This article needs additional citations for verification .(August 2016) |
Nurses in South Africa practise in a wide variety of specialties, with a wide variety of training and experience.
This article needs additional citations for verification .(August 2016) |
Nurses in South Africa practise in a wide variety of specialties, with a wide variety of training and experience.
To take the exam to practice as an enrolled nurse, students must complete a two-year academic course that includes 2,000 hours of clinical practice.
Subjects studied in the first year include:
The second year includes study of sciences fundamental to basic nursing and, depending on the area the nursing school is approved to teach, will include one of the following subjects:
There are multiple nurse categories. Registered Nurses may study for a diploma or degree. Both function the same. Maroon epaulettes indicate a Registered Nurse with a general nursing diploma ( all Registered Nurses have general nursing) Then there is a variety of courses that can be completed and the color strips are added on the Maroon epaulettes
White epaulets indicate an enrolled nurse (staff nurse), who helps registered nurses with their duties and also helps the lower category of nurses when needed. In most hospitals, staff nurse give medications and help with doctors rounds. Staff nurses are also guided by their scope of practice and duties are under direct and indirect supervision of the Registered Nurse. If the staff nurse agrees to perform a duty s/he is accountable for her actions.
Enrolled Nursing assistants wear a blue button. They ensure all needs and comfort of the patients are met. They do everything within their scope of practice. Enrolled nurses may not penetrate the skin or body a patient without direct supervision of a registered nurse.
The South African Nursing Council (SANC) was initially established by the Nursing Act, No. 45 of 1944, and currently by the Nursing Act, No. 50 of 1978 as amended. [1] SANC inspects and approves nursing schools and education programs; examines, registers, and enrolls nurses, midwives, and nursing auxiliaries; licenses nursing agencies; and monitors nursing employers. Nurses and nurse auxiliaries are required to wear "distinguishing devices" consisting of pins and colored epaulettes to identify them as licensed professionals.

A registered nurse (RN) is a nurse who has graduated or successfully passed a nursing program from a recognized nursing school and met the requirements outlined by a country, state, province or similar government-authorized licensing body to obtain a nursing license. An RN's scope of practice is determined by legislation, and is regulated by a professional body or council.
Nurse education consists of the theoretical and practical training provided to nurses with the purpose to prepare them for their duties as nursing care professionals. This education is provided to student nurses by experienced nurses and other medical professionals who have qualified or experienced for educational tasks, traditionally in a type of professional school known as a nursing school or college of nursing. Most countries offer nurse education courses that can be relevant to general nursing or to specialized areas including mental health nursing, pediatric nursing, and post-operative nursing. Nurse education also provides post-qualification courses in specialist subjects within nursing.
Psychiatric nursing or mental health nursing is the appointed position of a nurse that specialises in mental health, and cares for people of all ages experiencing mental illnesses or distress. These include: neurodevelopmental disorders, schizophrenia, schizoaffective disorder, mood disorders, addiction, anxiety disorders, personality disorders, eating disorders, suicidal thoughts, psychosis, paranoia, and self-harm.
A licensed practical nurse (LPN), in much of the United States and Canada, is a nurse who provides direct nursing care for people who are sick, injured, convalescent, or disabled. In the United States, LPNs work under the direction of physicians, mid-level practitioners, and may work under the direction of registered nurses depending on their jurisdiction.
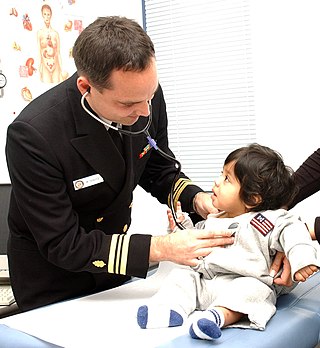
A nurse practitioner (NP) is an advanced practice registered nurse and a type of mid-level practitioner. NPs are trained to assess patient needs, order and interpret diagnostic and laboratory tests, diagnose disease, prescribe medications and formulate treatment plans. NP training covers basic disease prevention, coordination of care, and health promotion.
An advanced practice nurse (APN) is a nurse with post-graduate education and training in nursing. Nurses practicing at this level may work in either a specialist or generalist capacity. APNs are prepared with advanced didactic and clinical education, knowledge, skills, and scope of practice in nursing.
Home health is a nursing specialty in which nurses provide multidimensional home care to patients of all ages. Home health care is a cost efficient way to deliver quality care in the convenience of the client's home. Home health nurses create care plans to achieve goals based on the client's diagnosis. These plans can include preventive, therapeutic, and rehabilitative actions. Home health nurses also supervise certified nursing assistants. The professional nursing organization for home health nurses is the Home Healthcare Nurses Association (HHNA). Home health care is intended for clients that are well enough to be discharged home, but still require skilled nursing personnel to assess, initiate and oversee nursing interventions.
An Associate of Science in Nursing (ASN) is a tertiary education nursing degree which typically takes 2–3 years to complete. In the United States, this type of degree is usually awarded by community colleges or similar nursing schools. Some four-year colleges also offer this degree. Students awarded an Associate of Science in Nursing are qualified to sit for the NCLEX-RN and apply for licensure as a Registered Nurse.
Psychiatric and mental health nurses in the U.S. Army Nurse Corps employing groundbreaking protocols and treatments in psychiatric issues to address the unique challenges that our service men and women face, more commonly post-traumatic stress disorder and traumatic brain injuries. Most people understand that trauma exposure is a popular occupational hazard for military members. Psychiatric screenings, before and during their enlistment, and treatments after being exposed to warfare, death, destruction, and torture have been extremely beneficial for military personnel and their dependents.
Nursing management consists of the performance of the leadership functions of governance and decision-making within organizations employing nurses. It includes processes common to all management like planning, organizing, staffing, directing and controlling. It is common for registered nurses to seek additional education to earn a Master of Science in Nursing or Doctor of Nursing Practice to prepare for leadership roles within nursing. Management positions increasingly require candidates to hold an advanced degree in nursing.

Nursing in Australia is a healthcare profession. Nurses and midwives form the majority (54%) of Australian health care professionals. Nurses are either registered or enrolled. Registered nurses have broader and deeper education than enrolled nurses. Nurse practitioners complete a yet higher qualification. Nurses are not limited to working in hospitals, instead working in a variety of settings. Australian nurses are in demand as traveling nurses, particularly those with advanced qualifications.

Nursing in the United States is a professional health care occupation. It is the largest such occupation, employing millions of certified professionals. As of 2023, 3,175,390 registered nurses were employed, paid a median income of $86,070.

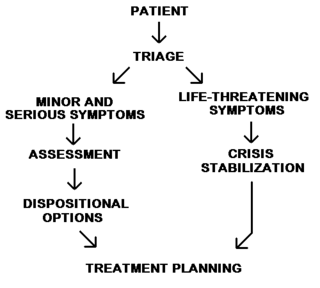
Emergency nursing is a specialty within the field of professional nursing focusing on the care of patients who require prompt medical attention to avoid long-term disability or death. In addition to addressing "true emergencies," emergency nurses increasingly care for people who are unwilling or unable to get primary medical care elsewhere and come to emergency departments for help. In fact, only a small percentage of emergency department (ED) patients have emergency conditions such as a stroke, heart attack or major trauma. Emergency nurses also tend to patients with acute alcohol and/or drug intoxication, psychiatric and behavioral problems and those who have been raped.
A surgical nurse, also referred to as a theatre nurse or scrub nurse, specializes in perioperative care, providing care to patients before, during and after surgery. To become a theatre nurse, Registered Nurses or Enrolled Nurses must complete extra training. Theatre nurses can focus on different speciality areas, depending on which they are interested in.
In the United States, a psychiatric-mental health nurse practitioner (PMHNP) is an advanced practice registered nurse trained to provide a wide range of mental health services to patients and families in a variety of settings. PMHNPs diagnose, conduct therapy, and prescribe medications for patients who have psychiatric disorders, medical organic brain disorders or substance abuse problems. They are licensed to provide emergency psychiatric services, psychosocial and physical assessments of their patients, treatment plans, and manage patient care. They may also serve as consultants or as educators for families and staff. The PMHNP has a focus on psychiatric diagnosis, including the differential diagnosis of medical disorders with psychiatric symptoms, and on medication treatment for psychiatric disorders.

A flight nurse is a registered nurse specializing in the field of providing comprehensive pre-hospital, emergency critical care, and hospital care to a vast scope of patients. The care of these patients is generally provided during aeromedical evacuation or rescue operations aboard helicopters, propeller aircraft, or jet aircraft. On board a rescue aircraft, is a flight nurse, accompanied by flight medics and respiratory practitioners, as well as the option of a flight physician for comprehensive emergency and critical transport teams. The inclusion of a flight physician is more common in pediatric and neonatal transport teams. A critical care flight nurse must be able to deal with all age groups with broad critical emergencies. With no physicians on site, the nurses scope of practice is expanded. The critical care experience is transferred over to a flight nurse with impacting factors such as altitude and changes in pressure, gravitational forces, and weather. Some patients may experience exacerbations because of factors related to the cabin environment, including hypoxia, limited mobility, gas expansion, and the risk of injury related to turbulence. Resources for definitive care are limited. Aeromedical evacuation crews coordinate with other organizations to plan for the safe and timely care and evacuation of patients. Crews must be prepared for patients with trauma and mental health illnesses.

Unlicensed assistive personnel (UAP) are paraprofessionals who assist individuals with physical disabilities, mental impairments, and other health care needs with their activities of daily living (ADLs). UAPs also provide bedside care—including basic nursing procedures—all under the supervision of a registered nurse, licensed practical nurse or other health care professional. UAPs must demonstrate their ability and competence before gaining any expanded responsibilities in a clinical setting. While providing this care, UAPs offer compassion and patience and are part of the patient's healthcare support system. Communication between UAPs and registered nurses (RNs) is key as they are working together in their patients' best interests. The scope of care UAPs are responsible for is delegated by RNs or other clinical licensed professionals.
Nursing in Kenya began in 1908 and was conducted without a formal framework until 1950. Over the decades, with demand for healthcare providers increasing due to marked growth in the population of Kenya, training programs were implemented.
Nursing in Japan did not develop as an occupation until the end of the nineteenth century. Initially introduced only in Tokyo in the late 1860s, small schools utilizing Western models were being opened by the late 1880s. In response to disaster relief, the Japanese Red Cross became an integral part of nursing development. By 1915, nurse registration had been established and public health nurses began working throughout the country. Nursing universities were established in the twentieth century and regulations were passed to develop standards for training and public health.
Nursing is the largest healthcare profession in the United States, with more than 3.1 million registered nurses. Between 2012 and 2022, employment for nurses is projected to grow by 19 percent, which is more than any other profession. Nurses make up the largest component of staff in hospitals but are also able to provide care in clinic settings, patient's homes, schools, nursing homes, public health agencies, and mental health centers. In addition, nurses can be found in the military, in industry, nursing education, and do health care research. Nurses in these various roles and settings can provide direct patient care and case management, but also develop and establish nursing practice and quality standards within complex healthcare systems. As each degree can provide a different level of care for patients and function in vastly different roles, it is important to differentiate between them. The levels of nursing degrees have different educational requirements, licensure, and credentialing that can vary state to state.