Related Research Articles

Compartment syndrome is a condition in which increased pressure within one of the body's anatomical compartments results in insufficient blood supply to tissue within that space. There are two main types: acute and chronic. Compartments of the leg or arm are most commonly involved.

Gangrene is a type of tissue death caused by a lack of blood supply. Symptoms may include a change in skin color to red or black, numbness, swelling, pain, skin breakdown, and coolness. The feet and hands are most commonly affected. If the gangrene is caused by an infectious agent, it may present with a fever or sepsis.

De Quervain syndrome occurs when two tendons that control movement of the thumb become constricted by their tendon sheath in the wrist. This results in pain and tenderness on the thumb side of the wrist. Radial abduction of the thumb is painful. On some occasions, there is uneven movement or triggering of the thumb with radial abduction. Symptoms can come on gradually or be noted suddenly.
Malingering is the fabrication, feigning, or exaggeration of physical or psychological symptoms designed to achieve a desired outcome, such as personal gain, relief from duty or work, avoiding arrest, receiving medication, and mitigating prison sentencing. It presents a complex ethical dilemma within domains of society, including healthcare, legal systems, and employment settings.

Necrotizing fasciitis (NF), also known as flesh-eating disease, is a bacterial infection that results in the death of parts of the body's soft tissue. It is a severe disease of sudden onset that spreads rapidly. Symptoms usually include red or purple skin in the affected area, severe pain, fever, and vomiting. The most commonly affected areas are the limbs and perineum.

Ischemia or ischaemia is a restriction in blood supply to any tissue, muscle group, or organ of the body, causing a shortage of oxygen that is needed for cellular metabolism. Ischemia is generally caused by problems with blood vessels, with resultant damage to or dysfunction of tissue i.e. hypoxia and microvascular dysfunction. It also implies local hypoxia in a part of a body resulting from constriction.
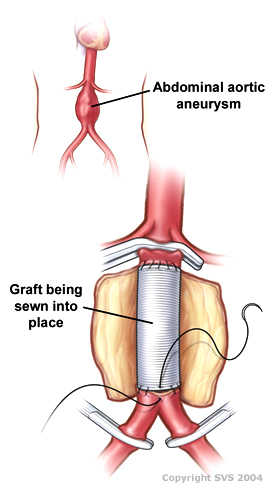
Vascular surgery is a surgical subspecialty in which vascular diseases involving the arteries, veins, or lymphatic vessels, are managed by medical therapy, minimally-invasive catheter procedures and surgical reconstruction. The specialty evolved from general and cardiovascular surgery where it refined the management of just the vessels, no longer treating the heart or other organs. Modern vascular surgery includes open surgery techniques, endovascular techniques and medical management of vascular diseases - unlike the parent specialities. The vascular surgeon is trained in the diagnosis and management of diseases affecting all parts of the vascular system excluding the coronaries and intracranial vasculature. Vascular surgeons also are called to assist other physicians to carry out surgery near vessels, or to salvage vascular injuries that include hemorrhage control, dissection, occlusion or simply for safe exposure of vascular structures.

Abdominal pain, also known as a stomach ache, is a symptom associated with both non-serious and serious medical issues. Since the abdomen contains most of the body's vital organs, it can be an indicator of a wide variety of diseases. Given that, approaching the examination of a person and planning of a differential diagnosis is extremely important.

Plantar fasciitis or plantar heel pain is a disorder of the plantar fascia, which is the connective tissue that supports the arch of the foot. It results in pain in the heel and bottom of the foot that is usually most severe with the first steps of the day or following a period of rest. Pain is also frequently brought on by bending the foot and toes up towards the shin. The pain typically comes on gradually, and it affects both feet in about one-third of cases.

Mallory–Weiss syndrome is a condition where high intra-abdominal pressures causes laceration and bleeding of the mucosa called Mallory-Weiss tears. Additionally, Mallory-Weiss syndrome is one of the most common causes of acute upper gastrointestinal bleeding, counting of around 1-15% of all cases in adults and less than 5% in children. It has been found that tears are up to 2 to 4 times more prevalent in men than women. The tears can cause upper gastrointestinal bleeding and predominantly occur where the esophagus meets the stomach. However, the tears can happen anywhere from the middle of the esophagus to the cardia of the stomach. Mallory-Weiss syndrome is often caused by constant vomiting and retching from alcoholism or bulimia. Gastroesophageal reflux disease (GERD) is another risk factor that is often linked with Mallory-Weiss syndrome. However, not every individual with Mallory-Weiss syndrome will have these risk factors. Individuals with Mallory-Weiss syndrome will have hematemesis, however the symptoms can vary.

Epiglottitis is the inflammation of the epiglottis—the flap at the base of the tongue that prevents food entering the trachea (windpipe). Symptoms are usually rapid in onset and include trouble swallowing which can result in drooling, changes to the voice, fever, and an increased breathing rate. As the epiglottis is in the upper airway, swelling can interfere with breathing. People may lean forward in an effort to open the airway. As the condition worsens, stridor and bluish skin may occur.

Costochondritis, also known as chest wall pain syndrome or costosternal syndrome, is a benign inflammation of the upper costochondral and sternocostal joints. 90% of patients are affected in multiple ribs on a single side, typically at the 2nd to 5th ribs. Chest pain, the primary symptom of costochondritis, is considered a symptom of a medical emergency, making costochondritis a common presentation in the emergency department. One study found costochondritis was responsible for 30% of patients with chest pain in an emergency department setting.

Ischemic colitis is a medical condition in which inflammation and injury of the large intestine result from inadequate blood supply (ischemia). Although uncommon in the general population, ischemic colitis occurs with greater frequency in the elderly, and is the most common form of bowel ischemia. Causes of the reduced blood flow can include changes in the systemic circulation or local factors such as constriction of blood vessels or a blood clot. In most cases, no specific cause can be identified.

In the anatomy of the human digestive tract, there are two colic flexures, or curvatures in the transverse colon. The right colic flexure is also known as the hepatic flexure, and the left colic flexure is also known as the splenic flexure. Note that "right" refers to the patient's anatomical right, which may be depicted on the left of a diagram.
An acute abdomen refers to a sudden, severe abdominal pain. It is in many cases a medical emergency, requiring urgent and specific diagnosis. Several causes need immediate surgical treatment.
Abdominal angina is abdominal pain after eating that occurs in individuals with ongoing poor blood supply to their small intestines known as chronic mesenteric ischemia. Although the term angina alone usually denotes angina pectoris, angina by itself can also mean "any spasmodic, choking, or suffocative pain", with an anatomic adjective defining its focus; so, in this case, spasmodic pain in the abdomen. Stedman's Medical Dictionary Online defines abdominal angina as "intermittent abdominal pain, frequently occurring at a fixed time after eating, caused by inadequacy of the mesenteric circulation resulting from arteriosclerosis or other arterial disease. Synonym: intestinal angina."
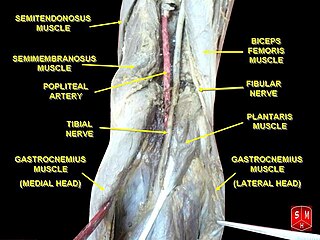
The popliteal artery entrapment syndrome (PAES) is an uncommon pathology that occurs when the popliteal artery is compressed by the surrounding popliteal fossa myofascial structures. This results in claudication and chronic leg ischemia. This condition mainly occurs more in young athletes than in the elderlies. Elderlies, who present with similar symptoms, are more likely to be diagnosed with peripheral artery disease with associated atherosclerosis. Patients with PAES mainly present with intermittent feet and calf pain associated with exercises and relieved with rest. PAES can be diagnosed with a combination of medical history, physical examination, and advanced imaging modalities such as duplex ultrasound, computer tomography, or magnetic resonance angiography. Management can range from non-intervention to open surgical decompression with a generally good prognosis. Complications of untreated PAES can include stenotic artery degeneration, complete popliteal artery occlusion, distal arterial thromboembolism, or even formation of an aneurysm.
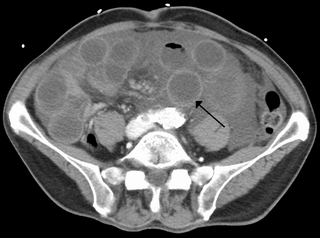
Intestinal ischemia is a medical condition in which injury to the large or small intestine occurs due to not enough blood supply. It can come on suddenly, known as acute intestinal ischemia, or gradually, known as chronic intestinal ischemia. The acute form of the disease often presents with sudden severe abdominal pain and is associated with a high risk of death. The chronic form typically presents more gradually with abdominal pain after eating, unintentional weight loss, vomiting, and fear of eating.

Superior mesenteric artery (SMA) syndrome is a gastro-vascular disorder in which the third and final portion of the duodenum is compressed between the abdominal aorta (AA) and the overlying superior mesenteric artery. This rare, potentially life-threatening syndrome is typically caused by an angle of 6–25° between the AA and the SMA, in comparison to the normal range of 38–56°, due to a lack of retroperitoneal and visceral fat. In addition, the aortomesenteric distance is 2–8 millimeters, as opposed to the typical 10–20. However, a narrow SMA angle alone is not enough to make a diagnosis, because patients with a low BMI, most notably children, have been known to have a narrow SMA angle with no symptoms of SMA syndrome.

Mueller–Weiss syndrome, also known as Mueller–Weiss disease, is a rare idiopathic degenerative disease of the adult navicular bone characterized by progressive collapse and fragmentation, leading to mid- and hindfoot pain and deformity. It is most commonly seen in females, ages 40–60. Characteristic imaging shows lateral navicular collapse. This disease had been historically considered to be a form of adult onset osteonecrosis, with blood flow cutoff to the navicular.
References
- ↑ Goh, T.; Goh, L. G.; Ang, C. H.; Wong, C. H. (January 2014). "Early diagnosis of necrotizing fasciitis". The British Journal of Surgery. 101 (1): e119–125. doi: 10.1002/bjs.9371 . ISSN 1365-2168. PMID 24338771. S2CID 10472804.
- ↑ Willis, R. B.; Rorabeck, C. H. (April 1990). "Treatment of compartment syndrome in children". The Orthopedic Clinics of North America. 21 (2): 401–412. doi:10.1016/S0030-5898(20)31554-6. ISSN 0030-5898. PMID 2183136.
- ↑ Patel, Ronak; Costanza, Michael (2017). "Chronic Mesenteric Ischemia". StatPearls. Treasure Island (FL): StatPearls Publishing. PMID 28613499.
- ↑ "Mueller-Weiss-syndrome | The Foot and Ankle Online Journal" . Retrieved 2022-06-09.
- ↑ 2024 ICD-10-CM Diagnosis Code Z76.5 - Malingerer [conscious simulation