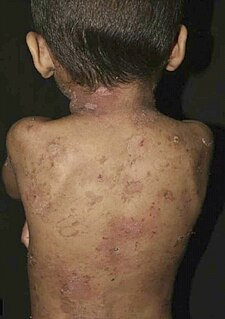
Epidermolytic ichthyosis (EI), also known as bullous epidermis ichthyosis (BEI), epidermolytic hyperkeratosis (EHK), bullous congenital ichthyosiform erythroderma (BCIE), bullous ichthyosiform erythroderma or bullous congenital ichthyosiform erythroderma Brocq, is a rare and severe form of ichthyosis this skin disease affects around 1 in 300,000 people.

A skin condition, also known as cutaneous condition, is any medical condition that affects the integumentary system—the organ system that encloses the body and includes skin, nails, and related muscle and glands. The major function of this system is as a barrier against the external environment.

A boil, also called a furuncle, is a deep folliculitis, infection of the hair follicle. It is most commonly caused by infection by the bacterium Staphylococcus aureus, resulting in a painful swollen area on the skin caused by an accumulation of pus and dead tissue. Boils which are expanded are basically pus-filled nodules. Individual boils clustered together are called carbuncles. Most human infections are caused by coagulase-positive S. aureus strains, notable for the bacteria's ability to produce coagulase, an enzyme that can clot blood. Almost any organ system can be infected by S. aureus.

A seborrheic keratosis is a non-cancerous (benign) skin tumour that originates from cells in the outer layer of the skin. Like liver spots, seborrheic keratoses are seen more often as people age.

Hyperkeratosis is thickening of the stratum corneum, often associated with the presence of an abnormal quantity of keratin, and also usually accompanied by an increase in the granular layer. As the corneum layer normally varies greatly in thickness in different sites, some experience is needed to assess minor degrees of hyperkeratosis.

Sweet syndrome (SS), or acute febrile neutrophilic dermatosis, is a skin disease characterized by the sudden onset of fever, an elevated white blood cell count, and tender, red, well-demarcated papules and plaques that show dense infiltrates by neutrophil granulocytes on histologic examination.

Degos disease, also known as Köhlmeier-Degos disease or malignant atrophic papulosis, is an extremely rare condition caused by blockage of arteries and veins. Individuals with this condition will develop papules. Those diagnosed with this disease may also develop complications due to impairment of internal organs. The exact underlying mechanism is still unknown, and an effective treatment is still being developed. There are fewer than 50 living patients presently known worldwide, and fewer than 200 reported in medical literature. However, many individuals may go undiagnosed due to rarity of the disease. Most individuals develop symptoms between the ages of 20–50; however, cases outside of this age range have been reported as well.

Granuloma annulare (GA) is a common, sometimes chronic skin condition which presents as reddish bumps on the skin arranged in a circle or ring. It can initially occur at any age, though two-thirds of patients are under 30 years old, and it is seen most often in children and young adults. Females are two times as likely to have it than males.

Zunich–Kaye syndrome, also known as Zunich neuroectodermal syndrome, is a rare congenital ichthyosis first described in 1983. It is also referred to as CHIME syndrome, after its main symptoms. It is a congenital syndrome with only a few cases studied and published.
Josef Kyrle was an Austrian pathologist and dermatologist who was a native of Schärding.
Paraneoplastic pemphigus (PNP) is an autoimmune disorder stemming from an underlying tumor. It is hypothesized that antigens associated with the tumor trigger an immune response resulting in blistering of the skin and mucous membranes.
Acquired perforating dermatosis is clinically and histopathologically similar to perforating folliculitis, also associated with chronic kidney failure, with or without hemodialysis or peritoneal dialysis, and/or diabetes mellitus, but not identical to Kyrle disease.
Reactive perforating collagenosis is a rare, familial, nonpuritic skin disorder characterized by papules that grow in a diameter of 4 to 6mm and develop a central area of umbilication to which keratinous material is lodged. The cause of reactive perforating collagenosis is unknown.

Dermatosis neglecta is a skin condition in which accumulation of sebum, keratin, sweat, dirt and debris leads to a localized patch of skin discoloration or a wart-like plaque. It is caused by inadequate hygiene of a certain body part, usually due to some form of disability or a condition that is associated with pain or increased sensitivity to touch (hyperesthesia) or immobility.
An arsenical keratosis is a growth of keratin on the skin caused by arsenic, which occurs naturally in the earth's crust and is widely distributed in the environment, Arsenical compounds are used in industrial, agricultural, and medicinal substances. Arsenic is also found to be an environmental contaminant in drinking water and an occupational hazard for miners and glass workers. Arsenic may also causes other conditions including: Bowen's disease, cardiovascular diseases, developmental abnormalities, neurologic and neurobehavioral disorders, diabetes, hearing loss, hematologic disorders, and various types of cancer. Arsenical keratoses may persist indefinitely, and some may develop into invasive squamous cell carcinoma. Metastatic arsenic squamous cell carcinoma and arsenic-induced malignancies in internal organs such as the bladder, kidney, skin, liver, and colon, may result in death.

Warty dyskeratoma, also known as an Isolated dyskeratosis follicularis, is a benign epidermal proliferation with distinctive histologic findings that may mimic invasive squamous cell carcinoma and commonly manifests as an umbilicated lesion with a keratotic plug, WD have some histopathologic similarities to viral warts but it's not caused by HPV and the majority of these lesions display overall histopathologic features consistent with a follicular adnexal neoplasm. Usually limited to the head, neck, scalp or face and vulva. Lesions are generally solitary and sporadic and may be associated with a follicular unit. Oral involvement, particularly the hard palate, and genital involvement have been reported. it can also be thought of as one of the manifestations of focal acantholytic dyskeratosis, an epidermal reaction pattern that can be seen in several disorders, including Darier's disease and Grover's disease. But the main Difference between Darier disease and Warty dyskeratoma, is that Darier disease inherited dermatosis consisting of multiple keratotic papules on the face, trunk, and extremities, while WD occurs as an isolated, noninherited, single keratotic nodule mainly confined to the head and neck as mentioned earlier.

Porokeratosis is a specific disorder of keratinization that is characterized histologically by the presence of a cornoid lamella, a thin column of closely stacked, parakeratotic cells extending through the stratum corneum with a thin or absent granular layer.

Inflammatory Linear Verrucous Epidermal Nevus is a rare disease of the skin that presents as multiple, discrete, red papules that tend to coalesce into linear plaques that follow the Lines of Blaschko. The plaques can be slightly warty (psoriaform) or scaly (eczema-like). ILVEN is caused by somatic mutations that result in genetic mosaicism. There is no cure, but different medical treatments can alleviate the symptoms.

Majocchi's granuloma is a skin condition characterized by deep, pustular plaques, and is a form of tinea corporis. It is a localized form of fungal folliculitis. Lesions often have a pink and scaly central component with pustules or folliculocentric papules at the periphery. The name comes from Professor Domenico Majocchi, who discovered the disorder in 1883. Majocchi was a professor of dermatology at the University of Parma and later the University of Bologna. The most common dermatophyte is called Trichophyton rubrum.













