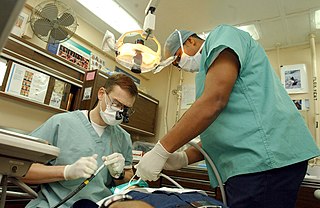
A dentist, also known as a dental surgeon, is a health care professional who specializes in dentistry, the branch of medicine focused on the teeth, gums, and mouth. The dentist's supporting team aids in providing oral health services. The dental team includes dental assistants, dental hygienists, dental technicians, and sometimes dental therapists.

A root canal is the naturally occurring anatomic space within the root of a tooth. It consists of the pulp chamber, the main canal(s), and more intricate anatomical branches that may connect the root canals to each other or to the surface of the root.
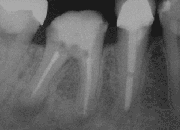
A root end surgery, also known as apicoectomy, apicectomy, retrograde root canal treatment or root-end filling, is an endodontic surgical procedure whereby a tooth's root tip is removed and a root end cavity is prepared and filled with a biocompatible material. It is an example of a periradicular surgery.
Dens invaginatus (DI), also known as tooth within a tooth, is a rare dental malformation and a developmental anomaly where there is an infolding of enamel into dentin. The prevalence of this condition is 0.3 - 10%, affecting males more frequently than females. The condition presents in two forms, coronal involving tooth crown and radicular involving tooth root, with the former being more common.
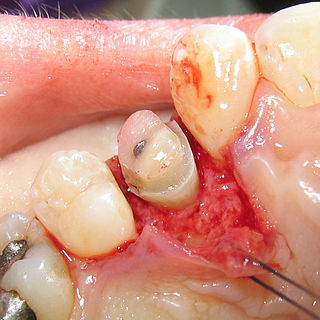
Crown lengthening is a surgical procedure performed by a dentist, or more frequently a periodontist, where more tooth is exposed by removing some of the gingival margin (gum) and supporting bone. Crown lengthening can also be achieved orthodontically by extruding the tooth.

Root canal treatment is a treatment sequence for the infected pulp of a tooth which is intended to result in the elimination of infection and the protection of the decontaminated tooth from future microbial invasion. Root canals, and their associated pulp chamber, are the physical hollows within a tooth that are naturally inhabited by nerve tissue, blood vessels and other cellular entities. Together, these items constitute the dental pulp.
Mineral trioxide aggregate (MTA) was developed for use as a dental root repair material by Mahmoud Torabinejad. It is formulated from commercial Portland cement, combined with bismuth oxide powder for radio-opacity. MTA is used for creating apical plugs during apexification, repairing root perforations during root canal therapy, and treating internal root resorption. This can be used for root-end filling material and as pulp capping material. Originally, MTA was dark gray in color, but white versions have been on the market since 2002.
Pulpotomy is a minimally invasive procedure performed in children on a primary tooth with extensive caries but without evidence of root pathology. The minimally invasive endodontic techniques of vital pulp therapy (VPT) are based on improved understanding of the capacity of pulp (nerve) tissues to heal and regenerate plus the availability of advanced endodontic materials. During the caries removal, this results in a carious or mechanical pulp exposure (bleeding) from the cavity. During pulpotomy, the inflamed/diseased pulp tissue is removed from the coronal pulp chamber of the tooth leaving healthy pulp tissue which is dressed with a long-term clinically successful medicament that maintains the survival of the pulp and promotes repair. There are various types of medicament placed above the vital pulp such as Buckley's Solution of formocresol, ferric sulfate, calcium hydroxide or mineral trioxide aggregate (MTA). MTA is a more recent material used for pulpotomies with a high rate of success, better than formocresol or ferric sulfate. It is also recommended to be the preferred pulpotomy agent in the future. After the coronal pulp chamber is filled, the tooth is restored with a filling material that seals the tooth from microleakage, such as a stainless steel crown which is the most effective long-term restoration. However, if there is sufficient remaining supporting tooth structure, other filling materials such as amalgam or composite resin can provide a functional alternative when the primary tooth has a life span of two years or less. The medium- to long-term treatment outcomes of pulpotomy in symptomatic permanent teeth with caries, especially in young people, indicate that pulpotomy can be a potential alternative to root canal therapy (RCT).
Pulp necrosis is a clinical diagnostic category indicating the death of cells and tissues in the pulp chamber of a tooth with or without bacterial invasion. It is often the result of many cases of dental trauma, caries and irreversible pulpitis.
Dental pulpal testing is a clinical and diagnostic aid used in dentistry to help establish the health of the dental pulp within the pulp chamber and root canals of a tooth. Such investigations are important in aiding dentists in devising a treatment plan for the tooth being tested.
A phoenix abscess is an acute exacerbation of a chronic periapical lesion. It is a dental abscess that can occur immediately following root canal treatment. Another cause is due to untreated necrotic pulp. It is also the result of inadequate debridement during the endodontic procedure. Risk of occurrence of a phoenix abscess is minimised by correct identification and instrumentation of the entire root canal, ensuring no missed anatomy.

An operating microscope or surgical microscope is an optical microscope specifically designed to be used in a surgical setting, typically to perform microsurgery.
In dentistry, the smear layer is a layer found on root canal walls after root canal instrumentation. It consists of microcrystalline and organic particle debris. It was first described in 1975 and research has been performed since then to evaluate its importance in bacteria penetration into the dentinal tubules and its effects on endodontic treatment. More broadly, it is the organic layer found over all hard tooth surfaces.

Regenerative endodontic procedures is defined as biologically based procedures designed to replace damaged structures such as dentin, root structures, and cells of the pulp-dentin complex. This new treatment modality aims to promote normal function of the pulp. It has become an alternative to heal apical periodontitis. Regenerative endodontics is the extension of root canal therapy. Conventional root canal therapy cleans and fills the pulp chamber with biologically inert material after destruction of the pulp due to dental caries, congenital deformity or trauma. Regenerative endodontics instead seeks to replace live tissue in the pulp chamber. The ultimate goal of regenerative endodontic procedures is to regenerate the tissues and the normal function of the dentin-pulp complex.

Pulp capping is a technique used in dental restorations to prevent the dental pulp from necrosis, after being exposed, or nearly exposed during a cavity preparation, from a traumatic injury, or by a deep cavity that reaches the center of the tooth causing the pulp to die. When dental caries is removed from a tooth, all or most of the infected and softened enamel and dentin are removed. This can lead to the pulp of the tooth either being exposed or nearly exposed which causes pulpitis (inflammation). Pulpitis, in turn, can become irreversible, leading to pain and pulp necrosis, and necessitating either root canal treatment or extraction. The ultimate goal of pulp capping or stepwise caries removal is to protect a healthy dental pulp and avoid the need for root canal therapy.
In the dental specialty of endodontics, periradicular surgery is surgery to the external root surface. Examples of periradicular surgery include apicoectomy, root resection, repair of root perforation or resorption defects, removal of broken fragments of the tooth or a filling material, and exploratory surgery to look for root fractures.
Periapical granuloma, also sometimes referred to as a radicular granuloma or apical granuloma, is an inflammation at the tip of a dead (nonvital) tooth. It is a lesion or mass that typically starts out as an epithelial lined cyst, and undergoes an inward curvature that results in inflammation of granulation tissue at the root tips of a dead tooth. This is usually due to dental caries or a bacterial infection of the dental pulp. Periapical granuloma is an infrequent disorder that has an occurrence rate between 9.3 to 87.1 percent. Periapical granuloma is not a true granuloma due to the fact that it does not contain granulomatous inflammation; however, periapical granuloma is a common term used.
Tooth replantation is a form of restorative dentistry in which an avulsed or luxated tooth is reinserted and secured into its socket through a combination of dental procedures. The purposes of tooth replantation is to resolve tooth loss and preserve the natural landscape of the teeth. Whilst variations of the procedure exist including, Allotransplantation, where a tooth is transferred from one individual to another individual of the same species. It is a largely defunct practice due to the improvements made within the field of dentistry and due to the risks and complications involved including the transmission of diseases such as syphilis, histocompatibility, as well as the low success rate of the procedure, has resulted in its practice being largely abandoned. Autotransplantation, otherwise known as intentional replantation in dentistry, is defined as the surgical movement of a tooth from one site on an individual to another location in the same individual. While rare, modern dentistry uses replantation as a form of proactive care to prevent future complications and protect the natural dentition in cases where root canal and surgical endodontic treatments are problematic. In the modern context, tooth replantation most often refers to reattachment of an avulsed or luxated permanent tooth into its original socket.
Apexification is a method of dental treatment to induce a calcific barrier in a root with incomplete formation or open apex of a tooth with necrotic pulp. Pulpal involvement usually occurs as a consequence of trauma or caries involvement of young or immature permanent teeth. As a sequelae of untreated pulp involvement, loss of pulp vitality or necrotic pulp took place for the involved teeth.
Root resection or root amputation is a type of periradicular surgery in which an entire root of a multiroot tooth is removed. It contrasts with an apicoectomy, where only the tip of the root is removed, and hemisection, where a root and its overlying portion of the crown are separated from the rest of the tooth, and optionally removed.









