Related Research Articles
Schizoaffective disorder is a mental disorder characterized by abnormal thought processes and an unstable mood. This diagnosis requires symptoms of both schizophrenia and a mood disorder: either bipolar disorder or depression. The main criterion is the presence of psychotic symptoms for at least two weeks without any mood symptoms. Schizoaffective disorder can often be misdiagnosed when the correct diagnosis may be psychotic depression, bipolar I disorder, schizophreniform disorder, or schizophrenia. This is a problem as treatment and prognosis differ greatly for most of these diagnoses.
A medical classification is used to transform descriptions of medical diagnoses or procedures into standardized statistical code in a process known as clinical coding. Diagnosis classifications list diagnosis codes, which are used to track diseases and other health conditions, inclusive of chronic diseases such as diabetes mellitus and heart disease, and infectious diseases such as norovirus, the flu, and athlete's foot. Procedure classifications list procedure code, which are used to capture interventional data. These diagnosis and procedure codes are used by health care providers, government health programs, private health insurance companies, workers' compensation carriers, software developers, and others for a variety of applications in medicine, public health and medical informatics, including:
Readiness for enhanced therapeutic regimen management is a NANDA approved nursing diagnosis which is defined as "A pattern of regulating and integrating into daily living a program(s) for treatment of illness and its sequelae that is sufficient for meeting health-related goals and can be strengthened." It was introduced at the 15th NANDA conference in 2002. Purpose: This book is devoted to a discussion of nursing diagnoses, outcomes, and interventions for older persons. As such, the diagnoses selected for the volume are not exhaustive, but represent a severely underdeveloped knowledge base. We have chosen diagnoses that are most prevalent, most difficult to treat, and/or most in need of further development to inform practicing nurses and nursing students and to improve the quality of life of older persons.
NANDA International is a professional organization of nurses interested in standardized nursing terminology, that was officially founded in 1982 and develops, researches, disseminates and refines the nomenclature, criteria, and taxonomy of nursing diagnoses. In 2002, NANDA became NANDA International in response to the broadening scope of its membership. NANDA International published Nursing Diagnosis quarterly, which became the International Journal of Nursing Terminologies and Classifications, and then later was reconceptualized as the International Journal of Nursing Knowledge, which remains in print today. The Membership Network Groups foster collaboration among NANDA-I members in countries and for languages: the German Language Group and the Dutch Language Group.

The nursing process is a modified scientific method which is a fundamental part of nursing practices in many countries around the world. Nursing practise was first described as a four-stage nursing process by Ida Jean Orlando in 1958. It should not be confused with nursing theories or health informatics. The diagnosis phase was added later.
Nursing assessment is the gathering of information about a patient's physiological, psychological, sociological, and spiritual status by a licensed Registered Nurse. Nursing assessment is the first step in the nursing process. A section of the nursing assessment may be delegated to certified nurses aides. Vitals and EKG's may be delegated to certified nurses aides or nursing techs. It differs from a medical diagnosis. In some instances, the nursing assessment is very broad in scope and in other cases it may focus on one body system or mental health. Nursing assessment is used to identify current and future patient care needs. It incorporates the recognition of normal versus abnormal body physiology. Prompt recognition of pertinent changes along with the skill of critical thinking allows the nurse to identify and prioritize appropriate interventions. An assessment format may already be in place to be used at specific facilities and in specific circumstances.
A nursing care plan provides direction on the type of nursing care the individual/family/community may need. The main focus of a nursing care plan is to facilitate standardised, evidence-based and holistic care. Nursing care plans have been used for quite a number of years for human purposes and are now also getting used in the veterinary profession. A care plan includes the following components: assessment, diagnosis, expected outcomes, interventions, rationale and evaluation.
In health care, diagnosis codes are used as a tool to group and identify diseases, disorders, symptoms, poisonings, adverse effects of drugs and chemicals, injuries and other reasons for patient encounters. Diagnostic coding is the translation of written descriptions of diseases, illnesses and injuries into codes from a particular classification. In medical classification, diagnosis codes are used as part of the clinical coding process alongside intervention codes. Both diagnosis and intervention codes are assigned by a health professional trained in medical classification such as a clinical coder or Health Information Manager.

In medicine, nodules are small firm lumps, usually greater than 1 cm in diameter. If filled with fluid they are referred to as cysts. Smaller raised soft tissue bumps may be termed papules.
In medicine, a biomarker is a measurable indicator of the severity or presence of some disease state. It may be defined as a "cellular, biochemical or molecular alteration in cells, tissues or fluids that can be measured and evaluated to indicate normal biological processes, pathogenic processes, or pharmacological responses to a therapeutic intervention." More generally a biomarker is anything that can be used as an indicator of a particular disease state or some other physiological state of an organism. According to the WHO, the indicator may be chemical, physical, or biological in nature - and the measurement may be functional, physiological, biochemical, cellular, or molecular.
A clinical nurse specialist (CNS) is an advanced practice nurse who can provide advice related to specific conditions or treatment pathways. According to the International Council of Nurses (ICN), an Advanced Practice Nurse is a registered nurse who has acquired the expert knowledge base, complex decision-making skills and clinical competencies for expanded practice, the characteristics of which are shaped by the context and/or country in which s/he is credentialed to practice.
The Nursing Interventions Classification (NIC) is a care classification system which describes the activities that nurses perform as a part of the planning phase of the nursing process associated with the creation of a nursing care plan.
The Nursing Outcomes Classification (NOC) is a classification system which describes patient outcomes sensitive to nursing intervention. The NOC is a system to evaluate the effects of nursing care as a part of the nursing process. The NOC contains 330 outcomes, and each with a label, a definition, and a set of indicators and measures to determine achievement of the nursing outcome and are included The terminology is an American Nurses' Association-recognized terminology, is included in the UMLS, and is HL7 registered.
Evidence-based nursing (EBN) is an approach to making quality decisions and providing nursing care based upon personal clinical expertise in combination with the most current, relevant research available on the topic. This approach is using evidence-based practice (EBP) as a foundation. EBN implements the most up to date methods of providing care, which have been proven through appraisal of high quality studies and statistically significant research findings. The goal of EBN is to improve the health and safety of patients while also providing care in a cost-effective manner to improve the outcomes for both the patient and the healthcare system. EBN is a process founded on the collection, interpretation, appraisal, and integration of valid, clinically significant, and applicable research. The evidence used to change practice or make a clinical decision can be separated into seven levels of evidence that differ in type of study and level of quality. To properly implement EBN, the knowledge of the nurse, the patient's preferences, and multiple studies of evidence must all be collaborated and utilized in order to produce an appropriate solution to the task at hand. These skills are taught in modern nursing education and also as a part of professional training.
A psychiatric assessment, or psychological screening, is the process of gathering information about a person within a psychiatric service, with the purpose of making a diagnosis. The assessment is usually the first stage of a treatment process, but psychiatric assessments may also be used for various legal purposes. The assessment includes social and biographical information, direct observations, and data from specific psychological tests. It is typically carried out by a psychiatrist, but it can be a multi-disciplinary process involving nurses, psychologists, occupational therapist, social workers, and licensed professional counselors.
Ambulatory care nursing is the nursing care of patients who receive treatment on an outpatient basis, ie they do not require admission to a hospital for an overnight stay. Ambulatory care includes those clinical, organizational and professional activities engaged in by registered nurses with and for individuals, groups, and populations who seek assistance with improving health and/or seek care for health-related problems. The American Academy of Ambulatory Care Nursing (AAACN) describes ambulatory care nursing as a comprehensive practice which is built on a broad knowledge base of nursing and health sciences, and applies clinical expertise rooted in the nursing process.
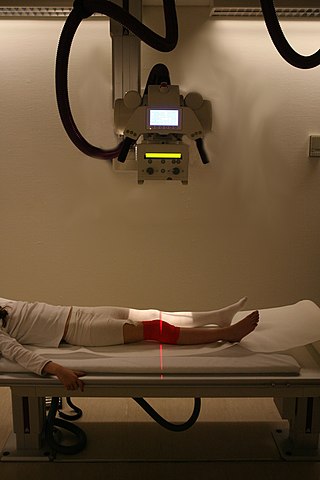
Medical diagnosis is the process of determining which disease or condition explains a person's symptoms and signs. It is most often referred to as a diagnosis with the medical context being implicit. The information required for a diagnosis is typically collected from a history and physical examination of the person seeking medical care. Often, one or more diagnostic procedures, such as medical tests, are also done during the process. Sometimes the posthumous diagnosis is considered a kind of medical diagnosis.
The Omaha System is a standardized health care terminology consisting of an assessment component, a care plan/services component, and an evaluation component. Approximately 22,000 health care practitioners, educators, and researchers use Omaha System to improve clinical practice, structure documentation, and analyze secondary data. Omaha System users from Canada, China, The Czech Republic, Estonia, Hong Kong, Japan, Mexico, New Zealand, The Netherlands, Turkey, the United States, and Wales, have presented at Omaha System International Conferences.
The Clinical Care Classification (CCC) System is a standardized, coded nursing terminology that identifies the discrete elements of nursing practice. The CCC provides a unique framework and coding structure. Used for documenting the plan of care; following the nursing process in all health care settings.
Nursing documentation is the record of nursing care that is planned and delivered to individual clients by qualified nurses or other caregivers under the direction of a qualified nurse. It contains information in accordance with the steps of the nursing process. Nursing documentation is the principal clinical information source to meet legal and professional requirements, care nurses' knowledge of nursing documentation, and is one of the most significant components in nursing care. Quality nursing documentation plays a vital role in the delivery of quality nursing care services through supporting better communication between different care team members to facilitate continuity of care and safety of the clients.
References
- ↑ Potter, Patricia A.; Perry, Anne Griffin; Stockert, Patricia A.; Hall, Amy M. (2013). Fundamentals of Nursing (8 ed.). St. Louis: Mosby. p. 223. ISBN 978-0-323-07933-4.
- ↑ NANDA International (professional association of nurses), Glossary of Terms.
- 1 2 3 4 5 6 7 Potter, Patricia A.; Perry, Anne Griffin; Stockert, Patricia A.; Hall, Amy M. (2013). Fundamentals of Nursing (8 ed.). St. Louis: Mosby. p. 222. ISBN 978-0-323-07933-4.
- 1 2 "NANDA International" . Retrieved 2023-12-09.
- ↑ Brokel, J & C Heath (2009). The value of nursing diagnoses in electronic health records. In Herdman, TH (Ed.), Nursing diagnoses: definitions and classification 2009–2011. Wiley-Blackwell: Singapore
- ↑ Weir-Hughes, Dickon (2010). "Nursing Diagnosis in Administration". Nursing Diagnoses 2009–2011, Custom: Definitions and Classification. John Wiley & Sons. pp. 37–40. ISBN 978-1-4443-2727-4.
- ↑ Zarzycka, D; Górajek-Jóźwik, J (2004). "Nursing diagnosis with the ICNP in the teaching context". International Nursing Review. 51 (4): 240–49. doi:10.1111/j.1466-7657.2004.00249.x. PMID 15530164.
- ↑ Lunney, Margaret (2008). "The Need for International Nursing Diagnosis Research and a Theoretical Framework". International Journal of Nursing Terminologies and Classifications. 19 (1): 28–34. doi:10.1111/j.1744-618X.2007.00076.x. PMID 18331482.
- ↑ "Standardized Nursing Language: What Does It Mean for Nursing Practice?". www.nursingworld.org. Retrieved 2016-05-17.
- ↑ "FindArticles.com | CBSi". findarticles.com. Retrieved 2016-05-17.
- ↑ Herdman, TH (Ed.) (2009). Nursing diagnoses: definitions and classification 2009–2011. Wiley-Blackwell: Singapore.
- ↑ Potter, Patricia A.; Perry, Anne Griffin; Stockert, Patricia A.; Hall, Amy M. (2013). Fundamentals of Nursing (8 ed.). St. Louis: Mosby. p. 224. ISBN 978-0-323-07933-4.
- ↑ "Nursing Process Steps". www.nursingprocess.org. Retrieved 2016-05-17.
- ↑ Fima, Odile; Langlassé, Armelle (1994). "Proposition d'un diagnostic infirmier: constipation colique chronique chez la personne âgée" [Proposition for nursing diagnosis. Chronic colonic constipation in the elderly]. Soins (in French) (584): 30–4. PMID 8029726. INIST 4073742.
- ↑ "American Nurses Association". www.nursingworld.org. Retrieved 2016-05-17.
- ↑ Potter, Patricia A.; Perry, Anne Griffin; Stockert, Patricia A.; Hall, Amy M. (2013). Fundamentals of Nursing. St. Louis: Mosby. p. 2225edition=8. ISBN 978-0-323-07933-4.