
Radiation therapy or radiotherapy is a treatment using ionizing radiation, generally provided as part of cancer therapy to either kill or control the growth of malignant cells. It is normally delivered by a linear particle accelerator. Radiation therapy may be curative in a number of types of cancer if they are localized to one area of the body, and have not spread to other parts. It may also be used as part of adjuvant therapy, to prevent tumor recurrence after surgery to remove a primary malignant tumor. Radiation therapy is synergistic with chemotherapy, and has been used before, during, and after chemotherapy in susceptible cancers. The subspecialty of oncology concerned with radiotherapy is called radiation oncology. A physician who practices in this subspecialty is a radiation oncologist.

In medicine, proton therapy, or proton radiotherapy, is a type of particle therapy that uses a beam of protons to irradiate diseased tissue, most often to treat cancer. The chief advantage of proton therapy over other types of external beam radiotherapy is that the dose of protons is deposited over a narrow range of depth; hence in minimal entry, exit, or scattered radiation dose to healthy nearby tissues.

Radiosurgery is surgery using radiation, that is, the destruction of precisely selected areas of tissue using ionizing radiation rather than excision with a blade. Like other forms of radiation therapy, it is usually used to treat cancer. Radiosurgery was originally defined by the Swedish neurosurgeon Lars Leksell as "a single high dose fraction of radiation, stereotactically directed to an intracranial region of interest".

Stereotactic surgery is a minimally invasive form of surgical intervention that makes use of a three-dimensional coordinate system to locate small targets inside the body and to perform on them some action such as ablation, biopsy, lesion, injection, stimulation, implantation, radiosurgery (SRS), etc.

Varian Medical Systems is an American radiation oncology treatments and software maker based in Palo Alto, California. Their medical devices include linear accelerators (LINACs) and software for treating cancer and other medical conditions with radiotherapy, radiosurgery, proton therapy, and brachytherapy. The company supplies software for managing cancer clinics, radiotherapy centers, and medical oncology practices. Varian Medical Systems employs more than 7,100 people at manufacturing sites in North America, Europe, and China and approximately 70 sites globally.
Elekta is a global Swedish company that develops and produces radiation therapy and radiosurgery-related equipment and clinical management for the treatment of cancer and brain disorders. Elekta has a global presence in more than 120 countries, with over 40 offices around the world and about 4,700 employees.

In radiotherapy, radiation treatment planning (RTP) is the process in which a team consisting of radiation oncologists, radiation therapist, medical physicists and medical dosimetrists plan the appropriate external beam radiotherapy or internal brachytherapy treatment technique for a patient with cancer.

Tomotherapy is a type of radiation therapy treatment machine. In tomotherapy a thin radiation beam is modulated as it rotates around the patient, while they are moved through the bore of the machine. The name comes from the use of a strip-shaped beam, so that only one “slice” of the target is exposed at any one time by the radiation. The external appearance of the system and movement of the radiation source and patient can be considered analogous to a CT scanner, which uses lower doses of radiation for imaging. Like a conventional machine used for X-ray external beam radiotherapy, it [the tomotherapy machine] generates the radiation beam, but the external appearance of the machine, patient positioning, and treatment delivery differ. Conventional linacs do not work on a slice-by-slice basis but typically have a large area beam which can also be resized and modulated.
Particle therapy is a form of external beam radiotherapy using beams of energetic neutrons, protons, or other heavier positive ions for cancer treatment. The most common type of particle therapy as of August 2021 is proton therapy.
The CyberKnife system is a radiation therapy device manufactured by Accuray. The system is used to deliver radiosurgery for the treatment of benign tumors, malignant tumors and other medical conditions.
Maurice Lenz was a pioneer in the field of radiation therapy. Born in Kovno, Russian Empire, Lenz studied at New York University and Bellevue Medical College, and received his medical degree from Columbia University College of Physicians and Surgeons in 1913. He was a professor of radiation oncology at the Columbia University College of Physicians and Surgeons, a past president of the American Radium Society and held many other clinical and administrative roles throughout his long career in medicine.
Docrates Cancer Center is the first and currently the only private hospital in the Nordic countries that comprehensively specialises in cancer treatment. It operates in Helsinki, Finland. It characterises its operations as those complementing the public sector. Docrates Oy was established in 2006 and the hospital started its operations at the premises of Eira Hospital in autumn 2007. It moved to its own premises in Jätkäsaari, Helsinki, in 2009, where it has hospital rights. There is a ward and Health and Recovery Center located at Docrates Cancer Center. Among other things, diagnostics, pharmacotherapy, radiation therapy and isotopic treatments are carried out at the hospital. Cancer surgeries are performed in partner hospitals. Docrates also participates in clinical trials and the testing and development of new treatments.
Joaquín Gómez Mira is a scientist and physician specialized in radiation oncology. Born and raised in Spain, he completed his studies and developed his career in the United States, where he moved in 1967. He is a member of the American Society of Clinical Oncology, and a Fellow and appointed councilor of the American College of Radiology. His work, achievements and lectures in the field of radiation oncology are held in high regard.

Northern Westchester Hospital (NWH) is a not-for-profit, 245-bed, all-private-room facility in Mount Kisco, New York. Founded in 1916, it serves residents of Northern Westchester, Putnam County and southern Dutchess County, as well as parts of Fairfield County, Connecticut. It is owned by Northwell Health.
Eleanor D. Montague was an American radiologist and educator who established breast-conserving therapy in the United States and improved radiation therapy techniques. She became a member of the Texas Women's Hall of Fame in 1993.
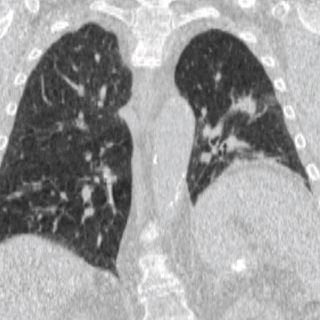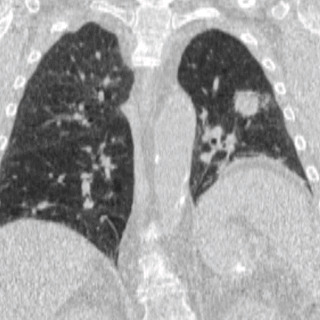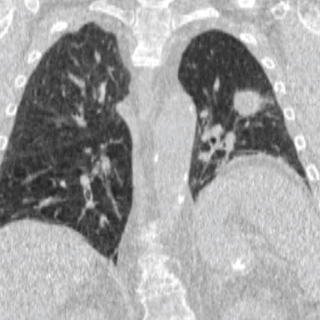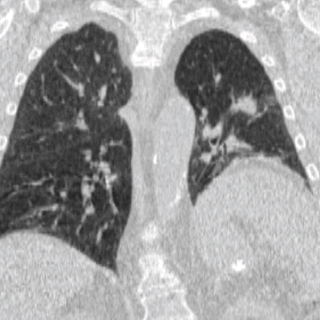
Four-dimensional computed tomography (4DCT) is a type of CT scanning which records multiple images over time. It allows playback of the scan as a video, so that physiological processes can be observed and internal movement can be tracked. The name is derived from the addition of time to traditional 3D computed tomography. Alternatively, the phase of a particular process, such as respiration, may be considered the fourth dimension.

Radiumhemmet is a non-surgical cancer treatment and radiotherapy research institution in Solna, Sweden. Since 1938, it has been a division of what is now the Karolinska University Hospital. It was founded in 1910 in central Stockholm as the first oncological clinic in Sweden, succeeding a radium research and treatment institution at the Serafimerlasarett founded in 1906, and played a major role in the development of radiotherapy, especially in gynaecological cancers.

Jay Steven Loeffler was an American physician at Massachusetts General Hospital, where he served as chair of the Department of Radiation Oncology since 2000. He was the Herman and Joan Suit Professor of Radiation Oncology and professor of neurosurgery at Harvard Medical School.

Dr. Daniel Przybysz is a Brazilian Radiation-Oncologist. His practice is mainly focused on lung cancer treatment and high technology approaches toward better patient care

Shakardokht (Shakar) Jafari is a Medical Physicist and an award-winning innovator based at the Surrey Technology Centre. She developed an efficient and low-cost method of measuring a medical dose of radiation.












