreaks in the DRC, on the express decision of the then DRC Minister of Health, Dr Oly Ilunga, despite a prior negative advice from the World Health Organization.

In May 2022, the World Health Organization (WHO) made an emergency announcement of the existence of a multi-country outbreak of mpox, a viral disease then commonly known as "monkeypox". The initial cluster of cases was found in the United Kingdom, where the first case was detected in London on 6 May 2022 in a patient with a recent travel history from Nigeria where the disease has been endemic. On 16 May, the UK Health Security Agency (UKHSA) confirmed four new cases with no link to travel to a country where mpox is endemic. Subsequently, cases have been reported from many countries and regions. The outbreak marked the first time mpox had spread widely outside Central and West Africa. The disease had been circulating and evolving in human hosts over a number of years prior to the outbreak and was caused by the clade IIb variant of the virus.

The 2022–2023 mpox outbreak in the United Kingdom is part of the larger outbreak of human mpox caused by the West African clade (type) of the monkeypox virus. The United Kingdom was the first country, outside of the endemic African areas, to experience an outbreak. As of 22 July 2022, there were 2,208 confirmed cases in the United Kingdom, with 2,115 in England, 54 in Scotland, 24 in Wales, and 15 in Northern Ireland.

The 2022–2023 mpox outbreak in Canada is a part of the outbreak of human mpox caused by the West African clade of the monkeypox virus. The outbreak started in Canada on May 19, 2022, with the country since then becoming one of the most affected in the Americas.
The 2022–2023 mpox outbreak in Italy is part of the larger outbreak of human mpox caused by the West African clade of the monkeypox virus. Italy was the sixth country, outside of the African countries with endemic mpox, to experience an outbreak in 2022. The first case was documented in Rome, Italy, on May 19, 2022. As of August 5th, Italy has 505 cases.
The 2022–2023 mpox outbreak in Belgium is part of the larger outbreak of human mpox caused by the West African clade of the monkeypox virus. Belgium was the fifth country, outside of the African countries with endemic mpox, to experience an outbreak in 2022. The first case was documented in Antwerp, Belgium, on 19 May 2022. As of 10 August, Belgium has 546 cases and 1 suspected case.
The 2022–2023 mpox outbreak in Israel is a part of the ongoing outbreak of human mpox caused by the West African clade of the monkeypox virus. The outbreak was first reported in Israel on 20 May 2022 when the Health Ministry announced a suspected case which was confirmed on 21 May 2022. One month later, on 21 June, the first locally transmitted case was reported.
The 2022–2023 mpox outbreak in Austria is part of the larger outbreak of human mpox caused by the West African clade of the monkeypox virus. Austria is the fifteenth country outside of Africa to experience an endemic mpox outbreak. The first case was reported in Vienna, Austria, on 22 May 2022. As of 2 December, Austria has confirmed a total of 327 cases.

The 2022–2023 mpox outbreak in Mexico is part of the larger outbreak of human mpox caused by the West African clade of the monkeypox virus. Mexico is the twenty-fourth country outside of Africa to experience an endemic mpox outbreak. The first case was reported in Mexico City, Mexico, on May 28, 2022. As of December 8th 2022, Mexico had confirmed a total of 3455 cases in all 32 states and 4 deaths.

The 2022–2023 mpox outbreak in Brazil is a part of the ongoing outbreak of human mpox caused by the West African clade of the monkeypox virus. The outbreak was first reported in Brazil on 9 June 2022 when a man in São Paulo was registered as the country's index case.

The 2022–2023 mpox outbreak in India is a part of the ongoing outbreak of human mpox caused by the West African clade of the monkeypox virus. The outbreak was first reported in India on 14 July 2022 when Kerala's State Health Minister Veena George announced a suspected imported case which was confirmed hours later by the NIV. India was the tenth country to report a mpox case in Asia and the first in South Asia. Currently, India has reported 23 cases of mpox.
In 2017, mpox reemerged in humans in Nigeria after 39 years. By the end of 2017, there were at least 115 confirmed cases.

The 2022 mpox outbreak in Asia is a part of the ongoing outbreak of human mpox caused by the West African clade of the monkeypox virus. The outbreak was reported in Asia on 20 May 2022 when Israel reported a suspected case of mpox, which was confirmed on 21 May. As of 10 August 2022, seven West Asian, three Southeast Asian, three East Asian and one South Asian country, along with Russia, have reported confirmed cases.
The 2022–2023 mpox outbreak in Europe is a part of the outbreak of human mpox caused by the West African clade of the monkeypox virus. The outbreak reached Europe on 6 May 2022 when the United Kingdom reported their first case of mpox. As of 13 July 2022, 35 European countries and territories have confirmed cases.