In genetics, shotgun sequencing is a method used for sequencing random DNA strands. It is named by analogy with the rapidly expanding, quasi-random shot grouping of a shotgun.
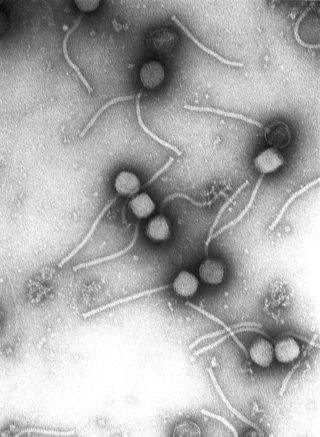
Virology is the scientific study of biological viruses. It is a subfield of microbiology that focuses on their detection, structure, classification and evolution, their methods of infection and exploitation of host cells for reproduction, their interaction with host organism physiology and immunity, the diseases they cause, the techniques to isolate and culture them, and their use in research and therapy.

Metagenomics is the study of genetic material recovered directly from environmental or clinical samples by a method called sequencing. The broad field may also be referred to as environmental genomics, ecogenomics, community genomics or microbiomics.

Fluorescence in situ hybridization (FISH) is a molecular cytogenetic technique that uses fluorescent probes that bind to only particular parts of a nucleic acid sequence with a high degree of sequence complementarity. It was developed by biomedical researchers in the early 1980s to detect and localize the presence or absence of specific DNA sequences on chromosomes. Fluorescence microscopy can be used to find out where the fluorescent probe is bound to the chromosomes. FISH is often used for finding specific features in DNA for use in genetic counseling, medicine, and species identification. FISH can also be used to detect and localize specific RNA targets in cells, circulating tumor cells, and tissue samples. In this context, it can help define the spatial-temporal patterns of gene expression within cells and tissues.

Antibiotic sensitivity testing or antibiotic susceptibility testing is the measurement of the susceptibility of bacteria to antibiotics. It is used because bacteria may have resistance to some antibiotics. Sensitivity testing results can allow a clinician to change the choice of antibiotics from empiric therapy, which is when an antibiotic is selected based on clinical suspicion about the site of an infection and common causative bacteria, to directed therapy, in which the choice of antibiotic is based on knowledge of the organism and its sensitivities.

QIAGEN is a provider of sample and assay technologies for molecular diagnostics, applied testing, academic and pharmaceutical research. The company operates in more than 35 offices in over 25 countries. QIAGEN N.V., the global corporate headquarter of the QIAGEN group, is located in Venlo, The Netherlands. European, American, and Asian regional headquarters are located in respectively Hilden, Germany; Germantown, Maryland United States; and Shanghai, China. QIAGEN's shares are listed at the NYSE and at the Frankfurt Stock Exchange in the Prime Standard. Thierry Bernard is the company's Chief Executive Officer(CEO). The main operative headquarters are located in Hilden, Germany.

Medical microbiology, the large subset of microbiology that is applied to medicine, is a branch of medical science concerned with the prevention, diagnosis and treatment of infectious diseases. In addition, this field of science studies various clinical applications of microbes for the improvement of health. There are four kinds of microorganisms that cause infectious disease: bacteria, fungi, parasites and viruses, and one type of infectious protein called prion.
Molecular pathology is an emerging discipline within pathology which is focused in the study and diagnosis of disease through the examination of molecules within organs, tissues or bodily fluids. Molecular pathology shares some aspects of practice with both anatomic pathology and clinical pathology, molecular biology, biochemistry, proteomics and genetics, and is sometimes considered a "crossover" discipline. It is multi-disciplinary in nature and focuses mainly on the sub-microscopic aspects of disease. A key consideration is that more accurate diagnosis is possible when the diagnosis is based on both the morphologic changes in tissues and on molecular testing.

A nucleic acid test (NAT) is a technique used to detect a particular nucleic acid sequence and thus usually to detect and identify a particular species or subspecies of organism, often a virus or bacterium that acts as a pathogen in blood, tissue, urine, etc. NATs differ from other tests in that they detect genetic materials rather than antigens or antibodies. Detection of genetic materials allows an early diagnosis of a disease because the detection of antigens and/or antibodies requires time for them to start appearing in the bloodstream. Since the amount of a certain genetic material is usually very small, many NATs include a step that amplifies the genetic material—that is, makes many copies of it. Such NATs are called nucleic acid amplification tests (NAATs). There are several ways of amplification, including polymerase chain reaction (PCR), strand displacement assay (SDA), or transcription mediated assay (TMA).
In the diagnostic laboratory, virus infections can be confirmed by a myriad of methods. Diagnostic virology has changed rapidly due to the advent of molecular techniques and increased clinical sensitivity of serological assays.

Exome sequencing, also known as whole exome sequencing (WES), is a genomic technique for sequencing all of the protein-coding regions of genes in a genome. It consists of two steps: the first step is to select only the subset of DNA that encodes proteins. These regions are known as exons—humans have about 180,000 exons, constituting about 1% of the human genome, or approximately 30 million base pairs. The second step is to sequence the exonic DNA using any high-throughput DNA sequencing technology.

Jumping libraries or junction-fragment libraries are collections of genomic DNA fragments generated by chromosome jumping. These libraries allow the analysis of large areas of the genome and overcome distance limitations in common cloning techniques. A jumping library clone is composed of two stretches of DNA that are usually located many kilobases away from each other. The stretch of DNA located between these two "ends" is deleted by a series of biochemical manipulations carried out at the start of this cloning technique.
Cell-free fetal DNA (cffDNA) is fetal DNA that circulates freely in the maternal blood. Maternal blood is sampled by venipuncture. Analysis of cffDNA is a method of non-invasive prenatal diagnosis frequently ordered for pregnant women of advanced maternal age. Two hours after delivery, cffDNA is no longer detectable in maternal blood.

Molecular diagnostics is a collection of techniques used to analyze biological markers in the genome and proteome, and how their cells express their genes as proteins, applying molecular biology to medical testing. In medicine the technique is used to diagnose and monitor disease, detect risk, and decide which therapies will work best for individual patients, and in agricultural biosecurity similarly to monitor crop- and livestock disease, estimate risk, and decide what quarantine measures must be taken.

Viral metagenomics is the metagenomic study of viral genetic material obtained from environmental DNA samples or clinical DNA samples obtained from a host or natural reservoir. Metagenomic methods can be applied to study viruses in any system and has been used to describe various viruses associated with cancerous tumors, extreme environments, terrestrial ecosystems, and the blood and feces of humans. The term virome is also used to refer to viruses investigated by metagenomic sequencing of viral nucleic acids and is frequently used to describe environmental shotgun metagenomes. Viral metagenomics is a culture independent methodology that provides insights on viral diversity, abundance, and functional potential of viruses within the environment. Viruses lack a universal phylogenetic marker making metagenomics the only way to assess the genetic diversity of viruses in an environmental sample. With the advancements of techniques that can exploit next-generation sequencing, viruses can now be studied outside of culturable virus-host pairs. This approach has created improvements in molecular epidemiology and accelerated the discovery of novel viruses.
Metatranscriptomics is the set of techniques used to study gene expression of microbes within natural environments, i.e., the metatranscriptome.

Surveyor nuclease assay is an enzyme mismatch cleavage assay used to detect single base mismatches or small insertions or deletions (indels).
Third-generation sequencing is a class of DNA sequencing methods currently under active development.
Urinary cell-free DNA (ucfDNA) refers to DNA fragments in urine released by urogenital and non-urogenital cells. Shed cells on urogenital tract release high- or low-molecular-weight DNA fragments via apoptosis and necrosis, while circulating cell-free DNA (cfDNA) that passes through glomerular pores contributes to low-molecular-weight DNA. Most of the ucfDNA is low-molecular-weight DNA in the size of 150-250 base pairs. The detection of ucfDNA composition allows the quantification of cfDNA, circulating tumour DNA, and cell-free fetal DNA components. Many commercial kits and devices have been developed for ucfDNA isolation, quantification, and quality assessment.











