| Intravenous therapy | |
|---|---|
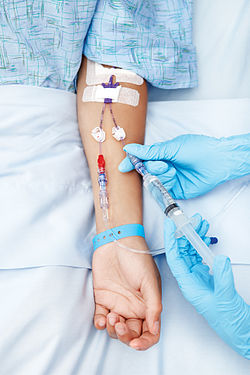 A person receiving a medication through an intravenous line (cannula) | |
| Other names | IV therapy |
| ICD-9-CM | 38.93 |
| MeSH | D007262 |
Intravenous therapy (abbreviated as IV therapy) is a medical process that administers fluids, medications and nutrients directly into a person's vein. The intravenous route of administration is commonly used for rehydration or to provide nutrients for those who cannot, or will not—due to reduced mental states or otherwise—consume food or water by mouth. It may also be used to administer medications or other medical therapy such as blood products or electrolytes to correct electrolyte imbalances. Attempts at providing intravenous therapy have been recorded as early as the 1400s, but the practice did not become widespread until the 1900s after the development of techniques for safe, effective use.
Contents
- Uses
- Medical uses
- Other uses
- Types
- Bolus
- Infusion
- Secondary
- Methods and equipment
- Access
- Infusions
- Techniques
- Adverse effects
- Pain
- Infection and inflammation
- Infiltration and extravasation
- Others 2
- History
- Discovery and development
- Modern usage
- See also
- References
- Further reading
- External links
The intravenous route is the fastest way to deliver medications and fluid replacement throughout the body as they are introduced directly into the circulatory system and thus quickly distributed. For this reason, the intravenous route of administration is also used for the consumption of some recreational drugs. Many therapies are administered as a "bolus" or one-time dose, but they may also be administered as an extended infusion or drip. The act of administering a therapy intravenously, or placing an intravenous line ("IV line") for later use, is a procedure which should only be performed by a skilled professional. The most basic intravenous access consists of a needle piercing the skin and entering a vein which is connected to a syringe or to external tubing. This is used to administer the desired therapy. In cases where a patient is likely to receive many such interventions in a short period (with consequent risk of trauma to the vein), normal practice is to insert a cannula which leaves one end in the vein, and subsequent therapies can be administered easily through tubing at the other end. In some cases, multiple medications or therapies are administered through the same IV line.
IV lines are classified as "central lines" if they end in a large vein close to the heart, or as "peripheral lines" if their output is to a small vein in the periphery, such as the arm. An IV line can be threaded through a peripheral vein to end near the heart, which is termed a "peripherally inserted central catheter" or PICC line. If a person is likely to need long-term intravenous therapy, a medical port may be implanted to enable easier repeated access to the vein without having to pierce the vein repeatedly. A catheter can also be inserted into a central vein through the chest, which is known as a tunneled line. The specific type of catheter used and site of insertion are affected by the desired substance to be administered and the health of the veins in the desired site of insertion.
Placement of an IV line may cause pain, as it necessarily involves piercing the skin. Infections and inflammation (termed phlebitis) are also both common side effects of an IV line. Phlebitis may be more likely if the same vein is used repeatedly for intravenous access, and can eventually develop into a hard cord which is unsuitable for IV access. The unintentional administration of a therapy outside a vein, termed extravasation or infiltration, may cause other side effects.