Related Research Articles

Parkinsonism is a clinical syndrome characterized by tremor, bradykinesia, rigidity, and postural instability. Both hypokinetic as well as hyperkinetic features are displayed by Parkinsonism.These are the four motor symptoms found in Parkinson's disease (PD) – after which it is named – dementia with Lewy bodies (DLB), Parkinson's disease dementia (PDD), and many other conditions. This set of symptoms occurs in a wide range of conditions and may have many causes, including neurodegenerative conditions, drugs, toxins, metabolic diseases, and neurological conditions other than PD.
This is a timeline of HIV/AIDS, including but not limited to cases before 1980.
Following infection with HIV-1, the rate of clinical disease progression varies between individuals. Factors such as host susceptibility, genetics and immune function, health care and co-infections as well as viral genetic variability may affect the rate of progression to the point of needing to take medication in order not to develop AIDS.

The neuroimmune system is a system of structures and processes involving the biochemical and electrophysiological interactions between the nervous system and immune system which protect neurons from pathogens. It serves to protect neurons against disease by maintaining selectively permeable barriers, mediating neuroinflammation and wound healing in damaged neurons, and mobilizing host defenses against pathogens.

The human immunodeficiency virus (HIV) is a retrovirus that attacks the immune system. It can be managed with treatment. Without treatment it can lead to a spectrum of conditions including acquired immunodeficiency syndrome (AIDS).
The central nervous system (CNS) controls most of the functions of the body and mind. It comprises the brain, spinal cord and the nerve fibers that branch off to all parts of the body. The CNS viral diseases are caused by viruses that attack the CNS. Existing and emerging viral CNS infections are major sources of human morbidity and mortality.

Janice Ellen Clements is vice dean for faculty at the Johns Hopkins School of Medicine and the Mary Wallace Stanton Professor of Faculty Affairs. She is a professor in the departments of Molecular and Comparative Pathobiology, Neurology, and Pathology, and has a joint appointment in molecular biology and genetics. Her molecular biology and virology research examines lentiviruses and how they cause neurological diseases.

Gladstone Institutes is an independent, non-profit biomedical research organization whose focus is to better understand, prevent, treat and cure cardiovascular, viral and neurological conditions such as heart failure, HIV/AIDS and Alzheimer's disease. Its researchers study these diseases using techniques of basic and translational science. Another focus at Gladstone is building on the development of induced pluripotent stem cell technology by one of its investigators, 2012 Nobel Laureate Shinya Yamanaka, to improve drug discovery, personalized medicine and tissue regeneration.
In biology, a pathogen, in the oldest and broadest sense, is any organism or agent that can produce disease. A pathogen may also be referred to as an infectious agent, or simply a germ.
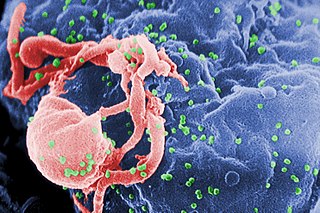
HIV/AIDS research includes all medical research that attempts to prevent, treat, or cure HIV/AIDS, as well as fundamental research about the nature of HIV as an infectious agent and AIDS as the disease caused by HIV.
Kalipada Pahan is a professor of Neurological Sciences, Biochemistry and Pharmacology, and the Floyd A. Davis, M.D., Endowed Chair in Neurology at the Rush University Medical Center. He is also a research career scientist at the Department of Veterans Affairs, Jesse Brown VA Medical Center. He is an eminent Indian American neuroscientist involved in translational research on multiple sclerosis, Parkinson's disease, Alzheimer's disease, dementia, and Batten disease. He is well known for his research on statins, cholesterol-lowering drugs. He first explored the application of statins in suppressing the inflammatory events in microglia, astroglia and macrophages. This finding has revolutionized the research on statin drugs. Later, his lab has shown that statins may be beneficial in protecting neurons and improving locomotor activities in Parkinson's disease by suppressing the activation of p21/Ras. His lab is also famous for research on cinnamon where they have described that this commonly-used natural spice may be beneficial for different brain disorders including improving memory and learning of poor learners. Recently his lab has delineated a unique crosstalk between fat and memory in which the lipid-lowering transcription factor PPARalpha controls the formation of hippocampal memory via transcriptional regulation of CREB, suggesting a possible reason for the connection between excess belly fat and memory loss.
Neuroinflammation is inflammation of the nervous tissue. It may be initiated in response to a variety of cues, including infection, traumatic brain injury, toxic metabolites, or autoimmunity. In the central nervous system (CNS), including the brain and spinal cord, microglia are the resident innate immune cells that are activated in response to these cues. The CNS is typically an immunologically privileged site because peripheral immune cells are generally blocked by the blood–brain barrier (BBB), a specialized structure composed of astrocytes and endothelial cells. However, circulating peripheral immune cells may surpass a compromised BBB and encounter neurons and glial cells expressing major histocompatibility complex molecules, perpetuating the immune response. Although the response is initiated to protect the central nervous system from the infectious agent, the effect may be toxic and widespread inflammation as well as further migration of leukocytes through the blood–brain barrier may occur.

Lauren V. Wood is an American allergist, immunologist, and staff physician at the National Cancer Institute (NCI) at the National Institutes of Health (NIH) in Bethesda, Maryland, where she has served as a principal investigator. She is known for conducting studies of vaccines for cancer, Human papillomavirus (HPV), Hepatitis C, and HIV especially for use with children, teens and young adults. She holds the rank of captain in the U.S. Public Health Service (PHS).
M. Juliana “Julie” McElrath is a senior vice president and director of the vaccine and infection disease division at Fred Hutchinson Cancer Research Center and the principal investigator of the HIV Vaccine Trials Network Laboratory Center in Seattle, Washington. She is also a professor at the University of Washington.

Sharon Ruth Lewin, FRACP, FAHMS is an Australian physician who is the inaugural Director of The Peter Doherty Institute for Infection and Immunity. She is also a Professor of Medicine at The University of Melbourne, a National Health and Medical Research Council (NHMRC) Practitioner Fellow, Director of the Cumming Global Centre for Pandemic Therapeutics, and President of the International AIDS Society (IAS).
Pontiano Kaleebu is a Ugandan physician, clinical immunologist, HIV/AIDS researcher, academic and medical administrator, who is the executive director of the Uganda Virus Research Institute.
Ya-Chi Ho is a Taiwanese infectious disease researcher and Associate Professor of Microbial Pathogenesis and Medicine at Yale University. Her research centers on the interaction between HIV and the host's immune system with the ultimate goal of curing HIV/AIDS.
Georgette D. Kanmogne is a Cameroonian American geneticist and molecular virologist and a full professor and vice chair for resource allocation and faculty development within the Department of Pharmacology and Experimental Neurosciences at the University of Nebraska Medical Center in Omaha, Nebraska. Kanmogne's research program focuses on exploring the pathogenesis of neuroAIDS by deciphering the mechanisms underlying blood brain barrier dysfunction and viral entry into the central nervous system. Her research also addresses the lack of HIV therapies that cross the blood brain barrier (BBB) and has played a critical role in the development of nanoparticles encapsulating HIV-drugs that can cross the BBB to prevent viral-mediated neuron death in the brain. Kanmogne collaborates with clinical and basic researchers across America, Cameroon, and West Africa, spanning disciplines from hematology to psychiatry, to explore how viral genetic diversity is correlated with the neurological impact of HIV.
Jasmine R. Marcelin is a Caribbean-American infectious disease physician and an Assistant Professor in the Department of Internal Medicine at the University of Nebraska Medical Center (UNMC). Marcelin is also the Associate Medical Director of the Antimicrobial Stewardship Program and as well as the Co-Director of Digital Innovation and Social Media Strategy at UNMC.

Monica Gandhi is an American physician and professor. She teaches medicine at the University of California, San Francisco (UCSF) and is director of the UCSF Gladstone Center for AIDS Research and the medical director of the San Francisco General Hospital HIV Clinic, Ward 86. Her research considers HIV prevalence in women, as well as HIV treatment and prevention. She has been noted as a critic of some aspects of the COVID-19 lockdowns in the US.
References
- ↑ Johnson, Amanda McGill (2022-01-28). "2022 Luncheon Honoreers". Nebraska Cures. Retrieved 2022-10-26./
- ↑ Temple University Health System (2019-07-02). "HIV eliminated from the genomes of living animals". Science Daily=en-US. Retrieved 2022-10-26.
- 1 2 3 4 Utesch, Margie (2018-07-03). "Humanitarian of the Year". The Jewish Community Center of Omaha. Retrieved 2021-12-16.
- ↑ "Potential new HIV treatment developed at UNMC". KMTV. 2020-04-29. Retrieved 2021-12-16.
- ↑ "Front Line (2009)" (PDF). University of Nebraska Medical Center, Department of Pharmacology and Experimental Neuroscience. Retrieved 2022-01-25.
- ↑ "About Us". University of Nebraska Medical Center, Department of Pharmacology and Experimental Neuroscience. Retrieved 2022-01-25.
- ↑ "UNMC Professor gets Fulbright to study in Israel (2001)". Daily Nebraskan. 21 March 2000. Retrieved 2022-11-04.
- 1 2 "The Pioneer in Neurovirology Award". International Society for NeurVirology. 2016. Retrieved 4 November 2022.
- ↑ Adachi, A; Gendelman, H E; Koenig, S; Folks, T; Willey, R; Rabson, A; Martin, M A (August 1986). "Production of acquired immunodeficiency syndrome-associated retrovirus in human and nonhuman cells transfected with an infectious molecular clone". Journal of Virology. 59 (2): 284–291. doi:10.1128/jvi.59.2.284-291.1986. ISSN 0022-538X. PMC 253077 . PMID 3016298. S2CID 12551511.
- ↑ Koenig, Scott; Gendelman, Howard E.; Orenstein, Jan M.; Dal Canto, Mauro C.; Pezeshkpour, Gholam H.; Yungbluth, Margaret; Janotta, Frank; Aksamit, Allen; Martin, Malcolm A.; Fauci, Anthony S. (1986-09-05). "Detection of AIDS Virus in Macrophages in Brain Tissue from AIDS Patients with Encephalopathy". Science. 233 (4768): 1089–1093. Bibcode:1986Sci...233.1089K. doi:10.1126/science.3016903. ISSN 0036-8075. PMID 3016903.
- ↑ Gendelman, H. E.; Narayan, O.; Molineaux, S.; Clements, J. E.; Ghotbi, Z. (October 1985). "Slow, persistent replication of lentiviruses: role of tissue macrophages and macrophage precursors in bone marrow". Proceedings of the National Academy of Sciences of the United States of America. 82 (20): 7086–7090. Bibcode:1985PNAS...82.7086G. doi: 10.1073/pnas.82.20.7086 . ISSN 0027-8424. PMC 391315 . PMID 2996004.
- ↑ Gendelman, Howard E.; Zheng, Jialin; Coulter, Cynthia L.; Ghorpade, Anuja; Che, Myhanh; Thylin, Michael; Rubocki, Ronald; Persidsky, Yuri; Hahn, Francis; Reinhard, Jr., John; Swindells, Susan (October 1998). "Suppression of Inflammatory Neurotoxins by Highly Active Antiretroviral Therapy in Human Immunodeficiency Virus-Associated Dementia". The Journal of Infectious Diseases. 178 (4): 1000–1007. doi: 10.1086/515693 . ISSN 0022-1899. PMID 9806027. S2CID 42427863.
- ↑ Spellman, Lisa (2019-08-09). "Science Cafe explores possibility of HIV cure". University of Nebraska Medical Center. Retrieved 2021-12-16.
- ↑ Gendelman, Howard E. (2012). The neurology of AIDS. Oxford University Press. ISBN 978-0-19-539934-9. OCLC 828615707.
- ↑ "Scientists say they found a cure for HIV in some mice. Humans could be next". www.washingtonpost.com. Retrieved 2022-11-23.
- ↑ "In a first, scientists eliminate HIV from an animal's genome". www.cbsnews.com. 3 July 2019. Retrieved 2021-12-17.
- ↑ Yancey-Bragg, N'dea. "Researchers have eliminated HIV in mice for the first time. Is a cure for humans next?". USA TODAY. Retrieved 2021-12-17.
- ↑ Dash, Prasanta K.; Kaminski, Rafal; Bella, Ramona; Su, Hang; Mathews, Saumi; Ahooyi, Taha M.; Chen, Chen; Mancuso, Pietro; Sariyer, Rahsan; Ferrante, Pasquale; Donadoni, Martina (December 2019). "Sequential LASER ART and CRISPR Treatments Eliminate HIV-1 in a Subset of Infected Humanized Mice". Nature Communications. 10 (1): 2753. Bibcode:2019NatCo..10.2753D. doi:10.1038/s41467-019-10366-y. ISSN 2041-1723. PMC 6606613 . PMID 31266936.
- ↑ Kulkarni, Tanmay A.; Bade, Aditya N.; Sillman, Brady; Shetty, Bhagya Laxmi Dyavar; Wojtkiewicz, Melinda S.; Gautam, Nagsen; Hilaire, James R.; Sravanam, Sruthi; Szlachetka, Adam; Lamberty, Benjamin G.; Morsey, Brenda M. (August 2020). "A year-long extended release nanoformulated cabotegravir prodrug". Nature Materials. 19 (8): 910–920. Bibcode:2020NatMa..19..910K. doi:10.1038/s41563-020-0674-z. ISSN 1476-1122. PMC 7384935 . PMID 32341511.
- ↑ Soriano, Vicente; Barreiro, Pablo; de Mendoza, Carmen (August 2020). "Long-acting antiretroviral therapy". Nature Materials. 19 (8): 826–827. Bibcode:2020NatMa..19..826S. doi: 10.1038/s41563-020-0731-7 . ISSN 1476-4660. PMID 32704135. S2CID 220721631.
- ↑ "Nebraska Nanomedicine Production Plant | Pharmacology | University of Nebraska Medical Center". www.unmc.edu. Retrieved 2021-12-16.
- ↑ "Exavir Therapeutics". exavirtherapeutics.com. 2021-02-14. Retrieved 2021-12-16.
- ↑ Benner, Eric J.; Mosley, R. Lee; Destache, Chris J.; Lewis, Travis B.; Jackson-Lewis, Vernice; Gorantla, Santhi; Nemachek, Craig; Green, Steven R.; Przedborski, Serge; Gendelman, Howard E. (2004-06-22). "Therapeutic immunization protects dopaminergic neurons in a mouse model of Parkinson's disease". Proceedings of the National Academy of Sciences of the United States of America. 101 (25): 9435–9440. Bibcode:2004PNAS..101.9435B. doi: 10.1073/pnas.0400569101 . ISSN 0027-8424. PMC 438994 . PMID 15197276.
- ↑ Gendelman, Howard E.; Zhang, Yuning; Santamaria, Pamela; Olson, Katherine E.; Schutt, Charles R.; Bhatti, Danish; Shetty, Bhagya Laxmi Dyavar; Lu, Yaman; Estes, Katherine A.; Standaert, David G.; Heinrichs-Graham, Elizabeth (2017-03-23). "Evaluation of the safety and immunomodulatory effects of sargramostim in a randomized, double-blind phase 1 clinical Parkinson's disease trial". npj Parkinson's Disease. 3 (1): 10. doi:10.1038/s41531-017-0013-5. ISSN 2373-8057. PMC 5445595 . PMID 28649610.
- ↑ Olson, Katherine E.; Namminga, Krista L.; Lu, Yaman; Schwab, Aaron D.; Thurston, Mackenzie J.; Abdelmoaty, Mai M.; Kumar, Vikas; Wojtkiewicz, Melinda; Obaro, Helen; Santamaria, Pamela; Mosley, R. Lee (2021-05-01). "Safety, tolerability, and immune-biomarker profiling for year-long sargramostim treatment of Parkinson's disease". eBioMedicine. 67: 103380. doi:10.1016/j.ebiom.2021.103380. ISSN 2352-3964. PMC 8138485 . PMID 34000620.
- ↑ Gendelman, Howard E; Grant, Igor; Everall, Ian Paul; Fox, Howard S; Gelbard, Harris A; Lipton, Stuart A; Swindells, Susan, eds. (2012). The Neurology of AIDS. Oxford University Press. doi:10.1093/med/9780195399349.001.0001. ISBN 978-0-19-996519-9.
- ↑ Ikezu, Tsuneya; Gendelman, Howard E., eds. (2017). Neuroimmune Pharmacology. doi:10.1007/978-3-319-44022-4. ISBN 978-3-319-44020-0.
- ↑ "Innovation Awards". UNeMed.com. 23 October 2022. Retrieved 23 November 2022.
- ↑ "2022 Luncheon Honorees". Nebraska Cures. 28 January 2022. Retrieved 28 April 2022.
- ↑ "Tribute to Dr. Howard Gendelman and Dr. Bonnie Bloch". YouTube. Nebraska Cures. Retrieved 28 April 2022.
- ↑ "SNIP - Society on NeuroImmune Pharmacology". s-nip.org. Retrieved 2021-12-16.
- ↑ "$3 Million Grant Recognizes Potential of Research at the UNMC Center for Neurovirology and Neurodegenerative Disorders". University of Nebraska Medical Center. 2001. Retrieved 4 November 2022.