Related Research Articles

A dental implant is a prosthesis that interfaces with the bone of the jaw or skull to support a dental prosthesis such as a crown, bridge, denture, or facial prosthesis or to act as an orthodontic anchor. The basis for modern dental implants is a biological process called osseointegration, in which materials such as titanium or zirconia form an intimate bond to the bone. The implant fixture is first placed so that it is likely to osseointegrate, then a dental prosthetic is added. A variable amount of healing time is required for osseointegration before either the dental prosthetic is attached to the implant or an abutment is placed which will hold a dental prosthetic/crown.
Osseointegration is the direct structural and functional connection between living bone and the surface of a load-bearing artificial implant. A more recent definition defines osseointegration as "functional ankylosis ", where new bone is laid down directly on the implant surface and the implant exhibits mechanical stability. Osseointegration has enhanced the science of medical bone and joint replacement techniques as well as dental implants and improving prosthetics for amputees.
Periodontology or periodontics is the specialty of dentistry that studies supporting structures of teeth, as well as diseases and conditions that affect them. The supporting tissues are known as the periodontium, which includes the gingiva (gums), alveolar bone, cementum, and the periodontal ligament. A periodontist is a dentist that specializes in the prevention, diagnosis and treatment of periodontal disease and in the placement of dental implants.

Maxillary sinus floor augmentation is a surgical procedure which aims to increase the amount of bone in the posterior maxilla, in the area of the premolar and molar teeth, by lifting the lower Schneiderian membrane and placing a bone graft.
“Lateral periodontal cysts (LPCs) are defined as non-keratinised and non-inflammatory developmental cysts located adjacent or lateral to the root of a vital tooth.” LPCs are a rare form of jaw cysts, with the same histopathological characteristics as gingival cysts of adults (GCA). Hence LPCs are regarded as the intraosseous form of the extraosseous GCA. They are commonly found along the lateral periodontium or within the bone between the roots of vital teeth, around mandibular canines and premolars. Standish and Shafer reported the first well-documented case of LPCs in 1958, followed by Holder and Kunkel in the same year although it was called a periodontal cyst. Since then, there has been more than 270 well-documented cases of LPCs in literature.
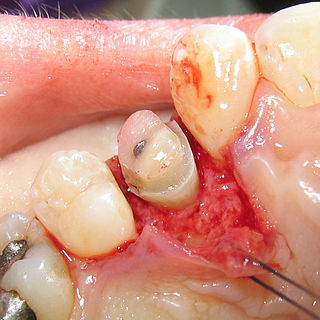
Crown lengthening is a surgical procedure performed by a dentist, or more frequently a periodontist, where more tooth is exposed by removing some of the gingival margin (gum) and supporting bone. Crown lengthening can also be achieved orthodontically by extruding the tooth.
Gingivectomy is a dental procedure in which a dentist or oral surgeon cuts away part of the gums in the mouth.

In dentistry, the subepithelial connective tissue graft is an oral and maxillofacial surgical procedure first described by Alan Edel in 1974. Currently, it is generally used to obtain root coverage following gingival recession, which was a later development by Burt Langer in the early 1980s.
Laser-assisted new attachment procedure (LANAP) is a surgical therapy for the treatment of periodontitis, intended to work through regeneration rather than resection. This therapy and the laser used to perform it have been in use since 1994. It was developed by Robert H. Gregg II and Delwin McCarthy.
Hessam Nowzari is the Director of the University of Southern California Advanced Periodontics program, since 1995, and is a diplomate of the American Board of Periodontology.
A barrier membrane is a device used in oral surgery and periodontal surgery to prevent epithelium, which regenerates relatively quickly, from growing into an area in which another, more slowly growing tissue type, such as bone, is desired. Such a method of preventing epithelial migration into a specific area is known as guided tissue regeneration (GTR).

In dentistry, a furcation defect is bone loss, usually a result of periodontal disease, affecting the base of the root trunk of a tooth where two or more roots meet. The extent and configuration of the defect are factors in both diagnosis and treatment planning.
Socket preservation or alveolar ridge preservation is a procedure to reduce bone loss after tooth extraction. After tooth extraction, the jaw bone has a natural tendency to become narrow, and lose its original shape because the bone quickly resorbs, resulting in 30–60% loss in bone volume in the first six months. Bone loss, can compromise the ability to place a dental implant, or its aesthetics and functional ability.
Chronic periodontitis is one of the seven categories of periodontitis as defined by the American Academy of Periodontology 1999 classification system. Chronic periodontitis is a common disease of the oral cavity consisting of chronic inflammation of the periodontal tissues that is caused by the accumulation of profuse amounts of dental plaque. Periodontitis initially begins as gingivitis and can progress onto chronic and subsequent aggressive periodontitis according to the 1999 classification.
Aggressive periodontitis describes a type of periodontal disease and includes two of the seven classifications of periodontitis as defined by the 1999 classification system:
- Localized aggressive periodontitis (LAP)
- Generalized aggressive periodontitis (GAP)

Peri-implantitis is a destructive inflammatory process affecting the soft and hard tissues surrounding dental implants. The soft tissues become inflamed whereas the alveolar bone, which surrounds the implant for the purposes of retention, is lost over time.

Angularis nigra, Latin for 'black angle', also known as open gingival embrasures, and colloquially known as "black triangle", is the space or gap seen at the cervical embrasure, below the contact point of some teeth. The interdental papilla does not fully enclose the space, leading to an aperture between adjacent teeth. This gap has many causes including gingival recession, and gingival withdrawal post-orthodontic work. Interdental "black triangles" were rated as the third-most-disliked aesthetic problem below caries and crown margins. Treatment of angularis nigra often requires an interdisciplinary approach, involving periodontal, orthodontic and restorative treatment. Possible treatments to correct angularis nigra include addition of composite resin in the space, veneer placement, or gum graft. Angularis nigra is generally only treated based on the aesthetic preference of the patient.
Platelet-rich fibrin (PRF) or leukocyte- and platelet-rich fibrin (L-PRF) is a derivative of PRP where autologous platelets and leukocytes are present in a complex fibrin matrix to accelerate the healing of soft and hard tissue and is used as a tissue-engineering scaffold in oral and maxillofacial surgeries. PRF falls under FDA Product Code KST, labeling it as a blood draw/Hematology product classifying it as 510(k) exempt.

Gingival grafting, also called gum grafting or periodontal plastic surgery, is a generic term for the performance of any of a number of periodontal surgical procedures in which the gum tissue is grafted. The aim may be to cover exposed root surfaces or merely to augment the band of keratinized tissue.
Periodontal surgery is a form of dental surgery that prevents or corrects anatomical, traumatic, developmental, or plaque-induced defects in the bone, gingiva, or alveolar mucosa. The objectives of this surgery include accessibility of instruments to root surface, elimination of inflammation, creation of an oral environment for plaque control, periodontal diseases control, oral hygiene maintenance, maintain proper embrasure space, address gingiva-alveolar mucosa problems, and esthetic improvement. The surgical procedures include crown lengthening, frenectomy, and mucogingival flap surgery.
References
- ↑ Larsen P, Ghali GE (2004). Peterson's Principals of Oral and Maxillofacial Surgery. Hamilton, Ont: B.C. Decker. ISBN 978-1-55009-234-9.[ page needed ]
- ↑ Hurley LA, Stinchfield FE, Bassett AL, Lyon WH (October 1959). "The role of soft tissues in osteogenesis. An experimental study of canine spine fusions". The Journal of Bone and Joint Surgery. American Volume. 41-A: 1243–54. doi:10.2106/00004623-195941070-00007. PMID 13852565.
- ↑ Melcher AH (May 1976). "On the repair potential of periodontal tissues". Journal of Periodontology. 47 (5): 256–60. doi:10.1902/jop.1976.47.5.256. PMID 775048.
- ↑ Mützel W, Tillmann K, Gerhards E (February 1979). "[Time of persistence of fluocortolone hexanoate in the knee-joint after intra-articular injection (author's transl)]". Deutsche Medizinische Wochenschrift. 104 (8): 293–5. doi:10.1055/s-0028-1103897. PMID 761531.
- 1 2 Wang HL, Boyapati L (March 2006). ""PASS" principles for predictable bone regeneration". Implant Dentistry. 15 (1): 8–17. doi:10.1097/01.id.0000204762.39826.0f. PMID 16569956. S2CID 3548845.
- 1 2 3 4 5 Liu J, Kerns DG (May 2014). "Mechanisms of guided bone regeneration: a review". The Open Dentistry Journal. 8: 56–65. doi: 10.2174/1874210601408010056 . PMC 4040931 . PMID 24894890.
- ↑ Nyman S, Lindhe J, Karring T, Rylander H (July 1982). "New attachment following surgical treatment of human periodontal disease". Journal of Clinical Periodontology. 9 (4): 290–6. doi:10.1111/j.1600-051X.1982.tb02095.x. PMID 6964676.
- ↑ Gottlow J, Nyman S, Karring T, Lindhe J (September 1984). "New attachment formation as the result of controlled tissue regeneration". Journal of Clinical Periodontology. 11 (8): 494–503. doi:10.1111/j.1600-051X.1984.tb00901.x. PMID 6384274.
- ↑ Gottlow J, Nyman S, Lindhe J, Karring T, Wennström J (July 1986). "New attachment formation in the human periodontium by guided tissue regeneration. Case reports". Journal of Clinical Periodontology. 13 (6): 604–16. doi:10.1111/j.1600-051X.1986.tb00854.x. PMID 3462208.
- ↑ Klokkevold PR, Newman MC, Takei HH (2006). Carranza's Clinical Periodontology. Philadelphia: Saunders. ISBN 978-1-4160-2400-2.[ page needed ]
- 1 2 Clinical periodontology and implant dentistry. Lindhe, Jan., Lang, Niklaus Peter., Karring, Thorkild. (5th ed.). Oxford: Blackwell Munksgaard. 2008. ISBN 978-1405160995. OCLC 171258234.
{{cite book}}: CS1 maint: others (link) - 1 2 3 4 5 Goldstep, Fay (9 December 2015). "Bone Grafts For Implant Dentistry: The Basics". Oral Health Group. Retrieved 2019-01-29.
- ↑ Barbu H, Comăneanu M, Bucur M (Mar 2012). "Guided Bone Regeneration in severely resorbed maxilla". Rev. chir. oro-maxilo-fac. implantol. (in Romanian). 3 (1): 24–29. ISSN 2069-3850. 61. Retrieved 2012-08-30.(webpage has a translation button)
- ↑ Dahlin, Christer; Gottlow, Jan; Linde, Anders; Nyman, Sture (January 1990). "Healing of Maxillary and Mandibular Bone Defects Using a Membrane Technique: An Experimental Study in Monkeys". Scandinavian Journal of Plastic and Reconstructive Surgery and Hand Surgery. 24 (1): 13–19. doi:10.3109/02844319009004514. ISSN 0284-4311. PMID 2389116.
- ↑ Liu, Jie; Kerns, David G (2014-05-16). "Mechanisms of Guided Bone Regeneration: A Review". The Open Dentistry Journal. 8 (Suppl 1): 56–65. doi: 10.2174/1874210601408010056 . ISSN 1874-2106. PMC 4040931 . PMID 24894890.
- ↑ Dahlin, C; Linde, A; Gottlow, J; Nyman, S (May 1988). "Healing of bone defects by guided tissue regeneration". Plastic and Reconstructive Surgery. 81 (5): 672–676. doi:10.1097/00006534-198805000-00004. PMID 3362985. S2CID 8014548.
- ↑ Buser, D.; Brägger, U.; Lang, N. P.; Nyman, S. (1990). "Regeneration and enlargement of jaw bone using guided tissue regeneration". Clinical Oral Implants Research. 1 (1): 22–32. doi:10.1034/j.1600-0501.1990.010104.x. ISSN 1600-0501. PMID 2099209.
- ↑ Esposito M, Grusovin MG, Papanikolaou N, Coulthard P, Worthington HV (October 2009). "Enamel matrix derivative (Emdogain(R)) for periodontal tissue regeneration in intrabony defects". The Cochrane Database of Systematic Reviews (4): CD003875. doi:10.1002/14651858.cd003875.pub3. PMC 6786880 . PMID 19821315.
- ↑ Arunjaroensuk S, Panmekiate S, Pimkhaokham A (2017-10-13). "The Stability of Augmented Bone Between Two Different Membranes Used for Guided Bone Regeneration Simultaneous with Dental Implant Placement in the Esthetic Zone". The International Journal of Oral & Maxillofacial Implants. 33 (1): 206–216. doi:10.11607/jomi.5492. PMID 29028848.
- 1 2 Bateman G, Saha S, Chapple IL (2007). Contemporary periodontal surgery: an illustrated guide to the art behind the science. London: Quintessence. ISBN 9781850971238.