Methylmalonic acidemia, also called methylmalonic aciduria, is an autosomal recessive metabolic disorder that disrupts normal amino acid metabolism. It is a classical type of organic acidemia. The result of this condition is the inability to properly digest specific fats and proteins, which in turn leads to a buildup of a toxic level of methylmalonic acid in the blood.

Zellweger syndrome is a rare congenital disorder characterized by the reduction or absence of functional peroxisomes in the cells of an individual. It is one of a family of disorders called Zellweger spectrum disorders which are leukodystrophies. Zellweger syndrome is named after Hans Zellweger (1909–1990), a Swiss-American pediatrician, a professor of pediatrics and genetics at the University of Iowa who researched this disorder.

Glycerophospholipids of biochemical relevance are divided into three subclasses based on the substitution present at the sn-1 position of the glycerol backbone: acyl, alkyl and alkenyl. Of these, the alkyl and alkenyl moiety in each case form an ether bond, which makes for two types of ether phospholipids, plasmanyl, and plasmenyl. Plasmalogens are plasmenyls with an ester linked lipid at the sn-2 position of the glycerol backbone, chemically designated 1-0(1Z-alkenyl)-2-acyl-glycerophospholipids. The lipid attached to the vinyl ether at sn-1 can be C16:0, C18:0, or C18:1, and the lipid attached to the acyl group at sn-2 can be C22:6 ω-3 or C20:4 ω-6, . Plasmalogens are classified according to their head group, mainly as PC plasmalogens (plasmenylcholines) and PE plasmalogens (plasmenylethalomines) Plasmalogens should not be confused with plasmanyls.
Refsum disease is an autosomal recessive neurological disease that results in the over-accumulation of phytanic acid in cells and tissues. It is one of several disorders named after Norwegian neurologist Sigvald Bernhard Refsum (1907–1991). Refsum disease typically is adolescent onset and is diagnosed by above average levels of phytanic acid. Humans obtain the necessary phytanic acid primarily through diet. It is still unclear what function phytanic acid plays physiologically in humans, but has been found to regulate fatty acid metabolism in the liver of mice.

Alpha-thalassemia mental retardation syndrome (ATRX), also called alpha-thalassemia X-linked intellectual disability syndrome, nondeletion type or ATR-X syndrome, is an X-linked recessive condition associated with a mutation in the ATRX gene. Males with this condition tend to be moderately intellectually disabled and have physical characteristics including coarse facial features, microcephaly, hypertelorism, a depressed nasal bridge, a tented upper lip and an everted lower lip. Mild or moderate anemia, associated with alpha-thalassemia, is part of the condition. Females with this mutated gene have no specific signs or features, but if they do, they may demonstrate skewed X chromosome inactivation.
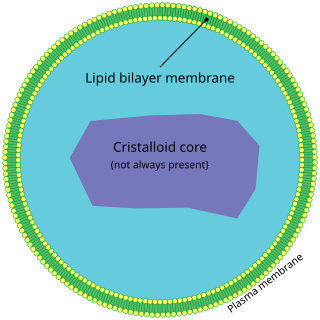
Peroxisomal disorders represent a class of medical conditions caused by defects in peroxisome functions. This may be due to defects in single enzymes important for peroxisome function or in peroxins, proteins encoded by PEX genes that are critical for normal peroxisome assembly and biogenesis.

Branchio-oto-renal syndrome (BOR) is an autosomal dominant genetic disorder involving the kidneys, ears, and neck. It is also known as Melnick-Fraser syndrome.
Infantile Refsum disease (IRD) is a rare autosomal recessive congenital peroxisomal biogenesis disorder within the Zellweger spectrum. These are disorders of the peroxisomes that are clinically similar to Zellweger syndrome and associated with mutations in the PEX family of genes. IRD is associated with deficient phytanic acid catabolism, as is adult Refsum disease, but they are different disorders that should not be confused.

Peroxisome biogenesis factor 1, also known as PEX1, is a protein which in humans is encoded by the PEX1 gene.

Peroxisomal biogenesis factor 2 is a protein that in humans is encoded by the PEX2 gene.

Peroxisomal membrane protein PEX13 is a protein that in humans is encoded by the PEX13 gene. It located on chromosome 2 next to KIAA1841

Peroxisome assembly factor 2 is a protein that in humans is encoded by the PEX6 gene. PEX6 is an AAA ATPase that localizes to the peroxisome. PEX6 forms a hexamer with PEX1 and is recruited to the membrane by PEX26.

Peroxisome biogenesis factor 10 is a protein that in humans is encoded by the PEX10 gene. Alternative splicing results in two transcript variants encoding different isoforms.

Peroxisomal membrane protein PEX16 is a protein that in humans is encoded by the PEX16 gene.

Orofaciodigital syndrome 1 (OFD1), also called Papillon-Léage and Psaume syndrome, is an X-linked congenital disorder characterized by malformations of the face, oral cavity, and digits with polycystic kidney disease and variable involvement of the central nervous system.
Oculocutaneous albinism type I or type 1A is an autosomal recessive skin disease. This subtype of oculocutaneous albinism is caused when the gene for tyrosinase does not function properly.
X-linked recessive chondrodysplasia punctata is a type of chondrodysplasia punctata that can involve the skin, hair, and cause short stature with skeletal abnormalities, cataracts, and deafness.

Anoctamin 5 (ANO5) is a protein that in humans is encoded by the ANO5 gene.
Cousin syndrome is a genetic condition characterized by short stature at birth, a short neck with low-positioned external ears, as well as congenital malformations of the skeletal system affecting the shoulders, the pelvis, the neck, and the limbs. The condition determines physical disability, particularly affecting deambulation, and hearing loss while intelligence is not affected.