Angiomas are benign tumors derived from cells of the vascular or lymphatic vessel walls (endothelium) or derived from cells of the tissues surrounding these vessels.

Lymphangioleiomyomatosis (LAM) is a rare, progressive and systemic disease that typically results in cystic lung destruction. It predominantly affects women, especially during childbearing years. The term sporadic LAM is used for patients with LAM not associated with tuberous sclerosis complex (TSC), while TSC-LAM refers to LAM that is associated with TSC.
A cystic hygroma is an abnormal growth that usually appears on a baby's neck or head. It consists of one or more cysts and tends to grow larger over time. The disorder usually develops while the fetus is still in the uterus, but can also appear after birth.

Angiokeratoma is a benign cutaneous lesion of capillaries, resulting in small marks of red to blue color and characterized by hyperkeratosis. Angiokeratoma corporis diffusum refers to Fabry's disease, but this is usually considered a distinct condition.
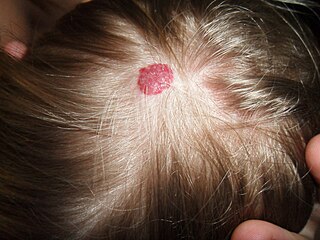
A vascular tumor is a tumor of vascular origin; a soft tissue growth that can be either benign or malignant, formed from blood vessels or lymph vessels. Examples of vascular tumors include hemangiomas, lymphangiomas, hemangioendotheliomas, Kaposi's sarcomas, angiosarcomas, and hemangioblastomas. An angioma refers to any type of benign vascular tumor.

Aneurysmal bone cyst (ABC) is a non-cancerous bone tumor composed of multiple varying sizes of spaces in a bone which are filled with blood. The term is a misnomer, as the lesion is neither an aneurysm nor a cyst. It generally presents with pain and swelling in the affected bone. Pressure on neighbouring tissues may cause compression effects such as neurological symptoms.

Lymphangiomatosis is a condition where a lymphangioma is not present in a single localised mass, but in a widespread or multifocal manner. It is a rare type of tumor which results from an abnormal development of the lymphatic system.

A persistent thyroglossal duct is a usually benign medical condition in which the thyroglossal duct, a structure usually only found during embryonic development, fails to atrophy. The duct persists as a midline structure forming an open connection between the back of the tongue and the thyroid gland. This opening can lead to fluid accumulation and infection, which necessitate the removal of the duct.
A vascular malformation is a type of vascular anomaly. They may cause aesthetic problems as they have a growth cycle, and can continue to grow throughout life.

Kimura's disease is a benign rare chronic inflammatory disorder. Its primary symptoms are subdermal lesions in the head or neck or painless unilateral inflammation of cervical lymph nodes.

Superficial lymphatic malformation is a congenital malformation of the superficial lymphatics, presenting as groups of deep-seated, vesicle-like papules resembling frog spawn, at birth or shortly thereafter. Lymphangioma circumscriptum is the most common congenital lymphatic malformation. It is a benign condition and treatment is not required if the person who has it does not have symptoms from it.

Spiradenomas (SA) are rare, benign cutaneous adnexal tumors that may progress to become their malignant counterparts, i.e. spiradenocarcinomas (SAC). Cutaneous adnexal tumors are a group of skin tumors consisting of tissues that have differentiated towards one of the four primary adnexal structures found in normal skin: hair follicles, sebaceous sweat glands, apocrine sweat glands, and eccrine sweat glands. SA and SAC tumors were regarded as eccrine gland tumors and termed eccrine spiradenomas and eccrine spiradenocarcinomas, respectively. However, more recent studies have found them to be hair follicle tumors and commonly term them spiradenomas and spiradenocarcinomas, respectively. Further confusing the situation, SA-like and SAC-like tumors are also 1) manifestations of the inherited disorder, CYLD cutaneous syndrome (CCS), and 2) have repeatedly been confused with an entirely different tumor, adenoid cystic carcinomas of the salivary gland. Here, SA and SAC are strictly defined as sporadic hair follicle tumors that do not include the hereditary CCS spiradenomas and heridtary spiradenocarcinoms of CCS or the adenoid cystic carcinomas.

Bonnet–Dechaume–Blanc syndrome, also known as Wyburn-Mason syndrome, is a rare congenital disorder characterized by arteriovenous malformations of the brain, retina or facial nevi. The syndrome has a number of possible symptoms and can, more rarely, affect the skin, bones, kidneys, muscles, and gastrointestinal tract. When the syndrome affects the brain, people can experience severe headaches, seizures, acute stroke, meningism, and progressive neurological deficits due to acute or chronic ischaemia caused by arteriovenous shunting.
A vascular anomaly is any of a range of lesions from a simple birthmark to a large tumor that may be disfiguring. They are caused by a disorder of the vascular system. A vascular anomaly is a localized defect in blood vessels or lymph vessels. These defects are characterized by an increased number of vessels, and vessels that are both enlarged and heavily curved. Some vascular anomalies are congenital, others appear within weeks to years after birth, and others are acquired by trauma or during pregnancy. Inherited vascular anomalies are also described and often present with a number of lesions that increase with age. Vascular anomalies can also be a part of a syndrome.
Lymphohemangioma is a disease characterized by swelling of the lymph nodes and blood vessels. It is variously described as a "mixture of clear fluid and blood-filled cysts", a mass of abnormal swollen veins and lymph nodes, or a tumorous growth of lymph and blood vessels. Oftentimes, it is described as a misnomer for combined lymphatic and capillary malformation. The lymphangiomas are known to be malformations of the lymph tissue, 75% of which is found near the head and neck. However, it can affect any region of the body. This disease is most commonly observed in children and male patients. In fact, Lymphangiomas account for 4% of all vascular tumors and 25% of the benign vascular tumors in children. Additionally, 50% of Lymphangiomas are noted at birth and become more evident by age 5.

Scrotalultrasound is a medical ultrasound examination of the scrotum. It is used in the evaluation of testicular pain, and can help identify solid masses.
Stasis papillomatosis is a disease characterized by chronic congestion of the extremities, with blood circulation interrupted in a specific area of the body. A consequence of this congestion and inflammation is long-term lymphatic obstruction (lymphedema). It is also typically characterized by the appearance of numerous papules. Injuries can range from small to large plates composed of brown or pink, smooth or hyperkeratotic papules. The most typical areas where injuries occur are the back of the feet, the toes, the legs, and the area around a venous ulcer formed in the extremities, although the latter is the rarest of all. These injuries include pachydermia, lymphedema, lymphomastic verrucosis and elephantosis verrucosa. The disease can be either localized or generalized; the localized form makes up 78% of cases. Treatment includes surgical and pharmaceutical intervention; indications for partial removal include advanced fibrotic lymphedema and elephantiasis. Despite the existence of these treatments, chronic venous edema, which is a derivation of stasis papillomatosis, is only partially reversible. The skin is also affected and its partial removal may mean that the skin and the subcutaneous tissue are excised. A side effect of the procedure is the destruction of existing cutaneous lymphatic vessels. It also risks papillomatosis, skin necrosis and edema exacerbation.
Fibro-adipose vascular anomaly, also known as FAVA, is a type of vascular anomaly that is both rare and painful. FAVA is characterized by tough fibrofatty tissue taking over portions of muscle, most often contained within a single limb. FAVA also causes venous and/or lymphatic abnormalities.
In CT scan of the thyroid, focal and diffuse thyroid abnormalities are commonly encountered. These findings can often lead to a diagnostic dilemma, as the CT reflects nonspecific appearances. Ultrasound (US) examination has a superior spatial resolution and is considered the modality of choice for thyroid evaluation. Nevertheless, CT detects incidental thyroid nodules (ITNs) and plays an important role in the evaluation of thyroid cancer.
Diffuse capillary malformation with overgrowth (DCMO) is a subset of capillary malformations (CM) associated with hypertrophy, i.e. increased size of body structures. CM can be considered an umbrella term for various vascular anomalies caused by increased diameter or number of capillary blood vessels. It is commonly referred to as "port-wine stain", and is thought to affect approximately 0.5% of the population. Typically capillaries in the papillary dermis are involved, and this gives rise to pink or violaceous colored lesions. The majority of DCMO lesions are diffuse, reticulated pale-colored stains.