Analytical chemistry studies and uses instruments and methods to separate, identify, and quantify matter. In practice, separation, identification or quantification may constitute the entire analysis or be combined with another method. Separation isolates analytes. Qualitative analysis identifies analytes, while quantitative analysis determines the numerical amount or concentration.

Clinical chemistry is a division in medical laboratory sciences focusing on qualitative tests of important compounds, referred to as analytes or markers, in bodily fluids and tissues using analytical techniques and specialized instruments. This interdisciplinary field includes knowledge from medicine, biology, chemistry, biomedical engineering, informatics, and an applied form of biochemistry.

A blood cell, also called a hematopoietic cell, hemocyte, or hematocyte, is a cell produced through hematopoiesis and found mainly in the blood. Major types of blood cells include red blood cells (erythrocytes), white blood cells (leukocytes), and platelets (thrombocytes). Together, these three kinds of blood cells add up to a total 45% of the blood tissue by volume, with the remaining 55% of the volume composed of plasma, the liquid component of blood.

The erythrocyte sedimentation rate is the rate at which red blood cells in anticoagulated whole blood descend in a standardized tube over a period of one hour. It is a common hematology test, and is a non-specific measure of inflammation. To perform the test, anticoagulated blood is traditionally placed in an upright tube, known as a Westergren tube, and the distance which the red blood cells fall is measured and reported in millimetres at the end of one hour.
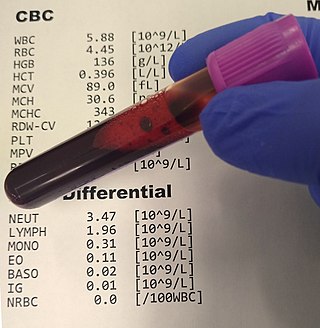
A complete blood count (CBC), also known as a full blood count (FBC), is a set of medical laboratory tests that provide information about the cells in a person's blood. The CBC indicates the counts of white blood cells, red blood cells and platelets, the concentration of hemoglobin, and the hematocrit. The red blood cell indices, which indicate the average size and hemoglobin content of red blood cells, are also reported, and a white blood cell differential, which counts the different types of white blood cells, may be included.

The Hitachi 917 is an automated biochemistry analyser utilise medical laboratories to process biological fluid specimens, such as urine, cerebrospinal fluid, and most commonly, blood.

Serum is the fluid and solvent component of blood which does not play a role in clotting. It may be defined as blood plasma without the clotting factors, or as blood with all cells and clotting factors removed. Serum contains all proteins except clotting factors, including all electrolytes, antibodies, antigens, hormones; and any exogenous substances. Serum also does not contain all the formed elements of blood, which include blood cells and platelets.
A blood bank is a center where blood gathered as a result of blood donation is stored and preserved for later use in blood transfusion. The term "blood bank" typically refers to a department of a hospital usually within a clinical pathology laboratory where the storage of blood product occurs and where pre-transfusion and blood compatibility testing is performed. However, it sometimes refers to a collection center, and some hospitals also perform collection. Blood banking includes tasks related to blood collection, processing, testing, separation, and storage.

A blood smear, peripheral blood smear or blood film is a thin layer of blood smeared on a glass microscope slide and then stained in such a way as to allow the various blood cells to be examined microscopically. Blood smears are examined in the investigation of hematological (blood) disorders and are routinely employed to look for blood parasites, such as those of malaria and filariasis.
An assay is an investigative (analytic) procedure in laboratory medicine, mining, pharmacology, environmental biology and molecular biology for qualitatively assessing or quantitatively measuring the presence, amount, or functional activity of a target entity. The measured entity is often called the analyte, the measurand, or the target of the assay. The analyte can be a drug, biochemical substance, chemical element or compound, or cell in an organism or organic sample. An assay usually aims to measure an analyte's intensive property and express it in the relevant measurement unit.

The prothrombin time (PT) – along with its derived measures of prothrombin ratio (PR) and international normalized ratio (INR) – is an assay for evaluating the extrinsic pathway and common pathway of coagulation. This blood test is also called protime INR and PT/INR. They are used to determine the clotting tendency of blood, in such things as the measure of warfarin dosage, liver damage, and vitamin K status. PT measures the following coagulation factors: I (fibrinogen), II (prothrombin), V (proaccelerin), VII (proconvertin), and X.

Apheresis is a medical technology in which the blood of a person is passed through an apparatus that separates out one particular constituent and returns the remainder to the circulation. It is thus an extracorporeal therapy.
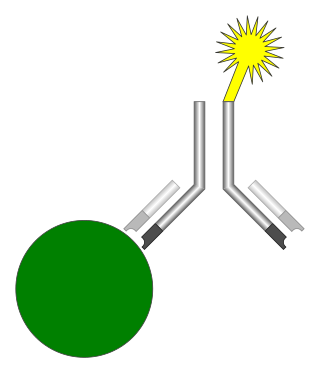
An immunoassay (IA) is a biochemical test that measures the presence or concentration of a macromolecule or a small molecule in a solution through the use of an antibody (usually) or an antigen (sometimes). The molecule detected by the immunoassay is often referred to as an "analyte" and is in many cases a protein, although it may be other kinds of molecules, of different sizes and types, as long as the proper antibodies that have the required properties for the assay are developed. Analytes in biological liquids such as serum or urine are frequently measured using immunoassays for medical and research purposes.

The AutoAnalyzer is an automated analyzer using a flow technique called continuous flow analysis (CFA), or more correctly segmented flow analysis (SFA) first made by the Technicon Corporation. The instrument was invented in 1957 by Leonard Skeggs, PhD and commercialized by Jack Whitehead's Technicon Corporation. The first applications were for clinical analysis, but methods for industrial and environmental analysis soon followed. The design is based on segmenting a continuously flowing stream with air bubbles.
Thromboplastin (TPL) is derived from cell membranes and is a mixture of both phospholipids and tissue factor, neither of which are enzymes. Thromboplastin acts on and accelerates the activity of Factor Xa, also known as thrombokinase, aiding blood coagulation through catalyzing the conversion of prothrombin to thrombin. Thromboplastin is found in brain, lung, and other tissues and especially in blood platelets.
Thromboelastometry (TEM), previously named rotational thromboelastography (ROTEG) or rotational thromboelastometry (ROTEM), is an established viscoelastic method for hemostasis testing in whole blood. It is a modification of traditional thromboelastography (TEG).
Pseudothrombocytopenia (PTCP) or spurious thrombocytopenia is an in-vitro sampling problem which may mislead the diagnosis towards the more critical condition of thrombocytopenia. The phenomenon occurs when the anticoagulant used while testing the blood sample causes clumping of platelets which mimics a low platelet count. The phenomenon has first been reported in 1969.
Hematology analyzers are used to count and identify blood cells at high speed with accuracy. During the 1950s, laboratory technicians counted each individual blood cell underneath a microscope. Tedious and inconsistent, this was replaced with the first, very basic hematology analyzer, engineered by Wallace H. Coulter. The early hematology analyzers relied on Coulter's principle. However, they have evolved to encompass numerous techniques.

A white blood cell differential is a medical laboratory test that provides information about the types and amounts of white blood cells in a person's blood. The test, which is usually ordered as part of a complete blood count (CBC), measures the amounts of the five normal white blood cell types – neutrophils, lymphocytes, monocytes, eosinophils and basophils – as well as abnormal cell types if they are present. These results are reported as percentages and absolute values, and compared against reference ranges to determine whether the values are normal, low, or high. Changes in the amounts of white blood cells can aid in the diagnosis of many health conditions, including viral, bacterial, and parasitic infections and blood disorders such as leukemia.

Celloscope automated cell counter was developed in the 50s for enumeration of erythrocytes, leukocytes, and thrombocytes in blood samples. Together with the Coulter counter, the Celloscope analyzer can be considered one of the predecessors of today’s automated hematology analyzers, as the principle of the electrical impedance method is still utilized in cell counters installed in clinical laboratories around the world.