
Pseudomonadota is a major phylum of Gram-negative bacteria. The renaming of several prokaryote phyla in 2021, including Pseudomonadota, remains controversial among microbiologists, many of whom continue to use the earlier name Proteobacteria, of long standing in the literature. The phylum Proteobacteria includes a wide variety of pathogenic genera, such as Escherichia, Salmonella, Vibrio, Yersinia, Legionella, and many others. Others are free-living (non-parasitic) and include many of the bacteria responsible for nitrogen fixation.
Pontiac fever is an acute, nonfatal respiratory disease caused by various species of Gram-negative bacteria in the genus Legionella. It causes a mild upper respiratory infection that resembles acute influenza. Pontiac fever resolves spontaneously and often goes undiagnosed. Both Pontiac fever and the more severe Legionnaire's disease may be caused by the same bacteria, but Pontiac fever does not include pneumonia.
Legionella is a genus of pathogenic gram-negative bacteria that includes the species L. pneumophila, causing legionellosis including a pneumonia-type illness called Legionnaires' disease and a mild flu-like illness called Pontiac fever.
Atypical pneumonia, also known as walking pneumonia, is any type of pneumonia not caused by one of the pathogens most commonly associated with the disease. Its clinical presentation contrasts to that of "typical" pneumonia. A variety of microorganisms can cause it. When it develops independently from another disease, it is called primary atypical pneumonia (PAP).

Legionella pneumophila is an aerobic, pleomorphic, flagellated, non-spore-forming, Gram-negative bacterium of the genus Legionella. L. pneumophila is the primary human pathogenic bacterium in this group. In nature, L. pneumophila infects freshwater and soil amoebae of the genera Acanthamoeba and Naegleria. This pathogen is found commonly near freshwater environments and will then invade the amoebae found in these environments, using them to carry out metabolic functions.
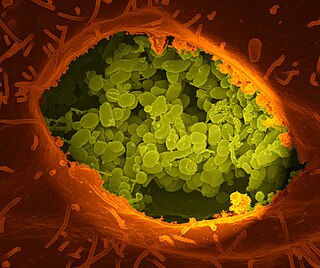
Coxiella burnetii is an obligate intracellular bacterial pathogen, and is the causative agent of Q fever. The genus Coxiella is morphologically similar to Rickettsia, but with a variety of genetic and physiological differences. C. burnetii is a small Gram-negative, coccobacillary bacterium that is highly resistant to environmental stresses such as high temperature, osmotic pressure, and ultraviolet light. These characteristics are attributed to a small cell variant form of the organism that is part of a biphasic developmental cycle, including a more metabolically and replicatively active large cell variant form. It can survive standard disinfectants, and is resistant to many other environmental changes like those presented in the phagolysosome.

Lassa mammarenavirus (LASV) is an arenavirus that causes Lassa hemorrhagic fever, a type of viral hemorrhagic fever (VHF), in humans and other primates. Lassa mammarenavirus is an emerging virus and a select agent, requiring Biosafety Level 4-equivalent containment. It is endemic in West African countries, especially Sierra Leone, the Republic of Guinea, Nigeria, and Liberia, where the annual incidence of infection is between 300,000 and 500,000 cases, resulting in 5,000 deaths per year.

Betaproteobacteria are a class of Gram-negative bacteria, and one of the eight classes of the phylum Pseudomonadota.

Alphaproteobacteria is a class of bacteria in the phylum Pseudomonadota. The Magnetococcales and Mariprofundales are considered basal or sister to the Alphaproteobacteria. The Alphaproteobacteria are highly diverse and possess few commonalities, but nevertheless share a common ancestor. Like all Proteobacteria, its members are gram-negative, although some of its intracellular parasitic members lack peptidoglycan and are consequently gram variable.
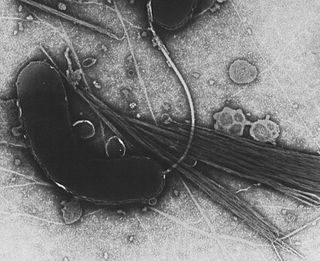
Gammaproteobacteria is a class of bacteria in the phylum Pseudomonadota. It contains about 250 genera, which makes it the most genus-rich taxon of the Prokaryotes. Several medically, ecologically, and scientifically important groups of bacteria belong to this class. All members of this class are Gram-negative. It is the most phylogenetically and physiologically diverse class of the Pseudomonadota.

Coxiella refers to a genus of Gram-negative bacteria in the family Coxiellaceae. It is named after Herald Rea Cox (1907–1986), an American bacteriologist. It is one of the Gammaproteobacteria.
Rickettsiella is a genus of the family Coxiellaceae. It should not be confused with Rickettsia. It is currently considered of the Gammaproteobacteria. However, its placement under Coxiellaceae instead of Legionellaceae has been challenged.

Charles C. Shepard was a microbiologist, and former director of the Centers for Disease Control’s Laboratory Division. It was the diligent efforts of Shepard, and cohort microbiologist Joseph McDade, which led to the 1977 discovery of the initially elusive bacterium Legionella pneumophila, the etiologic agent that causes ‘Legionnaires' disease’. In 1963, he was presented with the Gorgas Medal from the Association of Military Surgeons of the United States (AMSUS).

The 1976 Legionnaires' disease outbreak, occurring in the late summer in Philadelphia, Pennsylvania, United States was the first occasion in which a cluster of a particular type of pneumonia cases were determined to be caused by the Legionella pneumophila bacteria.
Conserved signature inserts and deletions (CSIs) in protein sequences provide an important category of molecular markers for understanding phylogenetic relationships. CSIs, brought about by rare genetic changes, provide useful phylogenetic markers that are generally of defined size and they are flanked on both sides by conserved regions to ensure their reliability. While indels can be arbitrary inserts or deletions, CSIs are defined as only those protein indels that are present within conserved regions of the protein.
Legionella anisa is a Gram-negative bacterium, one of more than 40 species in the family Legionellaceae. After Legionella pneumophila, this species has been isolated most frequently from water samples. This species is also one of the several pathogenic forms of Legionella having been associated with rare clinical cases of illness including Pontiac fever and Legionnaires' disease.
Legionella jordanis is a Gram-negative bacterium from the genus Legionella which was isolated from the Jordan River in Bloomington, Indiana and from the sewage in DeKalb County, Georgia. L. jordanis is a rare human pathogen and can cause respiratory tract infections.

Legionnaires' disease is a form of atypical pneumonia caused by any species of Legionella bacteria, quite often Legionella pneumophila. Signs and symptoms include cough, shortness of breath, high fever, muscle pains, and headaches. Nausea, vomiting, and diarrhea may also occur. This often begins 2–10 days after exposure.
Aquicella is a genus of Gram-negative rod-shaped cells and filaments in the family Coxiellaceae from the order Legionellales. The type species of this genus is Aquicella lusitana.












