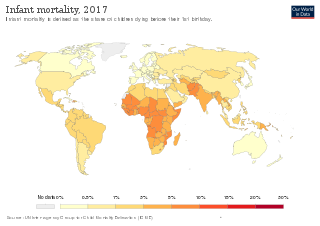
Infant mortality is the death of an infant before the infant's first birthday. The occurrence of infant mortality in a population can be described by the infant mortality rate (IMR), which is the number of deaths of infants under one year of age per 1,000 live births. Similarly, the child mortality rate, also known as the under-five mortality rate, compares the death rate of children up to the age of five.

An infant or baby is the very young offspring of human beings. Infant is a formal or specialised synonym for the common term baby. The terms may also be used to refer to juveniles of other organisms. A newborn is, in colloquial use, an infant who is only hours, days, or up to one month old. In medical contexts, a newborn or neonate is an infant in the first 28 days after birth; the term applies to premature, full term, and postmature infants.
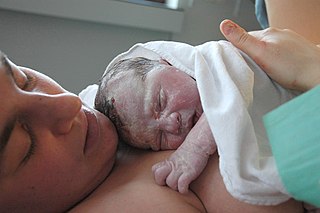
Childbirth, also known as labour, parturition and delivery, is the completion of pregnancy where one or more babies exits the internal environment of the mother via vaginal delivery or caesarean section. In 2019, there were about 140.11 million human births globally. In the developed countries, most deliveries occur in hospitals, while in the developing countries most are home births.

Maternal death or maternal mortality is defined in slightly different ways by several different health organizations. The World Health Organization (WHO) defines maternal death as the death of a pregnant mother due to complications related to pregnancy, underlying conditions worsened by the pregnancy or management of these conditions. This can occur either while they are pregnant or within six weeks of resolution of the pregnancy. The CDC definition of pregnancy-related deaths extends the period of consideration to include one year from the resolution of the pregnancy. Pregnancy associated death, as defined by the American College of Obstetricians and Gynecologists (ACOG), are all deaths occurring within one year of a pregnancy resolution. Identification of pregnancy associated deaths is important for deciding whether or not the pregnancy was a direct or indirect contributing cause of the death.

The postpartum period begins after childbirth and is typically considered to last for six weeks. However, there are three distinct but continuous phases of the postnatal period; the acute phase, lasting for six to twelve hours after birth; the subacute phase, lasting six weeks; and the delayed phase, lasting up to six months. During the delayed phase, some changes to the genitourinary system take much longer to resolve and may result in conditions such as urinary incontinence. The World Health Organization (WHO) describes the postnatal period as the most critical and yet the most neglected phase in the lives of mothers and babies; most maternal and newborn deaths occur during this period.
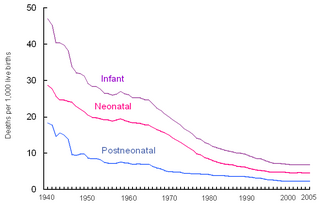
Perinatal mortality (PNM) is the death of a fetus or neonate and is the basis to calculate the perinatal mortality rate. Perinatal means "relating to the period starting a few weeks before birth and including the birth and a few weeks after birth."
Maternal health is the health of women during pregnancy, childbirth, and the postpartum period. In most cases, maternal health encompasses the health care dimensions of family planning, preconception, prenatal, and postnatal care in order to ensure a positive and fulfilling experience. In other cases, maternal health can reduce maternal morbidity and mortality. Maternal health revolves around the health and wellness of pregnant women, particularly when they are pregnant, at the time they give birth, and during child-raising. WHO has indicated that even though motherhood has been considered as a fulfilling natural experience that is emotional to the mother, a high percentage of women develop health problems and sometimes even die. Because of this, there is a need to invest in the health of women. The investment can be achieved in different ways, among the main ones being subsidizing the healthcare cost, education on maternal health, encouraging effective family planning, and ensuring progressive check up on the health of women with children. Maternal morbidity and mortality particularly affects women of color and women living in low and lower-middle income countries.

The Promotion of the Welfare and Hygiene of Maternity and Infancy Act, more commonly known as the Sheppard–Towner Act, was a 1921 U.S. Act of Congress that provided federal funding for maternity and childcare. It was sponsored by Senator Morris Sheppard (D) of Texas and Representative Horace Mann Towner (R) of Iowa and signed by President Warren G. Harding on November 23, 1921. It went out of effect in 1929.
Early postnatal hospital discharge generally refers to the postpartum hospital discharge of the mother and newborn within 48 hours. The duration of what is considered "early discharge" varies between countries from 12 to 72 hours due to the differences in average duration of hospital stay. The World Health Organisation (WHO) recommends healthy mothers and newborns following an uncomplicated vaginal delivery at a health facility to stay and receive care at the facility for at least 24 hours after delivery. This recommendation is based on findings which suggest that the first 24 hours after giving birth poses the greatest risks for both the mother and newborn.
The Baby Friendly Hospital Initiative (BFHI), also known as Baby Friendly Initiative (BFI), is a worldwide programme of the World Health Organization (WHO) and the United Nations Children's Fund (UNICEF), launched in 1992 in India following the adoption of the Innocenti Declaration on breastfeeding promotion in 1990. The initiative is a global effort for improving the role of maternity services to enable mothers to breastfeed babies for the best start in life. It aims at improving the care of pregnant women, mothers and newborns at health facilities that provide maternity services for protecting, promoting and supporting breastfeeding, in accordance with the International Code of Marketing of Breast-milk Substitutes.

The maternity package, known internationally as the Finnish "baby box," is a kit granted by the Finnish social security institution Kela, to all expectant or adoptive parents who live in Finland or are covered by the Finnish social security system. The package contains children's clothes and other necessary items, such as nappies, bedding, cloth, gauze towels and child-care products. It was first issued in 1938 to parents with a low income, and contained a blanket, crib sheets, diapers, and fabric which parents could use to make clothing for the baby.

Both maternal and child health are interdependent and substantially contributing to high burden of mortality worldwide. Every year, 289 000 women die due to complications in pregnancy and childbirth, and 6.6 million children below 5 years of age die of complications in the newborn period and of common childhood diseases. Sub-Saharan Africa (SSA), which includes Tanzania, contribute higher proportion of maternal and child mortality. Due to considerable proportion of mortality being attributed by maternal and child health, the United Nations together with other international agencies incorporated the two into Millennium Development Goals (MDGs) 4 and 5. In this regard, Tanzania through the Ministry of Health and Social Welfare (MoHSW) adopted different strategies and efforts to promote safe motherhood and improve child survival. Similarly, in an effort to improve maternal and child health, Tanzania's government has declared maternal and child health services to be exempt from user fees in government facilities.
Nils Bergman, is a Swedish specialist in perinatal neuroscience and a promoter of skin-to-skin contact between a mother and newborn.
This article provides a background on Nepal as a whole, with a focus on the nation's childbearing and birthing practices. While modern Western medicine has disseminated across the country to varying degrees, different regions in Nepal continue to practice obstetric and newborn care according to traditional beliefs, attitudes, and customs.
Childbirth practices in India are shaped by the prevalence of religious customs and joint-family living, India's young average population, the lower national average age at marriage, and disparities in social status and literacy between men and women. Inadequate maternal health care services in India are a result of poor organization, the huge rural-urban divide, and large interstate disparities coupled with stringent social-economic and cultural constraints.
The maternal mortality rate is 224 deaths per 100,000 births, which is the 23rd highest in the world. The mean age of mothers at birth is 19.3 years old, and the fertility rate is 5.72 children born per woman, which is the 7th highest in the world. The contraceptive rate is only 40.8%, and the birth rate is the 4th highest in the world at 42.13 births/1,000 population. Infectious disease is a key contributor to the poor health of the nation, and the risk is very high for diseases such as protozoal and bacterial diarrhea, hepatitis A, typhoid fever, malaria, dengue fever, schistosomiasis, and rabies. The adult prevalence rate of HIV/AIDS is 12.37%, which is the 7th highest in the world.
Midwives in South Africa are nurses who focus on the care of pregnant women and the delivery of babies. Midwives have the ability to work independently in cases of healthy pregnancies and problem-free deliveries; however, they can refer patients to gynaecologists or obstetricians when complications are diagnosed. The majority of pregnant women in South Africa use the public healthcare system, and most of this care is provided by midwives.

Salome Maswime is a South African clinician and global health expert. She is an Obstetrician and Gynaecologist and the Head of Global Surgery at the University of Cape Town. She advocates for women's health rights, equity in surgical and maternal care, and providing adequate health services to remote and underserved populations. She advises and consults for many institutions, including the World Health Organization. In 2017, she was honored with the Trailblazer and Young Achiever Award. She is a member of the Academy of Science of South Africa.

Joy Elizabeth Lawn is a British paediatrician and professor of maternal, reproductive and child health. She is Director of the London School of Hygiene & Tropical Medicine Maternal, Adolescent, Reproductive & Child Health (MARCH) Centre. She developed the epidemiological evidence for the worldwide policy and programming that looks to reduce neonatal deaths and stillbirths and works on large-scale implementation research.
Black maternal mortality in the United States refers to the death of women, specifically those who identify as Black or African American, during or after child delivery. In general, maternal death can be due to a myriad of factors, such as how the nature of the pregnancy or the delivery itself, but is not associated with unintentional or secondary causes. In the United States, around 700 women die from pregnancy-related illnesses or complications per year. This number does not include the approximately 50,000 women who experience life-threatening complications during childbirth, resulting in lifelong disabilities and complications. However, there are stark differences in maternal mortality rates for Black American women versus Indigenous American, Alaska Native, and White American women.











