
Contact dermatitis is a type of acute or chronic inflammation of the skin caused by exposure to chemical or physical agents. Symptoms of contact dermatitis can include itchy or dry skin, a red rash, bumps, blisters, or swelling. These rashes are not contagious or life-threatening, but can be very uncomfortable.

Latex allergy is a medical term encompassing a range of allergic reactions to the proteins present in natural rubber latex. It generally develops after repeated exposure to products containing natural rubber latex. When latex-containing medical devices or supplies come in contact with mucous membranes, the membranes may absorb latex proteins. In some susceptible people, the immune system produces antibodies that react immunologically with these antigenic proteins. Many items contain or are made from natural rubber, including shoe soles, pen grips, hot water bottles, elastic bands, rubber gloves, condoms, baby-bottle nipples, and balloons; consequently, there are many possible routes of exposure that may trigger a reaction. People with latex allergies may also have or develop allergic reactions to some fruits, such as bananas.

Hives, also known as urticaria, is a kind of skin rash with red, raised, itchy bumps. Hives may burn or sting. The patches of rash may appear on different body parts, with variable duration from minutes to days, and does not leave any long-lasting skin change. Fewer than 5% of cases last for more than six weeks. The condition frequently recurs.

Cold urticaria is a disorder in which large red welts called hives (urticaria) form on the skin after exposure to a cold stimulus. The hives are usually itchy and often the hands and feet will become itchy and swollen as well. Hives vary in size from about 7 mm in diameter to as big as about 27 mm or larger.
Aquagenic pruritus is a skin condition characterized by the development of severe, intense, prickling-like epidermal itching without observable skin lesions and evoked by contact with water.

Atopic dermatitis (AD), also known as atopic eczema, is a long-term type of inflammation of the skin (dermatitis). It results in itchy, red, swollen, and cracked skin. Clear fluid may come from the affected areas, which can thicken over time. AD may also simply be called eczema, a term that generally refers to a larger group of skin conditions.

Physical urticaria is a distinct subgroup of urticaria (hives) that are induced by an exogenous physical stimulus rather than occurring spontaneously. There are seven subcategories that are recognized as independent diseases. Physical urticaria is known to be painful, itchy and physically unappealing; it can recur for months to years.

Pruritic urticarial papules and plaques of pregnancy (PUPPP), known in United Kingdom as polymorphic eruption of pregnancy (PEP), is a chronic hives-like rash that strikes some women during pregnancy. Some skin changes are known to occur in people who are pregnant while other skin conditions, or dermatoses, that people have prior to getting pregnant will become altered or symptoms will increase. Pruritic urticarial papules and plaques of pregnancy (PUPPP) is one of many skin conditions that is specific to pregnancy and occurs in about 1 in every 160 (0.625%) of pregnancies.
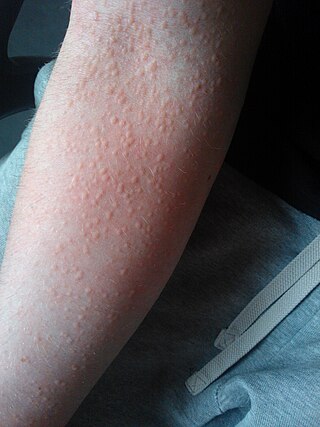
Cholinergic urticaria is a type of hives (urticaria) that is triggered by an increase in body temperature, such as during exercise, sweating, or exposure to heat. It is also sometimes called exercise-induced urticaria or heat hives. The condition is caused by an overreaction of the immune system to the release of histamine and other chemicals in response to the increase in body temperature. This results in the characteristic red, itchy, and sometimes raised bumps or welts on the skin that are associated with hives.

Solar urticaria (SU) is a rare condition in which exposure to ultraviolet or UV radiation, or sometimes even visible light, induces a case of urticaria or hives that can appear in both covered and uncovered areas of the skin. It is classified as a type of physical urticaria. The classification of disease types is somewhat controversial. One classification system distinguished various types of SU based on the wavelength of the radiation that causes the breakout; another classification system is based on the type of allergen that initiates a breakout.

Notalgia paresthetica or Notalgia paraesthetica (NP) (also known as "Hereditary localized pruritus", "Posterior pigmented pruritic patch", and "subscapular pruritus") is a chronic sensory neuropathy. Notalgia paresthetica is a common localized itch, affecting mainly the area between the shoulder blades (especially the T2–T6 dermatomes) but occasionally with a more widespread distribution, involving the shoulders, back, and upper chest. The characteristic symptom is pruritus (itch or sensation that makes a person want to scratch) on the back, usually on the left hand side below the shoulder blade (mid to upper back). It is occasionally accompanied by pain, paresthesia (pins and needles), or hyperesthesia (unusual or pathologically increased sensitivity of the skin to sensory stimuli, such as pain, heat, cold, or touch), which results in a well circumscribed hyperpigmentation of a skin patch in the affected area.
Autoimmune progesterone dermatitis(APD) occurs during the luteal phase of a woman's menstrual cycle and is an uncommon cyclic premenstrual reaction to progesterone. It can present itself in several ways, including eczema, erythema multiforme, urticaria, angioedema, and progesterone-induced anaphylaxis. The first case of autoimmune progesterone dermatitis was identified in 1964. Reproductive function may be impacted by APD.
Adrenergic urticaria is a skin condition characterized by an eruption consisting of small (1-5mm) red macules and papules with a pale halo, appearing within 10 to 15 min after emotional upset. There have been 10 cases described in medical literature, and involve a trigger followed by a rise in catecholamine and IgE. Treatment involves propranolol and trigger avoidance.
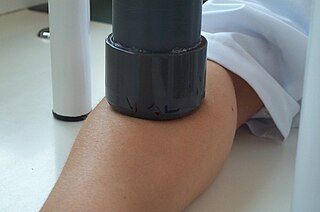
Pressure urticaria or delayed pressure urticaria is a physical urticaria caused by pressure applied to the skin, and is characterized by the development of swelling and pain that usually occurs 3 to 12 hours after local pressure has been applied.
Idiopathic pure sudomotor failure (IPSF) is the most common cause of a rare disorder known as acquired idiopathic generalized anhidrosis (AIGA), a clinical syndrome characterized by generalized decrease or absence of sweating without other autonomic and somatic nervous dysfunctions and without persistent organic cutaneous lesions.

Chronic spontaneous urticaria(CSU) also known as Chronic idiopathic urticaria(CIU) is defined by the presence of wheals, angioedema, or both for more than six weeks. Chronic spontaneous urticaria can be characterized by angioedema, excruciatingly itchy recurrent hives, or both. Chronic urticaria patients were found to have a higher prevalence of various autoimmune diseases. Many patients with chronic spontaneous urticaria report that certain triggers, such as stress, infections, specific foods, or nonsteroidal anti-inflammatory drug use, aggravate their condition.
A sweat allergy is the exacerbation of atopic dermatitis associated with an elevated body temperature and resulting increases in the production of sweat. It appears as small reddish welts that become visible in response to increased temperature and resulting production of sweat. It can affect all ages. Sweating can trigger intense itching or cholinergic urticaria. The protein MGL_1304 secreted by mycobiota (fungi) present on the skin such as Malassezia globosa acts as a histamine or antigen. People can be desensitized using their own samples of sweat that have been purified that contains small amounts of the allergen. The allergy is not due to the sweat itself but instead to an allergy-producing protein secreted by bacteria found on the skin.
Exercise-induced anaphylaxis is a rare condition in which anaphylaxis, a serious or life-threatening allergic response, is brought on by physical activity. Approximately 5–15% of all reported cases of anaphylaxis are thought to be exercise-induced.
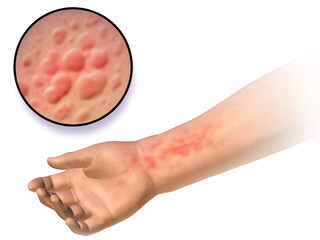
Autoimmune urticaria, also known as chronic autoimmune urticaria, is a type of chronic urticaria characterized by the presence of autoantibodies in the patient's immune system that target the body's own mast cells, leading to episodes of hives (urticaria). This immunologically distinct type of urticaria is considered autoimmune because the immune system, which normally protects the body from foreign organisms, mistakenly attacks the body's own cells, causing inflammation and other symptoms.











