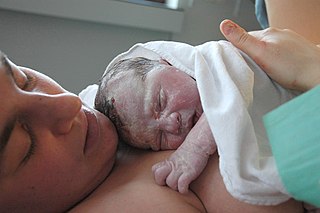
Childbirth, also known as labour and delivery, is the completion of pregnancy where one or more babies exits the internal environment of the mother via vaginal delivery or caesarean section. In 2019, there were about 140.11 million births globally. In the developed countries, most deliveries occur in hospitals, while in the developing countries most are home births.

Postpartum depression (PPD), also called postnatal depression, is a type of mood disorder associated with childbirth, which can affect both sexes. Symptoms may include extreme sadness, low energy, anxiety, crying episodes, irritability, and changes in sleeping or eating patterns. Onset is typically between one week and one month following childbirth. PPD can also negatively affect the newborn child.

Oxytocin is a peptide hormone and neuropeptide normally produced in the hypothalamus and released by the posterior pituitary. Present in animals since early stages of evolution, in humans it plays roles in behavior that include social bonding, reproduction, childbirth, and the period after childbirth. Oxytocin is released into the bloodstream as a hormone in response to sexual activity and during labour. It is also available in pharmaceutical form. In either form, oxytocin stimulates uterine contractions to speed up the process of childbirth. In its natural form, it also plays a role in bonding with the baby and milk production. Production and secretion of oxytocin is controlled by a positive feedback mechanism, where its initial release stimulates production and release of further oxytocin. For example, when oxytocin is released during a contraction of the uterus at the start of childbirth, this stimulates production and release of more oxytocin and an increase in the intensity and frequency of contractions. This process compounds in intensity and frequency and continues until the triggering activity ceases. A similar process takes place during lactation and during sexual activity.

The postpartum period begins after childbirth and is typically considered to end within 6 weeks as the mother's body, including hormone levels and uterus size, returns to a non-pregnant state. The terms puerperium, puerperal period, or immediate postpartum period are commonly used to refer to the first six weeks following childbirth. The World Health Organization (WHO) describes the postnatal period as the most critical and yet the most neglected phase in the lives of mothers and babies; most maternal and newborn deaths occur during this period.
Biological half-life is the time taken for concentration of a biological substance to decrease from its maximum concentration (Cmax) to half of Cmax in the blood plasma, and is denoted by the abbreviation .
Psychoneuroendocrinology is the clinical study of hormone fluctuations and their relationship to human behavior. It may be viewed from the perspective of psychiatry, where in certain mood disorders, there are associated neuroendocrine or hormonal changes affecting the brain. It may also be viewed from the perspective of endocrinology, where certain endocrine disorders can be associated with negative health outcomes and psychiatric illness. Brain dysfunctions associated with the hypothalamus-pituitary-adrenal axis HPA axis can affect the endocrine system, which in turn can result in physiological and psychological symptoms. This complex blend of psychiatry, psychology, neurology, biochemistry, and endocrinology is needed to comprehensively understand and treat symptoms related to the brain, endocrine system (hormones), and psychological health..

Postpartum bleeding or postpartum hemorrhage (PPH) is often defined as the loss of more than 500 ml or 1,000 ml of blood following childbirth. Some have added the requirement that there also be signs or symptoms of low blood volume for the condition to exist. Signs and symptoms may initially include: an increased heart rate, feeling faint upon standing, and an increased breathing rate. As more blood is lost, the patient may feel cold, blood pressure may drop, and they may become restless or unconscious. The condition can occur up to six weeks following delivery.

Carbetocin, sold under the brand names Pabal among others, is a medication used to prevent excessive bleeding after childbirth, particularly following Cesarean section. It appears to work as well as oxytocin. Due to it being less economical than other options, use is not recommended by NHS Scotland. It is given by injection into a vein or muscle.

Allopregnanolone is a naturally occurring neurosteroid which is made in the body from the hormone progesterone. As a medication, allopregnanolone is referred to as brexanolone, sold under the brand name Zulresso, and used to treat postpartum depression. It is given by injection into a vein.

Esketamine, also known as (S)-ketamine or S(+)-ketamine, is the S(+) enantiomer of ketamine, is a dissociative hallucinogen drug used as a general anesthetic and as an antidepressant for treatment of depression. It is sold under the brand names Spravato, Ketanest, among others. Esketamine is the active enantiomer of ketamine in terms of NMDA receptor antagonism and is more potent than racemic ketamine.

Postpartum psychosis(PPP), also known as puerperal psychosis or peripartum psychosis, involves the abrupt onset of psychotic symptoms shortly following childbirth, typically within two weeks of delivery but less than 4 weeks postpartum. PPP is a condition currently represented under "Brief Psychotic Disorder" in the Diagnostic and Statistical Manual of Mental Disorders, Volume V (DSM-V). Symptoms may include delusions, hallucinations, disorganized speech (e.g, incoherent speech), and/or abnormal motor behavior (e.g., catatonia). Other symptoms frequently associated with PPP include confusion, disorganized thought, severe difficulty sleeping, variations of mood disorders (including depression, agitation, mania, or a combination of the above), as well as cognitive features such as consciousness that comes and goes (waxing and waning) or disorientation.

Demoxytocin (INN), also known as desaminooxytocin or deaminooxytocin, as well as 1-(3-mercaptopropanoic acid)oxytocin ([Mpa1]OT), is an oxytocic peptide drug that is used to induce labor, promote lactation, and to prevent and treat puerperal (postpartum) mastitis. Demoxytocin is a synthetic analogue of oxytocin and has similar activities, but is more potent and has a longer half-life in comparison. Unlike oxytocin, which is given via intravenous injection, demoxytocin is administered as a buccal tablet formulation.
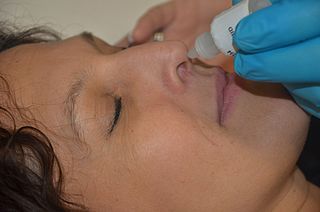
Nasal administration, popularly known as snorting, is a route of administration in which drugs are insufflated through the nose. It can be a form of either topical administration or systemic administration, as the drugs thus locally delivered can go on to have either purely local or systemic effects. Nasal sprays are locally acting drugs such as decongestants for cold and allergy treatment, whose systemic effects are usually minimal. Examples of systemically active drugs available as nasal sprays are migraine drugs, rescue medications for overdose and seizure emergencies, nicotine replacement, and hormone treatments.
A uterotonic, also known as an oxytocic or ecbolic, is a type of medication used to induce contraction or greater tonicity of the uterus. Uterotonics are used both to induce labor and to reduce postpartum hemorrhage.
Thyroid disease in pregnancy can affect the health of the mother as well as the child before and after delivery. Thyroid disorders are prevalent in women of child-bearing age and for this reason commonly present as a pre-existing disease in pregnancy, or after childbirth. Uncorrected thyroid dysfunction in pregnancy has adverse effects on fetal and maternal well-being. The deleterious effects of thyroid dysfunction can also extend beyond pregnancy and delivery to affect neurointellectual development in the early life of the child. Due to an increase in thyroxine binding globulin, an increase in placental type 3 deioidinase and the placental transfer of maternal thyroxine to the fetus, the demand for thyroid hormones is increased during pregnancy. The necessary increase in thyroid hormone production is facilitated by high human chorionic gonadotropin (hCG) concentrations, which bind the TSH receptor and stimulate the maternal thyroid to increase maternal thyroid hormone concentrations by roughly 50%. If the necessary increase in thyroid function cannot be met, this may cause a previously unnoticed (mild) thyroid disorder to worsen and become evident as gestational thyroid disease. Currently, there is not enough evidence to suggest that screening for thyroid dysfunction is beneficial, especially since treatment thyroid hormone supplementation may come with a risk of overtreatment. After women give birth, about 5% develop postpartum thyroiditis which can occur up to nine months afterwards. This is characterized by a short period of hyperthyroidism followed by a period of hypothyroidism; 20–40% remain permanently hypothyroid.

Parental experience, as well as changing hormone levels during pregnancy and postpartum, cause changes in the parental brain. Displaying maternal sensitivity towards infant cues, processing those cues and being motivated to engage socially with her infant and attend to the infant's needs in any context could be described as mothering behavior and is regulated by many systems in the maternal brain. Research has shown that hormones such as oxytocin, prolactin, estradiol and progesterone are essential for the onset and the maintenance of maternal behavior in rats, and other mammals as well. Mothering behavior has also been classified within the basic drives. Less is known about the paternal brain, but changes in the father's brain occur alongside the mother once the offspring is born.
Endocrinology of parenting has been the subject of considerable study with focus both on human females and males and on females and males of other mammalian species. Parenting as an adaptive problem in mammals involves specific endocrine signals that were naturally selected to respond to infant cues and environmental inputs. Infants across species produce a number of cues to inform caregivers of their needs. These include visual cues, like facial characteristics, or in some species smiling, auditory cues, such as vocalizations, olfactory cues, and tactile stimulation. A commonly mentioned hormone in parenting is oxytocin, however many other hormones relay key information that results in variations in behavior. These include estrogen, progesterone, prolactin, cortisol, and testosterone. While hormones are not necessary for the expression of maternal behavior, they may influence it.

Synthetic oxytocin, sold under the brand name Pitocin among others, is a medication made from the peptide oxytocin. As a medication, it is used to cause contraction of the uterus to start labor, increase the speed of labor, and to stop bleeding following delivery. For this purpose, it is given by injection either into a muscle or into a vein.
Paternal depression is a psychological disorder derived from parental depression. Paternal depression affects the mood of men; fathers and caregivers in particular. 'Father' may refer to the biological father, foster parent, social parent, step-parent or simply the carer of the child. This mood disorder exhibits symptoms similar to postpartum depression (PPD) including anxiety, insomnia, irritability, consistent breakdown and crying episodes, and low energy. This may negatively impact family relationships and the upbringing of children. Parents diagnosed with parental depression often experience increased stress and anxiety levels during early pregnancy, labor and postpartum. Those with parental depression may have developed it early on but some are diagnosed later on from when the child is a toddler up until a young adult.

Breastfeeding and mental health is the relationship between postpartum breastfeeding and the mother's and child's mental health. Research indicates breastfeeding may have positive effects on the mother's and child's mental health, though there have been conflicting studies that question the correlation and causation of breastfeeding and maternal mental health. Possible benefits include improved mood and stress levels in the mother, lower risk of postpartum depression, enhanced social emotional development in the child, stronger mother-child bonding and more. Given the benefits of breastfeeding, the World Health Organization (WHO), the European Commission for Public Health (ECPH) and the American Academy of Pediatrics (AAP) suggest exclusive breastfeeding for the first six months of life. Despite these suggestions, estimates indicate 70% of mothers breastfeed their child after birth and 13.5% of infants in the United States are exclusively breastfed. Breastfeeding promotion and support for mothers who are experiencing difficulties or early cessation in breastfeeding is considered a health priority.












