Related Research Articles

Orthopedic surgery or orthopedics is the branch of surgery concerned with conditions involving the musculoskeletal system. Orthopedic surgeons use both surgical and nonsurgical means to treat musculoskeletal trauma, spine diseases, sports injuries, degenerative diseases, infections, tumors, and congenital disorders.

Hip replacement is a surgical procedure in which the hip joint is replaced by a prosthetic implant, that is, a hip prosthesis. Hip replacement surgery can be performed as a total replacement or a hemi/semi(half) replacement. Such joint replacement orthopaedic surgery is generally conducted to relieve arthritis pain or in some hip fractures. A total hip replacement consists of replacing both the acetabulum and the femoral head while hemiarthroplasty generally only replaces the femoral head. Hip replacement is one of the most common orthopaedic operations, though patient satisfaction varies widely. Approximately 58% of total hip replacements are estimated to last 25 years. The average cost of a total hip replacement in 2012 was $40,364 in the United States, and about $7,700 to $12,000 in most European countries.
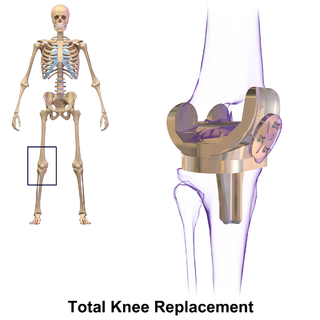
Knee replacement, also known as knee arthroplasty, is a surgical procedure to replace the weight-bearing surfaces of the knee joint to relieve pain and disability, most commonly offered when joint pain is not diminished by conservative sources. It may also be performed for other knee diseases, such as rheumatoid arthritis. In patients with severe deformity from advanced rheumatoid arthritis, trauma, or long-standing osteoarthritis, the surgery may be more complicated and carry higher risk. Osteoporosis does not typically cause knee pain, deformity, or inflammation, and is not a reason to perform knee replacement.

Joint replacement is a procedure of orthopedic surgery known also as arthroplasty, in which an arthritic or dysfunctional joint surface is replaced with an orthopedic prosthesis. Joint replacement is considered as a treatment when severe joint pain or dysfunction is not alleviated by less-invasive therapies. Joint replacement surgery is often indicated from various joint diseases, including osteoarthritis and rheumatoid arthritis.
A meniscus transplant or meniscal transplant is a transplant of the meniscus of the knee, which separates the thigh bone (femur) from the lower leg bone (tibia). The worn or damaged meniscus is removed and is replaced with a new one from a donor. The meniscus to be transplanted is taken from a cadaver, and, as such, is known as an allograft. Meniscal transplantation is technically difficult, as it must be sized accurately for each person, positioned properly and secured to the tibial plateau. Its success also depends on donor compatibility, stability of the transplant, and long-term health of the underlying articular cartilage.
Articular cartilage, most notably that which is found in the knee joint, is generally characterized by very low friction, high wear resistance, and poor regenerative qualities. It is responsible for much of the compressive resistance and load bearing qualities of the knee joint and, without it, walking is painful to impossible. Osteoarthritis is a common condition of cartilage failure that can lead to limited range of motion, bone damage and invariably, pain. Due to a combination of acute stress and chronic fatigue, osteoarthritis directly manifests itself in a wearing away of the articular surface and, in extreme cases, bone can be exposed in the joint. Some additional examples of cartilage failure mechanisms include cellular matrix linkage rupture, chondrocyte protein synthesis inhibition, and chondrocyte apoptosis. There are several different repair options available for cartilage damage or failure.
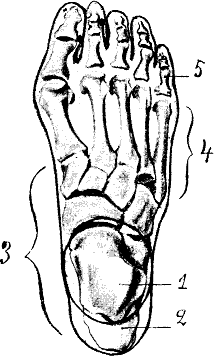
Hallux rigidus or stiff big toe is degenerative arthritis and stiffness due to bone spurs that affects the metatarsophalangeal joints (MTP) at the base of the hallux.

Hip resurfacing has been developed as a surgical alternative to total hip replacement (THR). The procedure consists of placing a cap, which is hollow and shaped like a mushroom, over the head of the femur while a matching metal cup is placed in the acetabulum, replacing the articulating surfaces of the person's hip joint and removing very little bone compared to a THR. When the person moves the hip, the movement of the joint induces synovial fluid to flow between the hard metal bearing surfaces lubricating them when the components are placed in the correct position. The surgeon's level of experience with hip resurfacing is most important; therefore, the selection of the right surgeon is crucial for a successful outcome. Health-related quality of life measures are markedly improved and the person's satisfaction is favorable after hip resurfacing arthroplasty.

Shoulder replacement is a surgical procedure in which all or part of the glenohumeral joint is replaced by a prosthetic implant. Such joint replacement surgery generally is conducted to relieve arthritis pain or fix severe physical joint damage.
Artificial disc replacement (ADR), or total disc replacement (TDR), is a type of arthroplasty. It is a surgical procedure in which degenerated intervertebral discs in the spinal column are replaced with artificial disc implants in the lumbar (lower) or cervical (upper) spine. The procedure is used to treat chronic, severe low back pain and cervical pain resulting from degenerative disc disease. Disc replacement is also an alternative intervention for symptomatic disc herniation with associated arm and hand, or leg symptoms.

A tear of a meniscus is a rupturing of one or more of the fibrocartilage strips in the knee called menisci. When doctors and patients refer to "torn cartilage" in the knee, they actually may be referring to an injury to a meniscus at the top of one of the tibiae. Menisci can be torn during innocuous activities such as walking or squatting. They can also be torn by traumatic force encountered in sports or other forms of physical exertion. The traumatic action is most often a twisting movement at the knee while the leg is bent. In older adults, the meniscus can be damaged following prolonged 'wear and tear'. Especially acute injuries can lead to displaced tears which can cause mechanical symptoms such as clicking, catching, or locking during motion of the joint. The joint will be in pain when in use, but when there is no load, the pain goes away.

Unicompartmental knee arthroplasty (UKA) is a surgical procedure used to relieve arthritis in one of the knee compartments in which the damaged parts of the knee are replaced. UKA surgery may reduce post-operative pain and have a shorter recovery period than a total knee replacement procedure, particularly in people over 75 years of age. Moreover, UKAs may require a smaller incision, less tissue damage, and faster recovery times.
Articular cartilage repair treatment involves the repair of the surface of the articular joint's hyaline cartilage, though these solutions do not perfectly restore the articular cartilage. These treatments have been shown to have positive results for patients who have articular cartilage damage. They can provide some measure of pain relief, while slowing down the accumulation of damage, or delaying the need for joint replacement surgery.
"Professor" Derek McMinn is a British orthopaedic surgeon and inventor who practised in Birmingham, United Kingdom at the BMI Edgbaston Hospital until his suspension in 2020. McMinn is currently under police investigation for allegedly keeping the body parts of thousands of patients over a 25-year period.
Metallosis is the medical condition involving deposition and build-up of metal debris in the soft tissues of the body.
Limb-sparing techniques, also known as limb-saving or limb-salvage techniques, are performed in order to preserve the look and function of limbs. Limb-sparing techniques are used to preserve limbs affected by trauma, arthritis, cancers such as high-grade bone sarcomas, and vascular conditions such as diabetic foot ulcers. As the techniques for chemotherapy, radiation, and diagnostic modalities improve, there has been a trend toward limb-sparing procedures to avoid amputation, which has been associated with a lower 5-year survival rate and cost-effectiveness compared to limb salvage in the long-run. There are many different types of limb-sparing techniques, including arthrodesis, arthroplasty, endoprosthetic reconstruction, various types of implants, rotationplasty, osseointegration limb replacement, fasciotomy, and revascularization.
The following outline is provided as an overview of and topical guide to trauma and orthopaedics:
Martinus Richter is a German orthopaedic surgeon, and Associate Professor at the Hannover Medical School and Head of the Department for Foot and Ankle Surgery Nuremberg and Rummelsberg at the Hospital Rummelsberg and Sana-Hospital Nuremberg.

Reverse shoulder replacement is a type of shoulder replacement in which the normal ball and socket relationship of glenohumeral joint is reversed, creating a more stable joint with a fixed fulcrum. This form of shoulder replacement is utilized in situations in which conventional shoulder replacement surgery would lead to poor outcomes and high failure rates.
Ankle fusion, or ankle arthrodesis, is surgery of the ankle to fuse the bones to treat arthritis and for other purposes. There are different types of ankle fusion surgery. The surgery involves the use of screws, plates, medical nails, and other hardware to achieve bone union. Ankle fusion is considered to be the gold standard for treatment of end-stage ankle arthritis. It trades joint mobility for relief from pain. Complications may include infection, non-union, and, rarely, amputation.
References
- ↑ Saltzman, C.L.; Mann, R.A.; Ahrens, J.E.; Amendola, A.; Anderson, R.B.; Berlet, G.C.; Brodky, J.W.; Chou, L.B.; Clanton, T.O.; Deland, J.T.; Deorio, J.K.; Horton, G.A.; Lee, T.H.; Mann, J.A.; Nunley, J.A.; Thordarson, D.B.; Walling, A.K.; Wapner, K.L.; Coughlin, M.J. (2009). "Prospective Controlled Trial of STAR Total Ankle Replacement Versus Ankle Fusion: Initial Results". Foot & Ankle International . 30 (7): 579–596. doi:10.3113/FAI.2009.0579. PMID 19589303. S2CID 787907.
- ↑ Kitaoka, Harold B.; Patzer, Gary L. (1996). "Clinical results of the Mayo total ankle arthroplasty". Journal of Bone and Joint Surgery . 78A (11): 1658–64. doi:10.2106/00004623-199611000-00004. PMID 8934479. S2CID 32382311. Archived from the original on 2010-06-04. Retrieved 2011-01-26.
- ↑ Lachiewicz, PF (1994). "Total ankle arthroplasty. Indications, techniques, and results". Orthopaedic Review . 23 (4): 315–20. PMID 8008441.
- 1 2 Giannini, Sandro; Romagnoli, Matteo; O’connor, John J.; Malerba, Francesco; Leardini, Alberto (2010). "Total Ankle Replacement Compatible with Ligament Function Produces Mobility, Good Clinical Scores, and Low Complication Rates: An Early Clinical Assessment". Clinical Orthopaedics and Related Research . 468 (10): 2746–53. doi:10.1007/s11999-010-1432-3. PMC 3049631 . PMID 20559763.
- ↑ Saltzman, CL; McIff, TE; Buckwalter, JA; Brown, TD (2000). "Total ankle replacement revisited". Journal of Orthopaedic & Sports Physical Therapy . 30 (2): 56–67. doi:10.2519/jospt.2000.30.2.56. PMID 10693083.
- ↑ Goodfellow, John; O'Connor, John (1978). "The mechanics of the knee and prosthesis design". Journal of Bone and Joint Surgery . 60B (3): 358–69. doi: 10.1302/0301-620X.60B3.581081 . PMID 581081.
- 1 2 Haddad, S.L.; Coetzee, J.C.; Estok, R.; Fahrbach, K.; Banel, D.; Nalysnyk, L. (2007). "Intermediate and Long-Term Outcomes of Total Ankle Arthroplasty and Ankle Arthrodesis. A Systematic Review of the Literature". Journal of Bone and Joint Surgery . 89A (9): 1899–905. doi:10.2106/JBJS.F.01149. PMID 17768184. S2CID 2665720.
- ↑ Stengel, Dirk; Bauwens, Kai; Ekkernkamp, Axel; Cramer, Jörg (2005). "Efficacy of total ankle replacement with meniscal-bearing devices: a systematic review and meta-analysis". Archives of Orthopaedic and Trauma Surgery . 125 (2): 109–19. doi:10.1007/s00402-004-0765-3. PMID 15690167. S2CID 13299426.
- ↑ Gougoulias, Nikolaos; Khanna, Anil; Maffulli, Nicola (2009). "How Successful are Current Ankle Replacements? All[sic] though most total ankle replacement are successful by reducing pain and improving mobility there is a very high possibility that the pain may be ten times worse. There have been several cases where the doctors have recommended amputation to resolve the issue of pain that was not there prior to the total ankle replacement. : A Systematic Review of the Literature". Clinical Orthopaedics and Related Research . 468 (1): 199–208. doi:10.1007/s11999-009-0987-3. PMC 2795846 . PMID 19618248.
- ↑ Mann, J.A.; Mann, R.A.; Horton, E. (2011). "STAR ankle: long-term results". Foot & Ankle International . 32 (5): S473–484. doi:10.3113/FAI.2011.0473. PMID 21733455. S2CID 12652720.
- ↑ Zaidi, Razi; Macgregor, Alexander J.; Goldberg, Andy (2016-05-01). "Quality measures for total ankle replacement, 30-day readmission and reoperation rates within 1 year of surgery: a data linkage study using the NJR data set". BMJ Open. 6 (5): e011332. doi:10.1136/bmjopen-2016-011332. ISSN 2044-6055. PMC 4885469 . PMID 27217286.
- ↑ Morley, D.; Jenkinson, C.; Doll, H.; Lavis, G.; Sharp, R.; Cooke, P.; Dawson, J. (2013-04-01). "The Manchester–Oxford Foot Questionnaire (MOXFQ)". Bone & Joint Research. 2 (4): 66–69. doi:10.1302/2046-3758.24.2000147. ISSN 2046-3758. PMC 3638305 . PMID 23673374.
- ↑ Conti S, Lalonde KA, Martin R (November 2006). "Kinematic analysis of the agility total ankle during gait". Foot & Ankle International . 27 (11): 980–4. doi:10.1177/107110070602701120. PMID 17144964. S2CID 33787160.
- ↑ Banks SA, Hodge WA (June 1996). "Accurate measurement of three-dimensional knee replacement kinematics using single-plane fluoroscopy". IEEE Transactions on Bio-Medical Engineering . 43 (6): 638–49. doi:10.1109/10.495283. PMID 8987268. S2CID 21845830.
- ↑ Goldberg, Andrew J.; Chowdhury, Kashfia; Bordea, Ekaterina; Blackstone, James; Brooking, Deirdre; Deane, Elizabeth L.; Hauptmannova, Iva; Cooke, Paul; Cumbers, Marion; Skene, Simon S.; Doré, Caroline J. (2023-03-30). "Total ankle replacement versus ankle arthrodesis for patients aged 50 85 years with end-stage ankle osteoarthritis: the TARVA RCT". Health Technology Assessment. 27 (5): 1–80. doi:10.3310/PTYJ1146. ISSN 2046-4924. PMC 10150410 . PMID 37022932.
- ↑ "Severe ankle osteoarthritis: which surgery should I have?". NIHR Evidence. 9 January 2024.