Related Research Articles

Blood transfusion is the process of transferring blood products into a person's circulation intravenously. Transfusions are used for various medical conditions to replace lost components of the blood. Early transfusions used whole blood, but modern medical practice commonly uses only components of the blood, such as red blood cells, white blood cells, plasma, clotting factors and platelets.

Bleeding, hemorrhage, haemorrhage or blood loss, is blood escaping from the circulatory system from damaged blood vessels. Bleeding can occur internally, or externally either through a natural opening such as the mouth, nose, ear, urethra, vagina or anus, or through a puncture in the skin. Hypovolemia is a massive decrease in blood volume, and death by excessive loss of blood is referred to as exsanguination. Typically, a healthy person can endure a loss of 10–15% of the total blood volume without serious medical difficulties. The stopping or controlling of bleeding is called hemostasis and is an important part of both first aid and surgery.

Platelets, also called thrombocytes, are a component of blood whose function is to react to bleeding from blood vessel injury by clumping, thereby initiating a blood clot. Platelets have no cell nucleus; they are fragments of cytoplasm that are derived from the megakaryocytes of the bone marrow or lung, which then enter the circulation. Platelets are found only in mammals, whereas in other vertebrates, thrombocytes circulate as intact mononuclear cells.
Bloodless surgery is a non-invasive surgical method developed by orthopedic surgeon, Adolf Lorenz, who was known as "the bloodless surgeon of Vienna". His medical practice was a consequence of his severe allergy to carbolic acid routinely used in operating rooms of the era. His condition forced him to become a "dry surgeon". Contemporary usage of the term refers to both invasive and noninvasive medical techniques and protocols. The expression does not mean surgery that makes no use of blood or blood transfusion. Rather, it refers to surgery performed without transfusion of allogeneic blood. Champions of bloodless surgery do, however, transfuse products made from allogeneic blood and they also make use of pre-donated blood for autologous transfusion. Interest in bloodless surgery has arisen for several reasons. Jehovah's Witnesses reject blood transfusions on religious grounds; others may be concerned about bloodborne diseases, such as hepatitis and AIDS.

Cardiopulmonary bypass (CPB) is a technique in which a machine temporarily takes over the function of the heart and lungs during surgery, maintaining the circulation of blood and oxygen to the body. The CPB pump itself is often referred to as a heart–lung machine or "the pump". Cardiopulmonary bypass pumps are operated by perfusionists. CPB is a form of extracorporeal circulation. Extracorporeal membrane oxygenation is generally used for longer-term treatment.
A blood bank is a center where blood gathered as a result of blood donation is stored and preserved for later use in blood transfusion. The term "blood bank" typically refers to a department of a hospital usually within a Clinical Pathology laboratory where the storage of blood product occurs and where pre-transfusion and Blood compatibility testing is performed. However, it sometimes refers to a collection center, and some hospitals also perform collection. Blood banking includes tasks related to blood collection, processing, testing, separation, and storage.

A blood donation occurs when a person voluntarily has blood drawn and used for transfusions and/or made into biopharmaceutical medications by a process called fractionation. Donation may be of whole blood, or of specific components directly (apheresis). Blood banks often participate in the collection process as well as the procedures that follow it.
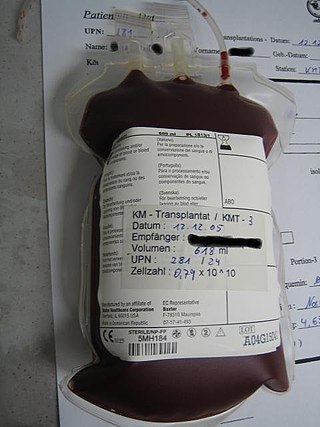
Hematopoietic stem-cell transplantation (HSCT) is the transplantation of multipotent hematopoietic stem cells, usually derived from bone marrow, peripheral blood, or umbilical cord blood in order to replicate inside of a patient and to produce additional normal blood cells. It may be autologous, allogeneic or syngeneic.

Plateletpheresis is the process of collecting thrombocytes, more commonly called platelets, a component of blood involved in blood clotting. The term specifically refers to the method of collecting the platelets, which is performed by a device used in blood donation that separates the platelets and returns other portions of the blood to the donor. Platelet transfusion can be a life-saving procedure in preventing or treating serious complications from bleeding and hemorrhage in patients who have disorders manifesting as thrombocytopenia or platelet dysfunction. This process may also be used therapeutically to treat disorders resulting in extraordinarily high platelet counts such as essential thrombocytosis.

Fresh frozen plasma (FFP) is a blood product made from the liquid portion of whole blood. It is used to treat conditions in which there are low blood clotting factors or low levels of other blood proteins. It may also be used as the replacement fluid in plasma exchange. Using ABO compatible plasma, while not required, may be recommended. Use as a volume expander is not recommended. It is given by slow injection into a vein.
Thromboelastography (TEG) is a method of testing the efficiency of blood coagulation. It is a test mainly used in surgery and anesthesiology, although increasingly used in resuscitations in Emergency Departments, intensive care units, and labor and delivery suites. More common tests of blood coagulation include prothrombin time (PT) and partial thromboplastin time (aPTT) which measure coagulation factor function, but TEG also can assess platelet function, clot strength, and fibrinolysis which these other tests cannot.
Jehovah's Witnesses believe that the Bible prohibits Christians from accepting blood transfusions. Their literature states that, "'abstaining from ... blood' means not accepting blood transfusions and not donating or storing their own blood for transfusion." The belief is based on an interpretation of scripture that differs from other Christian denominations. It is one of the doctrines for which Jehovah's Witnesses are best known.

Transfusion-related acute lung injury (TRALI) is the serious complication of transfusion of blood products that is characterized by the rapid onset of excess fluid in the lungs. It can cause dangerous drops in the supply of oxygen to body tissues. Although changes in transfusion practices have reduced the incidence of TRALI, it was the leading cause of transfusion-related deaths in the United States from fiscal year 2008 through fiscal year 2012.
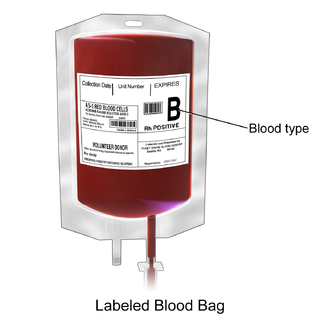
Packed red blood cells, also known as packed cells, are red blood cells that have been separated for blood transfusion. The packed cells are typically used in anemia that is either causing symptoms or when the hemoglobin is less than usually 70–80 g/L. In adults, one unit brings up hemoglobin levels by about 10 g/L. Repeated transfusions may be required in people receiving cancer chemotherapy or who have hemoglobin disorders. Cross-matching is typically required before the blood is given. It is given by injection into a vein.
An oxygenator is a medical device that is capable of exchanging oxygen and carbon dioxide in the blood of human patient during surgical procedures that may necessitate the interruption or cessation of blood flow in the body, a critical organ or great blood vessel. These organs can be the heart, lungs or liver, while the great vessels can be the aorta, pulmonary artery, pulmonary veins or vena cava.
Autotransfusion is a process wherein a person receives their own blood for a transfusion, instead of banked allogenic (separate-donor) blood. There are two main kinds of autotransfusion: Blood can be autologously "pre-donated" before a surgery, or alternatively, it can be collected during and after the surgery using an intraoperative blood salvage device. The latter form of autotransfusion is utilized in surgeries where there is expected a large volume blood loss – e.g. aneurysm, total joint replacement, and spinal surgeries. The effectiveness, safety, and cost-savings of intraoperative cell salvage in people who are undergoing thoracic or abdominal surgery following trauma is not known.
Patient Blood Management (PBM) is a set of medical practices designed to optimise the care of patients who might need a blood transfusion. Patient blood management programs use an organized framework to improve blood health, thus increasing patient safety and quality of life, reducing costs, and improving clinical outcomes. Some strategies to accomplish this include ensuring that anemia is treated prior to a surgical operation, using surgical techniques that limit blood loss, and returning blood lost during surgery to the patient via intraoperative blood salvage.
The fibrinolysis system is responsible for removing blood clots. Hyperfibrinolysis describes a situation with markedly enhanced fibrinolytic activity, resulting in increased, sometimes catastrophic bleeding. Hyperfibrinolysis can be caused by acquired or congenital reasons. Among the congenital conditions for hyperfibrinolysis, deficiency of alpha-2-antiplasmin or plasminogen activator inhibitor type 1 (PAI-1) are very rare. The affected individuals show a hemophilia-like bleeding phenotype. Acquired hyperfibrinolysis is found in liver disease, in patients with severe trauma, during major surgical procedures, and other conditions. A special situation with temporarily enhanced fibrinolysis is thrombolytic therapy with drugs which activate plasminogen, e.g. for use in acute ischemic events or in patients with stroke. In patients with severe trauma, hyperfibrinolysis is associated with poor outcome. Moreover, hyperfibrinolysis may be associated with blood brain barrier impairment, a plasmin-dependent effect due to an increased generation of bradykinin.
An autotransfusionist, also known as a perioperative blood management technologist, is a specialized allied health professional who operates the cell saver machine during surgeries that expect significant blood loss.
Retrograde autologous priming (RAP) is a means to effectively and safely restrict the hemodilution caused by the direct homologous blood transfusion and reduce the blood transfusion requirements during cardiac surgery. It is also generally considered a blood conservation method used in most patients during the cardiopulmonary bypass (CPB). The processing of RAP includes three main steps, and the entire procedure of RAP could be completed within 5 to 8 minutes. This technique is proposed by Panico in 1960 for the first time and restated by Rosengart in 1998 to eliminate or reduce the risk of hemodilution during CPB. Moreover, to precisely determine the clinical efficacy of RAP, many related studies were conducted. Most results of researches indicate that RAP is available to provide some benefits to reducing the requirements for red blood cell transfusion. However, there are still some studies showing a failure of RAP to limit the hemodilution after the open heart operation.
References
- ↑ Bolton-Maggs, Paula (2017). The 2016 Annual SHOT Report (2017). Serious Hazards of Transfusion (SHOT). ISBN 978-0-9558648-9-6.
- ↑ Standards for Perioperative Autologous Blood Collection and Administration, 5th edition. Bethesda, MD: AABB. 2013. p. 47. ISBN 978-1-56395-840-3.
- ↑ Hemobag
- ↑ http://www.noblood.org/forum/content/209-Intraoperative_blood_salvage%5B%5D
- ↑ Boldt J, Zickmann B, Fedderson B, Herold C, Dapper F, Hempelmann G (May 1991). "Six different hemofiltration devices for blood conservation in cardiac surgery". Ann Thorac Surg. 51 (5): 747–53. doi: 10.1016/0003-4975(91)90116-8 . PMID 2025077.
- ↑ Sutton RG, Kratz JM, Spinale FG, Crawford FA Jr (October 1993). "Comparison of three blood-processing techniques during and after cardiopulmonary bypass". Ann Thorac Surg. 56 (4): 938–43. doi:10.1016/0003-4975(93)90360-T. PMID 8215672.
- ↑ Eichert I, Isgro F, Kiessling AH, Saggau W (June 2001). "Cell saver, ultrafiltration and direct transfusion: comparative study of three blood processing techniques". Thorac Cardiovasc Surg. 49 (3): 149–52. doi:10.1055/s-2001-14291. PMID 11432472.
- ↑ Freischlag, Julie Ann (2004). "Intraoperative blood salvage in vascular surgery - worth the effort?". Crit Care. 8 (Suppl 2): S53–S56. doi:10.1186/cc2409. PMC 3226144 . PMID 15196326.
- ↑ Beckmann SR, Carlile D, Bissinger RC, Burrell M, Winkler T, Shely WW (June 2007). "Improved coagulation and blood conservation in the golden hours after cardiopulmonary bypass". J Extra Corpor Technol. 39 (2): 105–8. PMC 4680662 . PMID 17672193.