Related Research Articles
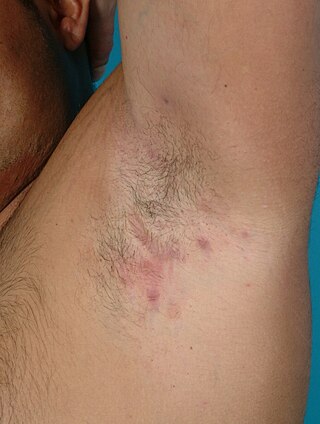
Hidradenitis suppurativa (HS), sometimes known as acne inversa or Verneuil's disease, is a long-term dermatological condition characterized by the occurrence of inflamed and swollen lumps. These are typically painful and break open, releasing fluid or pus. The areas most commonly affected are the underarms, under the breasts, perineum, buttocks, and the groin. Scar tissue remains after healing. HS may significantly limit many everyday activities, for instance, walking, hugging, moving, and sitting down. Sitting disability may occur in patients with lesions in sacral, gluteal, perineal, femoral, groin or genital regions; and prolonged periods of sitting down can also worsen the condition of the skin of these patients.

Palmoplantar keratodermas are a heterogeneous group of disorders characterized by abnormal thickening of the stratum corneum of the palms and soles.

Sweat glands, also known as sudoriferous or sudoriparous glands, from Latin sudor 'sweat', are small tubular structures of the skin that produce sweat. Sweat glands are a type of exocrine gland, which are glands that produce and secrete substances onto an epithelial surface by way of a duct. There are two main types of sweat glands that differ in their structure, function, secretory product, mechanism of excretion, anatomic distribution, and distribution across species:

Erythema nodosum (EN) is an inflammatory condition characterized by inflammation of the fat cells under the skin, resulting in tender red nodules or lumps that are usually seen on both shins. It can be caused by a variety of conditions, and typically resolves spontaneously within 30 days. It is common in young people aged 12–20 years.

Hidradenoma refers to a benign adnexal tumor of the apical sweat gland. These are 1–3 cm translucent blue cystic nodules. It usually presents as a single, small skin-colored lesion, and may be considered closely related to or a variant of poromas. Hidradenomas are often sub-classified based on subtle histologic differences, for example:
Subcutaneous fat necrosis of the newborn is a rare form of lobular panniculitis occurring in newborns that is usually self-remitting and non-recurring. Proposed causes include perinatal stress, local trauma, hypoxia and hypothermia, though the exact cause is unknown. It has been suggested that the brown fat seen in newborns is more sensitive to hypoxic injury than fat seen in adults, and that such hypoxia, usually in the context of a complicated birth, leads to the fat necrosis. Complications can include hypercalcemia, hyperlipidemia, dehydration, hypoglycemia, seizures, vomiting, constipation, and thrombocytopenia, and can present months after the onset of SCFN symptoms.

Pitted keratolysis is a bacterial skin infection of the foot. The infection is characterized by craterlike pits on the sole of the feet and toes, particularly weight bearing areas.
Hidradenitis is any disease in which the histologic abnormality is primarily an inflammatory infiltrate around the eccrine glands. This group includes neutrophilic eccrine hidradenitis and recurrent palmoplantar hidradenitis.

Chemotherapy-induced acral erythema, also known as palmar-plantar erythrodysesthesia or hand-foot syndrome is reddening, swelling, numbness and desquamation on palms of the hands and soles of the feet that can occur after chemotherapy in patients with cancer. Hand-foot syndrome is also rarely seen in sickle-cell disease. These skin changes usually are well demarcated. Acral erythema typically disappears within a few weeks after discontinuation of the offending drug.
Palisaded neutrophilic and granulomatous dermaititis (PNGS) is usually associated with a well-defined connective tissue disease, lupus erythematosus or rheumatoid arthritis most commonly, and often presents with eroded or ulcerated symmetrically distributed umbilicated papules or nodules on the elbows.
Eccrine angiomatous hamartoma (EAH), first described by Lotzbeck in 1859, is a rare benign vascular hamartoma characterized histologically by a proliferation of eccrine and vascular components. EAH exists on a spectrum of cutaneous tumors that include eccrine nevus, mucinous eccrine nevus and EAH. Each diagnostic subtype is characterized by an increase in the number as well as size of mature eccrine glands or ducts, with EAH being distinguished by the added vascular component.
Keratosis pilaris atropicans is a group of idiopathic genodermatoses that consists of three unique clinical entities: atrophoderma vermiculatum, keratosis follicularis spinulosa decalvans, and keratosis pilaris atrophicans faciei.
Neutrophilic eccrine hidradenitis (NEH) usually is a cutaneous complication of chemotherapy, but it can also occur for other reasons. It consists of fever and non specific skin lesions. It is rare, and self-limited.

Palmoplantar hyperhidrosis is excessive sweating localized to the palms of the hands and soles of the feet. It is a form of focal hyperhidrosis in that the excessive sweating is limited to a specific region of the body. As with other types of focal hyperhidrosis the sweating tends to worsen during warm weather.
An eccrine nevus is an extremely rare cutaneous condition that, histologically, is characterized by an increase in size or number of eccrine secretory coils. Hyperhidrosis is the most common symptom. It can present as discoloured nodules, papules, or plaques. Eccrine nevus mostly affects the extremities. Eccrine nevus are diagnosed based of histology. Treatment includes surgical excision or topical medications.

Poromas are rare, benign, cutaneous adnexal tumors. Cutaneous adnexal tumors are a group of skin tumors consisting of tissues that have differentiated towards one or more of the four primary adnexal structures found in normal skin: hair follicles, sebaceous sweat glands, apocrine sweat glands, and eccrine sweat glands. Poromas are eccrine or apocrine sweat gland tumors derived from the cells in the terminal portion of these glands' ducts. This part of the sweat gland duct is termed the acrosyringium and had led to grouping poromas in the acrospiroma class of skin tumors. Here, poromas are regarded as distinct sweat gland tumors that differ from other sweat gland tumors by their characteristic clinical presentations, microscopic histopathology, and the genetic mutations that their neoplastic cells have recently been found to carry.

Eccrine carcinoma is a rare skin condition characterized by a plaque or nodule on the scalp, trunk, or extremities. It originates from the eccrine sweat glands of the skin, accounting for less than 0.01% of diagnosed cutaneous malignancies. Eccrine carcinoma tumors are locally aggressive, with a high rate of recurrence. Lack of reliable immunohistochemical markers and similarity to other common tumors has made identification of eccrine carcinoma difficult.
Congenital erosive and vesicular dermatosis is a cutaneous condition characterized by generalized erosions, vesicles, crusting and ‘scalded skin-like’ erythematous areas affecting up to 75% of the body surface area.
Idiopathic pure sudomotor failure (IPSF) is the most common cause of a rare disorder known as acquired idiopathic generalized anhidrosis (AIGA), a clinical syndrome characterized by generalized decrease or absence of sweating without other autonomic and somatic nervous dysfunctions and without persistent organic cutaneous lesions.
References
- ↑ Rapini, Ronald P.; Bolognia, Jean L.; Jorizzo, Joseph L. (2007). Dermatology: 2-Volume Set. St. Louis: Mosby. ISBN 978-1-4160-2999-1.
- ↑ James, William; Berger, Timothy; Elston, Dirk (2005). Andrews' Diseases of the Skin: Clinical Dermatology. (10th ed.). Saunders. ISBN 0-7216-2921-0.
- 1 2 3 Barradah, Rasheed K. (2021-07-26). "Pseudomonas-Contaminated Pool Triggering an Episode of Idiopathic Palmoplantar Hidradenitis". Case Reports in Dermatology. 13 (2): 411–416. doi:10.1159/000516355. ISSN 1662-6567. PMC 8436668 . PMID 34594199.
- 1 2 Michl, R.; Rusche, T.; Grimm, S.; Limpert, E.; Beck, J.; Dost, A. (2012). "Outbreak of Hot-Foot Syndrome – Caused by Pseudomonas Aeruginosa". Klinische Pädiatrie (in German). 224 (4): 252–255. doi:10.1055/s-0031-1297949. ISSN 0300-8630. PMID 22187332.
- ↑ Yu, Yue; Cheng, Amy S.; Wang, Lawrence; Dunne, W. Michael; Bayliss, Susan J. (2007). "Hot tub folliculitis or hot hand–foot syndrome caused by Pseudomonas aeruginosa". Journal of the American Academy of Dermatology. 57 (4): 596–600. doi:10.1016/j.jaad.2007.04.004. PMID 17658195.
- 1 2 Lee, Grace L.; Chen, Amy Y-Y. (2017). "Neutrophilic dermatoses: Kids are not just little people". Clinics in Dermatology. 35 (6). Elsevier BV: 541–554. doi:10.1016/j.clindermatol.2017.08.005. ISSN 0738-081X. PMID 29191346.
- ↑ Tlougan, B. E.; Podjasek, J. O.; Dickman, P. S.; Hansen, R. C. (2008). "Painful Plantar Papules and Nodules in a Child". Pediatric Annals. 37 (2): 83–4, 87. doi:10.3928/00904481-20080201-01. ISSN 0090-4481. PMID 18335877.
- ↑ Weigl, L.; Eberlein-KÖnig, B.; Ring, J.; Abeck, D. (2000). "Is recurrent plantar hidradenitis in children induced by exposure to a wet and cold milieu?: CORRESPONDENCE". British Journal of Dermatology. 142 (5): 1048–1050. doi:10.1046/j.1365-2133.2000.03497.x. PMID 10809873.
- 1 2 3 Piccini, Paola; Venturini, Elisabetta; Bianchi, Leila; Galli, Luisa; de Martino, Maurizio; Bassi, Andrea (2018). "Bilateral Painful Erythematous Nodules on the Sole". The Journal of Pediatrics. 199: 278. doi:10.1016/j.jpeds.2018.03.017. PMID 29730146.
- ↑ Erro-Vincent, T; Souillet, A.L; Fouilhoux, A; Kanitakis, J; David, L (2001). "Hidradénite eccrine neutrophilique : forme plantaire idiopathique de l'enfant". Archives de Pédiatrie (in French). 8 (3). Elsevier BV: 290–293. doi:10.1016/s0929-693x(00)00195-0. ISSN 0929-693X. PMID 11270254.
- ↑ Bártolo, Elvira; Anes, Isabel; Capitão-Mor, Manuela; Brandão, Francisco M. (1998). "Idiopathic plantar hidradenitis". Journal of the European Academy of Dermatology and Venereology. 10 (3): 257–261. doi:10.1111/j.1468-3083.1998.tb00747.x. ISSN 0926-9959. PMID 9643332.
- 1 2 3 Rubinson, Rebeca; Larralde, Margarita; Santos-Muñoz, Andrea; Parra, Viviana; De Parra, Nelida Pizzi (2004). "Palmoplantar Eccrine Hidradenitis: Seven New Cases". Pediatric Dermatology. 21 (4): 466–468. doi:10.1111/j.0736-8046.2004.21410.x. ISSN 0736-8046. PMID 15283792.