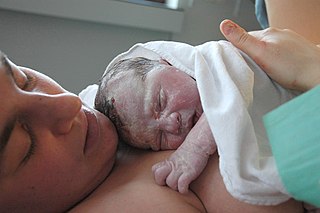
Childbirth, also known as labour and delivery, is the completion of pregnancy where one or more babies exits the internal environment of the mother via vaginal delivery or caesarean section. In 2019, there were about 140.11 million births globally. In the developed countries, most deliveries occur in hospitals, while in the developing countries most are home births.
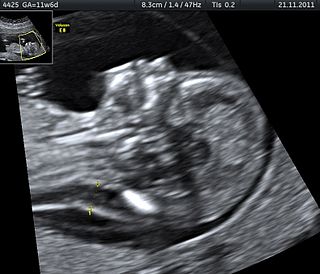
Stillbirth is typically defined as fetal death at or after 20 or 28 weeks of pregnancy, depending on the source. It results in a baby born without signs of life. A stillbirth can result in the feeling of guilt or grief in the mother. The term is in contrast to miscarriage, which is an early pregnancy loss, and Sudden Infant Death Syndrome, where the baby dies a short time after being born alive.
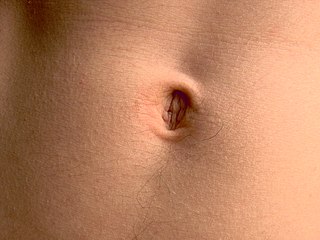
The navel is a protruding, flat, or hollowed area on the abdomen at the attachment site of the umbilical cord. All placental mammals have a navel, although it is generally more conspicuous in humans.

In placental mammals, the umbilical cord is a conduit between the developing embryo or fetus and the placenta. During prenatal development, the umbilical cord is physiologically and genetically part of the fetus and normally contains two arteries and one vein, buried within Wharton's jelly. The umbilical vein supplies the fetus with oxygenated, nutrient-rich blood from the placenta. Conversely, the fetal heart pumps low-oxygen, nutrient-depleted blood through the umbilical arteries back to the placenta.

Acute necrotizing ulcerative gingivitis (ANUG) is a common, non-contagious infection of the gums with sudden onset. The main features are painful, bleeding gums, and ulceration of inter-dental papillae. This disease, along with necrotizing (ulcerative) periodontitis is classified as a necrotizing periodontal disease, one of the seven general types of gum disease caused by inflammation of the gums (periodontitis).

Omphalocele or omphalocoele also called exomphalos, is a rare abdominal wall defect. Beginning at the 6th week of development, rapid elongation of the gut and increased liver size reduces intra abdominal space, which pushes intestinal loops out of the abdominal cavity. Around 10th week, the intestine returns to the abdominal cavity and the process is completed by the 12th week. Persistence of intestine or the presence of other abdominal viscera in the umbilical cord results in an omphalocele.

Congenital syphilis is syphilis present in utero and at birth, and occurs when a child is born to a mother with syphilis. Untreated early syphilis infections results in a high risk of poor pregnancy outcomes, including saddle nose, lower extremity abnormalities, miscarriages, premature births, stillbirths, or death in newborns. Some infants with congenital syphilis have symptoms at birth, but many develop symptoms later. Symptoms may include rash, fever, an enlarged liver and spleen, and skeletal abnormalities. Newborns will typically not develop a primary syphilitic chancre but may present with signs of secondary syphilis. Often these babies will develop syphilitic rhinitis ("snuffles"), the mucus from which is laden with the T. pallidum bacterium, and therefore highly infectious. If a baby with congenital syphilis is not treated early, damage to the bones, teeth, eyes, ears, and brain can occur.

Gastroschisis is a birth defect in which the baby's intestines extend outside of the abdomen through a hole next to the belly button. The size of the hole is variable, and other organs including the stomach and liver may also occur outside the baby's body. Complications may include feeding problems, prematurity, intestinal atresia, and intrauterine growth restriction.

Lotus birth is the practice of leaving the umbilical cord uncut after childbirth so that the baby is left attached to the placenta until the cord naturally separates at the umbilicus. This usually occurs within 3–10 days after birth. The practice is performed mainly for spiritual purposes, including for the perceived spiritual connection between the placenta and the newborn.

Ear pain, also known as earache or otalgia, is pain in the ear. Primary ear pain is pain that originates from the ear. Secondary ear pain is a type of referred pain, meaning that the source of the pain differs from the location where the pain is felt.
Necrotizing enterocolitis (NEC) is a devastating intestinal disease that affects premature or very low birth weight infants. Symptoms may include poor feeding, bloating, decreased activity, blood in the stool, vomiting of bile, bowel death, multiorgan failure, and even death.

Prelabor rupture of membranes (PROM), previously known as premature rupture of membranes, is breakage of the amniotic sac before the onset of labor. Women usually experience a painless gush or a steady leakage of fluid from the vagina. Complications in the baby may include premature birth, cord compression, and infection. Complications in the mother may include placental abruption and postpartum endometritis.
Omphalitis of newborn is the medical term for inflammation of the umbilical cord stump in the neonatal newborn period, most commonly attributed to a bacterial infection. Typically immediately after an infant is born, the umbilical cord is cut with a small remnant left behind. Normally the stump separates from the skin within 3–45 days after birth. A small amount of pus-like material is commonly seen at the base of the stump and can be controlled by keeping the stump open to air to dry. Certain bacteria can grow and infect the stump during this process and as a result significant redness and swelling may develop, and in some cases the infection can then spread through the umbilical vessels to the rest of the body. While currently an uncommon anatomical location for infection in the newborn in the United States, it has caused significant morbidity and mortality both historically and in areas where health care is less readily available. In general, when this type of infection is suspected or diagnosed, antibiotic treatment is given, and in cases of serious complications surgical management may be appropriate.

Neurosyphilis refers to infection of the central nervous system in a patient with syphilis. In the era of modern antibiotics, the majority of neurosyphilis cases have been reported in HIV-infected patients. Meningitis is the most common neurological presentation in early syphilis. Tertiary syphilis symptoms are exclusively neurosyphilis, though neurosyphilis may occur at any stage of infection.

Chorioamnionitis, also known as intra-amniotic infection (IAI), is inflammation of the fetal membranes, usually due to bacterial infection. In 2015, a National Institute of Child Health and Human Development Workshop expert panel recommended use of the term "triple I" to address the heterogeneity of this disorder. The term triple I refers to intrauterine infection or inflammation or both and is defined by strict diagnostic criteria, but this terminology has not been commonly adopted although the criteria are used.
Clostridial necrotizing enteritis (CNE) is a severe and potentially fatal type of food poisoning caused by a β-toxin of Clostridium perfringens, Type C. It occurs in some developing regions, particularly in New Guinea, where it is known as pig-bel. The disease was also documented in Germany following World War II, where it was called Darmbrand. The toxin is normally inactivated by certain proteolytic enzymes and by normal cooking, but when these protections are impeded by diverse factors, and high protein is consumed, the disease can emerge.
Umbilical granuloma is the most common umbilical abnormality in newborn children or neonates, causing inflammation and drainage. It may appear in the first few weeks of newborn infants during the healing process of the umbilical cord due to an umbilical mass. It is the overgrowth of the umbilical tissue. It develops in about 1 out of 500 newborns. With appropriate treatment, it is expected to heal in 1~2 weeks.

Circumvallate placenta is a rare condition affecting about 1-2% of pregnancies, in which the amnion and chorion fetal membranes essentially "double back" on the fetal side around the edges of the placenta. After delivery, a circumvallate placenta has a thick ring of membranes on its fetal surface. Circumvallate placenta is a placental morphological abnormality associated with increased fetal morbidity and mortality due to the restricted availability of nutrients and oxygen to the developing fetus.
Neonatal stroke, similar to a stroke which occurs in adults, is defined as a disturbance to the blood supply of the developing brain in the first 28 days of life. This description includes both ischemic events, which results from a blockage of vessels, and hypoxic events, which results from a lack of oxygen to the brain tissue, as well as some combination of the two. One treatment with some proven benefits is hypothermia, but may be most beneficial in conjunction with pharmacological agents. Well-designed clinical trials for stroke treatment in neonates are lacking, but some current studies involve the transplantation of neural stem cells and umbilical cord stem cells; it is not yet known if this therapy is likely to be successful.

Neonatal infections are infections of the neonate (newborn) acquired during prenatal development or within the first four weeks of life. Neonatal infections may be contracted by mother to child transmission, in the birth canal during childbirth, or after birth. Neonatal infections may present soon after delivery, or take several weeks to show symptoms. Some neonatal infections such as HIV, hepatitis B, and malaria do not become apparent until much later. Signs and symptoms of infection may include respiratory distress, temperature instability, irritability, poor feeding, failure to thrive, persistent crying and skin rashes.















