
Plague is an infectious disease caused by the bacterium Yersinia pestis. Symptoms include fever, weakness and headache. Usually this begins one to seven days after exposure. There are three forms of plague, each affecting a different part of the body and causing associated symptoms. Pneumonic plague infects the lungs, causing shortness of breath, coughing and chest pain; bubonic plague affects the lymph nodes, making them swell; and septicemic plague infects the blood and can cause tissues to turn black and die.

Typhoid fever, also known as typhoid, is a disease caused by Salmonella serotype Typhi bacteria. Symptoms vary from mild to severe, and usually begin six to 30 days after exposure. Often there is a gradual onset of a high fever over several days. This is commonly accompanied by weakness, abdominal pain, constipation, headaches, and mild vomiting. Some people develop a skin rash with rose colored spots. In severe cases, people may experience confusion. Without treatment, symptoms may last weeks or months. Diarrhea may be severe, but is uncommon. Other people may carry it without being affected, but are still contagious. Typhoid fever is a type of enteric fever, along with paratyphoid fever. S. enterica Typhi is believed to infect and replicate only within humans.

An infection is the invasion of tissues by pathogens, their multiplication, and the reaction of host tissues to the infectious agent and the toxins they produce. An infectious disease, also known as a transmissible disease or communicable disease, is an illness resulting from an infection.

Epidemic typhus, also known as louse-borne typhus, is a form of typhus so named because the disease often causes epidemics following wars and natural disasters where civil life is disrupted. Epidemic typhus is spread to people through contact with infected body lice, in contrast to endemic typhus which is usually transmitted by fleas.

Rickettsia is a genus of nonmotile, gram-negative, nonspore-forming, highly pleomorphic bacteria that may occur in the forms of cocci, bacilli, or threads. The term "rickettsia" has nothing to do with rickets ; the bacterial genus Rickettsia instead was named after Howard Taylor Ricketts, in honor of his pioneering work on tick-borne spotted fever.

Rocky Mountain spotted fever (RMSF) is a bacterial disease spread by ticks. It typically begins with a fever and headache, which is followed a few days later with the development of a rash. The rash is generally made up of small spots of bleeding and starts on the wrists and ankles. Other symptoms may include muscle pains and vomiting. Long-term complications following recovery may include hearing loss or loss of part of an arm or leg.

Psittacosis—also known as parrot fever, and ornithosis—is a zoonotic infectious disease in humans caused by a bacterium called Chlamydia psittaci and contracted from infected parrots, such as macaws, cockatiels, and budgerigars, and from pigeons, sparrows, ducks, hens, gulls and many other species of birds. The incidence of infection in canaries and finches is believed to be lower than in psittacine birds.
Trench fever is a moderately serious disease transmitted by body lice. It infected armies in Flanders, France, Poland, Galicia, Italy, Macedonia, Mesopotamia, Russia and Egypt in World War I. Three noted cases during WWI were the authors J. R. R. Tolkien, A. A. Milne, and C. S. Lewis. From 1915 to 1918 between one-fifth and one-third of all British troops reported ill had trench fever while about one-fifth of ill German and Austrian troops had the disease. The disease persists among the homeless. Outbreaks have been documented, for example, in Seattle and Baltimore in the United States among injection drug users and in Marseille, France, and Burundi.

Leptospirosis is a blood infection caused by the bacteria Leptospira that can infect humans, dogs, rodents and many other wild and domesticated animals. Signs and symptoms can range from none to mild to severe. Weil's disease, the acute, severe form of leptospirosis, causes the infected individual to become jaundiced, develop kidney failure, and bleed. Bleeding from the lungs associated with leptospirosis is known as severe pulmonary haemorrhage syndrome.

Scrub typhus or bush typhus is a form of typhus caused by the intracellular parasite Orientia tsutsugamushi, a Gram-negative α-proteobacterium of family Rickettsiaceae first isolated and identified in 1930 in Japan.
Murray Valley encephalitis virus (MVEV) is a zoonotic flavivirus endemic to northern Australia and Papua New Guinea. It is the causal agent of Murray Valley encephalitis. In humans, it can cause permanent neurological disease or death. MVEV is related to Kunjin virus, which has a similar ecology, but a lower morbidity rate. Although the arbovirus is endemic to Northern Australia, it has occasionally spread to the southern states during times of heavy rainfall during the summer monsoon season via seasonal flooding of the Murray-Darling River system. These outbreaks can be "...decades apart, with no or very few cases identified in between".
The Weil–Felix test is an agglutination test for the diagnosis of rickettsial infections. It was first described in 1916. By virtue of its long history and of its simplicity, it has been one of the most widely employed tests for rickettsia on a global scale, despite being superseded in many settings by more sensitive and specific diagnostic tests. The Weil-Felix antibody was recently found to target rickettsia LPS O-antigen.
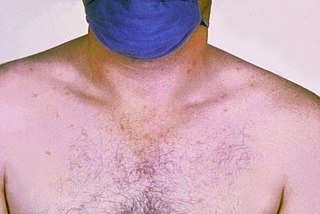
Paratyphoid fever, also known simply as paratyphoid, is a bacterial infection caused by one of three types of Salmonella enterica. Symptoms usually begin 6–30 days after exposure and are the same as those of typhoid fever. Often, a gradual onset of a high fever occurs over several days. Weakness, loss of appetite, and headaches also commonly occur. Some people develop a skin rash with rose-colored spots. Without treatment, symptoms may last weeks or months. Other people may carry the bacteria without being affected; however, they are still able to spread the disease to others. Typhoid and paratyphoid are of similar severity. Paratyphoid and typhoid fever are types of enteric fever.
Globalization, the flow of information, goods, capital, and people across political and geographic boundaries, allows infectious diseases to rapidly spread around the world, while also allowing the alleviation of factors such as hunger and poverty, which are key determinants of global health. The spread of diseases across wide geographic scales has increased through history. Early diseases that spread from Asia to Europe were bubonic plague, influenza of various types, and similar infectious diseases.
A rickettsiosis is a disease caused by intracellular bacteria.

Orientia tsutsugamushi is a mite-borne bacterium belonging to the family Rickettsiaceae and is responsible for a disease called scrub typhus in humans. It is a natural and an obligate intracellular parasite of mites belonging to the family Trombiculidae. With a genome of only 2.0–2.7 Mb, it has the most repeated DNA sequences among bacterial genomes sequenced so far. The disease, scrub typhus, occurs when infected mite larvae accidentally bite humans. Primarily indicated by undifferentiated febrile illnesses, the infection can be complicated and often fatal.
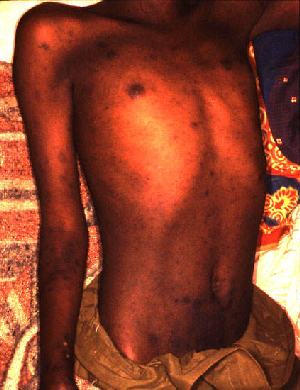
Typhus, also known as typhus fever, is a group of infectious diseases that include epidemic typhus, scrub typhus, and murine typhus. Common symptoms include fever, headache, and a rash. Typically these begin one to two weeks after exposure.
Rickettsia typhi is a small, aerobic, obligate intracellular, rod shaped gram negative bacterium. It belongs to the typhus group of the Rickettsia genus, along with R. prowazekii. R. typhi has an uncertain history, as it may have long gone shadowed by epidemic typhus. This bacterium is recognized as a biocontainment level 2/3 organism. R. typhi is a flea-borne disease that is best known to be the causative agent for the disease murine typhus, which is an endemic typhus in humans that is distributed worldwide. As with all rickettsial organisms, R. typhi is a zoonotic agent that causes the disease murine typhus, displaying non-specific mild symptoms of fevers, headaches, pains and rashes. There are two cycles of R. typhi transmission from animal reservoirs containing R. typhi to humans: a classic rat-flea-rat cycle that is most well studied and common, and a secondary periodomestic cycle that could involve cats, dogs, opossums, sheep, and their fleas.

African tick bite fever (ATBF) is a bacterial infection spread by the bite of a tick. Symptoms may include fever, headache, muscle pain, and a rash. At the site of the bite there is typically a red skin sore with a dark center. The onset of symptoms usually occurs 4–10 days after the bite. Complications are rare but may include joint inflammation. Some people do not develop symptoms.
Queensland tick typhus is a zoonotic disease caused by the bacterium Rickettsia australis. It is transmitted by the ticks Ixodes holocyclus and Ixodes tasmani.












