
Dandruff is a skin condition that mainly affects the scalp. Symptoms include flaking and sometimes mild itchiness. It can result in social or self-esteem problems. A more severe form of the condition, which includes inflammation of the skin, is known as seborrhoeic dermatitis.
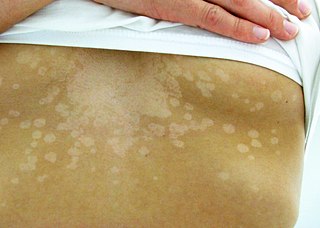
Tinea versicolor is a condition characterized by a skin eruption on the trunk and proximal extremities. The majority of tinea versicolor is caused by the fungus Malassezia globosa, although Malassezia furfur is responsible for a small number of cases. These yeasts are normally found on the human skin and become troublesome only under certain conditions, such as a warm and humid environment, although the exact conditions that cause initiation of the disease process are poorly understood.

Seborrhoeic dermatitis is a long-term skin disorder. Symptoms include flaky, scaly, greasy, and occasionally itchy and inflamed skin. Areas of the skin rich in oil-producing glands are often affected including the scalp, face, and chest. It can result in social or self-esteem problems. In babies, when the scalp is primarily involved, it is called cradle cap. Seborrhoeic dermatitis of the scalp may be described in lay terms as dandruff due to the dry, flaky character of the skin. However, as dandruff may refer to any dryness or scaling of the scalp, not all dandruff is seborrhoeic dermatitis. Seborrhoeic dermatitis is sometimes inaccurately referred to as seborrhoea.
Skin disorders are among the most common health problems in dogs, and have many causes. The condition of a dog's skin and coat is also an important indicator of its general health. Skin disorders of dogs vary from acute, self-limiting problems to chronic or long-lasting problems requiring life-time treatment. Skin disorders may be primary or secondary in nature, making diagnosis complicated.

Malassezia furfur is a species of yeast that is naturally found on the skin surfaces of humans and some other mammals. It is associated with a variety of dermatological conditions caused by fungal infections, notably seborrhoeic dermatitis and tinea versicolor. As an opportunistic pathogen, it has further been associated with dandruff, malassezia folliculitis, pityriasis versicolor (alba), and malassezia intertrigo, as well as catheter-related fungemia and pneumonia in patients receiving hematopoietic transplants.

Trichosporon is a genus of anamorphic fungi in the family Trichosporonaceae. All species of Trichosporon are yeasts with no known teleomorphs. Most are typically isolated from soil, but several species occur as a natural part of the skin microbiota of humans and other animals. Proliferation of Trichosporon yeasts in the hair can lead to an unpleasant but non-serious condition known as white piedra. Trichosporon species can also cause severe opportunistic infections (trichosporonosis) in immunocompromised individuals.

Malassezia globosa is a species of yeast-like fungus.
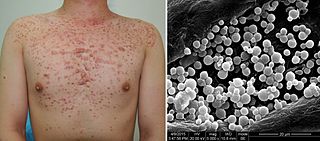
Malassezia folliculitis or Pityrosporum folliculitis, is a skin condition caused by infection by Malassezia yeast.
Moniliella is a genus of fungi in the subdivision Ustilaginomycotina. It is in the monotypic family MoniliellaceaeQ.M. Wang, F.Y. Bai & Boekhout, which is in the monotypic order MoniliellalesQ.M. Wang, F.Y. Bai & Boekhout which is in the monotypic class MoniliellomycetesQ.M. Wang, F.Y. Bai & Boekhout.
Malassezia japonica is a fungus that can cause opportunistic infections in animals.
Malassezia dermatis is a fungus that can cause opportunistic infections in animals.
Malassezia equina is a fungus first isolated in horses, which can cause opportunistic infections in animals. Its type strain is MA146=CBS 9969. This species will not grow without any lipid supplementation. It grows slowly and forms small colonies. In the lab, colonies will not grow at temperatures of 40 °C, differing from M. sympodialis-related species, such M. dermatis and M. nana, which can grow at this temperature. Malassezia caprae cells are ovoidal.
Malassezia caprae is a fungus first isolated in goats, which can cause opportunistic infections in animals. Its type strain is MA383=CBS 10434. This species will not grow without any lipid supplementation. It grows slowly and forms small colonies. In the lab, colonies will not grow at temperatures of 40 °C, differing from M. sympodialis-related species, such M. dermatis and M. nana, which can grow at this temperature. Malassezia caprae cells are ellipsoidal to more or less spherical.
Malassezia nana is a fungus that can cause opportunistic infections in animals. It was first isolated from animals in Japan and Brazil. M. nana resembles M. dermatis and M. sympodialis, but is distinguished from these species by its inability to use Kolliphor EL (Sigma) as the sole lipid source and to hydrolyse aesculin. The type strain of M. nana is NUSV 1003T(=CBS 9557T=JCM 12085T).
Malassezia pachydermatis is a zoophilic yeast in the division Basidiomycota. It was first isolated in 1925 by Fred Weidman, and it was named pachydermatis after the original sample taken from an Indian rhinoceros with severe exfoliative dermatitis. Within the genus Malassezia, M. pachydermatis is most closely related to the species M. furfur. A commensal fungus, it can be found within the microflora of healthy mammals such as humans, cats and dogs, However, it is capable of acting as an opportunistic pathogen under special circumstances and has been seen to cause skin and ear infections, most often occurring in canines.
Malassezia sympodialis is a species in the genus Malassezia. It is characterized by a pronounced lipophily, unilateral, percurrent or sympodial budding and an irregular, corrugated cell wall ultrastructure. It is one of the most common species found on the skin of healthy and diseased individuals. It is considered to be part of the skin's normal human microbiota and begins to colonize the skin of humans shortly after birth. Malassezia sympodialis, often has a symbiotic or commensal relationship with its host, but it can act as a pathogen causing a number of different skin diseases, such as atopic dermatitis.

Trichosporon asteroides is an asexual basidiomycetous fungus first described from human skin but now mainly isolated from blood and urine. T. asteroides is a hyphal fungus with a characteristically yeast-like appearance due to the presence of slimy arthroconidia. Infections by this species usually respond to treatment with azoles and amphotericin B.
Fungal genomes are among the smallest genomes of eukaryotes. The sizes of fungal genomes range from less than 10 Mbp to hundreds of Mbp. The average genome size is approximately 37 Mbp in Ascomycota, 47 Mbp in Basidiomycota and 75 Mbp in Oomycota. The sizes and gene numbers of the smallest genomes of free-living fungi such as those of Wallemia ichthyophaga, Wallemia mellicola or Malassezia restricta are comparable to bacterial genomes. The genome of the extensively researched yeast Saccharomyces cerevisiae contains approximately 12 Mbp and was the first completely sequenced eukaryotic genome. Due to their compact size fungal genomes can be sequenced with less resources than most other eukaryotic genomes and are thus important models for research. Some fungi exist as stable haploid, diploid, or polyploid cells, others change ploidy in response to environmental conditions and aneuploidy is also observed in novel environments or during periods of stress.
Malassezia arunalokei is a species of yeast-like fungus that was identified as a new to science in 2016. It has been isolated from the skin of both seborrheic dermatitis patients and healthy individuals from India. A combination of several phenotypic characteristics distinguish this species from others in genus Malassezia. These include: colony morphology ; the absence of activity from the enzyme catalase; growth at 37 °C (99 °F); and the precipitation that results when grown with the chemicals Tween 20 or Cremophor EL.
Topical antifungaldrugs are used to treat fungal infections on the skin, scalp, nails, vagina or inside the mouth. These medications come as creams, gels, lotions, ointments, powders, shampoos, tinctures and sprays. Most antifungal drugs induce fungal cell death by destroying the cell wall of the fungus. These drugs inhibit the production of ergosterol, which is a fundamental component of the fungal cell membrane and wall.









