
Plague is an infectious disease caused by the bacterium Yersinia pestis. Symptoms include fever, weakness and headache. Usually this begins one to seven days after exposure. There are three forms of plague, each affecting a different part of the body and causing associated symptoms. Pneumonic plague infects the lungs, causing shortness of breath, coughing and chest pain; bubonic plague affects the lymph nodes, making them swell; and septicemic plague infects the blood and can cause tissues to turn black and die.

Mumps is a viral disease caused by the mumps virus. Initial symptoms of mumps are non-specific and include fever, headache, malaise, muscle pain, and loss of appetite. These symptoms are usually followed by painful swelling of the parotid glands, called parotitis, which is the most common symptom of a mumps infection. Symptoms typically occur 16 to 18 days after exposure to the virus and resolve within two weeks. About one third of infections are asymptomatic.

Shigellosis is an infection of the intestines caused by Shigella bacteria. Symptoms generally start one to two days after exposure and include diarrhea, fever, abdominal pain, and feeling the need to pass stools even when the bowels are empty. The diarrhea may be bloody. Symptoms typically last five to seven days and it may take several months before bowel habits return entirely to normal. Complications can include reactive arthritis, sepsis, seizures, and hemolytic uremic syndrome.

Coccidioidomycosis, commonly known as cocci, Valley fever, as well as California fever, desert rheumatism, or San Joaquin Valley fever, is a mammalian fungal disease caused by Coccidioides immitis or Coccidioides posadasii. Coccidioidomycosis is endemic in certain parts of the United States in Arizona, California, Nevada, New Mexico, Texas, Utah, and northern Mexico.

Psittacosis—also known as parrot fever, and ornithosis—is a zoonotic infectious disease in humans caused by a bacterium called Chlamydia psittaci and contracted from infected parrots, such as macaws, cockatiels, and budgerigars, and from pigeons, sparrows, ducks, hens, gulls and many other species of birds. The incidence of infection in canaries and finches is believed to be lower than in psittacine birds.

Hepatitis A is an infectious disease of the liver caused by Hepatovirus A (HAV); it is a type of viral hepatitis. Many cases have few or no symptoms, especially in the young. The time between infection and symptoms, in those who develop them, is 2–6 weeks. When symptoms occur, they typically last 8 weeks and may include nausea, vomiting, diarrhea, jaundice, fever, and abdominal pain. Around 10–15% of people experience a recurrence of symptoms during the 6 months after the initial infection. Acute liver failure may rarely occur, with this being more common in the elderly.

Leptospirosis is a blood infection caused by the bacteria Leptospira that can infect humans, dogs, rodents and many other wild and domesticated animals. Signs and symptoms can range from none to mild to severe. Weil's disease, the acute, severe form of leptospirosis, causes the infected individual to become jaundiced, develop kidney failure, and bleed. Bleeding from the lungs associated with leptospirosis is known as severe pulmonary haemorrhage syndrome.

Fasciolosis is a parasitic worm infection caused by the common liver fluke Fasciola hepatica as well as by Fasciola gigantica. The disease is a plant-borne trematode zoonosis, and is classified as a neglected tropical disease (NTD). It affects humans, but its main host is ruminants such as cattle and sheep. The disease progresses through four distinct phases; an initial incubation phase of between a few days up to three months with little or no symptoms; an invasive or acute phase which may manifest with: fever, malaise, abdominal pain, gastrointestinal symptoms, urticaria, anemia, jaundice, and respiratory symptoms. The disease later progresses to a latent phase with less symptoms and ultimately into a chronic or obstructive phase months to years later. In the chronic state the disease causes inflammation of the bile ducts, gall bladder and may cause gall stones as well as fibrosis. While chronic inflammation is connected to increased cancer rates, it is unclear whether fasciolosis is associated with increased cancer risk.

Salmonellosis is a symptomatic infection caused by bacteria of the Salmonella type. It is also a food-borne disease and these are defined as diseases, usually either infectious or toxic in nature, caused by agents that enter the body through the ingestion of food. In humans, the most common symptoms are diarrhea, fever, abdominal cramps, and vomiting. Symptoms typically occur between 12 hours and 36 hours after exposure, and last from two to seven days. Occasionally more significant disease can result in dehydration. The old, young, and others with a weakened immune system are more likely to develop severe disease. Specific types of Salmonella can result in typhoid fever or paratyphoid fever.
Colic in horses is defined as abdominal pain, but it is a clinical symptom rather than a diagnosis. The term colic can encompass all forms of gastrointestinal conditions which cause pain as well as other causes of abdominal pain not involving the gastrointestinal tract. What makes it tricky is that different causes can manifest with similar signs of distress in the animal. Recognizing and understanding these signs is pivotal, as timely action can spell the difference between a brief moment of discomfort and a life-threatening situation. The most common forms of colic are gastrointestinal in nature and are most often related to colonic disturbance. There are a variety of different causes of colic, some of which can prove fatal without surgical intervention. Colic surgery is usually an expensive procedure as it is major abdominal surgery, often with intensive aftercare. Among domesticated horses, colic is the leading cause of premature death. The incidence of colic in the general horse population has been estimated between 4 and 10 percent over the course of the average lifespan. Clinical signs of colic generally require treatment by a veterinarian. The conditions that cause colic can become life-threatening in a short period of time.

The schedule for childhood immunizations in the United States is published by the Centers for Disease Control and Prevention (CDC). The vaccination schedule is broken down by age: birth to six years of age, seven to eighteen, and adults nineteen and older. Childhood immunizations are key in preventing diseases with epidemic potential.

Dicrocoelium dendriticum, the lancet liver fluke, is a parasite fluke that tends to live in cattle or other grazing mammals.
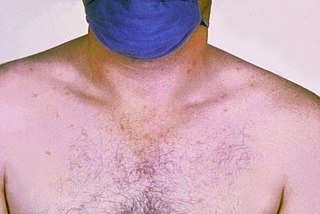
Paratyphoid fever, also known simply as paratyphoid, is a bacterial infection caused by one of three types of Salmonella enterica. Symptoms usually begin 6–30 days after exposure and are the same as those of typhoid fever. Often, a gradual onset of a high fever occurs over several days. Weakness, loss of appetite, and headaches also commonly occur. Some people develop a skin rash with rose-colored spots. Without treatment, symptoms may last weeks or months. Other people may carry the bacteria without being affected; however, they are still able to spread the disease to others. Typhoid and paratyphoid are of similar severity. Paratyphoid and typhoid fever are types of enteric fever.

Ehrlichiosis is a tick-borne bacterial infection, caused by bacteria of the family Anaplasmataceae, genera Ehrlichia and Anaplasma. These obligate intracellular bacteria infect and kill white blood cells.
Neorickettsia is a genus of bacteria. Species or strains in this genus are coccoid or pleomorphic cells that reside in cytoplasmic vacuoles within monocytes and macrophages of dogs, horses, bats, and humans.

Mosquito-borne diseases or mosquito-borne illnesses are diseases caused by bacteria, viruses or parasites transmitted by mosquitoes. Nearly 700 million people get a mosquito-borne illness each year resulting in over 725,000 deaths.
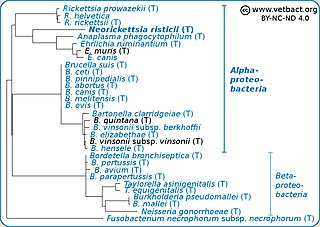
Neorickettsia risticii, formerly Ehrlichia risticii, is an obligate intracellular gram negative bacteria that typically lives as an endosymbiont to parasitic flatworms, specifically flukes. N. risticii is the known causative agent of equine neorickettsiosis, which gets its name from its discovery near the Potomac River in Maryland and Virginia. N. risticii was first recovered from horses in this region in 1984 but was not recognized as the causative agent of PHF until 1979. Potomac horse fever is currently endemic in the United States but has also been reported with lower frequency in other regions, including Canada, Brazil, Uruguay, and Europe. PHF is a condition that is clinically important for horses since it can cause serious signs such as fever, diarrhea, colic, and laminitis. PHF has a fatality rate of approximately 30%, making this condition one of the concerns for horse owners in endemic regions N. risticii is typically acquired in the middle to late summer near freshwater streams or rivers, as well as on irrigated pastures. This is a seasonal infection because it relies on the ingestion of an arthropod vector, which are more commonly found on pasture in the summer months. Although N. risticii is a well known causative agent for PHF in horses, it may act as a potential pathogen in cats and dogs as well. Not only has N. risticii been successfully cultured from monocytes of dogs and cats, but cats have become clinically ill after experimental infection with the bacteria. In addition, N. risticii has been isolated and cultured from human histiocytic lymphoma cells.

A feline zoonosis is a viral, bacterial, fungal, protozoan, nematode or arthropod infection that can be transmitted to humans from the domesticated cat, Felis catus. Some of these diseases are reemerging and newly emerging infections or infestations caused by zoonotic pathogens transmitted by cats. In some instances, the cat can display symptoms of infection and sometimes the cat remains asymptomatic. There can be serious illnesses and clinical manifestations in people who become infected. This is dependent on the immune status and age of the person. Those who live in close association with cats are more prone to these infections. But those that do not keep cats as pets are also able to acquire these infections because of the transmission can be from cat feces and the parasites that leave their bodies.
Neorickettsia helminthoeca is a bacterium in the Neorickettsia genus that causes Salmon poisoning disease.

Gastropod-borne parasitic diseases (GPDs) are a group of infectious diseases that require a gastropod species to serve as an intermediate host for a parasitic organism that can infect humans upon ingesting the parasite or coming into contact with contaminated water sources. These diseases can cause a range of symptoms, from mild discomfort to severe, life-threatening conditions, with them being prevalent in many parts of the world, particularly in developing regions. Preventive measures such as proper sanitation and hygiene practices, avoiding contact with infected gastropods and cooking or boiling food properly can help to reduce the risk of these diseases.

















