
Expressive aphasia, also known as Broca's aphasia, is a type of aphasia characterized by partial loss of the ability to produce language, although comprehension generally remains intact. A person with expressive aphasia will exhibit effortful speech. Speech generally includes important content words but leaves out function words that have more grammatical significance than physical meaning, such as prepositions and articles. This is known as "telegraphic speech". The person's intended message may still be understood, but their sentence will not be grammatically correct. In very severe forms of expressive aphasia, a person may only speak using single word utterances. Typically, comprehension is mildly to moderately impaired in expressive aphasia due to difficulty understanding complex grammar.
Hemiparesis, or unilateral paresis, is weakness of one entire side of the body. Hemiplegia is, in its most severe form, complete paralysis of half of the body. Hemiparesis and hemiplegia can be caused by different medical conditions, including congenital causes, trauma, tumors, or stroke.
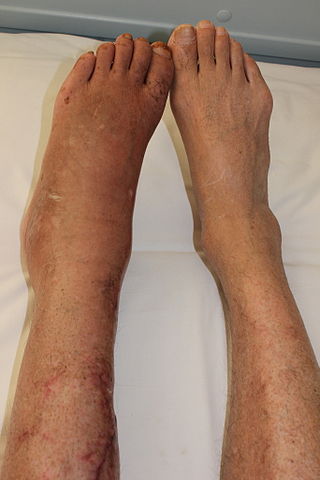
Complex regional pain syndrome is a form of amplified musculoskeletal pain syndrome (AMPS) in which pain from a physical trauma outlasts the expected recovery time. The symptoms and associations of Type 1 and 2 are the same except Type 2 is associated with nerve injury. This type of AMPS must include a specific cause and is often accompanied by various visible changes, such as skin changes. The lack of an observed cause for the condition, or the lack of visible symptoms, creates the diagnosis of diffuse amplified pain.

Apraxia is a motor disorder caused by damage to the brain, which causes difficulty with motor planning to perform tasks or movements. The nature of the damage determines the disorder's severity, and the absence of sensory loss or paralysis helps to explain the level of difficulty. Children may be born with apraxia; its cause is unknown, and symptoms are usually noticed in the early stages of development. Apraxia occurring later in life, known as acquired apraxia, is typically caused by traumatic brain injury, stroke, dementia, Alzheimer's disease, brain tumor, or other neurodegenerative disorders. The multiple types of apraxia are categorized by the specific ability and/or body part affected.

In medicine, a prosthesis, or a prosthetic implant, is an artificial device that replaces a missing body part, which may be lost through trauma, disease, or a condition present at birth. Prostheses are intended to restore the normal functions of the missing body part. Amputee rehabilitation is primarily coordinated by a physiatrist as part of an inter-disciplinary team consisting of physiatrists, prosthetists, nurses, physical therapists, and occupational therapists. Prostheses can be created by hand or with computer-aided design (CAD), a software interface that helps creators design and analyze the creation with computer-generated 2-D and 3-D graphics as well as analysis and optimization tools.

A phantom limb is the sensation that an amputated or missing limb is still attached. Approximately 80–100% of individuals with an amputation experience sensations in their amputated limb. However, only a small percentage will experience painful phantom limb sensation. These sensations are relatively common in amputees and usually resolve within two to three years without treatment. Research continues to explore the underlying mechanisms of phantom limb pain (PLP) and effective treatment options.

Vilayanur Subramanian Ramachandran is an Indian-American neuroscientist. He is known for his wide-ranging experiments and theories in behavioral neurology, including the invention of the mirror box. Ramachandran is a distinguished professor in UCSD's Department of Psychology, where he is the director of the Center for Brain and Cognition.
Anosognosia is a condition in which a person with a disability is cognitively unaware of having it due to an underlying physical condition. Anosognosia results from physiological damage to brain structures, typically to the parietal lobe or a diffuse lesion on the fronto-temporal-parietal area in the right hemisphere, and is thus a neuropsychiatric disorder. A deficit of self-awareness, the term was first coined by the neurologist Joseph Babinski in 1914, in order to describe the unawareness of hemiplegia.
The primary goals of stroke management are to reduce brain injury and promote maximum patient recovery. Rapid detection and appropriate emergency medical care are essential for optimizing health outcomes. When available, patients are admitted to an acute stroke unit for treatment. These units specialize in providing medical and surgical care aimed at stabilizing the patient's medical status. Standardized assessments are also performed to aid in the development of an appropriate care plan. Current research suggests that stroke units may be effective in reducing in-hospital fatality rates and the length of hospital stays.
The Bobath concept is an approach to neurological rehabilitation that is applied in patient assessment and treatment. The goal of applying the Bobath concept is to promote motor learning for efficient motor control in various environments, thereby improving participation and function. This is done through specific patient handling skills to guide patients through the initiation and completing of intended tasks. This approach to neurological rehabilitation is multidisciplinary, primarily involving physiotherapists, occupational therapists, and speech and language therapists. In the United States, the Bobath concept is also known as 'neuro-developmental treatment' (NDT).
Phantom pain is a painful perception that an individual experiences relating to a limb or an organ that is not physically part of the body, either because it was removed or was never there in the first place.
Neuroplasticity, also known as neural plasticity or brain plasticity, is the ability of neural networks in the brain to change through growth and reorganization. It is when the brain is rewired to function in some way that differs from how it previously functioned. These changes range from individual neuron pathways making new connections, to systematic adjustments like cortical remapping or neural oscillation. Other forms of neuroplasticity include homologous area adaptation, cross modal reassignment, map expansion, and compensatory masquerade. Examples of neuroplasticity include circuit and network changes that result from learning a new ability, information acquisition, environmental influences, practice, and psychological stress.
Monoplegia is paralysis of a single limb, usually an arm. Common symptoms associated with monoplegic patients are weakness, numbness, and pain in the affected limb. Monoplegia is a type of paralysis that falls under hemiplegia. While hemiplegia is paralysis of half of the body, monoplegia is localized to a single limb or to a specific region of the body. Monoplegia of the upper limb is sometimes referred to as brachial monoplegia, and that of the lower limb is called crural monoplegia. Monoplegia in the lower extremities is not as common of an occurrence as in the upper extremities. Monoparesis is a similar, but less severe, condition because one limb is very weak, not paralyzed. For more information, see paresis.
Virtual reality therapy (VRT), also known as virtual reality immersion therapy (VRIT), simulation for therapy (SFT), virtual reality exposure therapy (VRET), and computerized CBT (CCBT), is the use of virtual reality technology for psychological or occupational therapy and in affecting virtual rehabilitation. Patients receiving virtual reality therapy navigate through digitally created environments and complete specially designed tasks often tailored to treat a specific ailment; and is designed to isolate the user from their surrounding sensory inputs and give the illusion of immersion inside a computer-generated, interactive virtual environment. This technology has a demonstrated clinical benefit as an adjunctive analgesic during burn wound dressing and other painful medical procedures. Technology can range from a simple PC and keyboard setup, to a modern virtual reality headset. It is widely used as an alternative form of exposure therapy, in which patients interact with harmless virtual representations of traumatic stimuli in order to reduce fear responses. It has proven to be especially effective at treating PTSD, and shows considerable promise in treating a variety of neurological and physical conditions. Virtual reality therapy has also been used to help stroke patients regain muscle control, to treat other disorders such as body dysmorphia, and to improve social skills in those diagnosed with autism.
Constraint-induced movement therapy is a form of rehabilitation therapy that improves upper extremity function in stroke and other central nervous system damage patients by increasing the use of their affected upper limb. Due to its high duration of treatment, the therapy has been found to frequently be infeasible when attempts have been made to apply it to clinical situations, and both patients and treating clinicians have reported poor compliance and concerns with patient safety. In the United States, the high duration of the therapy has also made the therapy not able to get reimbursed in most clinical environments.
Body schema is an organism's internal model of its own body, including the position of its limbs. The neurologist Sir Henry Head originally defined it as a postural model of the body that actively organizes and modifies 'the impressions produced by incoming sensory impulses in such a way that the final sensation of body position, or of locality, rises into consciousness charged with a relation to something that has happened before'. As a postural model that keeps track of limb position, it plays an important role in control of action.
Aquatic therapy refers to treatments and exercises performed in water for relaxation, fitness, physical rehabilitation, and other therapeutic benefit. Typically a qualified aquatic therapist gives constant attendance to a person receiving treatment in a heated therapy pool. Aquatic therapy techniques include Ai Chi, Aqua Running, Bad Ragaz Ring Method, Burdenko Method, Halliwick, Watsu, and other aquatic bodywork forms. Therapeutic applications include neurological disorders, spine pain, musculoskeletal pain, postoperative orthopedic rehabilitation, pediatric disabilities, and pressure ulcers.
Cortical remapping, also referred to as cortical reorganization, is the process by which an existing cortical map is affected by a stimulus resulting in the creating of a 'new' cortical map. Every part of the body is connected to a corresponding area in the brain which creates a cortical map. When something happens to disrupt the cortical maps such as an amputation or a change in neuronal characteristics, the map is no longer relevant. The part of the brain that is in charge of the amputated limb or neuronal change will be dominated by adjacent cortical regions that are still receiving input, thus creating a remapped area. Remapping can occur in the sensory or motor system. The mechanism for each system may be quite different. Cortical remapping in the somatosensory system happens when there has been a decrease in sensory input to the brain due to deafferentation or amputation, as well as a sensory input increase to an area of the brain. Motor system remapping receives more limited feedback that can be difficult to interpret.

Tactile hallucination is the false perception of tactile sensory input that creates a hallucinatory sensation of physical contact with an imaginary object. It is caused by the faulty integration of the tactile sensory neural signals generated in the spinal cord and the thalamus and sent to the primary somatosensory cortex (SI) and secondary somatosensory cortex (SII). Tactile hallucinations are recurrent symptoms of neurological diseases such as schizophrenia, Parkinson's disease, Ekbom's syndrome and delirium tremens. Patients who experience phantom limb pains also experience a type of tactile hallucination. Tactile hallucinations are also caused by drugs such as cocaine and alcohol.

Limb telescoping is the progressive shortening of a phantom limb as the cortical regions are reorganized following an amputation. During this reorganization, proximal portions of the residual limb are perceived as more distal parts of the phantom limb. Such effect is responsible for increased phantom pain due to the discrepancy between the patient’s body perception and their actual body. This effect may last from weeks up to years after post-amputation.











