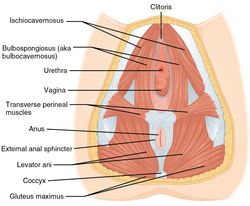
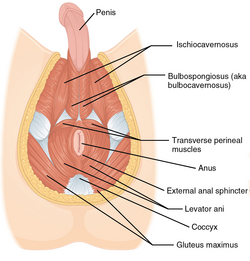
The perineum in mammals is the space between the anus and the genitals. The human perineum is between the anus and scrotum in the male or between the anus and vulva in the female. The perineum is the region of the body between the pubic symphysis and the coccyx, including the perineal body and surrounding structures. The perineal raphe is visible and pronounced to varying degrees. The perineum is an erogenous zone. This area is also known as the taint or gooch in American slang.

The Bartholin's glands are two pea-sized compound alveolar glands located slightly posterior and to the left and right of the opening of the vagina. They secrete mucus to lubricate the vagina.

The levator ani is a broad, thin muscle group, situated on either side of the pelvis. It is formed from three muscle components: the pubococcygeus, the iliococcygeus, and the puborectalis.

The bulbospongiosus muscles are a subgroup of the superficial muscles of the perineum. They have a slightly different origin, insertion and function in males and females. In males, these muscles cover the bulb of the penis, while in females, they cover the vestibular bulbs.

The pelvic floor or pelvic diaphragm is an anatomical location in the human body, which has an important role in urinary and anal continence, sexual function and support of the pelvic organs. The pelvic floor includes muscles, both skeletal and smooth, ligaments and fascia. and separates between the pelvic cavity from above, and the perineum from below. It is formed by the levator ani muscle and coccygeus muscle, and associated connective tissue.
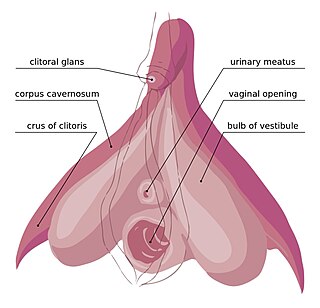
In female anatomy, the vestibular bulbs, bulbs of the vestibule or clitoral bulbs are two elongated masses of erectile tissue typically described as being situated on either side of the vaginal opening. They are united to each other in front by a narrow median band. Some research indicates that they do not surround the vaginal opening, and are more closely related to the clitoris than to the vestibule. They constitute the root of the clitoris along with the crura.

The posterior cutaneous nerve of the thigh is a sensory nerve of the thigh. It is a branch of the sacral plexus. It supplies the skin of the posterior surface of the thigh, leg, buttock, and also the perineum.
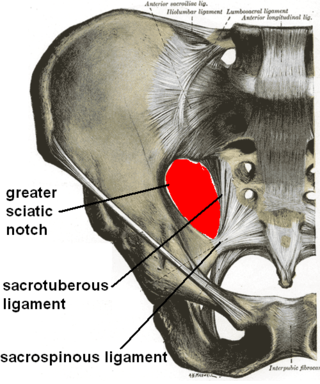
The sacrotuberous ligament is situated at the lower and back part of the pelvis. It is flat, and triangular in form; narrower in the middle than at the ends.
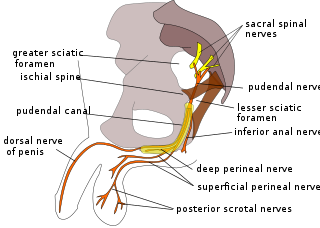
The perineal nerve is a nerve of the pelvis. It arises from the pudendal nerve in the pudendal canal. It gives superficial branches to the skin, and a deep branch to muscles. It supplies the skin and muscles of the perineum. Its latency is tested with electrodes.

The membranous layer of the superficial fascia of the perineum is the deeper layer of the superficial perineal fascia. It is thin, aponeurotic in structure, and of considerable strength, serving to bind down the muscles of the root of the penis. Colles' fascia emerges from the perineal membrane, which divides the base of the penis from the prostate. Colles' fascia emerges from the inferior side of the perineal membrane and continues along the ventral (inferior) penis without covering the scrotum. It separates the skin and subcutaneous fat from the superficial perineal pouch.

The posterior scrotal branches are two in number, medial and lateral. They are branches of the perineal nerve, which is itself a branch of the pudendal nerve. The pudendal nerve arises from spinal roots S2 through S4, travels through the pudendal canal on the fascia of the obturator internus muscle, and gives off the perineal nerve in the perineum. The major branch of the perineal nerve is the posterior scrotal/posterior labial.

The perineal membrane is an anatomical term for a fibrous membrane in the perineum. The term "inferior fascia of urogenital diaphragm", used in older texts, is considered equivalent to the perineal membrane.

The superficial perineal pouch is a compartment of the perineum.

The deep perineal pouch is the anatomic space enclosed in part by the perineum and located superior to the perineal membrane.

The anal triangle is the posterior part of the perineum. It contains the anus in mammals.

The posterior labial nerves are branches of the pudendal nerve. They supply the female labia majora.

The bulb of penis is the proximal/posterior end of the corpus spongiosum. Together with the two crura, it constitutes the root of the penis. It is covered by the bulbospongiosus.

The following outline is provided as an overview of and topical guide to human anatomy:

In human male anatomy, the radix or root of the penis is the internal and most proximal portion of the human penis that lies in the perineum. Unlike the pendulous body of the penis, which is suspended from the pubic symphysis, the root is attached to the pubic arch of the pelvis and is not visible externally. It is triradiate in form, consisting of three masses of erectile tissue; the two diverging crura, one on either side, and the median bulb of the penis or urethral bulb. Approximately one third to one half of the penis is embedded in the pelvis and can be felt through the scrotum and in the perineum.

The vaginal support structures are those muscles, bones, ligaments, tendons, membranes and fascia, of the pelvic floor that maintain the position of the vagina within the pelvic cavity and allow the normal functioning of the vagina and other reproductive structures in the female. Defects or injuries to these support structures in the pelvic floor leads to pelvic organ prolapse. Anatomical and congenital variations of vaginal support structures can predispose a woman to further dysfunction and prolapse later in life. The urethra is part of the anterior wall of the vagina and damage to the support structures there can lead to incontinence and urinary retention.