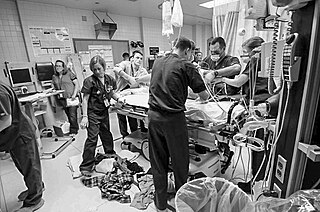
Emergency medicine is the medical speciality concerned with the care of illnesses or injuries requiring immediate medical attention. Emergency physicians specialize in providing care for unscheduled and undifferentiated patients of all ages. As first-line providers, in coordination with emergency medical services, they are primarily responsible for initiating resuscitation and stabilization and performing the initial investigations and interventions necessary to diagnose and treat illnesses or injuries in the acute phase. Emergency medical physicians generally practice in hospital emergency departments, pre-hospital settings via emergency medical services, and intensive care units. Still, they may also work in primary care settings such as urgent care clinics.

Health care, or healthcare, is the improvement of health via the prevention, diagnosis, treatment, amelioration or cure of disease, illness, injury, and other physical and mental impairments in people. Health care is delivered by health professionals and allied health fields. Medicine, dentistry, pharmacy, midwifery, nursing, optometry, audiology, psychology, occupational therapy, physical therapy, athletic training, and other health professions all constitute health care. The term includes work done in providing primary care, secondary care, and tertiary care, as well as in public health.
Palliative care is an interdisciplinary medical caregiving approach aimed at optimizing quality of life and mitigating suffering among people with serious, complex, and often terminal illnesses. Within the published literature, many definitions of palliative care exist. The World Health Organization (WHO) describes palliative care as "an approach that improves the quality of life of patients and their families facing the problems associated with life-threatening illness, through the prevention and relief of suffering by means of early identification and impeccable assessment and treatment of pain, illnesses including other problems whether physical, psychosocial, and spiritual". In the past, palliative care was a disease specific approach, but today the WHO takes a broader patient-centered approach that suggests that the principles of palliative care should be applied as early as possible to any chronic and ultimately fatal illness. This shift was important because if a disease-oriented approach is followed, the needs and preferences of the patient are not fully met and aspects of care, such as pain, quality of life, and social support, as well as spiritual and emotional needs, fail to be addressed. Rather, a patient-centered model prioritizes relief of suffering and tailors care to increase the quality of life for terminally ill patients.

Primary care is the day-to-day healthcare given by a health care provider. Typically this provider acts as the first contact and principal point of continuing care for patients within a healthcare system, and coordinates other specialist care that the patient may need. Patients commonly receive primary care from professionals such as a primary care physician, a physician assistant, a physical therapist, or a nurse practitioner. In some localities, such a professional may be a registered nurse, a pharmacist, a clinical officer, or an Ayurvedic or other traditional medicine professional. Depending on the nature of the health condition, patients may then be referred for secondary or tertiary care.

Family medicine is a medical specialty within primary care that provides continuing and comprehensive health care for the individual and family across all ages, genders, diseases, and parts of the body. The specialist, who is usually a primary care physician, is named a family physician. It is often referred to as general practice and a practitioner as a general practitioner. Historically, their role was once performed by any doctor with qualifications from a medical school and who works in the community. However, since the 1950s, family medicine / general practice has become a specialty in its own right, with specific training requirements tailored to each country. The names of the specialty emphasize its holistic nature and/or its roots in the family. It is based on knowledge of the patient in the context of the family and the community, focusing on disease prevention and health promotion. According to the World Organization of Family Doctors (WONCA), the aim of family medicine is "promoting personal, comprehensive and continuing care for the individual in the context of the family and the community". The issues of values underlying this practice are usually known as primary care ethics.
In the healthcare industry, pay for performance (P4P), also known as "value-based purchasing", is a payment model that offers financial incentives to physicians, hospitals, medical groups, and other healthcare providers for meeting certain performance measures. Clinical outcomes, such as longer survival, are difficult to measure, so pay for performance systems usually evaluate process quality and efficiency, such as measuring blood pressure, lowering blood pressure, or counseling patients to stop smoking. This model also penalizes health care providers for poor outcomes, medical errors, or increased costs. Integrated delivery systems where insurers and providers share in the cost are intended to help align incentives for value-based care.
The American College of Radiology (ACR), founded in 1923, is a professional medical society representing nearly 40,000 diagnostic radiologists, radiation oncologists, interventional radiologists, nuclear medicine physicians and medical physicists.
Fee-for-service (FFS) is a payment model where services are unbundled and paid for separately.
Patient safety is a discipline that emphasizes safety in health care through the prevention, reduction, reporting and analysis of error and other types of unnecessary harm that often lead to adverse patient events. The frequency and magnitude of avoidable adverse events, often known as patient safety incidents, experienced by patients was not well known until the 1990s, when multiple countries reported significant numbers of patients harmed and killed by medical errors. Recognizing that healthcare errors impact 1 in every 10 patients around the world, the World Health Organization (WHO) calls patient safety an endemic concern. Indeed, patient safety has emerged as a distinct healthcare discipline supported by an immature yet developing scientific framework. There is a significant transdisciplinary body of theoretical and research literature that informs the science of patient safety with mobile health apps being a growing area of research.
Hospital accreditation has been defined as “A self-assessment and external peer assessment process used by health care organizations to accurately assess their level of performance in relation to established standards and to implement ways to continuously improve”. Critically, accreditation is not just about standard-setting: there are analytical, counseling and self-improvement dimensions to the process. There are parallel issues in evidence-based medicine, quality assurance and medical ethics, and the reduction of medical error is a key role of the accreditation process. Hospital accreditation is therefore one component in the maintenance of patient safety. However, there is limited and contested evidence supporting the effectiveness of accreditation programs.

The Erlanger Health System, incorporated as the Chattanooga-Hamilton County Hospital Authority, a non-profit, public benefit corporation registered in the State of Tennessee, is a system of hospitals, physicians, and medical services based in Chattanooga, Tennessee. Erlanger's main location, Erlanger Baroness Hospital, is a tertiary referral hospital and Level I Trauma Center serving a 50,000 sq mi (130,000 km2) region of East Tennessee, North Georgia, North Alabama, and western North Carolina. The system provides critical care services to patients within a 150 mi (240 km) radius through six Life Force air ambulance helicopters, which are equipped to perform in-flight surgical procedures and transfusions.
The Patient-Centered Primary Care Collaborative (PCPCC) is a coalition of approximately 1,000 organizations and individuals, employers, consumer and patient/family advocacy groups, patient quality organizations, health plans, labor unions, hospitals, physicians, and other health professionals. They work on establishing the patient-centered medical home (PCMH) model, an approach to providing comprehensive care for children, youth, and adults. They are headquartered in downtown Washington, D.C.
Guided Care is a model of proactive, comprehensive health care for people with several chronic conditions. A form of medical home, the model has been developed and tested by a multidisciplinary team of experts at the Roger C. Lipitz Center for Integrated Health Care in the Johns Hopkins Bloomberg School of Public Health. Guided Care is provided by physician-nurse teams in primary care practices to the physicians' most complex patients, mainly older adults with chronic conditions and complicated health needs. It is designed to increase patients' quality of care and quality of life, while improving the efficiency of their use of health care resources, thus reducing their overall health care costs.
Bundled payment is the reimbursement of health care providers "on the basis of expected costs for clinically-defined episodes of care." It has been described as "a middle ground" between fee-for-service reimbursement and capitation, given that risk is shared between payer and provider. Bundled payments have been proposed in the health care reform debate in the United States as a strategy for reducing health care costs, especially during the Obama administration (2009–2016). Commercial payers have shown interest in bundled payments in order to reduce costs. In 2012, it was estimated that approximately one-third of the United States healthcare reimbursement used bundled methodology.
Clinical peer review, also known as medical peer review is the process by which health care professionals, including those in nursing and pharmacy, evaluate each other's clinical performance. A discipline-specific process may be referenced accordingly.
An accountable care organization (ACO) is a healthcare organization that ties provider reimbursements to quality metrics and reductions in the cost of care. ACOs in the United States are formed from a group of coordinated health-care practitioners. They use alternative payment models, normally, capitation. The organization is accountable to patients and third-party payers for the quality, appropriateness and efficiency of the health care provided. According to the Centers for Medicare and Medicaid Services, an ACO is "an organization of health care practitioners that agrees to be accountable for the quality, cost, and overall care of Medicare beneficiaries who are enrolled in the traditional fee-for-service program who are assigned to it".
Health care quality is a level of value provided by any health care resource, as determined by some measurement. As with quality in other fields, it is an assessment of whether something is good enough and whether it is suitable for its purpose. The goal of health care is to provide medical resources of high quality to all who need them; that is, to ensure good quality of life, cure illnesses when possible, to extend life expectancy, and so on. Researchers use a variety of quality measures to attempt to determine health care quality, including counts of a therapy's reduction or lessening of diseases identified by medical diagnosis, a decrease in the number of risk factors which people have following preventive care, or a survey of health indicators in a population who are accessing certain kinds of care.
The Oncology Care Model (OCM) is an episode-based payment system developed by the Center for Medicare and Medicaid Innovation. The multipayer model is designed for discrete instances of care, especially those involving chemotherapy, which triggers the six-month episode. The program combines fee-for-service (FFS) payments for established services, monthly payments for additional care under a structured guideline, and performance-based payments weighed against quality metrics and benchmarks.
Federal and state governments, insurance companies and other large medical institutions are heavily promoting the adoption of electronic health records. The US Congress included a formula of both incentives and penalties for EMR/EHR adoption versus continued use of paper records as part of the Health Information Technology for Economic and Clinical Health (HITECH) Act, enacted as part of the, American Recovery and Reinvestment Act of 2009.
Jacqueline Nwando Olayiwola is an American family physician, public health professional, author, professor, and women's empowerment leader. She is the Senior Vice President and Chief Health Equity Officer of Humana and a chair and Professor in the Department of Family Medicine at Ohio State University Wexner Medical Center. Prior to her appointment at OSU, she served as the inaugural Chief Clinical Transformation Officer for RubiconMD, an eConsult platform that improves primary care access to specialty care for underserved patients. Olayiwola is dedicated to serving marginalized patient populations and addressing the social determinants through community and technology-based infrastructures of healthcare reform. She has published articles on the use of eConsults and telehealth to provide underserved patients with primary care treatments so that they have a low cost and efficient means of reaching specialized care. Olayiwola has founded numerous non-profits and healthcare start-ups such as GIRLTALK Inc, Inspire Health Solutions LLC, and the Minority Women Professionals are MVPs Program. She has been recognized at the national and international level for her work and efforts to educate, advocate and provide healthcare to those in need. She was named Woman of the Year by the American Telemedicine Association in 2019, and received the Public Health Innovator Award from Harvard School of Public Health in 2019, as well as being named one of America's Top Family Doctors from 2007 to 2008 by the Consumers Research Council of America.




