Management is the directing of a group of people or entities toward a goal.
Contents
Management may also refer to:
Management is the directing of a group of people or entities toward a goal.
Management may also refer to:

Risk management is the identification, evaluation, and prioritization of risks, followed by the minimization, monitoring, and control of the impact or probability of those risks occurring. Risks can come from various sources including uncertainty in international markets, political instability, dangers of project failures, legal liabilities, credit risk, accidents, natural causes and disasters, deliberate attack from an adversary, or events of uncertain or unpredictable root-cause.
Health has a variety of definitions, which have been used for different purposes over time. In general, it refers to physical and emotional well-being, especially that associated with normal functioning of the human body, absent of disease, pain, or injury.
In science and engineering, root cause analysis (RCA) is a method of problem solving used for identifying the root causes of faults or problems. It is widely used in IT operations, manufacturing, telecommunications, industrial process control, accident analysis (e.g., in aviation, rail transport, or nuclear plants), medical diagnosis, the healthcare industry (e.g., for epidemiology), etc. Root cause analysis is a form of inductive inference (first create a theory, or root, based on empirical evidence, or causes) and deductive inference (test the theory, i.e., the underlying causal mechanisms, with empirical data).
Registry may refer to:

Health informatics combines communications, information technology (IT), and health care to enhance patient care and is at the forefront of the medical technological revolution. It can be viewed as a branch of engineering and applied science.

The Health Insurance Portability and Accountability Act of 1996 is a United States Act of Congress enacted by the 104th United States Congress and signed into law by President Bill Clinton on August 21, 1996. It aimed to alter the transfer of healthcare information, stipulated the guidelines by which personally identifiable information maintained by the healthcare and healthcare insurance industries should be protected from fraud and theft, and addressed some limitations on healthcare insurance coverage. It generally prohibits healthcare providers and businesses called covered entities from disclosing protected information to anyone other than a patient and the patient's authorized representatives without their consent. The bill does not restrict patients from receiving information about themselves. Furthermore, it does not prohibit patients from voluntarily sharing their health information however they choose, nor does it require confidentiality where a patient discloses medical information to family members, friends or other individuals not employees of a covered entity.
Control may refer to:
The term managed care or managed healthcare is used in the United States to describe a group of activities intended to reduce the cost of providing health care and providing American health insurance while improving the quality of that care. It has become the predominant system of delivering and receiving American health care since its implementation in the early 1980s, and has been largely unaffected by the Affordable Care Act of 2010.
...intended to reduce unnecessary health care costs through a variety of mechanisms, including: economic incentives for physicians and patients to select less costly forms of care; programs for reviewing the medical necessity of specific services; increased beneficiary cost sharing; controls on inpatient admissions and lengths of stay; the establishment of cost-sharing incentives for outpatient surgery; selective contracting with health care providers; and the intensive management of high-cost health care cases. The programs may be provided in a variety of settings, such as Health Maintenance Organizations and Preferred Provider Organizations.

A medical device is any device intended to be used for medical purposes. Significant potential for hazards are inherent when using a device for medical purposes and thus medical devices must be proved safe and effective with reasonable assurance before regulating governments allow marketing of the device in their country. As a general rule, as the associated risk of the device increases the amount of testing required to establish safety and efficacy also increases. Further, as associated risk increases the potential benefit to the patient must also increase.
eHealth describes healthcare services which are supported by digital processes, communication or technology such as electronic prescribing, Telehealth, or Electronic Health Records (EHRs). The term "eHealth" originated in the 1990s, initially conceived as "Internet medicine," but has since evolved to have a broader range of technologies and innovations aimed at enhancing healthcare delivery and accessibility. According to the World Health Organization (WHO), eHealth encompasses not only internet-based healthcare services but also modern advancements such as artificial intelligence, mHealth, and telehealth, which collectively aim to improve accessibility and efficiency in healthcare delivery. Usage of the term varies widely. A study in 2005 found 51 unique definitions of eHealth, reflecting its diverse applications and interpretations. While some argue that it is interchangeable with health informatics as a broad term covering electronic/digital processes in health, others use it in the narrower sense of healthcare practice specifically facilitated by the Internet. It also includes health applications and links on mobile phones, referred to as mHealth or m-Health.. Key components of eHealth include electronic health records (EHRs), telemedicine, health information exchange, mobile health applications, wearable devices, and online health information. For example, diabetes monitoring apps allow patients to track health metrics in real time, bridging the gap between home and clinical care. These technologies enable healthcare providers, patients, and other stakeholders to access, manage, and exchange health information more effectively, leading to improved communication, decision-making, and overall healthcare outcomes.
Public health surveillance is, according to the World Health Organization (WHO), "the continuous, systematic collection, analysis and interpretation of health-related data needed for the planning, implementation, and evaluation of public health practice." Public health surveillance may be used to track emerging health-related issues at an early stage and find active solutions in a timely manner. Surveillance systems are generally called upon to provide information regarding when and where health problems are occurring and who is affected.
Monitoring may refer to:
Clinical research is a branch of medical research that involves people and aims to determine the effectiveness (efficacy) and safety of medications, devices, diagnostic products, and treatment regimens intended for improving human health. These research procedures are designed for the prevention, treatment, diagnosis or understanding of disease symptoms.
Public health informatics has been defined as the systematic application of information and computer science and technology to public health practice, research, and learning. It is one of the subdomains of health informatics, data management applied to medical systems.
The following outline is provided as an overview of and topical guide to business management:

Patient education is a planned interactive learning process designed to support and enable expert patients to manage their life with a disease and/or optimise their health and well-being.
Chronic care management encompasses the oversight and education activities conducted by health care professionals to help patients with chronic diseases and health conditions such as diabetes, high blood pressure, systemic lupus erythematosus, multiple sclerosis, and sleep apnea learn to understand their condition and live successfully with it. This term is equivalent to disease management for chronic conditions. The work involves motivating patients to persist in necessary therapies and interventions and helping them to achieve an ongoing, reasonable quality of life.
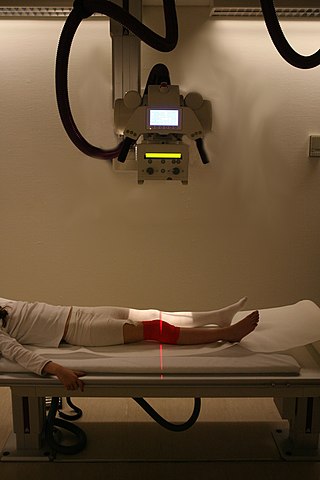
Medical diagnosis is the process of determining which disease or condition explains a person's symptoms and signs. It is most often referred to as a diagnosis with the medical context being implicit. The information required for a diagnosis is typically collected from a history and physical examination of the person seeking medical care. Often, one or more diagnostic procedures, such as medical tests, are also done during the process. Sometimes the posthumous diagnosis is considered a kind of medical diagnosis.
A glossary of terms used in clinical research.
Clinical nutrition centers on the prevention, diagnosis, and management of nutritional changes in patients linked to chronic diseases and conditions primarily in health care. Clinical in this sense refers to the management of patients, including not only outpatients at clinics and in private practice, but also inpatients in hospitals. It incorporates primarily the scientific fields of nutrition and dietetics. Furthermore, clinical nutrition aims to maintain a healthy energy balance, while also providing sufficient amounts of nutrients such as protein, vitamins, and minerals to patients.