| Arterial insufficiency ulcer | |
|---|---|
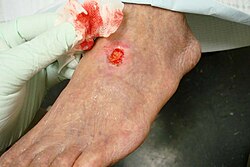 | |
| A 71-year-old diabetic male smoker with severe peripheral arterial disease presented with a dorsal foot ulceration (2.5 cm X 2.4cm) that had been chronically open for nearly 2 years. |
Arterial insufficiency ulcers (also known as ischemic ulcers, or ischemic wounds) are ulcers mostly located on the lateral surface of the ankle or the distal digits. [1] They are commonly caused by peripheral artery disease (PAD).
