
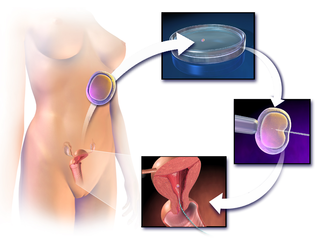
In vitro fertilisation (IVF) is a process of fertilisation where an egg is combined with sperm in vitro. The process involves monitoring and stimulating a patient's ovulatory process, removing an ovum or ova from their ovaries and letting sperm fertilise them in a culture medium in a laboratory. After the fertilised egg (zygote) undergoes embryo culture for 2–6 days, it is transferred by catheter into the uterus, with the intention of establishing a successful pregnancy.

The Human Fertilisation and Embryology Authority (HFEA) is an executive non-departmental public body of the Department of Health and Social Care in the United Kingdom. It is a statutory body that regulates and inspects all clinics in the United Kingdom providing in vitro fertilisation (IVF), artificial insemination and the storage of human eggs, sperm or embryos. It also regulates human embryo research.
Assisted reproductive technology (ART) includes medical procedures used primarily to address infertility. This subject involves procedures such as in vitro fertilization (IVF), intracytoplasmic sperm injection (ICSI), cryopreservation of gametes or embryos, and/or the use of fertility medication. When used to address infertility, ART may also be referred to as fertility treatment. ART mainly belongs to the field of reproductive endocrinology and infertility. Some forms of ART may be used with regard to fertile couples for genetic purpose. ART may also be used in surrogacy arrangements, although not all surrogacy arrangements involve ART. The existence of sterility will not always require ART to be the first option to consider, as there are occasions when its cause is a mild disorder that can be solved with more conventional treatments or with behaviors based on promoting health and reproductive habits.
Embryo donation is one disposition option for users of in vitro fertilisation with remaining fresh or frozen embryos. It is defined as the giving—generally without compensation—of embryos remaining after in vitro fertilization procedures to recipients for procreative implantation or research. Most IVF users with supernumerary embryos make embryo donation decisions after completing their families or discontinuing use of in vitro fertilization. Recipients of embryos donated for procreative implantation typically plan to transfer fresh or frozen embryos into a prepared uterus in order to facilitate pregnancy and childbirth. Recipients of embryos donated for research typically use them for clinical training, quality improvement research, or human embryonic stem cell research.
Third-party reproduction or donor-assisted reproduction is any human reproduction in which DNA or gestation is provided by a third party or donor other than the one or two parents who will raise the resulting child. This goes beyond the traditional father–mother model, and the third party's involvement is limited to the reproductive process and does not extend into the raising of the child. Third-party reproduction is used by couples unable to reproduce by traditional means, by same-sex couples, and by men and women without a partner. Where donor gametes are provided by a donor, the donor will be a biological parent of the resulting child, but in third party reproduction, he or she will not be the caring parent.

A sperm bank, semen bank, or cryobank is a facility or enterprise which purchases, stores and sells human semen. The semen is produced and sold by men who are known as sperm donors. The sperm is purchased by or for other persons for the purpose of achieving a pregnancy or pregnancies other than by a sexual partner. Sperm sold by a sperm donor is known as donor sperm.
The British Pregnancy Advisory Service (BPAS) is a British charity whose stated purpose is to avoid unwanted pregnancy by advocating and providing high quality, affordable services to prevent or end unwanted pregnancies with contraception or by abortion."
Jane Denton,, is a United Kingdom nurse and midwife notable for her contributions to fertility nursing and genetics. She was made a Fellow of the Royal College of Nursing in 2006.
The hamster zona-free ovum test, or hamster egg-penetration test, or sometimes just hamster test, is an in-vitro test used to study physiological profile of spermatozoa. The primary application of the test is to diagnose male infertility caused by sperm unable to penetrate the ova. The test has limited value, due to expense and a high false negative rate.

Oocyte cryopreservation is a procedure to preserve a woman's eggs (oocytes). This technique has been used to enable women to postpone pregnancy to a later date – whether for medical or social reasons. Several studies have shown that most infertility problems are due to germ cell deterioration related to aging. The procedure intends that the woman may choose to have the eggs thawed, fertilized, and transferred to the uterus as embryos to facilitate a pregnancy in the future. The procedure's success rate varies depending on the age of the woman, with the odds being higher in younger, adult women.
Donor registration facilitates donor conceived people, sperm donors and egg donors to establish contact with genetic kindred. Registries are mostly used by donor conceived people to find out their genetic heritage and to find half-siblings from the same egg or sperm donor. In some jurisdictions donor registration is compulsory, while in others it is voluntary; but most jurisdictions do not have any registration system.
Sperm donation laws vary by country. Most countries have laws to cover sperm donations which, for example, place limits on how many children a sperm donor may give rise to, or which limit or prohibit the use of donor semen after the donor has died, or payment to sperm donors. Other laws may restrict use of donor sperm for in vitro fertilisation (IVF) treatment, which may itself be banned or restricted in some way, such as to married heterosexual couples, banning such treatment to single women or lesbian couples. Donated sperm may be used for insemination or as part of IVF treatment. Notwithstanding such laws, informal and private sperm donations take place, which are largely unregulated.
Fertility tourism is the practice of traveling to another country or jurisdiction for fertility treatment, and may be regarded as a form of medical tourism. A person who can become pregnant is considered to have fertility issues if they are unable to have a clinical pregnancy after 12 months of unprotected intercourse. Infertility, or the inability to get pregnant, affects about 8-12% of couples looking to conceive or 186 million people globally. In some places, rates of infertility surpass the global average and can go up to 30% depending on the country. Areas with lack of resources, such as assisted reproductive technologies (ARTs), tend to correlate with the highest rates of infertility.
Sperm donation is the provision by a man of his sperm with the intention that it be used in the artificial insemination or other "fertility treatment" of one or more women who are not his sexual partners in order that they may become pregnant by him. Where pregnancies go to full term, the sperm donor will be the biological father of every baby born from his donations. The man is known as a sperm donor and the sperm he provides is known as "donor sperm" because the intention is that the man will give up all legal rights to any child produced from his sperm, and will not be the legal father. Sperm donation may also be known as "semen donation".
Religious response to assisted reproductive technology deals with the new challenges for traditional social and religious communities raised by modern assisted reproductive technology. Because many religious communities have strong opinions and religious legislation regarding marriage, sex and reproduction, modern fertility technology has forced religions to respond.

The Human Fertilisation and Embryology Act 2008 is an Act of the Parliament of the United Kingdom. The Act constitutes a major review and update of the Human Fertilisation and Embryology Act 1990.
Cryopreservation of embryos is the process of preserving an embryo at sub-zero temperatures, generally at an embryogenesis stage corresponding to pre-implantation, that is, from fertilisation to the blastocyst stage.
Partner-assisted reproduction, reception of oocytes from partner (ROPA), reciprocal IVF,shared motherhood, partner IVF or co-IVF is a method of family building that is used by couples who both possess female reproductive organs. The method uses in vitro fertilization (IVF), a method that means eggs are removed from the ovaries, fertilized in a laboratory, and then one or more of the resulting embryos are placed in the uterus to hopefully create a pregnancy. Reciprocal IVF differs from standard IVF in that two partners are involved: the eggs are taken from one partner, and the other partner carries the pregnancy. In this way, the process is mechanically identical to IVF with egg donation. Reciprocal IVF offers the highest chance for pregnancy and a lower chance of a multiple births.

The legal aspects of surrogacy in any particular jurisdiction tend to hinge on a few central questions:

LGBT reproduction refers to lesbian, gay, bisexual, and transgender (LGBT) people having biological children by means of assisted reproductive technology. It is distinct from LGBT parenting, which is a broader cultural phenomenon including LGBT adoption. In recent decades, developmental biologists have been researching and developing techniques to facilitate same-sex reproduction.








