Related Research Articles

A thrombus,, colloquially called a blood clot, is the final product of the blood coagulation step in hemostasis. There are two components to a thrombus: aggregated platelets and red blood cells that form a plug, and a mesh of cross-linked fibrin protein. The substance making up a thrombus is sometimes called cruor. A thrombus is a healthy response to injury intended to stop and prevent further bleeding, but can be harmful in thrombosis, when a clot obstructs blood flow through healthy blood vessels in the circulatory system.

Arteriosclerosis is the thickening, hardening, and loss of elasticity of the walls of arteries. This process gradually restricts the blood flow to one's organs and tissues and can lead to severe health risks brought on by atherosclerosis, which is a specific form of arteriosclerosis caused by the buildup of fatty plaques, cholesterol, and some other substances in and on the artery walls. It can be brought on by smoking, a bad diet, or many genetic factors.
Vascular dementia (VaD) is dementia caused by problems in the supply of blood to the brain, typically a series of minor strokes, leading to worsening cognitive abilities, the decline occurring step by step. The term refers to a syndrome consisting of a complex interaction of cerebrovascular disease and risk factors that lead to changes in brain structures due to strokes and lesions, resulting in changes in cognition. The temporal relationship between a stroke and cognitive deficits is needed to make the diagnosis.

Binswanger's disease, also known as subcortical leukoencephalopathy and subcortical arteriosclerotic encephalopathy (SAE), is a form of small vessel vascular dementia caused by damage to the white brain matter. White matter atrophy can be caused by many circumstances including chronic hypertension as well as old age. This disease is characterized by loss of memory and intellectual function and by changes in mood. These changes encompass what are known as executive functions of the brain. It usually presents between 54 and 66 years of age, and the first symptoms are usually mental deterioration or stroke.

Cerebrovascular disease includes a variety of medical conditions that affect the blood vessels of the brain and the cerebral circulation. Arteries supplying oxygen and nutrients to the brain are often damaged or deformed in these disorders. The most common presentation of cerebrovascular disease is an ischemic stroke or mini-stroke and sometimes a hemorrhagic stroke. Hypertension is the most important contributing risk factor for stroke and cerebrovascular diseases as it can change the structure of blood vessels and result in atherosclerosis. Atherosclerosis narrows blood vessels in the brain, resulting in decreased cerebral perfusion. Other risk factors that contribute to stroke include smoking and diabetes. Narrowed cerebral arteries can lead to ischemic stroke, but continually elevated blood pressure can also cause tearing of vessels, leading to a hemorrhagic stroke.

An arteriole is a small-diameter blood vessel in the microcirculation that extends and branches out from an artery and leads to capillaries.

Ischemia or ischaemia is a restriction in blood supply to any tissues, muscle group, or organ of the body, causing a shortage of oxygen that is needed for cellular metabolism. Ischemia is generally caused by problems with blood vessels, with resultant damage to or dysfunction of tissue i.e. hypoxia and microvascular dysfunction. It also means local hypoxia in a given part of a body sometimes resulting from constriction. Ischemia comprises not only insufficiency of oxygen, but also reduced availability of nutrients and inadequate removal of metabolic wastes. Ischemia can be partial or total blockage. The inadequate delivery of oxygenated blood to the organs must be resolved either by treating the cause of the inadequate delivery or reducing the oxygen demand of the system that needs it. For example, patients with myocardial ischemia have a decreased blood flow to the heart and are prescribed with medications that reduce chronotrophy and ionotrophy to meet the new level of blood delivery supplied by the stenosed so that it is adequate.
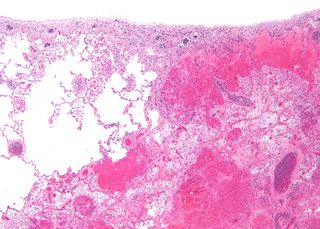
Infarction is tissue death (necrosis) due to inadequate blood supply to the affected area. It may be caused by artery blockages, rupture, mechanical compression, or vasoconstriction. The resulting lesion is referred to as an infarct (from the Latin infarctus, "stuffed into").

Hypertensive kidney disease is a medical condition referring to damage to the kidney due to chronic high blood pressure. It manifests as hypertensive nephrosclerosis. It should be distinguished from renovascular hypertension, which is a form of secondary hypertension, and thus has opposite direction of causation.

A perivascular space, also known as a Virchow–Robin space, is a fluid-filled space surrounding certain blood vessels in several organs, including the brain, potentially having an immunological function, but more broadly a dispersive role for neural and blood-derived messengers. The brain pia mater is reflected from the surface of the brain onto the surface of blood vessels in the subarachnoid space. In the brain, perivascular cuffs are regions of leukocyte aggregation in the perivascular spaces, usually found in patients with viral encephalitis.
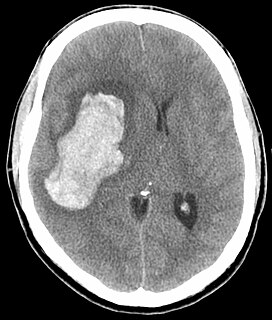
A hypertensive emergency is very high blood pressure with potentially life-threatening symptoms and signs of acute damage to one or more organ systems. It is different from a hypertensive urgency by this additional evidence for impending irreversible hypertension-mediated organ damage (HMOD). Blood pressure is often above 200/120 mmHg, however there are no universally accepted cutoff values. Signs of organ damage will be discussed below.

Intraparenchymal hemorrhage (IPH) is one form of intracerebral bleeding in which there is bleeding within brain parenchyma. The other form is intraventricular hemorrhage (IVH).

Arteriolosclerosis is a form of cardiovascular disease involving hardening and loss of elasticity of arterioles or small arteries and is most often associated with hypertension and diabetes mellitus. Types include hyaline arteriolosclerosis and hyperplastic arteriolosclerosis, both involved with vessel wall thickening and luminal narrowing that may cause downstream ischemic injury. The following two terms whilst similar, are distinct in both spelling and meaning and may easily be confused with arteriolosclerosis.

A cerebral infarction is the pathologic process that results in an area of necrotic tissue in the brain. It is caused by disrupted blood supply (ischemia) and restricted oxygen supply (hypoxia), most commonly due to thromboembolism, and manifests clinically as ischemic stroke. In response to ischemia, the brain degenerates by the process of liquefactive necrosis.

A watershed stroke is defined as a brain ischemia that is localized to the vulnerable border zones between the tissues supplied by the anterior, posterior and middle cerebral arteries. The actual blood stream blockage/restriction site can be located far away from the infarcts. Watershed locations are those border-zone regions in the brain supplied by the major cerebral arteries where blood supply is decreased. Watershed strokes are a concern because they comprise approximately 10% of all ischemic stroke cases. The watershed zones themselves are particularly susceptible to infarction from global ischemia as the distal nature of the vasculature predisposes these areas to be most sensitive to profound hypoperfusion.

Lacunar stroke or lacunar cerebral infarct (LACI) is the most common type of ischemic stroke, resulting from the occlusion of small penetrating arteries that provide blood to the brain's deep structures. Patients who present with symptoms of a lacunar stroke, but who have not yet had diagnostic imaging performed, may be described as suffering from lacunar stroke syndrome (LACS).

Complications of hypertension are clinical outcomes that result from persistent elevation of blood pressure. Hypertension is a risk factor for all clinical manifestations of atherosclerosis since it is a risk factor for atherosclerosis itself. It is an independent predisposing factor for heart failure, coronary artery disease, stroke, kidney disease, and peripheral arterial disease. It is the most important risk factor for cardiovascular morbidity and mortality, in industrialized countries.
A silent stroke is a stroke that does not have any outward symptoms associated with stroke, and the patient is typically unaware they have suffered a stroke. Despite not causing identifiable symptoms, a silent stroke still causes damage to the brain and places the patient at increased risk for both transient ischemic attack and major stroke in the future. In a broad study in 1998, more than 11 million people were estimated to have experienced a stroke in the United States. Approximately 770,000 of these strokes were symptomatic and 11 million were first-ever silent MRI infarcts or hemorrhages. Silent strokes typically cause lesions which are detected via the use of neuroimaging such as MRI. The risk of silent stroke increases with age but may also affect younger adults. Women appear to be at increased risk for silent stroke, with hypertension and current cigarette smoking being amongst the predisposing factors.
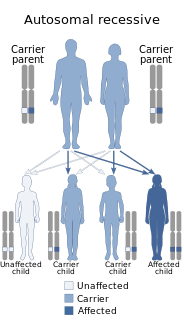
Cerebral autosomal recessive arteriopathy with subcortical infarcts and leukoencephalopathy (CARASIL), is disease of the arteries in the brain, which causes tissue loss in the subcortical region of the brain and the destruction of myelin in the CNS. CARASIL is characterized by symptoms such as gait disturbances, hair loss, low back pain, dementia, and stroke. CARASIL is a rare disease, having only been diagnosed in about 50 patients, of which ten have been genetically confirmed. Most cases have been reported in Japan, but Chinese and caucasian individuals have also been diagnosed with the disease. CARASIL is inherited in an autosomal recessive pattern. There is currently no cure for CARASIL. Other names for CARASIL include familial young-adult-onset arteriosclerotic leukoencephalopathy with alopecia and lumbago without arterial hypertension, Nemoto disease and Maeda syndrome.

Hypertension is a condition characterized by an elevated blood pressure in which the long term consequences include cardiovascular disease, kidney disease, adrenal gland tumors, vision impairment, memory loss, metabolic syndrome, stroke and dementia. It affects nearly 1 in 2 Americans and remains as a contributing cause of death in the United States. There are many genetic and environmental factors involved with the development of hypertension including genetics, diet, and stress.
References
- 1 2 3 Rosenblum, William I. "Fibrinoid Necrosis of Small Brain Arteries and Arterioles and Miliary Aneurysms as Causes of Hypertensive Hemorrhage: A Critical Reappraisal." Acta Neuropathologica 116, no. 4 (October 2008): 361–69. https://doi.org/10.1007/s00401-008-0416-9.
- 1 2 Lammie, G Alistair. “Pathology of Small Vessel Stroke.” British Medical Bulletin 56, no. 2 (2000): 296–306.
- ↑ Brenner D, Labreuche J, Pico F, et al. "The renin-angiotensin-aldosterone system in cerebral small vessel disease". J Neurol. May 2, 2000
- ↑ Coca, Antonio, ed. Hypertension and Brain Damage. Updates in Hypertension and Cardiovascular Protection Ser. Cham: Springer, 2016.
- ↑ Droste, D. W., M. A. Ritter, R. Dittrich, S. Heidenreich, T. Wichter, M. Freund, and E. B. Ringelstein. "Arterial Hypertension and Ischaemic Stroke." Acta Neurologica Scandinavica 107, no. 4 (April 2003): 241–51. https://doi.org/10.1034/j.1600-0404.2003.00098.x.
- 1 2 3 4 Aiyagari, Venkatesh, and Philip B. Gorelick, eds. Hypertension and Stroke: Pathophysiology and Management. 2nd ed. Clinical Hypertension and Vascular Diseases. Humana Press, 2016.
- 1 2 Lastilla, Marcello. “Lacunar Infarct.” Clinical & Experimental Hypertension 28, no. 3/4 (April 2006): 205–15. https://doi.org/10.1080/10641960600549082.
- ↑ Caplan, Louis R. “Lacunar Infarction and Small Vessel Disease: Pathology and Pathophysiology.” Journal of Stroke 17, no. 1 (January 2015): 2–6. https://doi.org/10.5853/jos.2015.17.1.2.
- ↑ Thal, Dietmar Rudolf, Estifanos Ghebremedhin, Mario Orantes, and Otmar D. Wiestler. “Vascular Pathology in Alzheimer Disease: Correlation of Cerebral Amyloid Angiopathy and Arteriosclerosis/Lipohyalinosis with Cognitive Decline.” Journal of Neuropathology & Experimental Neurology 62, no. 12 (December 1, 2003): 1287–1301. https://doi.org/10.1093/jnen/62.12.1287.
- 1 2 Baker, John G., Amy J. Williams, Catalina C. Ionita, Peterkin Lee-Kwen, Marilou Ching, and Robert S. Miletich. “Cerebral Small Vessel Disease: Cognition, Mood, Daily Functioning, and Imaging Findings from a Small Pilot Sample.” Dementia and Geriatric Cognitive Disorders EXTRA 2, no. 1 (April 18, 2012): 169–79. https://doi.org/10.1159/000333482.
- ↑ Østergaard, Leif, Thorbjørn S Engedal, Fiona Moreton, Mikkel B Hansen, Joanna M Wardlaw, Turgay Dalkara, Hugh S Markus, and Keith W Muir. "Cerebral Small Vessel Disease: Capillary Pathways to Stroke and Cognitive Decline." Journal of Cerebral Blood Flow & Metabolism 36, no. 2 (February 2016): 302–25. https://doi.org/10.1177/0271678X15606723.
- ↑ Kasper, Dennis, Anthony Fauci, Stephen Hauser, Dan Longo, J. Larry Jameson, and Joseph Loscalzo, eds. "Cerebrovascular Diseases." In Harrison's Principles of Internal Medicine, 19th ed. McGraw-Hill Medical.