Related Research Articles

Cardiac arrest is when the heart suddenly and unexpectedly stops beating. It is a medical emergency that, without immediate medical intervention, will result in sudden cardiac death within minutes. Cardiopulmonary resuscitation (CPR) and possibly defibrillation are needed until further treatment can be provided. Cardiac arrest results in a rapid loss of consciousness, and breathing may be abnormal or absent.

Cardiopulmonary resuscitation (CPR) is an emergency procedure consisting of chest compressions often combined with artificial ventilation in an effort to manually preserve intact brain function until further measures are taken to restore spontaneous blood circulation and breathing in a person who is in cardiac arrest. It is recommended in those who are unresponsive with no breathing or abnormal breathing, for example, agonal respirations.

Mouth-to-mouth resuscitation, a form of artificial ventilation, is the act of assisting or stimulating respiration in which a rescuer presses their mouth against that of the victim and blows air into the person's lungs. Artificial respiration takes many forms, but generally entails providing air for a person who is not breathing or is not making sufficient respiratory effort on their own. It is used on a patient with a beating heart or as part of cardiopulmonary resuscitation (CPR) to achieve the internal respiration.

Drowning is a type of suffocation induced by the submersion of the mouth and nose in a liquid. Most instances of fatal drowning occur alone or in situations where others present are either unaware of the victim's situation or unable to offer assistance. After successful resuscitation, drowning victims may experience breathing problems, vomiting, confusion, or unconsciousness. Occasionally, victims may not begin experiencing these symptoms until several hours after they are rescued. An incident of drowning can also cause further complications for victims due to low body temperature, aspiration of vomit, or acute respiratory distress syndrome.
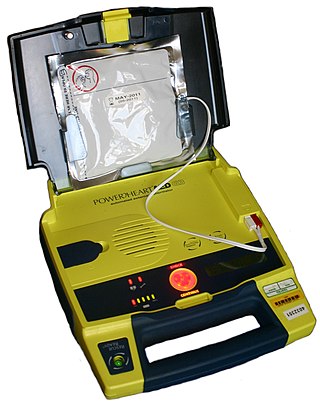
An automated external defibrillator (AED) is a portable electronic device that automatically diagnoses the life-threatening cardiac arrhythmias of ventricular fibrillation (VF) and pulseless ventricular tachycardia, and is able to treat them through defibrillation, the application of electricity which stops the arrhythmia, allowing the heart to re-establish an effective rhythm.
Basic life support (BLS) is a level of medical care which is used for patients with life-threatening illnesses or injuries until they can be given full medical care by advanced life support providers. It can be provided by trained medical personnel, such as emergency medical technicians, and by qualified bystanders.

Respiratory arrest is a sickness caused by apnea or respiratory dysfunction severe enough it will not sustain the body. Prolonged apnea refers to a patient who has stopped breathing for a long period of time. If the heart muscle contraction is intact, the condition is known as respiratory arrest. An abrupt stop of pulmonary gas exchange lasting for more than five minutes may permanently damage vital organs, especially the brain. Lack of oxygen to the brain causes loss of consciousness. Brain injury is likely if respiratory arrest goes untreated for more than three minutes, and death is almost certain if more than five minutes.
Precordial thump is a medical procedure used in the treatment of ventricular fibrillation or pulseless ventricular tachycardia under certain conditions. The procedure has a very low success rate, but may be used in those with witnessed, monitored onset of one of the "shockable" cardiac rhythms if a defibrillator is not immediately available. It should not delay cardiopulmonary resuscitation (CPR) and defibrillation, nor should it be used in those with unwitnessed out-of-hospital cardiac arrest.
Pulseless electrical activity (PEA) refers to cardiac arrest in which the electrocardiogram shows a heart rhythm that should produce a pulse, but does not. Pulseless electrical activity is found initially in about 55% of people in cardiac arrest.

Advanced Life Support (ALS) is a set of life saving protocols and skills that extend basic life support to further support the circulation and provide an open airway and adequate ventilation (breathing).

A bag valve mask (BVM), sometimes known by the proprietary name Ambu bag or generically as a manual resuscitator or "self-inflating bag", is a hand-held device commonly used to provide positive pressure ventilation to patients who are not breathing or not breathing adequately. The device is a required part of resuscitation kits for trained professionals in out-of-hospital settings (such as ambulance crews) and is also frequently used in hospitals as part of standard equipment found on a crash cart, in emergency rooms or other critical care settings. Underscoring the frequency and prominence of BVM use in the United States, the American Heart Association (AHA) Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiac Care recommend that "all healthcare providers should be familiar with the use of the bag-mask device." Manual resuscitators are also used within the hospital for temporary ventilation of patients dependent on mechanical ventilators when the mechanical ventilator needs to be examined for possible malfunction or when ventilator-dependent patients are transported within the hospital. Two principal types of manual resuscitators exist; one version is self-filling with air, although additional oxygen (O2) can be added but is not necessary for the device to function. The other principal type of manual resuscitator (flow-inflation) is heavily used in non-emergency applications in the operating room to ventilate patients during anesthesia induction and recovery.
Cough CPR is the subject of a hoax email that began circulating in 1999. It is described as a "resuscitation technique" in which through prolonged coughing and deep breathing every 2 seconds, a person suffering a cardiac dysrhythmia immediately before cardiac arrest can keep conscious until help arrives. Neither the American Heart Association nor the American Red Cross endorses cough CPR during a heart attack.

ABC and its variations are initialism mnemonics for essential steps used by both medical professionals and lay persons when dealing with a patient. In its original form it stands for Airway, Breathing, and Circulation. The protocol was originally developed as a memory aid for rescuers performing cardiopulmonary resuscitation, and the most widely known use of the initialism is in the care of the unconscious or unresponsive patient, although it is also used as a reminder of the priorities for assessment and treatment of patients in many acute medical and trauma situations, from first-aid to hospital medical treatment. Airway, breathing, and circulation are all vital for life, and each is required, in that order, for the next to be effective. Since its development, the mnemonic has been extended and modified to fit the different areas in which it is used, with different versions changing the meaning of letters or adding other letters.

The AutoPulse is an automated, portable, battery-powered cardiopulmonary resuscitation device created by Revivant and subsequently purchased and currently manufactured by ZOLL Medical Corporation. It is a chest compression device composed of a constricting band and half backboard that is intended to be used as an adjunct to CPR during advanced cardiac life support by professional health care providers. The AutoPulse uses a distributing band to deliver the chest compressions. In literature it is also known as LDB-CPR.
The chain of survival refers to a series of actions that, properly executed, reduce the mortality associated with sudden cardiac arrest. Like any chain, the chain of survival is only as strong as its weakest link. The six interdependent links in the chain of survival are early recognition of sudden cardiac arrest and access to emergency medical care, early CPR, early defibrillation, early advanced cardiac life support, and physical and emotional recovery. The first three links in the chain can be performed by lay bystanders, while the second three links are designated to medical professionals. Currently, between 70 and 90% of cardiac arrest patients die before they reach the hospital. However, a cardiac arrest does not have to be lethal if bystanders can take the right steps immediately.
The history of cardiopulmonary resuscitation (CPR) can be traced as far back as the literary works of ancient Egypt. However, it was not until the 18th century that credible reports of cardiopulmonary resuscitation began to appear in the medical literature.
Pediatric advanced life support (PALS) is a course offered by the American Heart Association (AHA) for health care providers who take care of children and infants in the emergency room, critical care and intensive care units in the hospital, and out of hospital. The course teaches healthcare providers how to assess injured and sick children and recognize and treat respiratory distress/failure, shock, cardiac arrest, and arrhythmias.

Rearrest is a phenomenon that involves the resumption of a lethal cardiac dysrhythmia after successful return of spontaneous circulation (ROSC) has been achieved during the course of resuscitation. Survival to hospital discharge rates are as low as 7% for cardiac arrest in general and although treatable, rearrest may worsen these survival chances. Rearrest commonly occurs in the out-of-hospital setting under the treatment of health care providers.
Extracorporeal cardiopulmonary resuscitation is a method of cardiopulmonary resuscitation (CPR) that passes the patient's blood through a machine in a process to oxygenate the blood supply. A portable extracorporeal membrane oxygenation (ECMO) device is used as an adjunct to standard CPR. A patient who is deemed to be in cardiac arrest refractory to CPR has percutaneous catheters inserted into the femoral vein and artery. Theoretically, the application of ECPR allows for the return of cerebral perfusion in a more sustainable manner than with external compressions alone. By attaching an ECMO device to a person who has acutely undergone cardiovascular collapse, practitioners can maintain end-organ perfusion whilst assessing the potential reversal of causal pathology, with the goal of improving long-term survival and neurological outcomes.
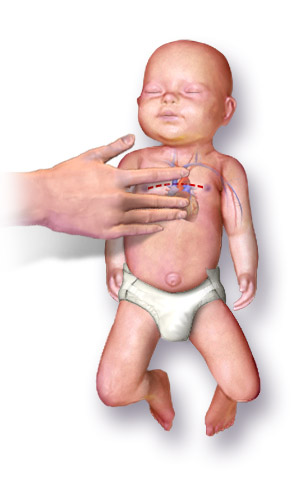
Neonatal resuscitation, also known as newborn resuscitation, is an emergency procedure focused on supporting approximately 10% of newborn children who do not readily begin breathing, putting them at risk of irreversible organ injury and death. Through positive airway pressure, and in severe cases chest compressions, medical personnel certified in neonatal resuscitation can often stimulate neonates to begin breathing on their own, with attendant normalization of heart rate.