
A picture archiving and communication system (PACS) is a medical imaging technology which provides economical storage and convenient access to images from multiple modalities. Electronic images and reports are transmitted digitally via PACS; this eliminates the need to manually file, retrieve, or transport film jackets, the folders used to store and protect X-ray film. The universal format for PACS image storage and transfer is DICOM. Non-image data, such as scanned documents, may be incorporated using consumer industry standard formats like PDF, once encapsulated in DICOM. A PACS consists of four major components: The imaging modalities such as X-ray plain film (PF), computed tomography (CT) and magnetic resonance imaging (MRI), a secured network for the transmission of patient information, workstations for interpreting and reviewing images, and archives for the storage and retrieval of images and reports. Combined with available and emerging web technology, PACS has the ability to deliver timely and efficient access to images, interpretations, and related data. PACS reduces the physical and time barriers associated with traditional film-based image retrieval, distribution, and display.
Digital Imaging and Communications in Medicine (DICOM) is the standard for the communication and management of medical imaging information and related data. DICOM is most commonly used for storing and transmitting medical images enabling the integration of medical imaging devices such as scanners, servers, workstations, printers, network hardware, and picture archiving and communication systems (PACS) from multiple manufacturers. It has been widely adopted by hospitals and is making inroads into smaller applications such as dentists' and doctors' offices.

The sievert is a unit in the International System of Units (SI) intended to represent the stochastic health risk of ionizing radiation, which is defined as the probability of causing radiation-induced cancer and genetic damage. The sievert is important in dosimetry and radiation protection. It is named after Rolf Maximilian Sievert, a Swedish medical physicist renowned for work on radiation dose measurement and research into the biological effects of radiation.
Medical physics deals with the application of the concepts and methods of physics to the prevention, diagnosis and treatment of human diseases with a specific goal of improving human health and well-being. Since 2008, medical physics has been included as a health profession according to International Standard Classification of Occupation of the International Labour Organization.

Medical imaging is the technique and process of imaging the interior of a body for clinical analysis and medical intervention, as well as visual representation of the function of some organs or tissues (physiology). Medical imaging seeks to reveal internal structures hidden by the skin and bones, as well as to diagnose and treat disease. Medical imaging also establishes a database of normal anatomy and physiology to make it possible to identify abnormalities. Although imaging of removed organs and tissues can be performed for medical reasons, such procedures are usually considered part of pathology instead of medical imaging.
Radiation dosimetry in the fields of health physics and radiation protection is the measurement, calculation and assessment of the ionizing radiation dose absorbed by an object, usually the human body. This applies both internally, due to ingested or inhaled radioactive substances, or externally due to irradiation by sources of radiation.

Nuclear medicine or nucleology is a medical specialty involving the application of radioactive substances in the diagnosis and treatment of disease. Nuclear imaging, in a sense, is "radiology done inside out" because it records radiation emitted from within the body rather than radiation that is transmitted through the body from external sources like X-ray generators. In addition, nuclear medicine scans differ from radiology, as the emphasis is not on imaging anatomy, but on the function. For such reason, it is called a physiological imaging modality. Single photon emission computed tomography (SPECT) and positron emission tomography (PET) scans are the two most common imaging modalities in nuclear medicine.

Fluoroscopy is an imaging technique that uses X-rays to obtain real-time moving images of the interior of an object. In its primary application of medical imaging, a fluoroscope allows a surgeon to see the internal structure and function of a patient, so that the pumping action of the heart or the motion of swallowing, for example, can be watched. This is useful for both diagnosis and therapy and occurs in general radiology, interventional radiology, and image-guided surgery.

A radiation burn is a damage to the skin or other biological tissue and organs as an effect of radiation. The radiation types of greatest concern are thermal radiation, radio frequency energy, ultraviolet light and ionizing radiation.
Moist desquamation is a description of the clinical pattern seen as a consequence of radiation exposure where the skin thins and then begins to weep because of loss of integrity of the epithelial barrier and decreased oncotic pressure. Moist desquamation is a rare complication for most forms of radiology, however it is far more common in fluoroscopy where threshold doses lie between 10-15 Gy and increasingly common above 15 Gy. It has been noted that fractionation of fluoroscopic procedures significantly reduces the likelihood of moist desquamation occurring. In animal studies done on pig skin, moist desquamation was found to occur with a 50% of the time after a single dose of 28 Gy, however a 2×18 Gy fractionation scheme was needed to produce the same 50% occurrence.
The American College of Radiology (ACR), founded in 1923, is a professional medical society representing nearly 40,000 diagnostic radiologists, radiation oncologists, interventional radiologists, nuclear medicine physicians and medical physicists.

Radiographers, also known as radiologic technologists, diagnostic radiographers and medical radiation technologists are healthcare professionals who specialise in the imaging of human anatomy for the diagnosis and treatment of pathology. Radiographers are infrequently, and almost always erroneously, known as x-ray technicians. In countries that use the title radiologic technologist they are often informally referred to as techs in the clinical environment; this phrase has emerged in popular culture such as television programmes. The term radiographer can also refer to a therapeutic radiographer, also known as a radiation therapist.
Image-guided radiation therapy is the process of frequent imaging, during a course of radiation treatment, used to direct the treatment, position the patient, and compare to the pre-therapy imaging from the treatment plan. Immediately prior to, or during, a treatment fraction, the patient is localized in the treatment room in the same position as planned from the reference imaging dataset. An example of IGRT would include comparison of a cone beam computed tomography (CBCT) dataset, acquired on the treatment machine, with the computed tomography (CT) dataset from planning. IGRT would also include matching planar kilovoltage (kV) radiographs or megavoltage (MV) images with digital reconstructed radiographs (DRRs) from the planning CT.
The collective effective dose, dose quantity S, is calculated as the sum of all individual effective doses over the time period or during the operation being considered due to ionizing radiation. It can be used to estimate the total health effects of a process or accidental release involving ionizing radiation to an exposed population. The total collective dose is the dose to the exposed human population between the time of release until its elimination from the environment, perhaps integrating to time equals infinity. However, doses are generally reported for specific populations and a stated time interval. The International Commission on Radiological Protection (ICRP) states: "To avoid aggregation of low individual doses over extended time periods and wide geographical regions the range in effective dose and the time period should be limited and specified.

Radiation dose reconstruction refers to the process of estimating radiation doses that were received by individuals or populations in the past as a result of particular exposure situations of concern. The basic principle of radiation dose reconstruction is to characterize the radiation environment to which individuals have been exposed using available information. In cases where radiation exposures can not be fully characterized based on available data, default values based on reasonable scientific assumptions can be used as substitutes. The extent to which the default values are used depends on the purpose of the reconstruction(s) being undertaken.
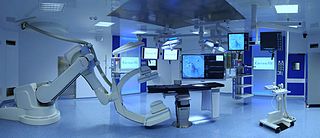
A hybrid operating room is a surgical theatre that is equipped with advanced medical imaging devices such as fixed C-Arms, X-ray computed tomography (CT) scanners or magnetic resonance imaging (MRI) scanners. These imaging devices enable minimally-invasive surgery. Minimally-invasive surgery is intended to be less traumatic for the patient and minimize incisions on the patient and perform surgery procedure through one or several small cuts.
The committed dose in radiological protection is a measure of the stochastic health risk due to an intake of radioactive material into the human body. Stochastic in this context is defined as the probability of cancer induction and genetic damage, due to low levels of radiation. The SI unit of measure is the sievert.
A Vendor Neutral Archive (VNA) is a medical imaging technology in which images and documents are stored (archived) in a standard format with a standard interface, such that they can be accessed in a vendor-neutral manner by other systems.

Medical image sharing is the electronic exchange of medical images between hospitals, physicians and patients. Rather than using traditional media, such as a CD or DVD, and either shipping it out or having patients carry it with them, technology now allows for the sharing of these images using the cloud. The primary format for images is DICOM. Typically, non-image data such as reports may be attached in standard formats like PDF during the sending process. Additionally, there are standards in the industry, such as IHE Cross Enterprise Document Sharing for Imaging (XDS-I), for managing the sharing of documents between healthcare enterprises. A typical architecture involved in setup is a locally installed server, which sits behind the firewall, allowing secure transmissions with outside facilities. In 2009, the Radiological Society of North America launched the "Image Share" project, with the goal of giving patients control of their imaging histories by allowing them to manage these records as they would online banking or shopping.

Integrating the Healthcare Enterprise (IHE) is a non-profit organization based in the US state of Illinois. It sponsors an initiative by the healthcare industry to improve the way computer systems share information. IHE was established in 1998 by a consortium of radiologists and information technology (IT) experts.










