Related Research Articles

Tracheal intubation, usually simply referred to as intubation, is the placement of a flexible plastic tube into the trachea (windpipe) to maintain an open airway or to serve as a conduit through which to administer certain drugs. It is frequently performed in critically injured, ill, or anesthetized patients to facilitate ventilation of the lungs, including mechanical ventilation, and to prevent the possibility of asphyxiation or airway obstruction.

An endoscopy is a procedure used in medicine to look inside the body. The endoscopy procedure uses an endoscope to examine the interior of a hollow organ or cavity of the body. Unlike many other medical imaging techniques, endoscopes are inserted directly into the organ.
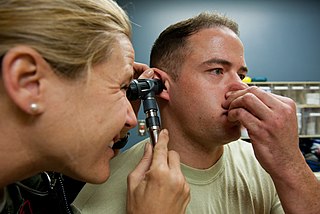
The Valsalva maneuver is performed by a forceful attempt of exhalation against a closed airway, usually done by closing one's mouth and pinching one's nose shut while expelling air out as if blowing up a balloon. Variations of the maneuver can be used either in medical examination as a test of cardiac function and autonomic nervous control of the heart, or to clear the ears and sinuses when ambient pressure changes, as in scuba diving, hyperbaric oxygen therapy, or air travel.
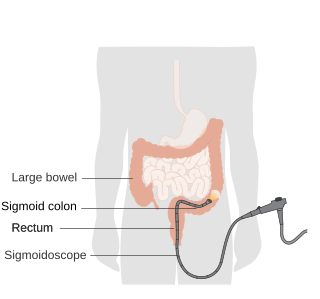
Sigmoidoscopy is the minimally invasive medical examination of the large intestine from the rectum through to the nearest part of the colon, the sigmoid colon. There are two types of sigmoidoscopy: flexible sigmoidoscopy, which uses a flexible endoscope, and rigid sigmoidoscopy, which uses a rigid device. Flexible sigmoidoscopy is generally the preferred procedure. A sigmoidoscopy is similar to, but not the same as, a colonoscopy. A sigmoidoscopy only examines up to the sigmoid, the most distal part of the colon, while colonoscopy examines the whole large bowel.

Laryngoscopy is endoscopy of the larynx, a part of the throat. It is a medical procedure that is used to obtain a view, for example, of the vocal folds and the glottis. Laryngoscopy may be performed to facilitate tracheal intubation during general anaesthesia or cardiopulmonary resuscitation or for surgical procedures on the larynx or other parts of the upper tracheobronchial tree.
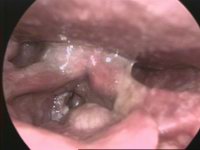
Laryngeal cancers are mostly squamous-cell carcinomas, reflecting their origin from the epithelium of the larynx.
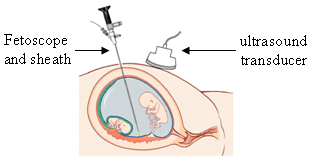
An endoscope is an inspection instrument composed of image sensor, optical lens, light source and mechanical device, which is used to look deep into the body by way of openings such as the mouth or anus. A typical endoscope applies several modern technologies including optics, ergonomics, precision mechanics, electronics, and software engineering. With an endoscope, it is possible to observe lesions that cannot be detected by X-ray, making it useful in medical diagnosis. Endoscopes use tubes which are only a few millimeters thick to transfer illumination in one direction and high-resolution images in real time in the other direction, resulting in minimally invasive surgeries. "Endo" is Greek for "within" while "scope" comes from the Greek word "skopos" meaning to target or look out. It is used to examine the internal organs like the throat or esophagus. Specialized instruments are named after their target organ. Examples include the cystoscope (bladder), nephroscope (kidney), bronchoscope (bronchus), arthroscope (joints) and colonoscope (colon), and laparoscope. They can be used to examine visually and diagnose, or assist in surgery such as an arthroscopy.

In a physical examination, medical examination, or clinical examination, a medical practitioner examines a patient for any possible medical signs or symptoms of a medical condition. It generally consists of a series of questions about the patient's medical history followed by an examination based on the reported symptoms. Together, the medical history and the physical examination help to determine a diagnosis and devise the treatment plan. These data then become part of the medical record.

Airway management includes a set of maneuvers and medical procedures performed to prevent and relieve airway obstruction. This ensures an open pathway for gas exchange between a patient's lungs and the atmosphere. This is accomplished by either clearing a previously obstructed airway; or by preventing airway obstruction in cases such as anaphylaxis, the obtunded patient, or medical sedation. Airway obstruction can be caused by the tongue, foreign objects, the tissues of the airway itself, and bodily fluids such as blood and gastric contents (aspiration).

Fine-needle aspiration (FNA) is a diagnostic procedure used to investigate lumps or masses. In this technique, a thin, hollow needle is inserted into the mass for sampling of cells that, after being stained, are examined under a microscope (biopsy). The sampling and biopsy considered together are called fine-needle aspiration biopsy (FNAB) or fine-needle aspiration cytology (FNAC). Fine-needle aspiration biopsies are very safe minor surgical procedures. Often, a major surgical biopsy can be avoided by performing a needle aspiration biopsy instead, eliminating the need for hospitalization. In 1981, the first fine-needle aspiration biopsy in the United States was done at Maimonides Medical Center. Today, this procedure is widely used in the diagnosis of cancer and inflammatory conditions.

Laryngeal papillomatosis, also known as recurrent respiratory papillomatosis (RRP) or glottal papillomatosis, is a rare medical condition in which benign tumors (papilloma) form along the aerodigestive tract. There are two variants based on the age of onset: juvenile and adult laryngeal papillomatosis. The tumors are caused by human papillomavirus (HPV) infection of the throat. The tumors may lead to narrowing of the airway, which may cause vocal changes or airway obstruction. Laryngeal papillomatosis is initially diagnosed through indirect laryngoscopy upon observation of growths on the larynx and can be confirmed through a biopsy. Treatment for laryngeal papillomatosis aims to remove the papillomas and limit their recurrence. Due to the recurrent nature of the virus, repeated treatments usually are needed. Laryngeal papillomatosis is primarily treated surgically, though supplemental nonsurgical and/or medical treatments may be considered in some cases. The evolution of laryngeal papillomatosis is highly variable. Though total recovery may be observed, it is often persistent despite treatment. The number of new cases of laryngeal papillomatosis cases is approximately 4.3 cases per 100,000 children and 1.8 cases per 100,000 adults annually.
Bronchoalveolar lavage (BAL) is a diagnostic method of the lower respiratory system in which a bronchoscope is passed through the mouth or nose into an appropriate airway in the lungs, with a measured amount of fluid introduced and then collected for examination. This method is typically performed to diagnose pathogenic infections of the lower respiratory airways, though it also has been shown to have utility in diagnosing interstitial lung disease. Bronchoalveolar lavage can be a more sensitive method of detection than nasal swabs in respiratory molecular diagnostics, as has been the case with SARS-CoV-2 where bronchoalveolar lavage samples detect copies of viral RNA after negative nasal swab testing.

Laryngomalacia is the most common cause of chronic stridor in infancy, in which the soft, immature cartilage of the upper larynx collapses inward during inhalation, causing airway obstruction. It can also be seen in older patients, especially those with neuromuscular conditions resulting in weakness of the muscles of the throat. However, the infantile form is much more common. Laryngomalacia is one of the most common laryngeal congenital disease in infancy and public education about the signs and symptoms of the disease is lacking.

Blunt trauma, also known as blunt force trauma or non-penetrating trauma, is physical trauma or impactful force to a body part, often occurring with road traffic collisions, direct blows, assaults, injuries during sports, and particularly in the elderly who fall. It is contrasted with penetrating trauma which occurs when an object pierces the skin and enters a tissue of the body, creating an open wound and bruise.
Oropharyngeal dysphagia arises from abnormalities of muscles, nerves or structures of the oral cavity, pharynx, and upper esophageal sphincter.
Müller's maneuver is a procedure used in medicine to diagnose some types of tinnitus, and other medical problems.
Bronchoscopy is an endoscopic technique of visualizing the inside of the airways for diagnostic and therapeutic purposes. An instrument (bronchoscope) is inserted into the airways, usually through the nose or mouth, or occasionally through a tracheostomy. This allows the practitioner to examine the patient's airways for abnormalities such as foreign bodies, bleeding, tumors, or inflammation. Specimens may be taken from inside the lungs. The construction of bronchoscopes ranges from rigid metal tubes with attached lighting devices to flexible optical fiber instruments with realtime video equipment.
Tracheal intubation, an invasive medical procedure, is the placement of a flexible plastic catheter into the trachea. For millennia, tracheotomy was considered the most reliable method of tracheal intubation. By the late 19th century, advances in the sciences of anatomy and physiology, as well as the beginnings of an appreciation of the germ theory of disease, had reduced the morbidity and mortality of this operation to a more acceptable rate. Also in the late 19th century, advances in endoscopic instrumentation had improved to such a degree that direct laryngoscopy had finally become a viable means to secure the airway by the non-surgical orotracheal route. Nasotracheal intubation was not widely practiced until the early 20th century. The 20th century saw the transformation of the practices of tracheotomy, endoscopy and non-surgical tracheal intubation from rarely employed procedures to essential components of the practices of anesthesia, critical care medicine, emergency medicine, gastroenterology, pulmonology and surgery.
Flexible Endoscopic Evaluation of Swallowing with Sensory Testing (FEESST), or laryngopharyngeal sensory testing, is a technique used to directly examine motor and sensory functions of swallowing so that proper treatment can be given to patients with swallowing difficulties to decrease their risk of aspiration and choking. FEESST was invented by Dr. Jonathan E. Aviv MD, FACS in 1993, and has been used by otolaryngologists, pulmonologists, gastroenterologists, intensivists and speech-language pathologists for the past 20 years.

Advanced airway management is the subset of airway management that involves advanced training, skill, and invasiveness. It encompasses various techniques performed to create an open or patent airway – a clear path between a patient's lungs and the outside world.
References
- ↑ "What is Nasopharynx Endoscopy: Overview, Benefits, and Expected Results". DocDoc.
- ↑ Anand, Vinod, MD, FACS (1993). "Nasopharyngoscopy" (PDF). noseandsinus.net. American Academy of Otolaryngology - Head and Neck Surgery, Inc., Alexandria, VA.
- ↑ "Flexible Nasopharyngoscopy/Laryngoscopy". Nationwide Children's Hospital. Retrieved 23 December 2020.
- ↑ Alvi, Sirhan; Harsha, Pooja (October 27, 2020). Flexible Nasopharyngoscopy. National Center for Biotechnology Information. PMID 30969562.
- ↑ Goldberg, Jeffrey E. (2020). "Fiberoptic Nasopharyngoscopy". jgoldbergmd.com. Retrieved 23 December 2020.
- ↑ Gregórioa, Marcelo Gervilla; Jacomellib, Márcia; Figueiredo, Adelaide C.; Cahali, Michel Burihan; Juniore, Wilson Leite Pedreira; Filho, Geraldo Lorenzi (7 February 2006). "Evaluation of airway obstruction by nasopharyngoscopy: comparison of the Müller maneuver versus induced sleep". Brazilian Journal of Otorhinolaryngology. 73 (5): 618–622. doi: 10.1016/S1808-8694(15)30121-X . PMC 9445644 . PMID 18094802.
- ↑ Shneerson, J.; Smith, I. (9 August 1997). "Rapid Response: Flexible nasopharyngoscopy". The BMJ . 315 (367): 367–369. doi:10.1136/bmj.315.7104.367. PMC 2127235 . PMID 9270464.
- ↑ O'Sullivan, Brian; Finger, Lenna; Zwerdling, Robert G. (2004). "Use of Nasopharyngoscopy in the Evaluation of Children With Noisy Breathing". Chest . 125 (4): 1265–1269. doi:10.1378/chest.125.4.1265. PMID 15078733.
- ↑ Goldberg, Jeffrey (2020). "Nasopharyngeal Tumors". jgoldbergmd.com. Retrieved 23 December 2020.
- ↑ "Nasopharyngeal Cancer". WebMD . Retrieved 23 December 2020.
- ↑ Yang, Shujuan; Wu, Siying; Y. Chen, Xiao (6 November 2015). "Screening for nasopharyngeal cancer". Cochrane Database of Systematic Reviews. 2015 (11): CD008423. doi:10.1002/14651858.CD008423.pub2. PMC 6486300 . PMID 26544798.