
Skin is the layer of usually soft, flexible outer tissue covering the body of a vertebrate animal, with three main functions: protection, regulation, and sensation.

7-Dehydrocholesterol (7-DHC) is a zoosterol that functions in the serum as a cholesterol precursor, and is photochemically converted to vitamin D3 in the skin, therefore functioning as provitamin-D3. The presence of this compound in human skin enables humans to manufacture vitamin D3 (cholecalciferol). Upon exposure to ultraviolet UV-B rays in the sun light, 7-DHC is converted into vitamin D3 via previtamin D3 as an intermediate isomer. It is also found in the milk of several mammalian species. Lanolin, a waxy substance that is naturally secreted by wool-bearing mammals, contains 7-DHC which is converted into vitamin D by sunlight and then ingested during grooming as a nutrient. In insects 7-dehydrocholesterol is a precursor for the hormone ecdysone, required for reaching adulthood. 7-DHC was discovered by Nobel-laureate organic chemist Adolf Windaus.

Melanocytes are melanin-producing neural crest-derived cells located in the bottom layer of the skin's epidermis, the middle layer of the eye, the inner ear, vaginal epithelium, meninges, bones, and heart found in many mammals and birds. Melanin is a dark pigment primarily responsible for skin color. Once synthesized, melanin is contained in special organelles called melanosomes which can be transported to nearby keratinocytes to induce pigmentation. Thus darker skin tones have more melanosomes present than lighter skin tones. Functionally, melanin serves as protection against UV radiation. Melanocytes also have a role in the immune system.

The integumentary system is the set of organs forming the outermost layer of an animal's body. It comprises the skin and its appendages, which act as a physical barrier between the external environment and the internal environment that it serves to protect and maintain the body of the animal. Mainly it is the body's outer skin.

Keratinocytes are the primary type of cell found in the epidermis, the outermost layer of the skin. In humans, they constitute 90% of epidermal skin cells. Basal cells in the basal layer of the skin are sometimes referred to as basal keratinocytes. Keratinocytes form a barrier against environmental damage by heat, UV radiation, water loss, pathogenic bacteria, fungi, parasites, and viruses. A number of structural proteins, enzymes, lipids, and antimicrobial peptides contribute to maintain the important barrier function of the skin. Keratinocytes differentiate from epidermal stem cells in the lower part of the epidermis and migrate towards the surface, finally becoming corneocytes and eventually being shed, which happens every 40 to 56 days in humans.
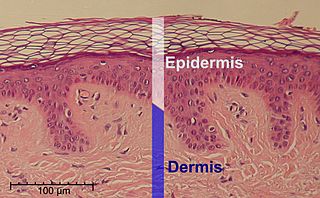
The epidermis is the outermost of the three layers that comprise the skin, the inner layers being the dermis and hypodermis. The epidermal layer provides a barrier to infection from environmental pathogens and regulates the amount of water released from the body into the atmosphere through transepidermal water loss.

The dermis or corium is a layer of skin between the epidermis and subcutaneous tissues, that primarily consists of dense irregular connective tissue and cushions the body from stress and strain. It is divided into two layers, the superficial area adjacent to the epidermis called the papillary region and a deep thicker area known as the reticular dermis. The dermis is tightly connected to the epidermis through a basement membrane. Structural components of the dermis are collagen, elastic fibers, and extrafibrillar matrix. It also contains mechanoreceptors that provide the sense of touch and thermoreceptors that provide the sense of heat. In addition, hair follicles, sweat glands, sebaceous glands, apocrine glands, lymphatic vessels, nerves and blood vessels are present in the dermis. Those blood vessels provide nourishment and waste removal for both dermal and epidermal cells.

The Malpighian layer of the epidermis is generally defined as both the stratum basale and the thicker stratum spinosum immediately above it as a single unit, although it is occasionally defined as the stratum basale specifically, or the stratum spinosum specifically.

A skin condition, also known as cutaneous condition, is any medical condition that affects the integumentary system—the organ system that encloses the body and includes skin, nails, and related muscle and glands. The major function of this system is as a barrier against the external environment.

The stratum corneum is the outermost layer of the epidermis. Consisting of dead tissue, it protects underlying tissue from infection, dehydration, chemicals and mechanical stress. It is composed of 15–20 layers of flattened cells with no nuclei and cell organelles.

The stratum lucidum is a thin, clear layer of dead skin cells in the epidermis named for its translucent appearance under a microscope. It is readily visible by light microscopy only in areas of thick skin, which are found on the palms of the hands and the soles of the feet.

The stratum granulosum is a thin layer of cells in the epidermis lying above the stratum spinosum and below the stratum corneum. Keratinocytes migrating from the underlying stratum spinosum become known as granular cells in this layer. These cells contain keratohyalin granules, which are filled with histidine- and cysteine-rich proteins that appear to bind the keratin filaments together. Therefore, the main function of keratohyalin granules is to bind intermediate keratin filaments together.

The stratum spinosum is a layer of the epidermis found between the stratum granulosum and stratum basale. This layer is composed of polyhedral keratinocytes. These are joined with desmosomes. Their spiny appearance is due to shrinking of the microfilaments between desmosomes that occurs when stained with H&E. Keratinization begins in the stratum spinosum, although the actual keratinocytes begin in the stratum basale. They have large pale-staining nuclei as they are active in synthesizing fibrillar proteins, known as cytokeratin, which build up within the cells aggregating together forming tonofibrils. The tonofibrils go on to form the desmosomes, which allow for strong connections to form between adjacent keratinocytes. The stratum spinosum also contains Langerhans cells, which functions as a macrophage by engulfing bacteria, foreign particles, and damaged cells that occur in this layer.
Protection from mechanical injury, chemical hazards, and bacterial invasion is provided by the skin because the epidermis is relatively thick and covered with keratin. Secretions from sebaceous glands and sweat glands also benefit this protective barrier. In the event of an injury that damages the skin's protective barrier, the body triggers a response called wound healing. After hemostasis, inflammation white blood cells, including phagocytic macrophages arrive at the injury site. Once the invading microorganisms have been brought under control, the skin proceeds to heal itself. The ability of the skin to heal even after considerable damage has occurred is due to the presence of stem cells in the dermis and cells in the stratum basale of the epidermis, all of which can generate new tissue.
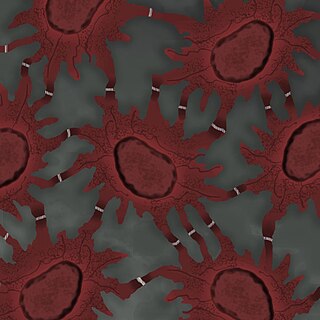
Spinous cells, or prickle cells, are keratin producing epidermal cells owing their prickly appearance to their numerous intracellular connections. They make up the stratum spinosum of the epidermis and provide a continuous net-like layer of protection for underlying tissue. They are susceptible to mutations caused by sunlight and can become malignant.

The human skin is the outer covering of the body and is the largest organ of the integumentary system. The skin has up to seven layers of ectodermal tissue guarding muscles, bones, ligaments and internal organs. Human skin is similar to most of the other mammals' skin, and it is very similar to pig skin. Though nearly all human skin is covered with hair follicles, it can appear hairless. There are two general types of skin: hairy and glabrous skin (hairless). The adjective cutaneous literally means "of the skin".
Corneocytes are terminally differentiated keratinocytes and compose most of the stratum corneum, the outermost layer of the epidermis. They are regularly replaced through desquamation and renewal from lower epidermal layers and are essential for its function as a skin barrier.
Skin sloughing is the process of shedding dead surface cells from the skin. It is most associated with cosmetic skin maintenance via exfoliation, but can also occur biologically or for medical reasons.
Tissue engineering of oral mucosa combines cells, materials and engineering to produce a three-dimensional reconstruction of oral mucosa. It is meant to simulate the real anatomical structure and function of oral mucosa. Tissue engineered oral mucosa shows promise for clinical use, such as the replacement of soft tissue defects in the oral cavity. These defects can be divided into two major categories: the gingival recessions which are tooth-related defects, and the non tooth-related defects. Non tooth-related defects can be the result of trauma, chronic infection or defects caused by tumor resection or ablation. Common approaches for replacing damaged oral mucosa are the use of autologous grafts and cultured epithelial sheets.














