| Testicular pain | |
|---|---|
| Other names | Scrotal pain, orchialgia |
 | |
| 1 - 6: Epididymis 7: Vas deferens | |
| Specialty | Urology |
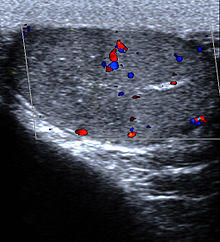
| Diagnostic method | Ultrasound, urine tests, blood tests [1] [2] |
| Differential diagnosis | Acute: Epididymitis, testicular torsion, testicular cancer, varicocele, Fournier gangrene [1] Chronic: Varicocele, spermatocele, Henoch–Schönlein purpura, post-vasectomy pain syndrome, chronic pelvic pain syndrome [2] |
Testicular pain, also known as scrotal pain, occurs when part or all of either one or both testicles hurts. Pain in the scrotum is also often included. Testicular pain may be of sudden onset or of long duration. [1] [2]
Contents
- Definition
- Chronic scrotal pain
- Differential diagnosis
- Testicular torsion
- Epididymitis and orchitis
- Fournier's gangrene
- Others
- Diagnostic approach
- Physical findings
- Laboratory tests
- Imaging
- References
- External links
Causes range from non serious muscular skeletal problems to emergency conditions such as Fournier gangrene and testicular torsion. The diagnostic approach involves making sure no serious conditions are present. Diagnosis may be supported by ultrasound, urine tests, and blood tests. [1] [2]
Pain management is typically given with definitive management depending on the underlying cause.