Related Research Articles

Ophthalmology is a clinical and surgical specialty within medicine that deals with the diagnosis and treatment of eye disorders. A former term is oculism.

Retinoblastoma (Rb) is a rare form of cancer that rapidly develops from the immature cells of a retina, the light-detecting tissue of the eye. It is the most common primary malignant intraocular cancer in children, and it is almost exclusively found in young children.
Retinopathy of prematurity (ROP), also called retrolental fibroplasia (RLF) and Terry syndrome, is a disease of the eye affecting prematurely born babies generally having received neonatal intensive care, in which oxygen therapy is used because of the premature development of their lungs. It is thought to be caused by disorganized growth of retinal blood vessels and may result in scarring and retinal detachment. ROP can be mild and may resolve spontaneously, but it may lead to blindness in serious cases. Thus, all preterm babies are at risk for ROP, and very low birth-weight is an additional risk factor. Both oxygen toxicity and relative hypoxia can contribute to the development of ROP.
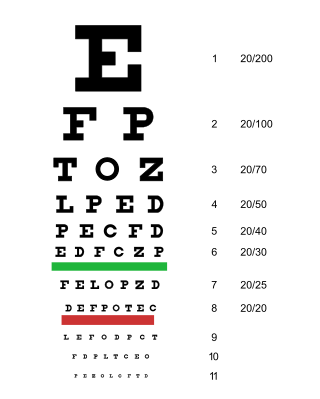
An eye examination is a series of tests performed to assess vision and ability to focus on and discern objects. It also includes other tests and examinations pertaining to the eyes. Eye examinations are primarily performed by an optometrist, ophthalmologist, or an orthoptist. Health care professionals often recommend that all people should have periodic and thorough eye examinations as part of routine primary care, especially since many eye diseases are asymptomatic.
Pediatric ophthalmology is a sub-speciality of ophthalmology concerned with eye diseases, visual development, and vision care in children.
Retinal hemorrhage is a disorder of the eye in which bleeding occurs in the retina, the light sensitive tissue, located on the back wall of the eye. There are photoreceptor cells in the retina called rods and cones, which transduce light energy into nerve signals that can be processed by the brain to form visual images. Retinal hemorrhage is strongly associated with child abuse in infants and young children and often leaves such abused infants permanently blind. In older children and adults, retinal hemorrhage can be caused by several medical conditions such as hypertension, retinal vein occlusion, anemia, leukemia or diabetes.
Leukocoria is an abnormal white reflection from the retina of the eye. Leukocoria resembles eyeshine, but leukocoria can also occur in animals that lack eyeshine because their retina lacks a tapetum lucidum.
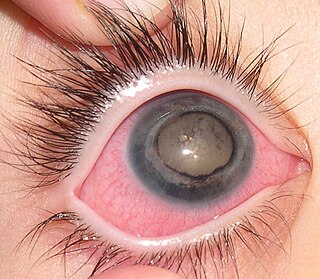
Coats' disease is a rare congenital, nonhereditary eye disorder, causing full or partial blindness, characterized by abnormal development of blood vessels behind the retina. Coats' disease can also fall under glaucoma.
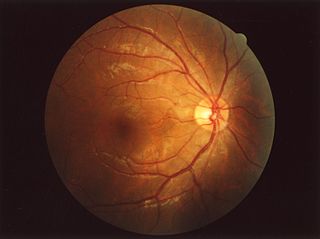
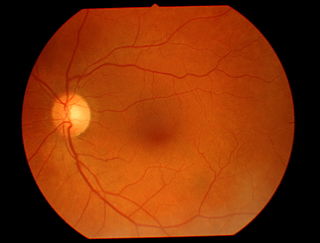
The fundus of the eye is the interior surface of the eye opposite the lens and includes the retina, optic disc, macula, fovea, and posterior pole. The fundus can be examined by ophthalmoscopy and/or fundus photography.

Dilated fundus examination (DFE) is a diagnostic procedure that uses mydriatic eye drops to dilate or enlarge the pupil in order to obtain a better view of the fundus of the eye. Once the pupil is dilated, examiners use ophthalmoscopy to view the eye's interior, which makes it easier to assess the retina, optic nerve head, blood vessels, and other important features. DFE has been found to be a more effective method for evaluating eye health when compared to non-dilated examination, and is the best method of evaluating structures behind the iris. It is frequently performed by ophthalmologists and optometrists as part of an eye examination.

Fundus photography involves photographing the rear of an eye, also known as the fundus. Specialized fundus cameras consisting of an intricate microscope attached to a flash enabled camera are used in fundus photography. The main structures that can be visualized on a fundus photo are the central and peripheral retina, optic disc and macula. Fundus photography can be performed with colored filters, or with specialized dyes including fluorescein and indocyanine green.
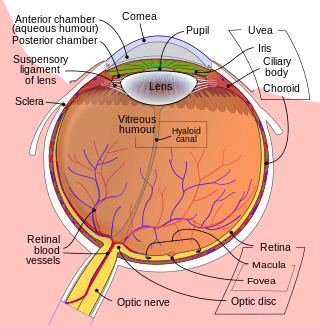
Intraocular hemorrhage is bleeding inside the eye. Bleeding can occur from any structure of the eye where there is vasculature or blood flow, including the anterior chamber, vitreous cavity, retina, choroid, suprachoroidal space, or optic disc.

Persistent fetal vasculature(PFV), also known as persistent fetal vasculature syndrome (PFVS), and until 1997 known primarily as persistent hyperplastic primary vitreous (PHPV), is a rare congenital anomaly which occurs when blood vessels within the developing eye, known as the embryonic hyaloid vasculature network, fail to regress as they normally would in-utero after the eye is fully developed. Defects which arise from this lack of vascular regression are diverse; as a result, the presentation, symptoms, and prognosis of affected patients vary widely, ranging from clinical insignificance to irreversible blindness. The underlying structural causes of PFV are considered to be relatively common, and the vast majority of cases do not warrant additional intervention. When symptoms do manifest, however, they are often significant, causing detrimental and irreversible visual impairment. Persistent fetal vasculature heightens the lifelong risk of glaucoma, cataracts, intraocular hemorrhages, and Retinal detachments, accounting for the visual loss of nearly 5% of the blind community in the developed world. In diagnosed cases of PFV, approximately 90% of patients with a unilateral disease have associated poor vision in the affected eye.
Elias I. Traboulsi is a physician in the fields of ophthalmic genetics and pediatric ophthalmology.

Congenital cataracts are a lens opacity that is present at birth. Congenital cataracts occur in a broad range of severity. Some lens opacities do not progress and are visually insignificant, others can produce profound visual impairment.
Teleophthalmology is a branch of telemedicine that delivers eye care through digital medical equipment and telecommunications technology. Today, applications of teleophthalmology encompass access to eye specialists for patients in remote areas, ophthalmic disease screening, diagnosis and monitoring; as well as distant learning.

Chloroquine retinopathy is a form of toxic retinopathy caused by the drugs chloroquine or hydroxychloroquine, which are sometimes used in the treatment of autoimmune disorders such as rheumatoid arthritis and systemic lupus erythematosus. This eye toxicity limits long-term use of the drugs.
Childhood cataract is cataract that occurs at birth or in childhood. It may be congenital or acquired.

Congenital blindness refers to blindness present at birth. Congenital blindness is sometimes used interchangeably with "Childhood Blindness." However, current literature has various definitions of both terms. Childhood blindness encompasses multiple diseases and conditions present in ages up to 16 years old, which can result in permanent blindness or severe visual impairment over time. Congenital blindness is a hereditary disease and can be treated by gene therapy. Visual loss in children or infants can occur either at the prenatal stage or postnatal stage. There are multiple possible causes of congenital blindness. In general, 60% of congenital blindness cases are contributed from prenatal stage and 40% are contributed from inherited disease. However, most of the congenital blindness cases show that it can be avoidable or preventable with early treatment.

Indocyanine green angiography (ICGA) is a diagnostic procedure used to examine choroidal blood flow and associated pathology. Indocyanine green (ICG) is a water soluble cyanine dye which shows fluorescence in near-infrared (790–805 nm) range, with peak spectral absorption of 800-810 nm in blood. The near infrared light used in ICGA penetrates ocular pigments such as melanin and xanthophyll, as well as exudates and thin layers of sub-retinal vessels. Age-related macular degeneration is the third main cause of blindness worldwide, and it is the leading cause of blindness in industrialized countries. Indocyanine green angiography is widely used to study choroidal neovascularization in patients with exudative age-related macular degeneration. In nonexudative AMD, ICGA is used in classification of drusen and associated subretinal deposits.
References
- ↑ "PhotoRED Technique". WE C Hope. Retrieved 2024-05-21.
- 1 2 3 4 5 6 7 American Association for Pediatric Ophthalmology and Strabismus; American Academy of Ophthalmology; American Association of Certified Orthoptists (2008). "Red Reflex Examination in Neonates, Infants, and Children". Pediatrics. 122 (6): 1401–1404. doi: 10.1542/peds.2008-2624 . PMID 19047263.
- ↑ Li, J.; Coats, D. K.; Fung, D.; Smith, E. O.; Paysse, E. (2010). "The Detection of Simulated Retinoblastoma by Using Red-Reflex Testing". Pediatrics. 126 (1): e202–e207. doi:10.1542/peds.2009-0882. PMID 20587677. S2CID 7071311.
- ↑ Shrestha, UD; Shrestha, MK; Yoon, PD; Yun, S.; Saiju, R. (2013). "Bruckner Red Light Reflex Test in a Hospital Setting". Kathmandu University Medical Journal. 10 (2): 23–26. doi: 10.3126/kumj.v10i2.7338 . PMID 23132470.
- ↑ Oğüt, M. S.; Bozkurt, N.; Ozek, E.; Birgen, H.; Kazokoğlú, H.; Oğüt, M. (1996). "Effects and side effects of mydriatic eyedrops in neonates". European Journal of Ophthalmology. 6 (2): 192–6. doi:10.1177/112067219600600218. PMID 8823596. S2CID 42351069.
- ↑ Gaynes BI (1998). "Monitoring drug safety: cardiac events in routine mydriasis". Optom Vis Sci. 75 (4): 245–246. doi:10.1097/00006324-199804000-00019. PMID 9586747.
- ↑ Pediatric eye exam and disease states, Mara Hover, DO. A T still University school of osteopathic medicine. November 2012.
- ↑ Procedures for the Evaluation of the Visual System by Pediatricians. Sean P. Donahue, MD, PhD, FAAP, Cynthia N Baker, MD, FAAP, COMMITTEE ON PRACTICE AND AMBULATORY MEDICINE, SECTION ON OPHTHALMOLOGY, AMERICAN ASSOCIATION OF CERTIFIED ORTHOPTISTS, AMERICAN ASSOCIATION FOR PEDIATRIC OPHTHALMOLOGY AND STRABISMUS, AMERICAN ACADEMY OF OPHTHALMOLOGY. https://pediatrics.aappublications.org/content/pediatrics/early/2015/12/07/peds.2015-3597.full-text.pdf
- ↑ Khan, A. O.; Al-Mesfer, S. (2005). "Lack of efficacy of dilated screening for retinoblastoma". Journal of Pediatric Ophthalmology and Strabismus. 42 (4): 205–10, quiz 233–4. doi:10.3928/01913913-20050701-01. PMID 16121549.
- ↑ American Academy of Ophthalmology Pediatric Ophthalmology/Strabismus Panel. Preferred practice pattern guidelines. Pediatric eye evaluations. San Francisco, Calif.: American Academy of Ophthalmology; 2007.
- ↑ Tongue, Andrea Cibis; Cibis, Gerhard W. (1981). "Brückner Test". Ophthalmology. 88 (10): 1041–1044. doi:10.1016/S0161-6420(81)80034-6. PMID 7335307.
- ↑ Paysse, E. A.; Williams, G. C.; Coats, D. K.; Williams, E. A. (2001). "Detection of Red Reflex Asymmetry by Pediatric Residents Using the Bruckner Reflex Versus the MTI Photoscreener". Pediatrics. 108 (4): e74. doi: 10.1542/peds.108.4.e74 . PMID 11581482.
- ↑ Wan, Michael J.; Vanderveen, Deborah K. (2015). "Eye disorders in newborn infants (Excluding retinopathy of prematurity)". Archives of Disease in Childhood - Fetal and Neonatal Edition. 100 (3): F264–F269. doi:10.1136/archdischild-2014-306215. PMID 25395469. S2CID 36687619.
- ↑ Hered RW (2011). "Effective vision screening of young children in the pediatric office". Pediatr Ann. 40 (2): 76–82. doi:10.3928/00904481-20110117-06. PMID 21323203.
- ↑ Melamud A, Palekar R, Singh A (2006). "Retinoblastoma [published correction appears in Am Fam Physician. 2007;75(7) 980]". Am Fam Physician. 73 (6): 1039–1044.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - 1 2 American Academy of Ophthalmology Pediatric Ophthalmology/Strabismus Panel. Preferred practice pattern guidelines. Pediatric eye evaluations. San Francisco, Calif.: American Academy of Ophthalmology; 2012.