
Syringomyelia is a generic term referring to a disorder in which a cyst or cavity forms within the spinal cord. Often, syringomyelia is used as a generic term before an etiology is determined. This cyst, called a syrinx, can expand and elongate over time, destroying the spinal cord. The damage may result in loss of feeling, paralysis, weakness, and stiffness in the back, shoulders, and extremities. Syringomyelia may also cause a loss of the ability to feel extremes of hot or cold, especially in the hands. It may also lead to a cape-like bilateral loss of pain and temperature sensation along the upper chest and arms. The combination of symptoms varies from one patient to another depending on the location of the syrinx within the spinal cord, as well as its extent.

An ulcer is a sore on the skin or a mucous membrane, accompanied by the disintegration of tissue. Ulcers can result in complete loss of the epidermis and often portions of the dermis and even subcutaneous fat. Ulcers are most common on the skin of the lower extremities and in the gastrointestinal tract. An ulcer that appears on the skin is often visible as an inflamed tissue with an area of reddened skin. A skin ulcer is often visible in the event of exposure to heat or cold, irritation, or a problem with blood circulation.

A podiatrist is a medical professional devoted to the treatment of disorders of the foot, ankle, and related structures of the leg. The term originated in North America but has now become the accepted term in the English-speaking world for all practitioners of podiatric medicine. The word chiropodist was previously used in the United States, but it is now regarded as antiquated.
Diabetic neuropathy is various types of nerve damage associated with diabetes mellitus. Symptoms depend on the site of nerve damage and can include motor changes such as weakness; sensory symptoms such as numbness, tingling, or pain; or autonomic changes such as urinary symptoms. These changes are thought to result from a microvascular injury involving small blood vessels that supply nerves. Relatively common conditions which may be associated with diabetic neuropathy include distal symmetric polyneuropathy; third, fourth, or sixth cranial nerve palsy; mononeuropathy; mononeuropathy multiplex; diabetic amyotrophy; and autonomic neuropathy.

Pes cavus, also known as high arch, is a human foot type in which the sole of the foot is distinctly hollow when bearing weight. That is, there is a fixed plantar flexion of the foot. A high arch is the opposite of a flat foot and is somewhat less common.

A hammer toe, hammertoe or contracted toe is a deformity of the muscles and ligaments of the proximal interphalangeal joint of the second, third, fourth, or fifth toe, bending it into a shape resembling a hammer. In the early stage, a flexible hammertoe is movable at the joints; a rigid hammertoe joint cannot be moved and usually requires surgery.
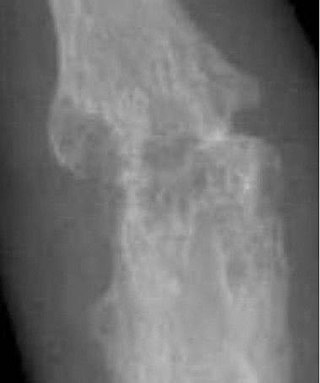
An arthropathy is a disease of a joint.
A peripheral vascular examination is a medical examination to discover signs of pathology in the peripheral vascular system. It is performed as part of a physical examination, or when a patient presents with leg pain suggestive of a cardiovascular pathology.

A calcaneal fracture is a break of the calcaneus. Symptoms may include pain, bruising, trouble walking, and deformity of the heel. It may be associated with breaks of the hip or back.
Becaplermin is a cicatrizant, available as a topical gel. Regranex is a human platelet-derived growth factor indicated along with good wound care for the treatment of lower extremity diabetic neuropathic ulcers. It is also known as "platelet-derived growth factor BB".

Diabetic shoes are specially designed shoes, or shoe inserts, intended to reduce the risk of skin breakdown in diabetics with existing foot disease and relieve pressure to prevent diabetic foot ulcers.

David G. Armstrong is an American podiatric surgeon and researcher most widely known for his work in amputation prevention, the diabetic foot, and wound healing. He and his frequent collaborators, Lawrence A. Lavery and Andrew J.M. Boulton, have together produced many key works in the taxonomy, classification and treatment of the diabetic foot. He is Professor of Surgery with Tenure and director of the Southwestern Academic Limb Salvage Alliance (SALSA) at the Keck School of Medicine of the University of Southern California and has produced more than 650 peer reviewed manuscripts and more than 110 book chapters.

Arterial insufficiency ulcers are mostly located on the lateral surface of the ankle or the distal digits. They are commonly caused by peripheral artery disease (PAD).

A diabetic foot disease is any condition that results directly from peripheral artery disease (PAD) or sensory neuropathy affecting the feet of people living with diabetes. Diabetic foot conditions can be acute or chronic complications of diabetes. Presence of several characteristic diabetic foot pathologies such as infection, diabetic foot ulcer and neuropathic osteoarthropathy is called diabetic foot syndrome. The resulting bone deformity is known as Charcot foot.

Malum perforans is a long-lasting, usually painless ulcer that penetrates deep into or through the skin, usually on the sole of the foot. It is often a complication in diabetes mellitus and other conditions affecting the nerves.

Diabetic foot ulcer is a breakdown of the skin and sometimes deeper tissues of the foot that leads to sore formation. It may occur due to a variety of mechanisms. It is thought to occur due to abnormal pressure or mechanical stress chronically applied to the foot, usually with concomitant predisposing conditions such as peripheral sensory neuropathy, peripheral motor neuropathy, autonomic neuropathy or peripheral arterial disease. It is a major complication of diabetes mellitus, and it is a type of diabetic foot disease. Secondary complications to the ulcer, such as infection of the skin or subcutaneous tissue, bone infection, gangrene or sepsis are possible, often leading to amputation.
Total contact casting (TCC) is a specially designed cast designed to take weight off of the foot (off-loading) in patients with diabetic foot ulcers (DFUs). Reducing pressure on the wound by taking weight off the foot has proven to be very effective in DFU treatment. DFUs are a major factor leading to lower leg amputations among the diabetic population in the US with 85% of amputations in diabetics being preceded by a DFU. Furthermore, the five-year post-amputation mortality rate among diabetics is estimated at 45% for those with neuropathic DFUs.
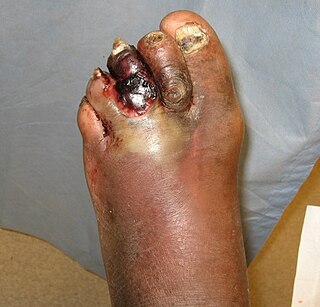
Diabetic foot infection is any infection of the foot in a diabetic person. The most frequent cause of hospitalization for diabetic patients is due to foot infections. Symptoms may include pus from a wound, redness, swelling, pain, warmth, tachycardia, or tachypnea. Complications can include infection of the bone, tissue death, amputation, or sepsis. They are common and occur equally frequently in males and females. Older people are more commonly affected.
Nachiappan Chockalingam, professionally known as Nachi Chockalingam is a British scientist, academic practitioner and expert in Clinical Biomechanics. He is a professor at Staffordshire University and a Fellow of the Institute of Physics and Engineering in Medicine and has been appointed to a panel of experts for the Research Excellence Framework. He was elected as a Fellow of the International Society of Biomechanics in 2023. Between 2016 and 2022, he has contributed to the NIHR Research for Patient Benefit Panel and serves in multiple other review panels of global grant awarding bodies including the EPSRC, MRC and the European Commission. He contributed to development of podiatric biomechanics in the UK and played a pivotal role in the establishment of the journals such as the Footwear Science and is on the editorial panel for a number of scientific and clinical journals.















