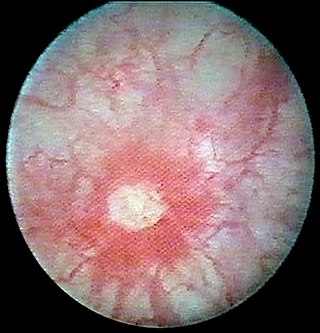
Interstitial cystitis (IC), a type of bladder pain syndrome (BPS), is chronic pain in the bladder and pelvic floor of unknown cause. It is the urologic chronic pelvic pain syndrome of women. Symptoms include feeling the need to urinate right away, needing to urinate often, and pain with sex. IC/BPS is associated with depression and lower quality of life. Many of those affected also have irritable bowel syndrome and fibromyalgia.

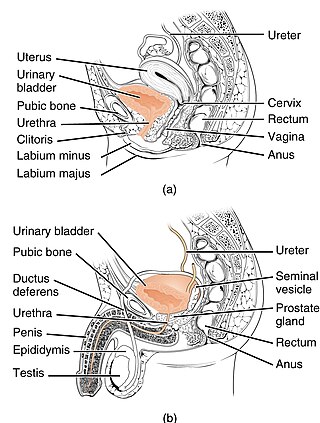
The urinary system, also known as the urinary tract or renal system, consists of the kidneys, ureters, bladder, and the urethra. The purpose of the urinary system is to eliminate waste from the body, regulate blood volume and blood pressure, control levels of electrolytes and metabolites, and regulate blood pH. The urinary tract is the body's drainage system for the eventual removal of urine. The kidneys have an extensive blood supply via the renal arteries which leave the kidneys via the renal vein. Each kidney consists of functional units called nephrons. Following filtration of blood and further processing, wastes exit the kidney via the ureters, tubes made of smooth muscle fibres that propel urine towards the urinary bladder, where it is stored and subsequently expelled from the body by urination. The female and male urinary system are very similar, differing only in the length of the urethra.
Urinary incontinence (UI), also known as involuntary urination, is any uncontrolled leakage of urine. It is a common and distressing problem, which may have a large impact on quality of life. It has been identified as an important issue in geriatric health care. The term enuresis is often used to refer to urinary incontinence primarily in children, such as nocturnal enuresis. UI is an example of a stigmatized medical condition, which creates barriers to successful management and makes the problem worse. People may be too embarrassed to seek medical help, and attempt to self-manage the symptom in secrecy from others.

Enuresis is a repeated inability to control urination. Use of the term is usually limited to describing people old enough to be expected to exercise such control. Involuntary urination is also known as urinary incontinence. The term "enuresis" comes from the Ancient Greek: ἐνούρησις, romanized: enoúrēsis.

Pelvic floor dysfunction is a term used for a variety of disorders that occur when pelvic floor muscles and ligaments are impaired. The condition affects up to 50 percent of women who have given birth. Although this condition predominantly affects women, up to 16 percent of men are affected as well. Symptoms can include pelvic pain, pressure, pain during sex, urinary incontinence (UI), overactive bladder, bowel incontinence, incomplete emptying of feces, constipation, myofascial pelvic pain and pelvic organ prolapse. When pelvic organ prolapse occurs, there may be visible organ protrusion or a lump felt in the vagina or anus. Research carried out in the UK has shown that symptoms can restrict everyday life for women. However, many people found it difficult to talk about it and to seek care, as they experienced embarassment and stigma.

Tolterodine, sold under the brand name Detrol among others, is a medication used to treat frequent urination, urinary incontinence, or urinary urgency. Effects are seen within an hour. It is taken by mouth.
Percutaneous tibial nerve stimulation (PTNS), also referred to as posterior tibial nerve stimulation, is the least invasive form of neuromodulation used to treat overactive bladder (OAB) and the associated symptoms of urinary urgency, urinary frequency and urge incontinence. These urinary symptoms may also occur with interstitial cystitis and following a radical prostatectomy. Outside the United States, PTNS is also used to treat fecal incontinence.

Oxybutynin, sold as under the brand name Ditropan among others, is an anticholinergic drug primarily used to treat overactive bladder. It is widely considered a first-line therapy for overactive bladder due to its well-studied side effect profile, broad applicability, and continued efficacy over long periods of time. It works similar to tolterodine, darifenacin, and solifenacin, although it is usually preferred over these medications. It is sometimes used off-label for treatment of hyperhidrosis, or excessive sweating. It has also been used off-label to treat bed wetting in children, but this use has declined, as it is most likely ineffective in this role. It is taken by mouth or applied to the skin.

Stress incontinence, also known as stress urinary incontinence (SUI) or effort incontinence is a form of urinary incontinence. It is due to inadequate closure of the bladder outlet by the urethral sphincter.

Darifenacin is a medication used to treat urinary incontinence due to an overactive bladder. It was discovered by scientists at the Pfizer research site in Sandwich, UK under the identifier UK-88,525 and used to be marketed by Novartis. In 2010, the US rights were sold to Warner Chilcott for US$400 million.

Solifenacin, sold as the brand name Vesicare among others, is a medicine used to treat overactive bladder and neurogenic detrusor overactivity (NDO). It may help with incontinence, urinary frequency, and urinary urgency.
Neurogenic bladder dysfunction, often called by the shortened term neurogenic bladder, refers to urinary bladder problems due to disease or injury of the central nervous system or peripheral nerves involved in the control of urination. There are multiple types of neurogenic bladder depending on the underlying cause and the symptoms. Symptoms include overactive bladder, urinary urgency, frequency, incontinence or difficulty passing urine. A range of diseases or conditions can cause neurogenic bladder including spinal cord injury, multiple sclerosis, stroke, brain injury, spina bifida, peripheral nerve damage, Parkinson's disease, or other neurodegenerative diseases. Neurogenic bladder can be diagnosed through a history and physical as well as imaging and more specialized testing. In addition to symptomatic treatment, treatment depends on the nature of the underlying disease and can be managed with behavioral changes, medications, surgeries, or other procedures. The symptoms of neurogenic bladder, especially incontinence, can severely degrade a person's quality of life.

Overactive bladder (OAB) is a common condition where there is a frequent feeling of needing to urinate to a degree that it negatively affects a person's life. The frequent need to urinate may occur during the day, at night, or both. Loss of bladder control may occur with this condition. Overactive bladder affects approximately 11% of the population and more than 40% of people with overactive bladder have incontinence. Conversely, about 40% to 70% of urinary incontinence is due to overactive bladder. Overactive bladder is not life-threatening, but most people with the condition have problems for years.

A sacral nerve stimulator is a small device usually implanted in the buttocks of people who have problems with bladder and/or bowel control. This device is implanted in the buttock and connected to the sacral nerve S3 by a wire. The device uses sacral nerve stimulation to stop urges to defecate and urinate by sending signals to the sacral nerve. The patient is able to control their bladder and/or bowel via an external device similar to a remote control.
Sacral nerve stimulation, also termed sacral neuromodulation, is a type of medical electrical stimulation therapy.
Urogynecology or urogynaecology is a surgical sub-specialty of urology and gynecology.

Overflow incontinence is a concept of urinary incontinence, characterized by the involuntary release of urine from an overfull urinary bladder, often in the absence of any urge to urinate. This condition occurs in people who have a blockage of the bladder outlet, or when the muscle that expels urine from the bladder is too weak to empty the bladder normally. Overflow incontinence may also be a side effect of certain medications.
Mirabegron, sold under the brand name Myrbetriq among others, is a medication used to treat overactive bladder. Its benefits are similar to antimuscarinic medication such as solifenacin or tolterodine. It is taken by mouth.

Vibegron, sold under the brand name Gemtesa, is a medication for the treatment of overactive bladder. Vibegron is a selective beta-3 adrenergic receptor agonist.
Prof Clare Fowler CBE is a British physician and academic who created the subspecialty of uro-neurology, a medical field that combines urology and neurology. This work was done at the Institute of Neurology, University College London, where she is an emeritus professor.













